Category: Geriatrics
Keywords: Constipation geriatric complex (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
A narrative review of literature involving older patients and constipation found:
“Major contributing factors include physical inactivity, sarcopenia, dehydration, inappropriate defecation posture, and polypharmacy, particularly opioids and anticholinergic agents. Importantly, these factors interact through the brain–gut–microbiota axis, contributing not only to gastrointestinal dysfunction but also to systemic outcomes such as frailty, cognitive decline, and increased healthcare burden, thereby supporting a multidimensional disease framework.”
It isn’t as simple as adding a laxative.
Mimura S, Morishita A, Kitaoka A, Sasaki K, Tai H, Yano R, Nakahara M, Oura K, Tadokoro T, Fujita K, et al. Constipation in Older Adults: Pathophysiology, Clinical Impact, and Management Strategies. Geriatrics. 2026; 11(2):47. https://doi.org/10.3390/geriatrics11020047
Category: Geriatrics
Keywords: Prescribing cascade (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 4/30/2026)
Click here to contact Robert Flint, MD
The article outlines how instead of looking at medications as the cause of symptoms, we often add more medications to treat the medication induced symptoms. Here is an example of how we get to polypharmacy in older patients
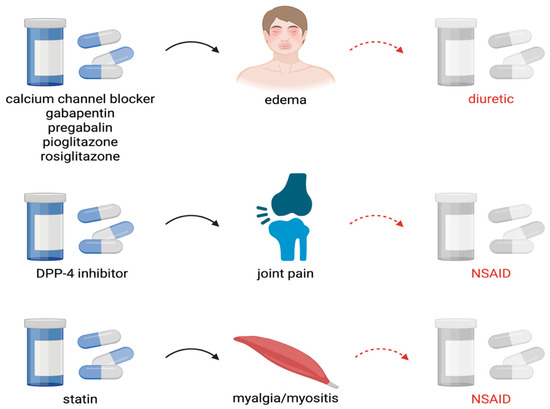
Bry?a A, Woro? J, Miedziaszczyk M, Lorkowska-Zawicka B, Bujak-Gi?ycka B, Orzechowski D, Po?etek P, Pa?ys W. Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity. Geriatrics. 2026; 11(2):37. https://doi.org/10.3390/geriatrics11020037
Category: Trauma
Keywords: Body armor, blunt injury, BABT (PubMed Search)
Posted: 4/26/2026 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
Body armor/ bullet resistant vests used by law enforcement are designed to stop penetration by handgun rounds. These rounds have less velocity than rifle rounds. When caring for someone who has been shot while wearing body armor, verify no penetration has occurred and then look for blunt injuries such as rib fractures, liver injuries, pneumothorax, cardiac contusion, vertebral injury, etc. Behind Armor Blunt Trauma (BABT) is the technical term for injuries caused by the transfer of kinetic energy that occurs when these vests are struck.
Volume 49, Issue 7, July 2018, Pages 1251-1257
Author links open overlay panelRosalind M. Jennings a, Chris Malbon b, Fiona Brock a, Stuart Harrisson c, Debra J. Carr b
Category: Trauma
Keywords: trauma, chronic pain, (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/23/2026)
Click here to contact Robert Flint, MD
This narrative review of the trauma literature looking at chronic pain after trauma found:
Kussé M, Hans G, Saldien V, Wildemeersch D. Chronic pain following major trauma: Prevalence, predictive models, and risk factors across common injury types. Trauma. 2026;0(0). doi:10.1177/14604086251404750
Category: Administration
Posted: 4/21/2026 by Steve Schenkel, MD, MPP
(Updated: 4/22/2026)
Click here to contact Steve Schenkel, MD, MPP
Ambient Artificial Intelligence based scribes that create visit notes based on the conversation in the room during patient evaluation may save documentation time and reduce total time in the health record but may not perform as well as human scribes in some circumstances, at least for pediatric patient charts.
