Category: Endocrine
Keywords: DKA (PubMed Search)
Posted: 6/6/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
This single center study looked at diabetic patients who had a POC glucose over 300 and POC ketone over 1.1 and reviewed their diagnosis vs the laboratory accepted diagnosis of DKA.
“The most recent international consensus laboratory definition of (non-euglycemic) DKA includes a glucose of >?250; a pH <?7.3 or a bicarbonate ??18?mmol/L; and a beta-hydroxybutyrate (BOHB) ??3.0?mmol/L or urine ketone strip ??2+”
They found that 53% met the laboratory definition of DKA.
Of the remainder:
“Of 740 screening positive by POC testing whose initial labs did not meet DKA criteria, 229 (31%, 95% CI: 28, 34) were diagnosed with DKA. Primary ED diagnoses of the remaining 511 included: hyperglycemia (196, 38%), starvation ketosis (58, 11%), hyperosmotic hyperglycemic state (11, 2%), and other ketosis (9, 2%), while 67 (13%) had a primary diagnosis of infection, 1 (<?1%) metabolic acidosis and 169 (33%) an unrelated diagnosis.”
Their conclusion was EPs diagnose DKA even when lab work doesn’t support the diagnosis as it is a clinical not a lab diagnosis. Most importantly these patients are getting insulin and fluid to correct their underlying metabolic derangement.
R. T.Griffey, N.Haas, R. M.Schneider, et al., “How Often Are Emergency Patients Diagnosed With Diabetic Ketoacidosis Despite Not Meeting Laboratory Criteria?,” Academic Emergency Medicine33, no. 5 (2026): e70315, https://doi.org/10.1111/acem.70315.
Category: Trauma
Keywords: spinal injury, concurrent injury (PubMed Search)
Posted: 6/4/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
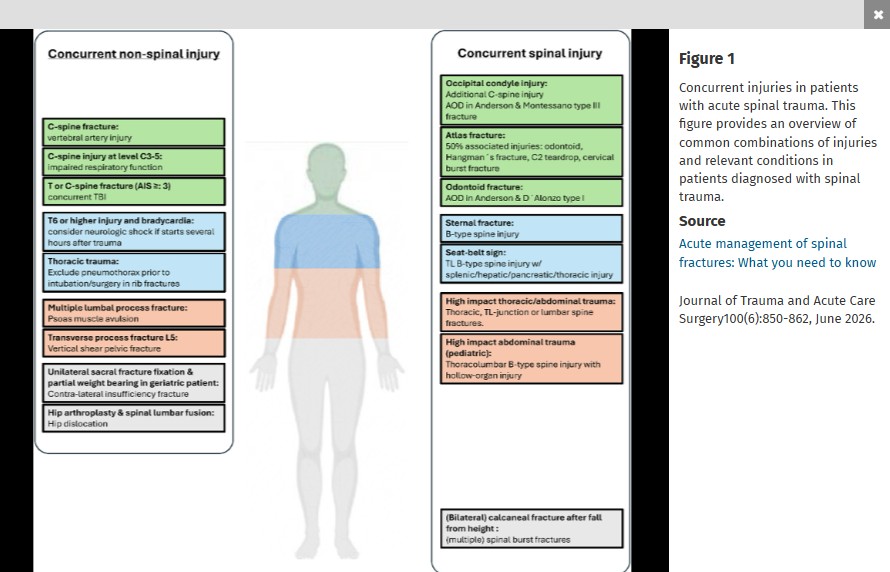
This nice review article reminds us “The AO-Spine classification is the most frequently utilized system for thoracic and lumbar fractures, and it categorizes fractures into three types. Type A fractures are compression injuries. In these fractures, the assessment of the involvement of the posterior elements of the vertebral body is essential. Type B fractures are distraction injuries implying tension band involvement, whereas type C fractures are translational or dislocated injuries. The AO-Spine Upper Cervical Injury Classification System… In this classification system, type A injuries have no ligamentous involvement and are considered stable. Type B injuries have tension band or ligamentous injury and may be unstable. Type C injuries are characterized by significant translation and loss of anatomic integrity and are considered unstable."
