Category: Pediatrics
Keywords: Pediatrics, Migraine, Abdominal Migraine, Headache (PubMed Search)
Posted: 7/13/2018 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
Abdominal pain in children can be just as frustrating as dizzy in the elderly. Your exam is targeted at quickly ruling out acute pathologies, but then what? The diagnosis is often functional gastrointestinal disorders, like the ever exciting constipation. Abdominal migraine (AM) is an additional entity to consider during your emergency department evaluation.
The following factors are often associated with AM:
- peak incidence at 7 years old
- paroxsymal, periumbilical abdominal pain lasting more than 1 hour
- family history of migraine
- episodes not otherwise explained by known pathology.
AM can be associated with headache, pallor, anorexia, photophobia, and fatigue. There are multiple theories on the pathogenesis, which can be found in the article cited below. If there is a known history, and the patient is presenting with an exacerbation, the treatment protocols for migraine headache may be employed with good success.
________________________________________________________________
Bottom Line:
AM is increasingly recognized as a source of recurrent abdominal pain in children. If other organic pathologies can be ruled out, this may be an important diagnosis to consider so your patient can get the appropriate follow up and outpatient management.
Category: Pediatrics
Keywords: Pediatrics, Abdominal Pain (PubMed Search)
Posted: 2/2/2018 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
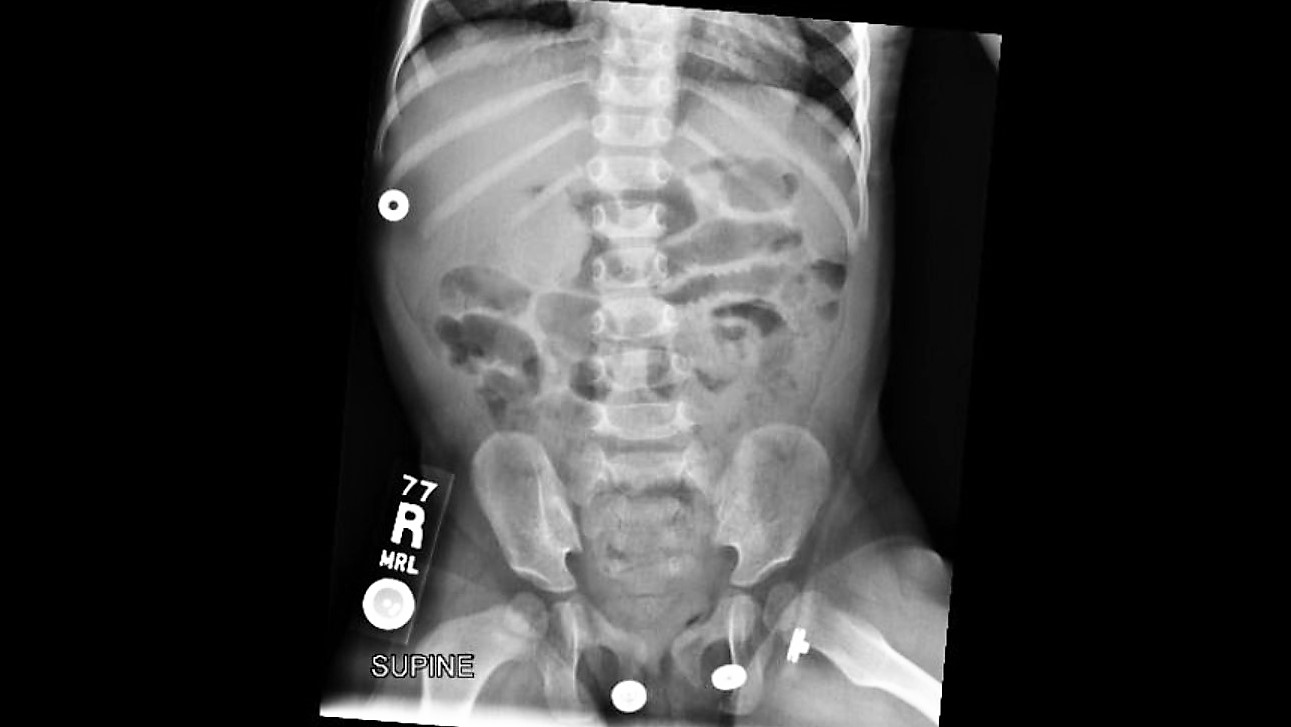 Your patient is an18 months old female with intermittent abdominal pain for the last 4-5 days. She has history of constipation and soy allergy, seen at an outside hospital three days ago for the same. She had an xray and was discharged home with instructions for at home clean out with diagnosis of constipation.
