Category: Pediatrics
Keywords: Fever, infants, blood culture (PubMed Search)
Posted: 6/15/2018 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
The rate of occult bacteremia in infants 3 months to 24 months with a temperature higher than 40.5C was slightly higher when compared to those with a temperature higher than 39C.
363 infants (3 months to 24 months) with a fever > 40.5C who were well appearing were evaluated in this study. 4 were diagnosed with occult bacteremia (1.1%). 3 of these were caused by S. pneumoniae and 2 were fully immunized.
A larger sample size is needed to see if reconditions to include empiric blood cultures on this subgroup of patients is warrented.
After introduction of the pneumococcal conjugate vaccine, occult bacteremia dramatically decreased. Previous cost effective analysis showed that if the rate of occult bacteremia was less than 0.5%, then empiric testing should be eliminated, but if it is over 1.5%, then obtaining blood work is cost effective. In vaccinated patients, the occult bacteremia rates is less than 0.5%. These studies that showed this included patients with temperatures > 39C. This study looked at higher temperatures to see if there was a higher rate of occult bacteremia in this subgroup. In this ED, in all children with a temperature > 40.5C it was recommended that patients get a blood culture, WBC, ANC, CRP, UA, procalcitonin and PCR for pneumococcus and meningococcus regardless of immunization status. Further testing was at the discretion of the physician.
Gangoiti et al. Prevalence of Occult Bacteremia in Infants with Very High Fever without a source. Pediatr Infect Dis J. 2018 Feb. epub ahead of print.
Category: Pediatrics
Keywords: augmentin, conjunctivitis, AOM, otitis media (PubMed Search)
Posted: 6/8/2018 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Although conjuncitivitis outside of the neonatal period is commonly caused by viruses, there are times when antibiotics are warranted due to bacterial infections, such as conjuncitivits-otitis syndrome.
Bottom line: Every patient with conjunctivitis should have an examination of his/her TMs, as your management may change.
Teoh DL, Reynolds S. Diagnosis and management of pediatric conjunctivitis. Pediatric Emergency Care: 2003; 19(1), pp. 48-55.
Bodor FF, Marchant CD, Shurin PA, Barenkamp SJ. Bacterial etiology of conjunctivitis-otitis media syndrome. Pediatrics: 1985; 76(1), pp.26-28.
Bodor FF. Conjunctivitis-Otitis Syndrome. Pediatrics: 1982; 69(6), 695-698.
Category: Pediatrics
Keywords: Button batteries, removal (PubMed Search)
Posted: 5/18/2018 by Jenny Guyther, MD
(Updated: 5/2/2026)
Click here to contact Jenny Guyther, MD
There were 180 battery ingestions over a 5 year period at two tertiary care children’s hospital. The median age was 3.8 years (0.7 to 18 years). The most common symptoms were abdominal pain (17%), and nausea and vomiting (14%). X-rays detected the location in 94% of patients.
Based on these patients, a treatment algorithm was developed (See attached). Prospective validation is needed.
All patients with esophageal batteries had an intervention (foley catheter removal with post procedure esophagram, ridged esophagram or EGD).
The majority of patients with a gastric battery or small bowel battery were managed non operatively.
20 patients had a colonic battery and 7 had symptoms of abdominal pain or nausea or vomiting.
For batteries distal to the gastroesophageal junction, 16 patients had an intervention. 13 had an EGD with a 69% retrieval rate. 1 patient had a colonoscopy with successful retrieval. 2 patients had abdominal surgery with retrieval.
Rosenfled et al. Battery ingestions in children: Variations in care and development of a clinical algorithm. Journal of Pediatric Surgery. 2018. Epub ahead of print.