Category: Toxicology
Keywords: Anticholinergic poisoning, antimuscarinic toxicity, jimson seeds, rivastigmine (PubMed Search)
Posted: 6/3/2026 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
A 22 year old normally healthy male presents with tachycardia (HR 140), dilated pupils (7 mm), dry flushed hot skin, and confusion/agitation. His mother states he has a 1 day history of “talking out of his head not making sense”, “seeing things that aren’t there”, and “speaking to video game characters”. He has suprapubic tenderness with markedly distended bladder on exam revealing over 1 liter of urine on bladder scan. She found a small bottle containing a large amount of small 2-3 mm black seeds in his room and suspects he ingested them. What treatment options would you consider?

This patient is exhibiting symptoms and signs consistent with muscarinic receptor blockade (aka anticholinergic toxicity) characterized by confusion, tachycardia, mydriasis, dry flushed skin, hyperthermia, and urinary retention. The small black seeds are jimson seeds from Datura stramonium (devil’s trumpet, thorn apple) and contain atropine, hyoscyamine and scopolamine in highest concentration and are used as a recreational drug for hallucinogenic effects.
Treatment options include gastric decontamination with activated charcoal and whole bowel irrigation to limit ongoing GI absorption. These small seeds are usually ingested in abundance and lodge throughout the GI tract and have variable and prolonged absorption which can cause resurgence of symptoms. After ingestion, anticholinergic effects are seen within 30-60 minutes with effects lasting up to 24-48 hours.
Benzodiazepines are often used as first line treatment for anticholinergic-induced CNS agitation. However repeat doses are often necessary leading to undesired effects including loss of airway protection, aspiration, and respiratory depression. In one retrospective study, benzodiazepines were shown not only to be less effective than true antidotal therapy but have higher complication rate. Antidotal treatment with reversible acetylcholinesterase inhibitor drugs provide safe and effective targeted therapy reversing both central and peripheral muscarinic effects and are indicated in cases of severe anticholinergic poisoning (intractable agitation, tachycardia, and hyperthermia).
Unfortunately, intravenous physostigmine (Antilirium) which was traditionally used has not been produced in the U.S. since February 2023 leading to this drug shortage. Alternatively, restricted use imported physostigmine (Anticholium) and rivastigmine (Exelon), a long-acting well tolerated acetylcholine inhibitor used for Alzheimer disease and Parkinsonism, have been utilized with good success in several reports of diphenhydramine overdose cases.
Rivastigmine is available only in oral and transdermal forms. Although, not as fast acting as IV physostigmine, it’s tertiary amine structure enables passage across the blood brain barrier. Several reported cases and small studies show effectiveness and safety of rivastigmine for anticholinergic poisoning. The recommended oral dose of rivastigmine is 3-6 mg every hour until resolution of symptoms (max 12 mg/day) and/or transdermal Patch 9.5-13.3 mg.
Rivastigmine as an alternative treatment for anticholinergic toxidrome in light of the physostigmine shortage: A case series. Berg M, Strand A, et al. Am J Emerg Med. 2025 Aug;94:144-147. doi: 10.1016/j.ajem.2025.04.047. Epub 2025 Apr 22. PMID: 40288328.
Rivastigmine for the management of anticholinergic delirium. Chiew AL, Holford AG, et al. Clin Toxicol (Phila). 2024 Feb;62(2):82-87. doi: 10.1080/15563650.2024.2319854. Epub 2024 Mar 11. PMID: 38465631.
Transdermal rivastigmine as a therapeutic option in severe diphenhydramine-induced anticholinergic toxicity: A case report and literature review. Gilbert BW, Santiago RD, et al. Pharmacotherapy. 2025 Jul;45(7):462-467. doi: 10.1002/phar.70031. Epub 2025 Jun 10. PMID: 40492363.
A comparison of physostigmine and benzodiazepines for the treatment of anticholinergic poisoning. Burns MJ, Linden CH, Graudins A, Brown RM, Fletcher KE. Ann Emerg Med. 2000;35:374–381. doi: 10.1016/S0196-0644(00)70057-6.
Category: Ultrasound
Keywords: cardiology; pocus; mitral regurgitation (PubMed Search)
Posted: 6/1/2026 by Alexis Salerno Rubeling, MD
Click here to contact Alexis Salerno Rubeling, MD
Do you have a patient with shortness of breath and pulmonary edema?
