Category: Trauma
Keywords: Mental health, trauma, intervention, blunt injury (PubMed Search)
Posted: 4/13/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
This study looked at pre-trauma mental health diagnosis (from medical records) and post-trauma mental health symptoms as assessed by survey. The majority of patients suffered blunt trauma and mean age was 67. Having pre/traumatic mental health diagnosis and particularly post-traumatic symptoms lead to worse health outcomes and financial conditions. Further work needs to be done to assess how to improve mental health symptoms post-traumatic injury.
Johnson, Patrick L. MD, MPH; Hemmila, Mark R. MD; Mullens, Cody L. MD, MPH; Oliphant, Bryant W. MD, MBA, MSc; Monahan, Janessa R. MS; Kelm, Julia D. BS; Jakubus, Jill L. PA-C, MHSA, MS; Curtiss, William J. MD; Mosher, Benjamin D. MD; Kieninger, Alicia N. MD; Scott, John W. MD, MPH
Journal of Trauma and Acute Care Surgery 98(3):p 425-434, March 2025. | DOI: 10.1097/TA.0000000000004521
Category: Gastrointestional
Keywords: Appendicitis, scoring, prediction, Alvarado Score (PubMed Search)
Posted: 4/6/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Missed appendicitis leading to rupture and peritonitis leads to morbidity, mortality, and malpractice claims. Part of a longer article looking at evaluation and management of appendicitis, these authors provide three scoring systems that can be used to identify appendicitis. Use of these scores can guide imaging and surgical consultation.
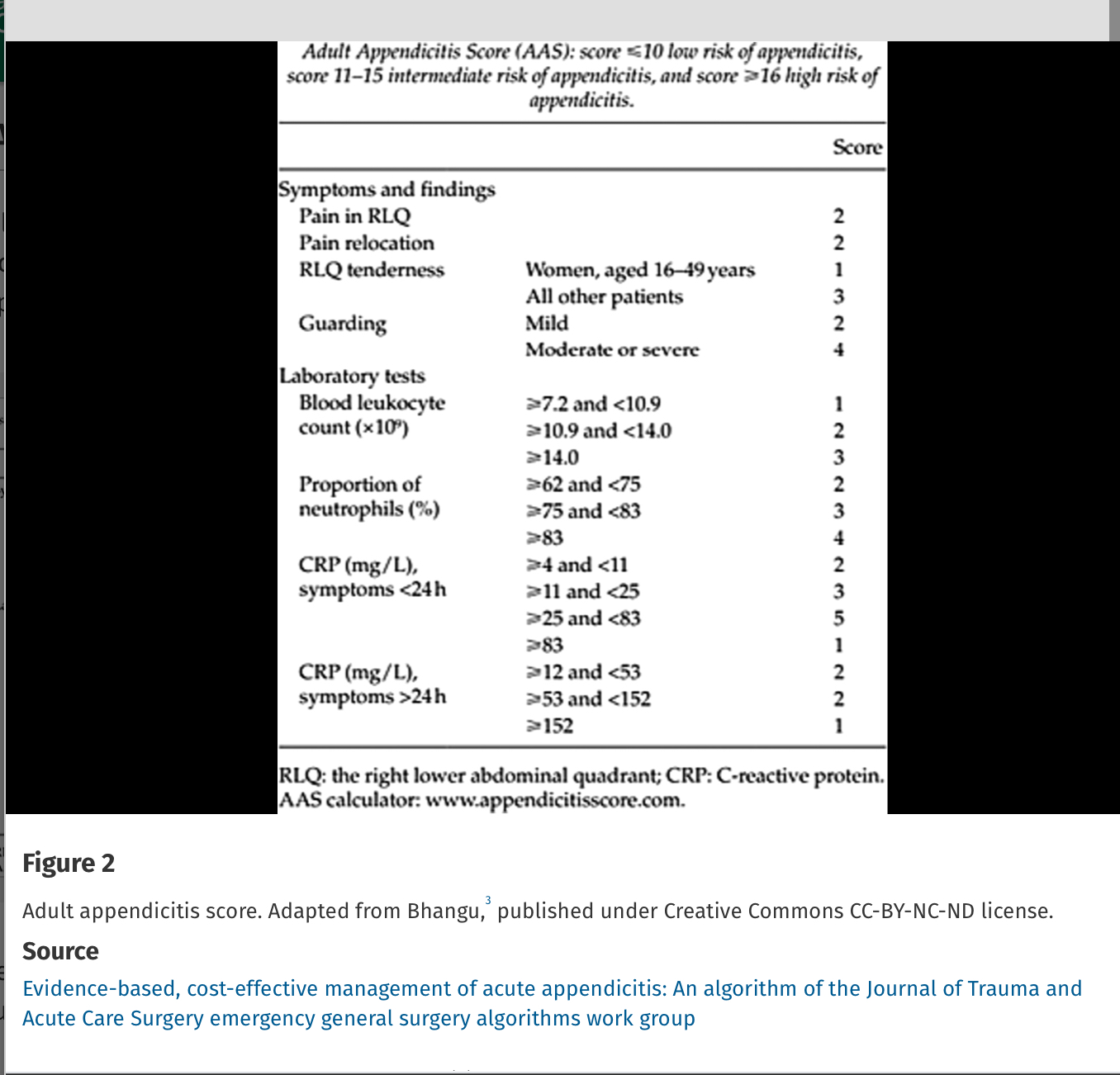
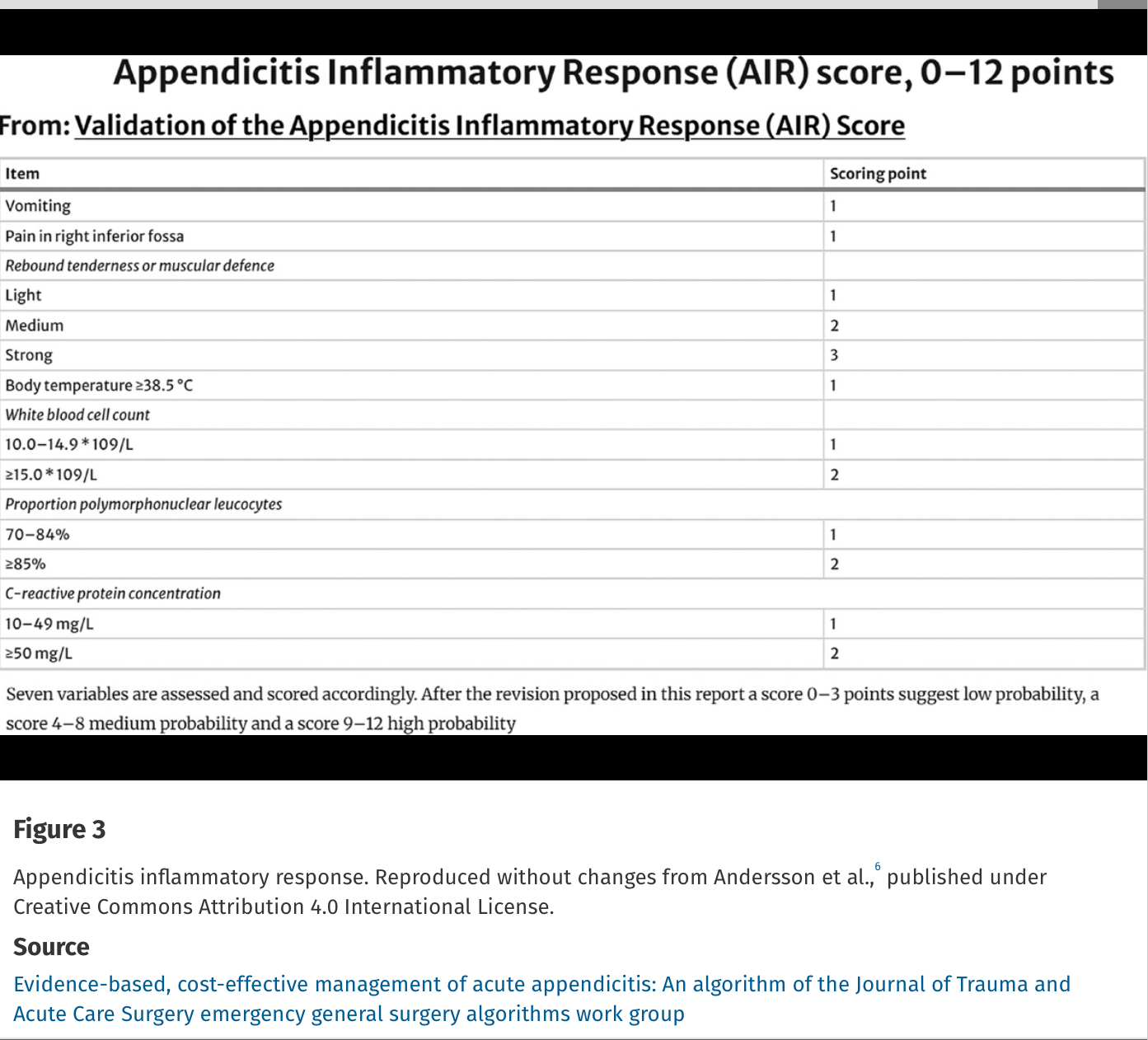
Alvarado Score: If a patient scores 1 to 4, the risk of appendicitis drops to 33%. If a patient scores >5, the risk of acute appendicitis is 66% or greater.