Category: Pediatrics
Keywords: supination with flexion, hyperpronation (PubMed Search)
Posted: 5/4/2018 by Sarah Kleist, MD
Click here to contact Sarah Kleist, MD
Nursemaid’s elbow is a common pediatric injury with peak incidence occurring between two and three years of age. It is a condition that typically arises from a sudden upward pull of the arm as an axial traction is placed on the forearm, and the radius is pulled through the annular ligament, resulting in subluxation of the radial head. Over the years, various maneuvers have been attempted, but the two most common are supination with flexion and hyperpronation. A 2017 Cochrane meta-analysis analyzed 8 trials specifically comparing supination with flexion versus hyperpronation. Data from those trials suggested that hyperpronation resulted in less failures at ?rst attempt than the supination-?exion, and although there was limited data, there was no obvious difference in adverse events or pain between the two techniques.
Bottom Line: There is likely a lower risk of failure with first attempt reduction with hyperpronation than with supination-flexion for nursemaid’s elbow.
References:
1. Schutzman SA, Teach S. Upper-extremity impairment in young children. Ann Emerg Med. 1995;26:474-479.
2. Hart GM. Subluxation of the head of the radius in young children. J Am Med Assoc. 1959;169:1734-1736.
3. Vitello S, Dvorkin R, Sattler S, Levy D, Ung L. Epidemiology of Nursemaid’s Elbow. Western Journal of Emergency Medicine, Vol 15, Iss 4, Pp 554-557 (2014). 2014:554.
4. Macias CG, Bothner J, Wiebe R. A comparison of supination/flexion to hyperpronation in the reduction of radial head subluxations. Pediatrics. 1998;102:e10-e10.
5. Bexkens R, Washburn FJ, Eygendaal D, van den Bekerom M,P.J., Oh LS. Effectiveness of reduction maneuvers in the treatment of nursemaid's elbow: A systematic review and meta-analysis. Am J Emerg Med. 2016;34.
6. Krul M, van der Wouden J,C., van Suijlekom-Smit LW, Koes BW. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database Syst Rev. 2009:CD007759.
7. Krul M, van der Wouden JC, van Suijlekom-Smit LW, Koes BW. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database Syst Rev. 2012.
8. Krul M. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database of Systematic Reviews. 2017.
Category: Pediatrics
Keywords: Infant fever, lumbar puncture, risks, ultrasound (PubMed Search)
Posted: 4/20/2018 by Jenny Guyther, MD
(Updated: 5/2/2026)
Click here to contact Jenny Guyther, MD
Unsuccessful lumbar punctures (LP) may lead to epidural hematoma (EH) formation at the site of needle insertion which may affect subsequent attempts and lead to no success or a grossly bloody sample. There is no standard definition of a traumatic LP based on CSF red blood cell counts. Gross blood may also be obtained by interrupting the vascular structures outside the spinal canal which would not result in EH formation.
This was a prospective study of children younger than 6 months who had an LP at a single children’s hospital. Post LP ultrasounds were completed by the investigating team and interpreted by a pediatric radiologist. 74 patients were included in the study. 31% of the patients had evidence of a post LP EH. 17% fully effaced the thecal sac which would likely preclude future success at that anatomic site. 25% of patients where the clinician did not feel there was a traumatic attempt had evidence of an EH.The study was not powered to determine the risk factors for EH formation. The study also did not look at any other consequences to EH.
Key points: Point of care ultrasound to evaluate EH and bleeding at the failed LP site my provide useful information for a location of subsequent attempts. Also US to evaluate for bleeding in the spinal canal may help with interpretation of the CSF when a large number of red blood cells are present.
Kusulas MP, Eutsler EP, DePiero AD. Bedside Ultrasound for the Evaluation of Epidural Hematoma After Infant Lumbar Puncture. Pediatric Emergency Care. Epub ahead of print. Feb 2018.
Category: Pediatrics
Posted: 3/30/2018 by Rose Chasm, MD
(Updated: 5/2/2026)
Click here to contact Rose Chasm, MD
Category: Pediatrics
Keywords: Asthma, pediatrics, fluid (PubMed Search)
Posted: 3/16/2018 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Fluid overload (defined in this study as (fluid input-output)/weight)) is associated with longer hospital stays, longer treatment duration and oxygen use.