Don’t forget to place the color doppler over the mitral valve to look for acute mitral regurgitation.
Acute mitral regurgitation can be missed on initial evaluation or misdiagnosed as a primary pulmonary process because patients often present with severe dyspnea, an abnormal chest x-ray, or an absence of an audible murmur. Classically, these patients develop acute heart failure due to a rapid rise in left atrial pressure leading to pulmonary congestion. The abrupt reduction in forward stroke volume may also result in hypotension and cardiogenic shock.
When evaluating a patient with acute dyspnea, remember to apply color Doppler over the mitral valve, such as in the apical 4 chamber view, to assess for severe mitral regurgitation. In the image below, notice the backward flow of color into the left atrium.

Watanabe N. Acute mitral regurgitation. Heart. 2019 May;105(9):671-677. doi: 10.1136/heartjnl-2018-313373. Epub 2019 Mar 1. PMID: 30824479.
Category: Trauma
Keywords: Diamond minutes, bystander (PubMed Search)
Posted: 5/31/2026 by Robert Flint, MD
(Updated: 6/6/2026)
Click here to contact Robert Flint, MD
These authors argue that bystander interventions in the early minutes (they call them the diamond minutes) can have an impact on trauma survival. Particular attention to External hemorrhage control; Airway opening and maintenance; Safe positioning of unconscious patients; Mitigation of early hypoxia and hypothermia could improve survival. We need to publicize this information and undo the years of teaching not to move these patients due to concern of secondary spinal cord injury. Many studies have dispelled that concern.

Imbriaco, G., D’Arrigo, S., Limonti, F. et al. The diamond minutes: rethinking the earliest link of the trauma chain of survival. Scand J Trauma Resusc Emerg Med 34, 79 (2026). https://doi.org/10.1186/s13049-026-01611-7
Category: Trauma
Keywords: Freeze dried plasma (PubMed Search)
Posted: 5/30/2026 by Robert Flint, MD
(Updated: 6/6/2026)
Click here to contact Robert Flint, MD
This article suggest that freeze-dried plasma (FDP) is an acceptable adjunct to whole blood for prehospital resuscitation of trauma patients. “FDP is pathogen-reduced, shelf-stable for up to two years at room temperature, lightweight, and rapidly reconstituted at the point of care.” This method offers an advantage when caring for patients in remote areas with long transport times and has been used by NATO and Canadian armed forces.
Peddle, M., Trojanowski, J. & Nolan, B. The role of freeze-dried plasma in a world of whole blood: a Canadian prehospital and transport perspective. Scand J Trauma Resusc Emerg Med 34 (Suppl 1), (2026). https://doi.org/10.1186/s13049-026-01629-x
Category: Trauma
Keywords: Head injury delayed injury (PubMed Search)
Posted: 5/28/2026 by Robert Flint, MD
(Updated: 6/6/2026)
Click here to contact Robert Flint, MD
Of the 215 Norwegian patients on oral anticoagulation seen for a head injury and having a normal initial head CT, none developed delayed hemorrhage. Median age was 83 years.
Bahr, M.A., Visnes, H. & Brommeland, T. No delayed intracranial hemorrhage in head injury patients on oral anticoagulants and with normal CT: a retrospective study of 215 patients. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01617-1
Category: Administration
Keywords: Metrics, LWBS, Quality, (PubMed Search)
Posted: 5/27/2026 by Mercedes Torres, MD
Click here to contact Mercedes Torres, MD
A recently published commentary highlights the importance of looking beyond the numbers and remembering the core mission of emergency practice. It warns against “gaming” the system to create processes that give better metrics using the example of rates of patients who leave without being seen (LWBS). In the author’s words, efforts aimed at improving this metric create strategies that “raise concerns about distributive justice, beneficence, and professional integrity.” See link for key take home points.
Key points from this commentary:
N.Chhabra, “When Metrics Replace Values: Ethical Concerns in Healthcare Performance Measures,” Academic Emergency Medicine. 33, no. 5 (2026): e70330, https://doi.org/10.1111/acem.70330.