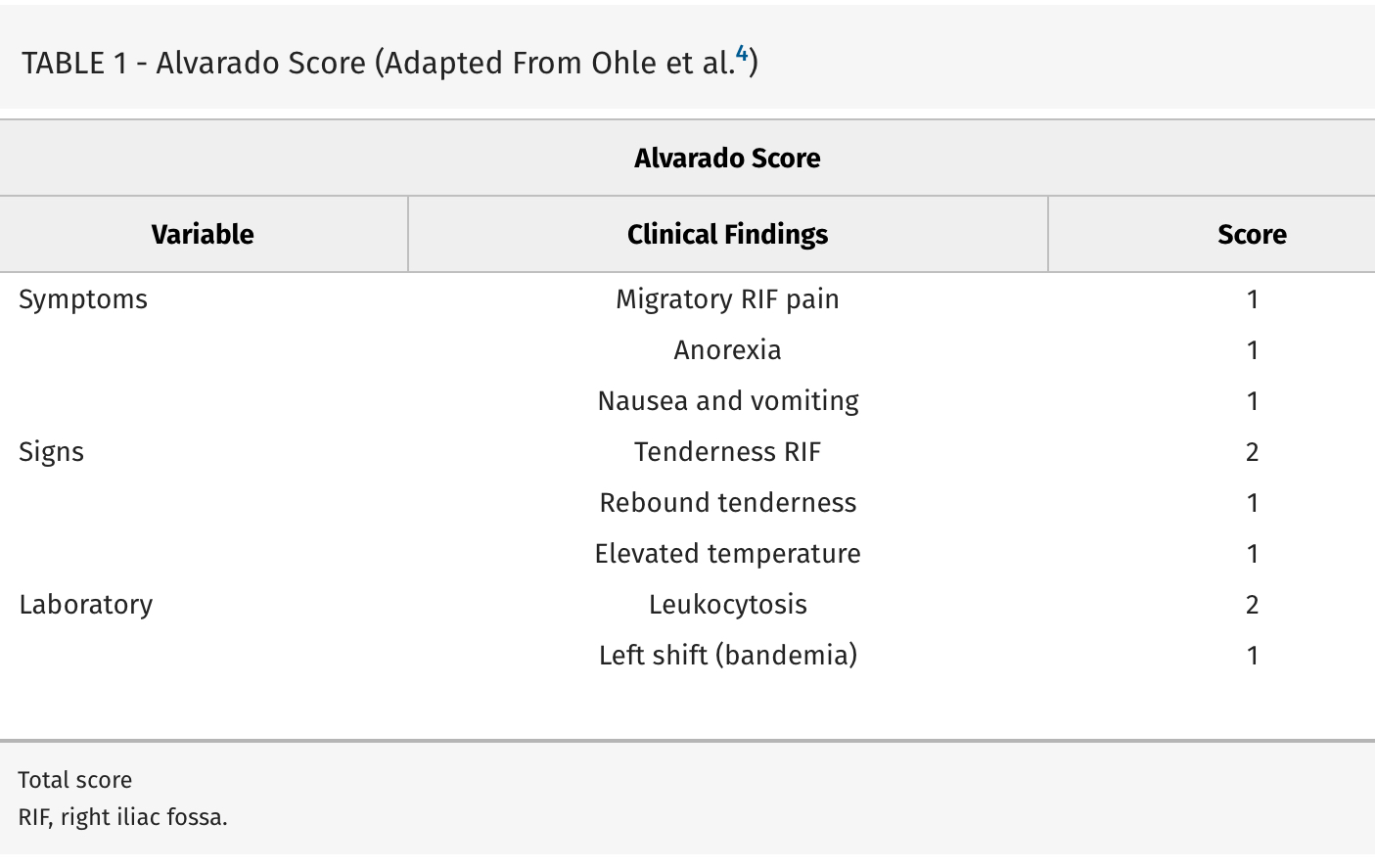
Evidence-based, cost-effective management of acute appendicitis: An algorithm of the Journal of Trauma and Acute Care Surgery emergency general surgery algorithms work group
Diaz, Jose J. MD, CPE, CNS, FACS, FCCM; Napolitano, Lena MD; Livingston, David H. MD; Costantini, Todd MD; Inaba, Kenji MD; Biffl, Walter L. MD; Winchell, Robert MD; Salim, Ali MD; Coimbra, Raul MD, PhD
Journal of Trauma and Acute Care Surgery 98(3):p 368-373, March 2025. | DOI: 10.1097/TA.0000000000004569
Category: Toxicology
Keywords: Toxicology, contaminate, opiate, stimulant (PubMed Search)
Posted: 4/5/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
This study from Australia reminds us that what patients think they ingested isn’t always what they did ingest. A high percentage of “cocaine” and other stimulants was actually fentanyl or other opiates. The authors do a nice job referencing similar studies in the United States. Any overdose could be a mixed picture due to impure street drugs.