Bottom line: Treat dehydration appropriately but try not to over resuscitate the asthmatic. Further studies are needed before definitive recommendations are made.
This was a retrospective cohort study over 7 years at a single children’s hospital. Children included were older than 6 years and were admitted with no pneumonia or history of chronic lung disease. Fluid intake and output were collected for the initial 72 hours of hospitalization or discharge. The study included 1175 encounters. On average, 1% increase in fluid overload was associated with about a 7 hour increase in hospital stay, 6 hours longer of beta agonist and 2 hours longer of supplemental oxygen. Fluid overload of more than 7% was determined to be clinically meaningful showing an increased risk of requiring supplemental oxygen and non-invasive pressure ventilation. One of the limitations of this study that the authors mention is that the weight they used is the admission weight and the patient may already be dehydrated, thereby overestimating fluid overload.
Kantor et al. Fluid balance is Associated with Clinical Outcomes and Extravascular Lung Water in Children with Acute Asthma Exacerbation. American Journal of Respiratory and Critical Care Medicine. Epub ahead of print, Jan 9, 2018.
Category: Pediatrics
Keywords: foreign body, choking (PubMed Search)
Posted: 2/16/2018 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Patient: 11 month old with trouble breathing and color change after a family member sprayed air freshener. Symptoms have since resolved.
What are you concerned about in the attached xrays?
Answer: Radiolucent foreign body
Bilateral decubitus lateral films allow assessment of air trapping. The expectation is that the dependent lung will collapse partially in the normal patient. When a foreign body is present, there will be air trapping and hyperlucency in the dependent lung. In older patients, you can also obtain expiratory films to look for air trapping.
The patient had a food/mucus plug that was taken out of the right mainstem on bronchoscopy.
Foreign body aspiration is the 4th most common cause of accidental death in children younger than 3 years. Coughing and choking are the most common presenting symptoms.
CXRs are negative in > 50% of tracheal foreign bodies and 25% of bronchial foreign bodies.
More than 75% of foreign bodies in children less than 3 years are radiolucent.
Indirect signs of radiolucent foreign bodies include unilateral hyperinflation, atelectasis, consolidation and bronchiectasis (if presentation is delayed).
Bottom line: Consider bilateral lateral decubitus xrays in patients with a history concerning for foreign body.
Baram et al. Trachoebronchial Foreign Bodies in Children: The Role of Emergency Rigid Bronchoscopy. Global Pediatric Health. 2017: 1-5.
Category: Pediatrics
Keywords: Kawasaki's disease, SJS, TEN, dermatitis (PubMed Search)
Posted: 2/9/2018 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Case: 5 year old presents to the ED with 2 weeks of fever. She has extensive cracked, bleeding lips and a rash on her hands and feet. She was recently diagnosed with “walking pneumonia” and hand, foot and mouth disease this week. Her pediatrician sent her in for further workup after she was found to have an elevated CRP on outpatient labs. A similar picture appears in the link below:
What's the diagnosis?
The diagnosis of Mycoplasma pneumonia-induced rash and mucositis (MIRM) was recently termed in the 2015 Journal of American Academy of Dermatology. It is characterized by mucocutaneous eruptions with prominent mucosal involvement. 94% of patients in the reviewed cases had extensive oral lesions that can range from erosions, ulcers or vesiculobullous lesions. 82% of patients had ocular involvement characterized by purulent bilateral conjunctivitis. In 63% of cases, patients were found to have urogenital lesions. Almost all of these patients had prodromal symptoms of cough and fever preceding the eruption by 1 week. The disease was found to be most prominent with young (11.9 ± 8.8 years) and with a 66% male predominance. The treatment is antibiotics such as azithromycin and oral corticosteroids with a minority of patients requiring IVIG. These patients have a good prognosis.
Bottom Line: Consider MIRM in patients with extensive mucosal disease that do not completely fit the criteria of Kawasaki’s or Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis.