Category: Critical Care
Keywords: Bicarbonate, metabolic acidosis (PubMed Search)
Posted: 5/26/2026 by Quincy Tran, MD, PhD
Click here to contact Quincy Tran, MD, PhD
Sodium bicarbonate significantly reduced the need of renal replacement therapy (risk ratio [RR] 0.69; 95% CI, 0.61–0.78) but not mortality (RR, 0.84; 95% CI, 0.55–1.30). However, there was not enough sample size to support the outcome of mortality.
There was still significant heterogeneity between studies as the sources of metabolic acidosis were different between different studies in this meta-analysis study of randomized control trial. One study recruited patients with septic shock only, while other studies enrolled patients with different disease states.
There was also heterogeneity in the threshold for pH to enter the study.
Sodium Bicarbonate for Acute Metabolic Acidosis in Critically Ill Adults: A Meta-Analysis of Randomized Clinical Trials. Chen, Jia-Jin MD; Lee, Tao-Han MD; Chang, Chih-Hsiang MD, PhD, Lai, Pei-Chun MD, PhD; Tu, Yu-Kang PhD; Huang, Yen-Ta MD, MSc, PhD. Critical Care Medicine ():10.1097/CCM.0000000000007179, May 22, 2026. | DOI: 10.1097/CCM.0000000000007179
Category: Infectious Disease
Keywords: Bacteremia, Bandemia, Mortality (PubMed Search)
Posted: 5/21/2026 by Lena Carleton, MD
(Updated: 5/25/2026)
Click here to contact Lena Carleton, MD
Bottom Line: In adults presenting to the ED with bacteremia, bandemia may be associated with increased short-term mortality, with higher band percentages correlating with greater risk. Although bacteremia is rarely diagnosed during the ED visit because blood cultures require time to result, the presence of bandemia should raise concern for possible occult critical illness.
Bandemia refers to an elevated number of banded (immature) neutrophils in the peripheral blood, reflecting bone marrow stimulation in response to infection. In this study, the authors evaluated the association between bandemia and short-term mortality.
This single-center retrospective cohort study was conducted in Taiwan from 2018 to 2023. The authors screened all ED encounters in which blood cultures were obtained. Eligible participants were treatment-naive adults with confirmed bacterial growth in blood cultures collected during the ED stay. Patients were excluded if blood cultures were deemed contaminants or if they had received antibiotics prior to ED presentation.
A total of 5,558 patients were included, with an overall 30-day mortality rate of 16.1%. Patients were stratified by band percentage: <10%, 10–19%, 20–29%, 30–39%, and ?40%. Each 10% increase in initial band percentage was independently associated with a 12% increase in 30-day mortality.
Bottom Line: In adults presenting to the ED with bacteremia, bandemia may be associated with increased short-term mortality, with higher band percentages correlating with greater risk. Although bacteremia is rarely diagnosed during the ED visit because blood cultures require time to result, the presence of bandemia should raise concern for possible occult critical illness.
Cheng H, et al. Association between initial bandemia degree and short-term mortality among adults with bacteremia in the emergency department. Am J Emerg Med. 2026;103. doi:10.1016/j.ajem.2026.05.008
Category: Trauma
Keywords: Central cord (PubMed Search)
Posted: 5/24/2026 by Robert Flint, MD
(Updated: 6/6/2026)
Click here to contact Robert Flint, MD
Category: Orthopedics
Posted: 5/23/2026 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
20yo college swimmer presents to the ED with a constellation of non-specific symptoms such as poor sleep, fatigue, depression/anxiety, weight loss.
Despite regular 2/day practices, his coach tells him his performance is worse than ever.
Overtraining syndrome
A maladaptive response to excessive exercise without adequate functional rest
-Results in disturbances of multiple body systems (neurologic, endocrinologic, immunologic and psychologic) which causes a broad constellation of symptoms
- May be caused by systemic inflammation and resultant neurohormonal changes (hypothalamic-pituitary-adrenal axis)
- Multiple hypotheses exist
The ACSM 2025 consensus statement on the adolescent athlete highlights that overtraining risk is particularly elevated in those who specialize in a single sport early, train more hours per week than their age, or maintain a >2:1 ratio of organized sport to free play.