Two side-by-side reports in the May Annals of Emergency Medicine portray related but slightly different pictures of ambient scribing.
Preiksaitis et al found that the offer of an ambient AI scribing system led to some adoption more for lower acuity visits. AI use led to shorter notes, shorter electronic health record time, and about one minute less documentation time per chart. Morey et al compared human and AI scribes and found that human scribes were associated with similar note lengths and metrics for adult patients and somewhat higher quality charts in pediatric patients. An associated editorial argues that AI charting may offer a moment of culture change. (I am one of the authors of the editorial.)
Preiksaitis C, Alvarez A, Winkel M, et al. Ambient Artificial Intelligence Scribe Adoption and Documentation Time in the Emergency Department. Annals of Emergency Medicine, 2026; 87, 569-574.
Morey J, Jones D, Walker L, et al. Ambient Artificial Intelligence Versus Human Scribes in the Emergency Department. Annals of Emergency Medicine, 2025; 87, 561-568.
Schriger D, Schenkel S. Can Ambient Charting Fix Emergency Medicine? Annals of Emergency Medicine, 2026; 87, 575-577.
Category: Critical Care
Keywords: Oxygenation, ARDS, P:F Ratio, S:F Ratio, Hypoxia, Mechanical Ventilation (PubMed Search)
Posted: 4/21/2026 by Mark Sutherland, MD
(Updated: 5/3/2026)
Click here to contact Mark Sutherland, MD
PaO2 to FiO2 (P:F) ratios, are often considered the gold standard in critical care for assessing the degree of oxygen-refractory hypoxia in various pathologies, particularly ARDS. P:F does have some limitations, including not accounting for the PEEP, but probably the most limiting is that it requires collecting an ABG, which is invasive and not always feasible or a top priority when resuscitating a critically ill hypoxic patient. On the other hand, SpO2 (pulse ox saturation) is routinely available, and of course the FiO2 should be known, so many have suggested perhaps using an SpO2 to FiO2 (S:F) ratio instead. But how S:F maps to P:F and how well they correlate is not fully known. Chaudhuri et al recently conducted a meta-analysis, published in Critical Care Medicine this month, which reviewed the literature on this.
Bottom Line: Yes, S:F ratios correlate well with P:F ratios, especially when the SpO2 is less than 97%, but you can't just substitute the S:F for P:F, you have to use one of the accepted formulas. See additional info on the website for the actual formula to apply and how a given S:F translates to P:F.
The authors identified 4 particularly high performing formulas from well-done studies. One was logarithmic, and two were non-linear, making the math hard, so the best is probably the linear one (correlation coefficient was 0.89, which is quite good). It is:
SF = 64 + 0.84 x PF
Usually you have the SF and want to figure out the PF, so rearranging to solve for PF (to save you all the trouble):
PF = (SF - 64) / 0.84
Since we usually care about P:F < 300 (mild ARDS), < 200 (moderate ARDS), and < 100 (severe ARDS), here are the S:F mappings for those P:Fs to make things super simple:
If P:F is 300 then S:F is 315
If P:F is 200 then S:F is 235
If P:F is 100 then S:F is148
And 150 is another P:F that is important since we often consider proning and/or paralysis under this level. That would equate to an S:F of 190 using this formula.
Don't forget! The SpO2 is expressed as a percentage, and FiO2 as a decimal. So for example, for a patient with a sat of 97% on RA (21% FiO2):
97 / 0.21 = 461 would be their S:F.
Chaudhuri D, Lazarte J, Shah K, Pitre T, Pekkarinen PT, Sendagire C, Martin GS, Jung C, Laffey JG, Rochwerg B; Sequential Organ Failure Assessment (SOFA)-2 study group. Approaches to Converting Sp o2 /F io2 Ratio to Pa o2 /F io2 Ratio for Assessment of Respiratory Failure in Critically Ill Patients: A Systematic Review. Crit Care Med. 2026 Apr 1;54(4):950-959. doi: 10.1097/CCM.0000000000007018. Epub 2026 Jan 2. PMID: 41493393.