Your patient is an18 months old female with intermittent abdominal pain for the last 4-5 days. She has history of constipation and soy allergy, seen at an outside hospital three days ago for the same. She had an xray and was discharged home with instructions for at home clean out with diagnosis of constipation.
Mother is bringing her to your ED because the pain is back. The laxatives helped somewhat, but her symptoms have returned. She reports that the patient cries spontaneously, lasting 1-2 minutes, then completely resolves. These episodes happen at multiple times during the day.
ROS: Decreased appetite and energy, but NO fevers, vomiting, diarrhea, bloody stool, abdominal distension, hematuria, or lethargy.
Intussusception classically presents with colicky abdominal pain, palpable mass, and currant jelly stools, but in less than 50% of patients. The clinical presentation of intussusception actually occurs on a spectrum. Children who present early in their course may look well with intermittent, unexplained crying episodes, while others may be febrile, dehydrated, with bloody stools, and be septic. The diagnosis can be missed in up to 60% of children presenting for initial evaluation. Identified risk factors include any syndrome or abnormality causing a lead point, ie Meckel's Diverticulum, Familial Polyposis, lymphoma and Henoch-Scholein Purpura, as well as GI infections, bacterial and viral, (Adenovirus, Rotavirus, and HHV6, etc.)
On exam, our patient's abdomen was soft but hard to evaluate due to behavior. Flat plate AXR demonstrated a circular hyperdensity in the RUQ, which on ultrasound, corresponded to a large ileocolic intussusception. She was successfully treated with air enema reduction, which in recent review has the lowest recurrence rate of intussusception.
Bottom Line -
In children with intermittent abdominal pain or unexplained crying episodes, consider intussusception on your differential, as more than half are missed on initial presentation, which can be subtle. Late presentations can include bowel perforation, peritonitis, sepsis, and shock. If diagnosed, arrange for enema reduction or transfer to a facility with this capability.
References:
Waseem M, Rosenberg HK. Intussusception. Pedi Emer Care. Nov 2008, 24(11): 793-800.
Gluckman S, Karpelowsky J, Webster AC, McGee RG. Management for intussusception in children. Cochrane Review of Systematic Databases. 2017; Issue 6.
Category: Pediatrics
Keywords: NAT, non-accidental trauma, abusive head trauma, intra-abdominal injury, burns (PubMed Search)
Posted: 1/6/2018 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
In addition to suspicion of NAT with traumatic brain injury and burns, remember these other high risk injuries and features:
- Duodenal injuries in children <4 y/o
- Frena injuries in non-ambulating children
- Proximal and midshaft humeral fractures > supracondylar fractures
- Any bruising on the trunk, ears, neck, or with larger size or pattern
- Delay in seeking care, inconsistent history, mechanism inconsistent with developmental age, and blame of a sibling or other child inflicting harm are all historical features also high risk.
Non-accidental trauma (NAT) continues to be a sad, but prevelant pathology in the United States. It is estimated that one million children in the US have been victims of maltreatment. As high as one third of children with NAT had the abuse missed on prior medical evaluation. There are several screening tools and clinical prediction rules that have been developed for clinical use, but none are to be used as substitutes for full skeletal survey and CT scan when indicated.
TEN-4 (clinical prediction rule): 97% sensitivity, 84% specificity with regards to NAT in the setting of bruising by age, location and characteristic.
PEDIBIRN (clinical prediction rule): 96% sensitive, 43% specificity with regards to abusive head trauma in children less than 3 years old.
PredAHT (clinical prediction rule): 72% sensitive, 86% specificity, also for abusive head trauma less than 3 years old.
PIBIS (screening tool): scoring system for well appearing infants presenting with brief resolved unexplained event (BRUE), previously called apparent life threatening event or ALTE.