Reference:
Canavan TN, Mathes EF, Frieden I, Shinkai K. Mycoplasma pneumoniae-induced rash and mucositis as a syndrome distinct from Stevens-Johnson syndrome and erythema multiforme: a systematic review. J Am Acad Dermatol. 2015
Feb;72(2):239-45.
Category: Pediatrics
Keywords: Pediatrics, Abdominal Pain (PubMed Search)
Posted: 2/2/2018 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
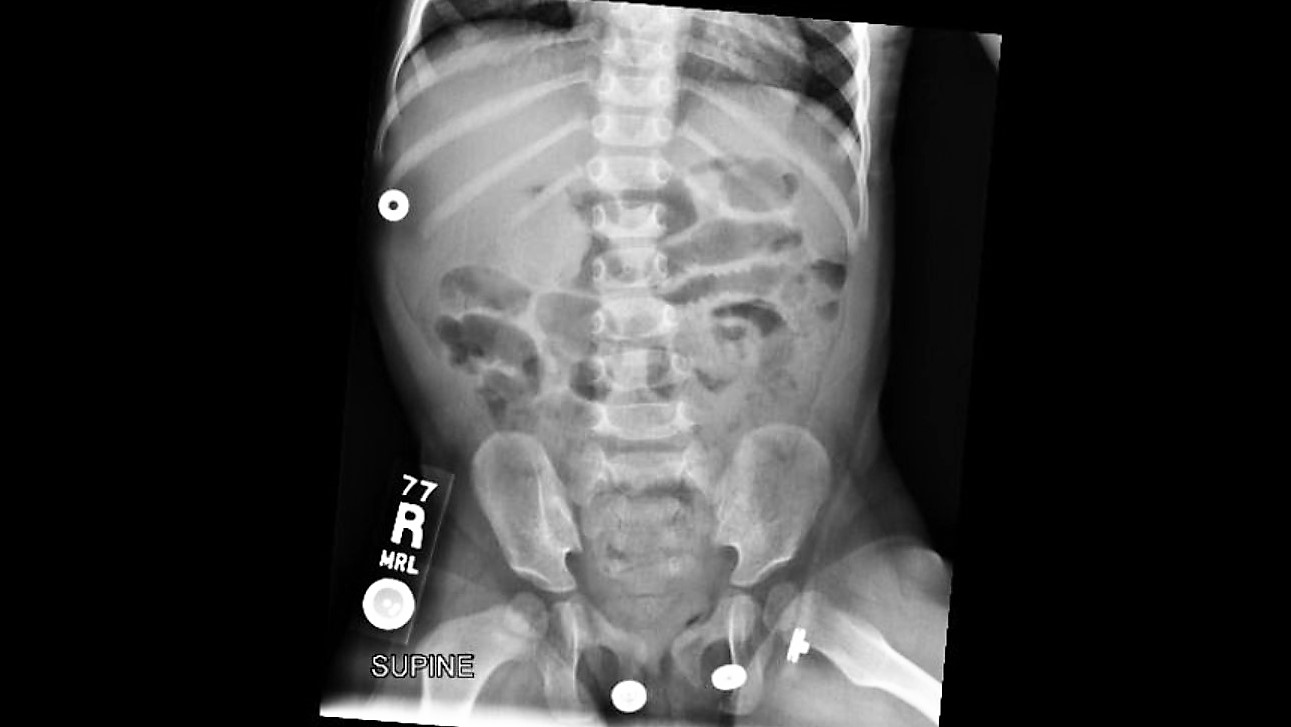 Your patient is an18 months old female with intermittent abdominal pain for the last 4-5 days. She has history of constipation and soy allergy, seen at an outside hospital three days ago for the same. She had an xray and was discharged home with instructions for at home clean out with diagnosis of constipation.
Your patient is an18 months old female with intermittent abdominal pain for the last 4-5 days. She has history of constipation and soy allergy, seen at an outside hospital three days ago for the same. She had an xray and was discharged home with instructions for at home clean out with diagnosis of constipation.