Category: Ultrasound
Keywords: soft tissue; point of care ultrasound (PubMed Search)
Posted: 4/20/2026 by Alexis Salerno Rubeling, MD
Click here to contact Alexis Salerno Rubeling, MD
Sonographic findings suggestive of necrotizing fasciitis include:
Remember the mnemonic: STAFF (subcutaneous thickening, air, and fascial fluid)
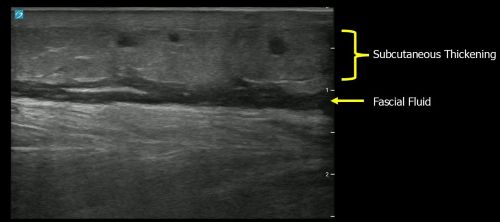
Castleberg E, Jenson N, Dinh VA. Diagnosis of necrotizing fascititis with bedside ultrasound: the STAFF exam. West J Emerg Med. 2014;15(1):111-3.
Category: Cardiology
Keywords: Atrial Fibrillation, Incidental Finding, ECG Monitoring, Anticoagulation (PubMed Search)
Posted: 4/19/2026 by Lena Carleton, MD
(Updated: 4/20/2026)
Click here to contact Lena Carleton, MD
Bottom line: Routine screening for atrial fibrillation (AF) is not recommended in the emergency department (ED). However, AF is often detected incidentally on continuous ECG monitoring. When identified, clinicians should inform the patient and consider anticoagulation if indicated.
Ischemic stroke remains a major cause of morbidity and mortality, with AF implicated in at least 12% of cases. Early detection allows for stroke prevention through timely anticoagulation.
In this single-center retrospective cohort study of 65,244 adult ED patients on continuous ECG monitoring (2020–2024), AF was detected in 10.1%. Of these, 48.7% had known AF, 21.6% were diagnosed or treated during the visit, and 29.6% were discharged without diagnosis or anticoagulation (“undiagnosed AF”), representing 3% of the total cohort. This group was more likely to be women, Black or Latino, Medicaid-insured, and without a primary care physician; 58.3% of the “undiagnosed AF” group met criteria for anticoagulation.
Over a median follow-up of 238 days, stroke incidence was 2.6 per 100 person-years in the undiagnosed AF group, compared with 2.4 in known AF and 0.5 in those without AF.
These findings suggest that opportunistic detection of AF in the ED may identify high-risk patients who could benefit from earlier diagnosis and anticoagulation.
Bottom line: Routine screening for atrial fibrillation (AF) is not recommended in the emergency department (ED). However, AF is often detected incidentally on continuous ECG monitoring. When identified, clinicians should inform the patient and consider anticoagulation if indicated. Though not explicitly discussed in this article, it is worth noting that incidental findings may also carry medicolegal implications.
Bismuth E, Jin BT, Molins E, et al. Opportunistic screening for atrial fibrillation with continuous ECG monitoring in the emergency department. Ann Emerg Med. 2026;87(1):56-65. doi:10.1016/j.annemergmed.2025.06.008
Category: Trauma
Keywords: obesity, trauma, mortality, organ failure, sepsis, ARDS (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/18/2026)
Click here to contact Robert Flint, MD
This German retrospective review of 1500 level one trauma center patients (ICU level or ISS over 9) found obesity was an independent predictor of ARDS, multisystem organ failure, and sepsis but not pneumonia or mortality.
Erdle, B., Mangold, J., Kalbhenn, J. et al. BMI is independently associated with ARDS, sepsis and multiorgan failure after major trauma—results of a high-volume retrospective observational cohort study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01603-7
Category: Administration
Posted: 4/17/2026 by Kevin Semelrath, MD
(Updated: 4/18/2026)
Click here to contact Kevin Semelrath, MD
Multiple past studies have shown that Black and female patients tend to be prescribed fewer opioids than White and male patients. This study looked at the rates of opioid usage post RSI.