Symptoms
The ACSM/AMSSM consensus statement categorizes these into physical and psychosocial domains:
Physical symptoms:
Psychosocial symptoms:
Decreased maximal heart rate during exercise testing (-3.6 to -7.5 bpm) is the most consistent cardiovascular finding
ED workup may include: CBC, CMP, iron studies, TSH, CK.
The only treatment is reduction in training combined with optimized nutrition, increased sleep, and stress reduction. Subsequent improvement in symptoms and performance confirms the diagnosis but may take months depending on the severity and duration of maladaptation.
Category: EMS
Keywords: HEMS, pediatric trauma (PubMed Search)
Posted: 5/15/2026 by Jenny Guyther, MD
(Updated: 5/21/2026)
Click here to contact Jenny Guyther, MD
Previous pediatric studies have shown that 1) air transport has shown improved outcomes compared to matched ground transports but 2) air transport may be overutilized.
This was a multicenter retrospective study using the Pediatric Emergency Care Applied Research Network Registry from 2012-2021 looking at pediatric patients transported to the ED by helicopter. This registry does not differentiate between field transports and interfacility transfers. The study looked to identify patients who were discharged from the ED or had a hospital stay < 48 hours. 7722 patients were included with a median age of 5.9 years. 20% of these patients were discharged from the ED. Among those admitted, over half were discharged within 48 hours. Patients who were discharged from the ED were found to have triage < ESI 1, missing a systolic blood pressure or temperature. Tachycardia, tachypnea, hypertension and abnormal temperature were associated with a lower rate of ED discharge.
Bottom line: Additional research is needed to identify patients who may be more appropriate for ground transport or when transport is not needed (or could be replaced with telemedicine).
Naik V, Bhardwaj P, Ramgopal S. Rapid Discharge Following Air Transport in Children. Prehosp Emerg Care. 2025 Jul 23:1-8. doi: 10.1080/10903127.2025.2531074. Epub ahead of print. PMID: 40643375.
Category: Critical Care
Keywords: Pulmonary embolism, massive PE, submassive PE, RV failure, cardiogenic shock, guidelines (PubMed Search)
Posted: 5/19/2026 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Not all patients with an acute PE will be crashing and critically ill, but it seemed worthwhile to remind everyone that there are new guidelines and recommendations from AHA/ACC/ACCP/ACEP/CHEST/SCAI/SHM/SIR/SVM/SVN/XYZLMNOP about the management of patients with acute pulmonary embolism in the 2026 AHA/ACC Joint Committee statement. A few key takeaways, with highlights for the sicker PE patients:
Highlights for the sicker PE patients, i.e. Categories C+:
For a great breakdown and further discussion of the new guidelines, I recommend checking out the Life in the Fast Lane blogpost here.


Creager MA et al. 2026 AHA/ACC/ACCP/ACEP/CHEST/SCAI/SHM/SIR/SVM/SVN Guideline for the Evaluation and Management of Acute Pulmonary Embolism in Adults: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2026 Mar 24;153(12):e977-e1051.
Category: Administration
Posted: 5/13/2026 by Kevin Semelrath, MD
(Updated: 5/17/2026)
Click here to contact Kevin Semelrath, MD
This is a small qualitative study that focused on barriers to care and how to overcome them when dealing with patients with dementia, who are primarily Spanish speaking. The authors found to big themes that patients and caretakers thought would improve their care:
1- use of a certified translator, either telephonically or in person, eased social dynamics in communication
2- those same translators tended to only be used in an episodic manner- during HPI, exlaining results or discharge planning. But the patients and caretakers would prefer to have access to them in the “in between” periods so that it would be a more patient centered experience
A. N.Chary, V.Lara, S.Yoon, et al., “Communicating Across Languages: Experiences of Spanish-Speaking People With Dementia and Care Partners in the Emergency Department,” Academic Emergency Medicine33, no. 3 (2026): e70198, https://doi.org/10.1111/acem.70198.