Escobar, MA, et al. The association of nonaccidental trauma with historical factors, examination findings, and diagnostic testing during the initial trauma evaluation. Journal Trauma Acute Care Surgery. 2017; 82(6).
Category: Pediatrics
Keywords: Pediatrics, Bronchiolitis, Respiratory Decompensation, Risk factors (PubMed Search)
Posted: 10/6/2017 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
Bronchiolitis season will soon be upon us. Here are some risk factors for children under 2 y/o with bronchiolitis, who may be more likely to suffer respiratory decompensation:
1. Age under 9 months
2. Black race
3. Hypoxia documented in the ED
4. Persisent accessory muscle use.
Bottom Line: Consider providing respiratory support sooner than later in bronchiolitic infants with risk factors for decompensation. For HFNC, start at 1.5 - 2.0 L/kg/min, and titrate to work of breathing and 02 saturations.
_______________________________________________________________________________
Pathophysiology: Bronchiolitis is a disease process that leads to inflammation of lower airways, causing bronchiolar edema, epithelial hyperplasia, mucus plugging, and air trapping or atelectasis. Common viral causes include RSV, Human Metapneumovirus, Rhinovirus, Influenza, and Parainfluenza.
Clinical Course: For most strains, the disease course is often 5-7 days with the worst days being 3-5. The disease process can last longer, especially in neonates. The predominant presenting symptoms are often rhinorrhea, low grade fevers, and cough, but apnea can be the primary symptom in younger infants. As a result of increased work of breathing, PO feeding tolerance decreases and leads to dehydration.
Treatment: Primarily supportive care with suctioning, hydration, supplemental oxygen via standard NC, HFNC, and in severe cases BiPAP, CPAP or intubation. Trial of bronchodilator is often used, but there is no role for repeated bronchodilator use if no benefit is seen in pre and posttreatment respiratory effort. Hypertonic saline is not recommended for routine use in the ED. Corticosteroids have no role for routine use in viral bronchiolitis, either.
Category: Pediatrics
Keywords: VTE, Thrombophilia, Enoxaparin, Children, Thromboembolism (PubMed Search)
Posted: 9/1/2017 by Megan Cobb, MD
Click here to contact Megan Cobb, MD
Background:
There is an increased incidence of venous thromboembolic events (VTE) in pediatrics due to improved diagnosis and survival of children with VTE.
The mortality rate is estimated at 2%.
The most common etiologies vary by age - Central venous catheters in neonates and infants, and inherited thrombophilia in children and adolescents.
Learning Points:
With neonates and infants, carefully assess medical history from neonatal period. Umbilical lines? PICC? Broviac? History of these is likely to be the cause.
In children and adolescents, unprovoked VTE is most likely due to inherited thrombophilia, and can be DVT, PE, Portal venous thrombus, etc.
Antithrombin deficiency: The first discovered inherited thrombophilia. The result is a lack of inhibition of coagulation factors – IIa, IXa, Xa, XIIa.
Protein C or/and S deficiency: The result is lack of inhibition of activated Factor V.
Factor V Leiden: Most common inherited thrombophilic defect. Resultant activated Factor V is resistant to normal Protein C and S activity.
Prothrombin Mutation: Second most common inherited thrombophilia. The result is increased levels of prothrombin, which increases the half-life of factor Va.
Initial treatment of clinically significant VTE can start with enoxaparin (1-1.5 mg/kg q12-24h, while checking Anti-Xa levels 4 hours after administration for therapeutic dosing.)
Pearl: Testing for thrombophilia is not always appropriate when diagnosing pediatric patients with their first VTE, but in children and adolescents with first diagnosed, unprovoked VTE, it is worthwhile to send off the initial hypercoaguability work up as this can affect the duration of treatment and need for testing or evaluation. Enoxaparin is a recommended medication to start therapeutic treatment of VTE, even in pediatric patients.
Van Ommen CH, Nowak-Gottl U. Inherited Thrombophilia in Pediatric Venous Thromboembolic Disease: Why and Who to Treat. Frontiers in Pediatrics. 2017: 5(20).
The Harriet Lane Handbook, 20th edition. Chapter 29: Drug Dosages. 2015