They found that while Black patients received opioids at a higher rate, they were given lower doses than white patients. Older patients were less likely to receive opioids post RSI than younger patients. They did not find a difference in rates of opioid usage between genders, but female patients received lower doses of opioids overall.
AuBuchon K, Amaru A, Cepero T ...
Exploring Demographic Differences in Postintubation Analgesia by Racial Group, Sex, and Age
Journal of Emergency Medicine, 2025; 84, 69-81
Category: Pediatrics
Keywords: Abdominal trauma, CT, lipase (PubMed Search)
Posted: 4/15/2026 by Jenny Guyther, MD
(Updated: 4/17/2026)
Click here to contact Jenny Guyther, MD
Pancreatic injury in pediatric blunt abdominal trauma is rare.
This study was a secondary analysis of the data collected by the Pediatric Emergency Care Applied Research Network (PECARN) in the Intra-abdominal Injury Study Group. Of the children who had blunt abdominal trauma, 6% had intraabdominal injuries and 1% had pancreatitis. A patient was considered as having traumatic pancreatitis if they had 2 of the following: 1) upper abdominal tenderness, 2) serum lipase of amylase > 3 x the upper limit of normal or 3) imaging study positive for pancreatitis.
Children diagnosed with pancreatitis were more likely to report abdominal pain, vomiting, shortness of breath, thoracic trauma and handlebar injury compared to those without a diagnosis of pancreatitis. On exam, they were more likely to be hypotensive, tachypneic, evidence of abdominal wall injury, costal tenderness, abdominal distention and abdominal tenderness. When the PECARN prediction rule was applied to these patients, the sensitivity was 99% with a specificity of 42%. The rule missed one patient who had traumatic pancreatitis, but this patient did not meet the definition for clinically important abdominal injury (requiring therapeutic laparotomy, embolization, blood transfusion or requiring IV fluids for > 2 days).
Marks MS, Liveris A, Blumberg SM, Reddy SH, Meltzer JA. Predicting Pancreatitis in Children With Blunt Abdominal Trauma. Pediatr Emerg Care. 2025 Jun 6. doi: 10.1097/PEC.0000000000003421. Epub ahead of print. PMID: 40476662.
Category: EMS
Keywords: MVC, c-spine injury, PECARN, rules (PubMed Search)
Posted: 4/15/2026 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
Cervical spine injuries (CSI) are uncommon in children, but when present, they are often devastating. However, the application of a cervical collar in children is not benign and adverse effects include neck pain and discomfort and the downward tunnel vision it may create at the hospital leading to unnecessary testing. Recently, the PECARN group published a set of criteria to determine who requires imaging of the cervical spine in the emergency department. A planned subset of this initial study was to collect the impressions of EMS as they pertained to the 9 criteria to determine if these criteria could safely be used by EMS. The patients who were brought in by EMS with the potential for cervical spine injury, who were evaluated by the trauma team and/or had cervical imaging AND had electronic case reports filled out by EMS were included in the final analysis. Only 57% of the patients possible could be included based on the number of electronic case reports that were filled out.
Overall, when the criteria were applied to the EMS patients based on the EMS assessment, the PECARN CSI had a sensitivity of 88.5%, a specificity of 63.1%, a PPV of 3.7% and a NPV of 99.7%.
Of 122 patients, 14 patients who did have CSI were not detected. Further analysis of these missed patients showed that 11 of the patients did have one of the 9 criteria present which was documented by the ED but not by EMS. Only one of the 14 missed patients required operative intervention. 12/14 of these patients were from motor vehicle collisions.
The study criteria did perform better in the ED setting compared to the EMS setting. Further research will need to examine if these clinical criteria can be applied to the field or if they should be modified to increase the specificity.