Emergency Medicine AustralasiaVolume 37, Issue 2 e70038
Original Research
Open Access
Peter Chisholm MBBS, B Med Sc, MPH, Jared Brown BPharm, MPH, Thanjira Jiranantakan MD, MPH, FAFPHM, FACOEM, Mary Ellen Harrod PhD, Catherine McDonald BSc, Una Cullinan BSc, Darren M Roberts MBBS, PhD, FRACP, FAChAM
First published: 03 April 2025
Category: Infectious Disease
Keywords: JHR, syphillis, penicillin (PubMed Search)
Posted: 3/31/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
The Jarisch-Herxheimer reaction (JHR) is a non-specific set of symptoms (fever, malaise, worsened rash, hemodynamic instability, leukocytosis) seen after treating syphillis and other spirochete induced infections. In this study 1 in 4 patients treated with 2.4 million units of benzathine penicillin G developed a short lived JHR. Those who developed the reaction were more likely HIV negative, had secondary syphillis and had successful treatment at 6 months.
Dionne JA, Zhu C, Mejia-Galvis J, et al. Jarisch-Herxheimer Reaction After Benzathine Penicillin G Treatment in Adults With Early Syphilis: Secondary Analysis of a Randomized Clinical Trial. JAMA Netw Open. 2025;8(2):e2459490. doi:10.1001/jamanetworkopen.2024.59490
Category: Trauma
Keywords: ASA score, trauma, head injury, prognostication (PubMed Search)
Posted: 3/29/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
The American Society of Anesthesia score was an independent predictor of 90-day mortality as
well as low functional status at one year in 720 patients presenting to a single center with
moderate to severe brain injury. When used in conjunction with other prognosticating tools such
as the Trauma and Injury Severity Score, it increased the prognostic value of these scales.
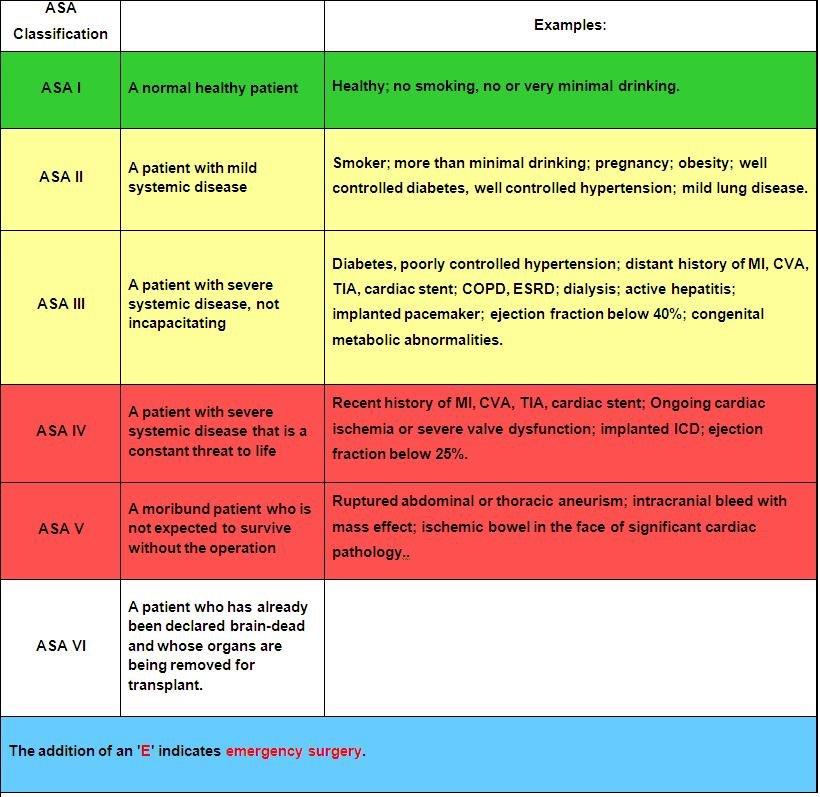
1. Kiwanuka, O., Lassarén, P., Fletcher-Sandersjöö, A. et al. ASA score is an independent
predictor of 1-year outcome after moderate-to-severe traumatic brain injury. Scand J Trauma
Resusc Emerg Med 33, 25 (2025). https://doi.org/10.1186/s13049-025-01338-x
2.Statement on ?ASA Physical Status Classification System.