Category: Trauma
Keywords: Removal, motorcycle helmet (PubMed Search)
Posted: 5/17/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
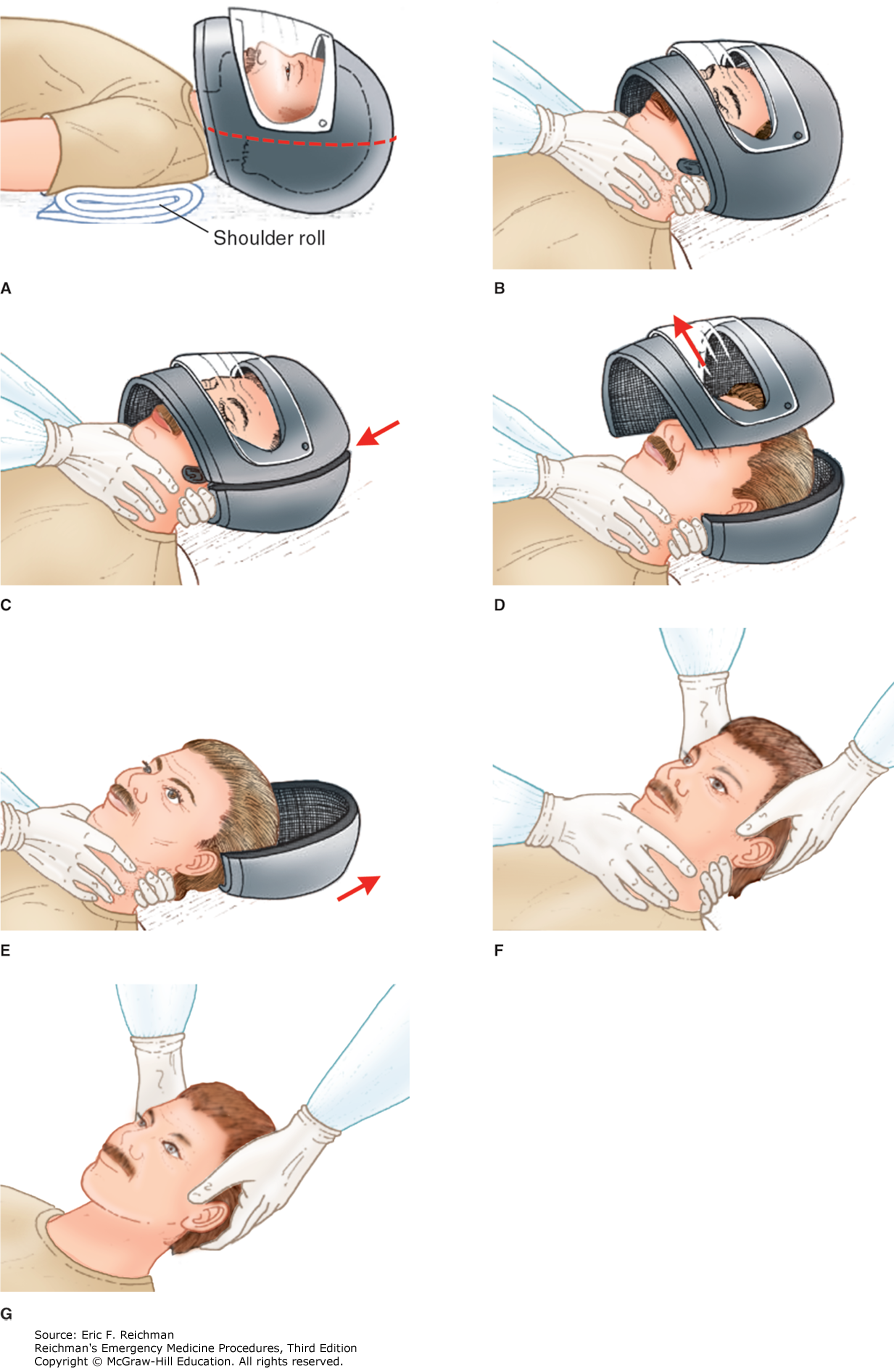
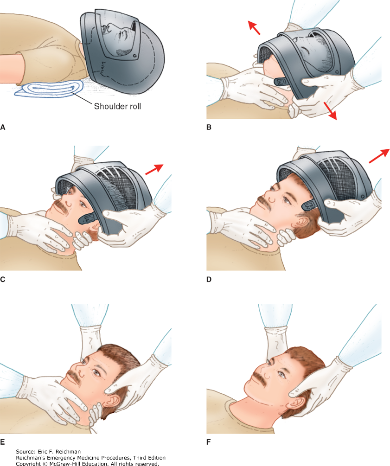
Here are two techniques to remove a helmet from an injured motorcyclist. The first uses a cast saw to bivalve the helmet. A link for a video is also provided.