Mother is bringing her to your ED because the pain is back. The laxatives helped somewhat, but her symptoms have returned. She reports that the patient cries spontaneously, lasting 1-2 minutes, then completely resolves. These episodes happen at multiple times during the day.
ROS: Decreased appetite and energy, but NO fevers, vomiting, diarrhea, bloody stool, abdominal distension, hematuria, or lethargy.
Intussusception classically presents with colicky abdominal pain, palpable mass, and currant jelly stools, but in less than 50% of patients. The clinical presentation of intussusception actually occurs on a spectrum. Children who present early in their course may look well with intermittent, unexplained crying episodes, while others may be febrile, dehydrated, with bloody stools, and be septic. The diagnosis can be missed in up to 60% of children presenting for initial evaluation. Identified risk factors include any syndrome or abnormality causing a lead point, ie Meckel's Diverticulum, Familial Polyposis, lymphoma and Henoch-Scholein Purpura, as well as GI infections, bacterial and viral, (Adenovirus, Rotavirus, and HHV6, etc.)
On exam, our patient's abdomen was soft but hard to evaluate due to behavior. Flat plate AXR demonstrated a circular hyperdensity in the RUQ, which on ultrasound, corresponded to a large ileocolic intussusception. She was successfully treated with air enema reduction, which in recent review has the lowest recurrence rate of intussusception.
Bottom Line -
In children with intermittent abdominal pain or unexplained crying episodes, consider intussusception on your differential, as more than half are missed on initial presentation, which can be subtle. Late presentations can include bowel perforation, peritonitis, sepsis, and shock. If diagnosed, arrange for enema reduction or transfer to a facility with this capability.
References:
Waseem M, Rosenberg HK. Intussusception. Pedi Emer Care. Nov 2008, 24(11): 793-800.
Gluckman S, Karpelowsky J, Webster AC, McGee RG. Management for intussusception in children. Cochrane Review of Systematic Databases. 2017; Issue 6.
Category: Pediatrics
Keywords: Pain control in children, opiates, NSAIDS, motrin, orthopedic (PubMed Search)
Posted: 1/19/2018 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Bottom line: Oral morphine was not superior to ibuprofen and both drugs decreased pain with no difference in efficacy. Morphine was associated with more adverse events.
Poonai et al. Oral Morphine versus ibuprofen administered at home for postoperative orthopedic pain in children: a randomized controlled trial. CMAJ 2017. 189: E1252-E1258.
Category: Pediatrics
Posted: 1/12/2018 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: NAT, non-accidental trauma, abusive head trauma, intra-abdominal injury, burns (PubMed Search)
Posted: 1/6/2018 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
In addition to suspicion of NAT with traumatic brain injury and burns, remember these other high risk injuries and features:
- Duodenal injuries in children <4 y/o
- Frena injuries in non-ambulating children
- Proximal and midshaft humeral fractures > supracondylar fractures
- Any bruising on the trunk, ears, neck, or with larger size or pattern
- Delay in seeking care, inconsistent history, mechanism inconsistent with developmental age, and blame of a sibling or other child inflicting harm are all historical features also high risk.
Non-accidental trauma (NAT) continues to be a sad, but prevelant pathology in the United States. It is estimated that one million children in the US have been victims of maltreatment. As high as one third of children with NAT had the abuse missed on prior medical evaluation. There are several screening tools and clinical prediction rules that have been developed for clinical use, but none are to be used as substitutes for full skeletal survey and CT scan when indicated.
TEN-4 (clinical prediction rule): 97% sensitivity, 84% specificity with regards to NAT in the setting of bruising by age, location and characteristic.
PEDIBIRN (clinical prediction rule): 96% sensitive, 43% specificity with regards to abusive head trauma in children less than 3 years old.
PredAHT (clinical prediction rule): 72% sensitive, 86% specificity, also for abusive head trauma less than 3 years old.