The 9 criteria and a brief description of the original study can be found at: https://pecarn.org/pecarn_news/clinical-decision-rule-cervical-spine/
Browne LR, Ward CE, Harding M, Cook LJ, Adelgais KM, Ahmad FA, Burger R, Chaudhari PP, Corwin DJ, Glomb NW, Kuppermann N, Lee LK, Leonard JR, Owusu-Ansah S, Riney LC, Rogers AJ, Rubalcava DM, Sapien RE, Szadkowski MA, Tzimenatos L, Yen K, Leonard JC. Performance of the PECARN cervical spine injury prediction rule based on EMS clinician observations. J Trauma Acute Care Surg. 2025 Aug 21. doi: 10.1097/TA.0000000000004772. Epub ahead of print. PMID: 40836370.
Category: Critical Care
Keywords: albumin, sepsis, septic shock, crystalloid, resuscitation (PubMed Search)
Posted: 4/14/2026 by Zachary Wynne, MD
Click here to contact Zachary Wynne, MD
Summary:
The recent ARISS (Albumin Resuscitation in Septic Shock) trial showed no difference in 90-day mortality or other secondary outcomes, similar to other trials comparing albumin and crystalloid. Notably however, the trial did not meet its predetermined enrollment requirement of patients (in the setting of the COVID-19 pandemic) and had a large portion of its intervention group failing to meet goal serum albumin level.
The Bottom Line:
There remains no evidence-based mortality benefit of albumin over crystalloid in patients with septic shock that do not have additional indications for albumin (such as hepatorenal syndrome). Crystalloid resuscitation remains a staple of appropriate and cost-effective care in septic shock. Albumin can be considered on a case-by-case basis after standard crystalloid resuscitation in this clinical setting.
Background:
What is the ideal fluid for resuscitation in septic shock? Crystalloids or colloids, such as albumin?
Many trials have sought to prove albumin would be beneficial in septic shock. Some data has suggested an immune modulatory role of albumin. Additionally, albumin is thought to help maintain serum oncotic pressure to prevent further capillary leak in vasodilatory shock. A summary of some trials before ARISS are summarized below:
With this background, researchers in Germany sought to further evaluate albumin's role in septic shock resuscitation.
ARISS (Albumin Resuscitation in Septic Shock) Trial - Feb 2026
Patients: Adults admitted to ICUs in Germany from 10/2019 to 5/2022 that had probable or definitive evidence of infection for septic shock, required vasopressors for at least one hour (MAP > 65 mmHg)?, had a lactate less than 18 mg/dL (2.0 mmol/L)?, and were enrolled within 24 hours of onset of septic shock. Exclusion criteria included patients that had a disease process that albumin is particularly harmful or advantageous (CHF, TBI, hepatorenal)?, pregnancy/lactation, alternative etiology of shock, and end of life care.
Intervention: All patients in intervention group received a 60-g loading dose of 20% albumin over 2-3 hours within 6-24 hrs after diagnosis of septic shock. Remainder of albumin administration was done by a resuscitation scheme to target an albumin greater than 3 g/dL while they remained alive and in the ICU.
Control: All patients in control group received crystalloid resuscitation but could receive albumin in certain situations deemed necessary (such as albumin < 1.5 g/dL).
Outcome: Primary outcome was 90-day all-cause mortality. Secondary outcomes included 28-day and 60-day mortality, ICU and hospital mortality, SOFA score change, ICU and hospital length of stay, ventilator-free and vasopressor-free days, and occurrence of adverse events.
Results: 440 patients were randomized, with 419 included in analysis. Albumin was administered in the intervention group for a median of 5 days. 15 patients received the full 28-day limit of protocol treatment with albumin. More than 50% of patients in the intervention group failed to achieve the target albumin level of greater than 3 g/dL. 90-day mortality by intention to treat analysis was 43.4% in the albumin group versus 45.9% in the control group (RR of 0.94 [95% CI, 0.76-1.17]) with no differences in subgroup analyzes. No secondary outcomes showed a statistically significant difference. There was no statistically significant difference in adverse events between groups.