Category: Pediatrics
Keywords: CPR, ILCOR, PALS, VF, defibrillation (PubMed Search)
Posted: 5/15/2026 by Jenny Guyther, MD
(Updated: 6/6/2026)
Click here to contact Jenny Guyther, MD
US and International guidelines differ on the initial defibrillation dose in pediatric patients. International, European, Australian and New Zealand guidelines had recommend an initial dose of 4 J/kg for the initial and all subsequent doses while the American Heart Association recommends an initial dose of 2-4J/kg (with 2 J/kg in the teaching algorithms) with subsequent shocks being at least at 4J/kg and no greater than 10 J/kg. More recently, ILCOR suggested an initial dose of 2-4 J/kg.
This was a systemic review of 7 observational studies, mostly involving in hospital pediatric cardiac arrests. Outcomes of termination of VF/pVT, ROSC and survival to hospital discharged were examined in relation to the initial J/kg dose that was used compared to initial doses of 2 J/kg. Outcomes were neither better or worse with doses < 1.5 J/kg or > 2.5 J/kg. Additional research is needed as this certainty of this evidence was considered “very low.”
Acworth J, Del Castillo J, Tiwari LK, Atkins D, de Caen A, Bansal A, Couto TB, Katzenschlager S, Kleinman M, Lopez-Herce J, Morgan RW, Myburgh M, Nadkarni V, Tijssen JA, Scholefield BR; International Liaison Committee on Resuscitation Paediatric Life Support Task Force. Energy doses for paediatric defibrillation in cardiac arrest: systematic review and meta-analysis. Resusc Plus. 2025 May 26;24:100991. doi: 10.1016/j.resplu.2025.100991. PMID: 40524976; PMCID: PMC12169708.
Category: Obstetrics & Gynecology
Keywords: contraception, reproductive care (PubMed Search)
Posted: 5/14/2026 by Ashley Martinelli
(Updated: 5/15/2026)
Click here to contact Ashley Martinelli
Access to reproductive care is being limited across the country, and the rate of undesired pregnancies is rising.
Discussing contraception preferences in the Emergency Department can support patients as well as and reduce the morbidity and mortality associated with an undesired pregnancy. Simply asking patients of childbearing age: "Are you interested in discussing pregnancy prevention?" can bridge a gap in access to reliable care. Easy and accessible tools can be used on shift to assist with appropriate initiation.
On Shift Tools:
Contraception Initiation • Clinical Resources • FemInEM
www.bedsider.org -Patient friendly comparisons of contraception options
Quick Start Contraception Care in the ED - Bridge to Treatment - ED oriented flow diagram
Cline L, Downey K, Rashid Y, et al. When Prevention is an Emergency: The Imperative of Contraception Initiation in the Emergency Department. J Emerg Med 2026; 85:177-182.
https://doi.org/10.1016/j.jemermed.2026.02.038.
(https://www.sciencedirect.com/science/article/pii/S0736467926000697)
Category: Gastrointestional
Keywords: Lower GI Bleeding (PubMed Search)
Posted: 5/13/2026 by Neeraja Murali, DO, MPH
Click here to contact Neeraja Murali, DO, MPH
Lower GI bleed is a common reason for ED visits. This study aimed to validate a scoring system to identify low-risk LGIB pts who could be safely discharged from the ED.