PIBIS (screening tool): scoring system for well appearing infants presenting with brief resolved unexplained event (BRUE), previously called apparent life threatening event or ALTE.
Escobar, MA, et al. The association of nonaccidental trauma with historical factors, examination findings, and diagnostic testing during the initial trauma evaluation. Journal Trauma Acute Care Surgery. 2017; 82(6).
Category: Pediatrics
Posted: 12/29/2017 by Rose Chasm, MD
(Updated: 5/2/2026)
Click here to contact Rose Chasm, MD
Children less than 8 years, and especially infants, are more susceptible to upper cervical spine injury. Moreover, validated decision rules for suspected cervical spine injury imaging have not been proven to be as sensitive or specific for children less than 8 years of age.
The pediatric cervical spine has greater elasticity of the ligamentous structures, while the cartilaginous structures are less calcified. An infant's neck musculature is underdeveloped, with a disproportionally large head. These factors increase the risk of cervical spine injury, and can make it difficult to properly place protective cervical collars in infants while assessing them for injury.
In very young children, consider placing padding under the shoulders to prevent abnormal flexion that can occur with placement of a cervical collar, and consider having a lower threshold to image if mechanism history or exam is concerning.
Children are not little adults! Clinicians must acknowledge the anatomic differences, varying age-related ability to cooperate with examination, pediatric specific injury mechanisms, and decreased reliability of validated decision rules for imaging in children, especially when younger than 8 years old.
Murray BL, Cordle RJ: Pediatric Trauma, in Walls RM, Hockberger RS, Gausche-Hill M, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 9. Philadelphia, Elsevier 2018, (Ch) 165:p 2042-2057.
Leonard JR, Jaffe DM, Kuppermann N, et al. Cervical spine injury patterns in children. Pediatrics 2014; 133:e1179.
Category: Pediatrics
Keywords: Croup, epinephrine, discharge, observation (PubMed Search)
Posted: 12/15/2017 by Jenny Guyther, MD
(Updated: 5/2/2026)
Click here to contact Jenny Guyther, MD
The peak age for croup is 6 months to 3 years. The cornerstone of treatment is corticosteroids, traditionally dexamethasone. With oral administration, the peak onset is 1-2 hours. Steroids shorten the duration of symptoms, reduce the need for nebulized epinephrine and decrease the need for intubation.
Racemic epinephrine has been used for moderate to severe croup and can show an improvement in patient symptoms for up to 120 minutes. There is little evidence to suggest how long to observe the patient for recurrence of symptoms after racemic epinephrine was given. Previous studies have suggested both 2 and 4 hour observation.
299 patients were included in this study. 136 patients were observed for 3.1 to 4 hours. In the 3.1 to 4 hour group, 21 (7%) failed treatment, 19 of those patients required admission and 2 returned within 24 hours. No patients who were discharged home after 4 hours returned to the emergency department within 24 hours.
Bottom Line: Consider a 4 hour period of observation after giving racemic epinephrine in order to decrease bounce backs.
Smith S, Giordano K, Thompson A and DePiero A. Failure of Outpatient Management With Different Observation Times After Racemic Epinephrine for Croup. Clinical Pediatrics. Epub ahead of print. Accessed October 2017.
Category: Pediatrics
Keywords: URI, AOM, wait-and-see, antibiotic stewardship (PubMed Search)
Posted: 11/24/2017 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
As we are approaching the winter in the northern hemisphere, the number of visits for ear pain or respiratory symptoms are expected to increase. The occurrence of acute otitis media (AOM) will also increase, but are these two disease processes related?
Drs. Heikkinen and Chonmaitree published a systematic review of previously reported studies regarding the correlation of these two disease processes (1). As far back as 1990, studies have shown that up to 94% of pediatric patients diagnosed with AOM have concomitant upper respiratory infection (URI) type symptoms at time of diagnosis (2). The viral infections most commonly associated with AOM are respiratory syncytial virus, influenza virus, and adenovirus (3).