Internal Validity: Enrollment did not meet need based on power calculation (estimated 1662 patients by their power calculation for a relative risk reduction of 15%. Factors affecting this included COVID-19 pandemic and a high exclusion rate for the trial enrollment of 72%. Additionally, many patients in the control group received albumin. The researchers additionally did a per-protocol analysis which also showed no statistically significant difference.
Ending Thoughts: This was a well designed trial combining elements of trials comparing albumin to crystalloids previously and using albumin to reach a defined target, similar to the ALBIOS trial. However, the lack of enrollment and not meeting their predetermined power calculation likely contributed to the results found in this trial. The trial leaves unanswered questions about albumin's role in septic shock, particularly with earlier timing and a clear concentration target.
Category: EMS
Keywords: prehospital, EMS, ultrasound (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/12/2026)
Click here to contact Robert Flint, MD
This German retrospective study compared the prehospital use of ultrasound by trained paramedics and compared their findings to in-hospital diagnosis and image results. The authors found:
“Diagnostic accuracy, defined as the concordance between prehospital POCUS-based working diagnoses and final in-hospital diagnoses, was particularly strong for lung ultrasound (pneumothorax, pulmonary edema, pneumonia and pleural effusion; sensitivity 91.7%, specificity 100%) and eFAST (sensitivity 100%, specificity 96.5%), while for the abdominal ultrasound examinations, the specificity was 70% and sensitivity was 71.43%.”
This study sets the stage for future prospective work looking at prehospital US use by paramedics.
Boehm, A., Bexten, T., Stanley, M. et al. Feasibility and diagnostic accuracy of paramedic-performed prehospital point-of-care ultrasound: a retrospective observational study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01595-4
Category: Orthopedics
Posted: 4/11/2026 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
What elements of the history are most helpful for diagnosing a concussion?
An estimated 1.1 million to 1.9 million pediatric concussions occur annually in the US.
OBJECTIVE: To determine the accuracy of clinical history for identifying concussion in children and adolescents.
While most children recover within 4 weeks, approximately 30% experience persistent symptoms beyond 28 days.
Early evaluation and timely management are associated with improved recovery—athletes who immediately reported their injury experienced almost five and half fewer days of symptoms compared to those who delayed reporting.
Key Diagnostic Findings
The review identified the most diagnostically useful symptoms (by likelihood ratio):
| Finding | Likelihood Ratio (LR+) | Specificity |
|---|---|---|
| Mental fog | 11.8–12.0 | 0.96 |
| Noise sensitivity | 6.9 | 0.94 |
| Nausea | 6.7 | 0.93 |
| Light sensitivity | 6.4 | 0.93 |
| Headache | 3.1 | 0.74 |
The ABSENCE of headache was the only finding that substantially reduced the likelihood of concussion (LR, 0.20; sensitivity, 0.86)
Shah SN, Chizuk HM, Fong H, Hannon M, Mannix RC. Does This Child Have a Concussion? The Rational Clinical Examination Systematic Review. JAMA.
Published online April 06, 2026.
Category: Pediatrics
Keywords: pediatrics, airway, intubation, infant, neonate (PubMed Search)
Posted: 4/10/2026 by Kathleen Stephanos, MD
(Updated: 5/3/2026)
Click here to contact Kathleen Stephanos, MD
BOTTOM LINE:
A 2024 meta analysis from the European Society of Anaesthesiology and Intensive Care and British Journal of Anaesthesia worked to develop joint guidelines for best practices for intubation of neonates and infants.
While this guide is focused primarily on anesthesia and operative care, several of the recommendations have practical application to the EM and ICU as well.