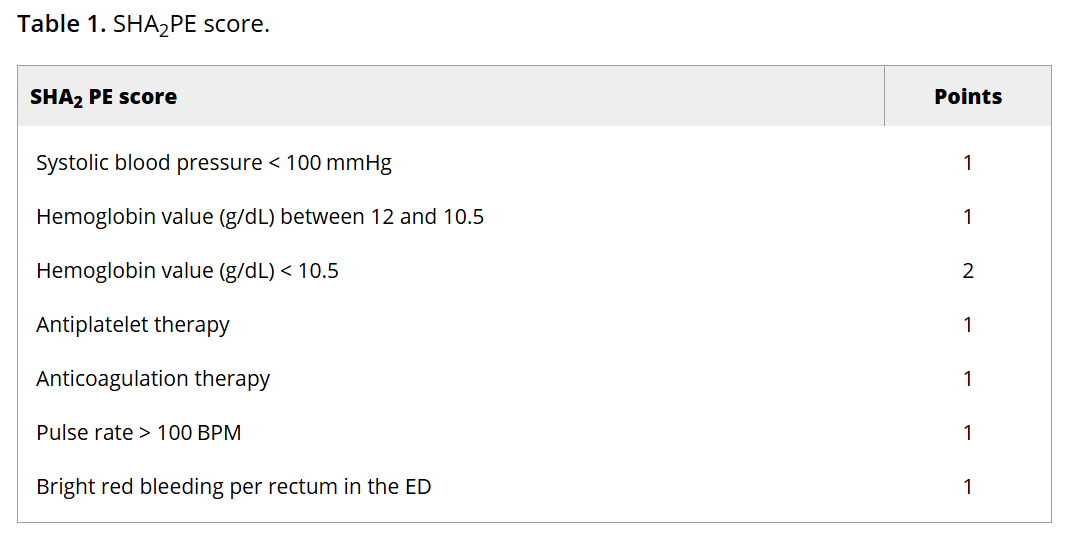
The SHA2PE score incorporates characteristics and data that are commonly collected on patients with this complaint; readers can click through to see the scoring system. A score of less than or equal to 1 helps identify patients suitable for outpatient management, with a NPV of 98.3% (95% CI [97.2-99.1]) for predicting the need for hospitalization and acute intervention. However, the findings should be interpreted with caution given the relatively low prevalence of interventions within the study population.
Ahmad AI, El Sabagh A, Zhang J, et al. External Validation of SHA2PE Score: A Score to Predict Low-Risk Lower Gastrointestinal Bleeding in the Emergency Department. Gastroenterol Res Pract. 2025;2025:5657404. Published 2025 Jan 3. doi:10.1155/grp/5657404
Category: Critical Care
Keywords: ventilator associated pneumonia, intubation, stroke, brain injury, antibiotics (PubMed Search)
Posted: 5/12/2026 by Jessica Downing, MD
Click here to contact Jessica Downing, MD
Should we give a dose of antibiotics after intubating to reduce risk of VAP down the line? A multicenter RCT conducted in 2024 - the PROPHY-VAP Trial - found that a single dose of 2g ceftriaxone administered within 12 hours of intubation reduced VAP within the first week of hospitalization for patients intubated for airway protection due to TBI, stroke or SAH, with a VAP rate of 14% in the CTX group vs 32% in the VAP group (HR 0.60; 95% CI 0.38-0.95).
Click the link below for details and additional discussion
Details:
Background: prior studies have investigated different antibiotic regimens in different groups. In 2023, the AMIKIHAL trial suggested that a 3d course of inhaled amikacin would reduce 28d risk of VAP among patients ventilated for >3d (not just neuro patients). In 2022, the SuDDICU trial suggested that “selective decontamination of the digestive tract” with a combination of IV abx, oral suspension of antibiotics, and topical abx to the oropharynx and buccal mucosa suggested a lower risk of in-hospital mortality in Baysian meta-analysis (though not in the primary study statistics). In 2005, the ANTHARTIC trial suggested a lower rate of VAP with a 2 days course of amoxicillin-clavulanate among patients admitted after OHCA.
Closing Thoughts: Together, these studies suggest that there may be a role for an early and short course of antibiotics for preventing VAP in a few patient populations. A single dose of CTX is easier and more benign than prior suggested regimens, and based on the available data, seems to offer benefit with minimal risk.
Dahyot-Fizelier C, Lasocki S, Kerforne T et al. Ceftriaxone to prevent early ventilator-associated pneumonia in patients with acute brain injury: a multicentre, randomised, double-blind, placebo-controlled, assessor-masked superiority trial. The Lancet Respiratory Medicine, 2024; 12, 375-385
Additional References