The most commonly taught risk factors for developing AOM include young age, male gender, multiple siblings, day care attendance, and passive smoking. These factors are also related to the development of upper respiratory symptoms, and the development of AOM should be thought of as a complication of the upper respiratory infection (4).
Koivunen et al noted the highest incidence of AOM at day 3 after the onset of an URI, and the median time to diagnosis was day 4 (5). If you see a patient in day 2-4 of an URI, who has started to develop an ear effusion, but not clinical AOM, you may want to consider a “Wait-to-see” treatment option if the patient meets treatment criteria (https://em.umaryland.edu/
(1) Heikkinen T, Chonmaitree T. Importance of Respiratory Viruses in Acute Otitis Media. Clinical Microbiology Reviews. 2003;16(2):230-241.
Category: Pediatrics
Keywords: Marijuana, symptoms, overdose (PubMed Search)
Posted: 11/17/2017 by Jenny Guyther, MD
(Updated: 5/2/2026)
Click here to contact Jenny Guyther, MD
In the US, there are an estimated 22.2 million users of cannabis based on the 2015 National Survey on Drug Use and Health. The incidence of unintentional cannabis ingestion has increased in states that have legalized medical and recreational marijuana. The cited article reviewed of 44 articles involving unintentional cannabis ingestion in children younger than 12 years.
The majority of intoxications were through cannabis resins followed by cookies and joints.
Lethargy was the most common presenting sign followed by ataxia. Tachycardia, mydriasis and hypotonia were also noted. Rarer but more serious presentations included respiratory depression and seizures.
Richards JR, Smith NE, Moulin AK. Unintentional Cannabis Ingestion in Children: A Systemic Review. The Journal of Pediatrics. 2017. Epub ahead of print.
Category: Pediatrics
Keywords: ARDS, oxygenation index, OI, PALICC, acute lung injury, respiratory distress, PARDS (PubMed Search)
Posted: 10/27/2017 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Some pediatric practitioners have adopted the oxygenation index (OI) ([FiO2 × mean airway pressure (Paw) × 100]/ PaO2) or oxygen saturation index (OSI) ([FiO2 × Paw × 100]/ SpO2) to assess hypoxemia in children instead of P/F ratios because of the less standardized approach to positive pressure ventilation in children relative to adults.
OI can be used in pediatric patients to define severity of Acute Respiratory Distress Syndrome (ARDS) in patients receiving invasive mechanical ventilation and assess for potential ECMO treatment.
In contrast, the P/F ratio should be used to diagnose Pediatric ARDS for patients receiving noninvasive continuous positive airway pressure [CPAP] or bilevel positive airway pressure [BiPAP]) with a minimum CPAP of 5 cm H2O.
Oxygen Index (OI) = FiO2 x MAP x 100
---------------------
PaO2
Category: Pediatrics
Keywords: Vomiting, pediatric, medication (PubMed Search)
Posted: 10/20/2017 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Within the first hour after administration, ondosterone, metoclopramide and bromopride were equally efficacious. At the 6 hour and 24 hour period after receiving the initial dose of medication, ondansetron was statistically superior to bromopride (not available in the US) and metoclopramide. There were no reported side effects in the ondansetron group (including diarrhea or sedation).
This was a randomized control trial of children 1 year to 12 years seen in the pediatric emergency department in Brazil for vomiting and given intramuscular bromopride (0.15mg/kg to a maximum of 10 mg), metoclopramide (0.15mg/kg to a maximum of 10 mg), or ondansetron (0.15mg/kg to a maximum of 8 mg). 175 children were included.
Epifanio et al. Bromopride, metoclopramide, or ondansetron for the treatment of vomiting in the emergency in the pediatric emergency department: a randomized control trial. J Pediatr 2017. Article in Press.
Category: Pediatrics
Keywords: Trauma, hematuria, kidney injury (PubMed Search)
Posted: 10/13/2017 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