They focused on general guidance including ensuring appropriate anesthesia and analgesia during intubation. But also discussed that videolaryngoscopy with standard blades is the most appropriate first line for all intubations in this age group. It allows for appropriate visualization either directly or by video and for learners allows instructors to observe as well.
When there are difficulties with intubation, hyperangulated blades have very high success rates, but LMA and video assisted intubation with a fiberoptic scope are also appropriate next steps for securing an airway.
When intubating, uncuffed endotracheal tubes are acceptable in all infants though cuffed are also safe in infants over 3kg in weight.
Finally, while apneic oxygenation is regularly used in adults, it is also recommended in the neonatal period to avoid hypoxia.
Disma N, Asai T, Cools E, Cronin A, Engelhardt T, Fiadjoe J, Fuchs A, Garcia-Marcinkiewicz A, Habre W, Heath C, Johansen M, Kaufmann J, Kleine-Brueggeney M, Kovatsis PG, Kranke P, Lusardi AC, Matava C, Peyton J, Riva T, Romero CS, von Ungern-Sternberg B, Veyckemans F, Afshari A; and airway guidelines groups of the European Society of Anaesthesiology and Intensive Care (ESAIC) and the British Journal of Anaesthesia (BJA). Airway management in neonates and infants: European Society of Anaesthesiology and Intensive Care and British Journal of Anaesthesia joint guidelines. Eur J Anaesthesiol. 2024 Jan 1;41(1):3-23.
Category: Pharmacology & Therapeutics
Keywords: central retinal artery occlusion, tenecteplase, thrombolytic (PubMed Search)
Posted: 4/8/2026 by Alicia Pycraft
(Updated: 4/9/2026)
Click here to contact Alicia Pycraft
TenCRAOS was a phase 3 randomized, multi-center, double blind, double dummy, placebo-controlled trial in 78 patients that showed no significant difference in visual outcomes at 30 days for IV tenecteplase 0.25 mg/kg compared to aspirin 300 mg alone within 4.5 hours of central retinal artery occlusion (CRAO) symptom onset. Tenecteplase was associated with more serious adverse events, one of which was a fatal intracerebral hemorrhage.
Bottom line: Although tenecteplase has theoretical advantages in CRAO, the results of this trial do not support routine use.
Study design:
Results:
Ryan SJ, Jørstad ØK, Skjelland M, Pesonen M, Simonsen CZ, Bek T et al. A randomized trial of tenecteplase in central retinal artery occlusion. N Engl J Med. 2026. 394(5): 442-450.
Category: Trauma
Keywords: trauma, treatment disparity, gender (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/8/2026)
Click here to contact Robert Flint, MD
This systematic literature review looking at gender differences in trauma care reveals:
Ghika-Nanchen, A., Marzorati, L., Merra, A. et al. Sex and gender bias in major trauma care: a scoping review. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01596-3
Category: Critical Care
Posted: 4/7/2026 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
In a large, randomized trial conducted in 42 ICUs in France, high-flow oxygen did not reduce 28-day all-cause mortality in adult patients with acute hypoxemic respiratory failure when compared to standard oxygen support.
The SOHO Trial
Category: Geriatrics
Keywords: prehospital, geriatric, education (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/5/2026)
Click here to contact Robert Flint, MD
A modified 2 round Delphi study was used to create 57 learning objectives in geriatric care for European prehospital providers. Based on in-hospital learning objectives and literature, these experts came up with what appears to be a very reasonable and helpful list of education objectives for pre-hospital providers that could easily apply to emergency medicine learners as a whole. Here is their table:
https://link.springer.com/article/10.1186/s13049-026-01550-3/tables/3
Krohn, JN., Barrett, J., Heeren, P. et al. A European paramedic curriculum for geriatric emergency medicine developed via a modified Delphi technique. Scand J Trauma Resusc Emerg Med 34, 14 (2026). https://doi.org/10.1186/s13049-026-01550-3