Category: Trauma
Keywords: Trauma, rib fracture, multimodal (PubMed Search)
Posted: 3/23/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Controlling pain from rib fractures impacts morbidity and mortality. Over the past decade there has been a focus on decreasing opiate use and approaching this painful condition in a multimodal way. “The multimodal approach utilizes a combination of delivery methods including oral, parenteral, and regional single-shot or catheter-based techniques. Oral medications include opioids, non-steroidal anti-inflammatory drugs (NSAIDs), acetaminophen, skeletal muscle relaxants, alpha-2 agonists, mood stabilizers, and neuropathic pain medications. Parenteral medications encompass most of the oral options in addition to ketamine and lidocaine. Regional anesthesia includes epidural analgesia (EA), paravertebral blocks, intercostal blocks, and myofascial plane blocks.”
This study is a single center in Canada looking at medication used for patients admitted over 10 years with rib fractures along with demographics, injury severity and outcomes. The authors concluded:
“Although multimodal pain management strategies have improved over time, a large proportion of patients, even among those with flail chest, still do not receive multimodal pain management. Elderly patients, at highest risk of adverse outcomes, were less likely to receive multimodal pain management strategies and should be the target of performance improvement initiatives.”
Naveed A, Adams-McGavin RC, Ladha K, et al. A 10-year review of pain management practices for rib fractures at a lead trauma hospital: Are we adopting all multimodal pain management strategies? Trauma. 2025;27(1):18-23. doi:10.1177/14604086231198764
Category: Trauma
Keywords: Whole blood, trauma (PubMed Search)
Posted: 3/22/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Achieving faster homeostasis in trauma patients leads to lower mortality, less coagulopathy, and lower total blood volume transfusion requirements. This study looked at time to achieving homeostasis as defined by transfusion requirements as well as laboratory measurements in critically ill trauma patients who either received whole blood or component therapy transfusion as part of their resuscitation. Those receiving whole blood achieved statistically significant faster homeostasis.
Chipman, Amanda M. MD; Luther, James F. MA; Guyette, Francis X. MD, MPH; Cotton, Bryan A. MD; Cannon, Jeremy W. MD; Schreiber, Martin A. MD; Moore, Ernest E. MD; Namias, Nicholas MD, MBA; Minei, Joseph P. MD; Yazer, Mark H. MD; Vincent, Laura MS, RN; Cotton, Abigail L. BS, MPH; Agarwal, Vikas MD; Brown, Joshua B. MD, MSc; Leeper, Christine M. MD; Neal, Matthew D. MD; Forsythe, Raquel M. MD; Wisniewski, Stephen R. PhD; Sperry, Jason L. MD, MPH; the SWAT Study Group. Early achievement of hemostasis defined by transfusion velocity: A possible mechanism for whole blood survival benefit. Journal of Trauma and Acute Care Surgery 98(3):p 393-401, March 2025. | DOI: 10.1097/TA.0000000000004507
Category: Trauma
Keywords: kidney trauma, grading, (PubMed Search)
Posted: 3/16/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Unless a patient is unstable, renal injuries are managed non-operatively or endovascularly. Here is the
2025 Kidney Injury Grading Scale from AAST.
AAST AIS
Grade Severity Imaging Criteria
I 2 –Subcapsular hematoma <3.5 cm without active bleeding
– Parenchymal contusion without laceration
II 2 – Parenchymal laceration length <2.5 cm
– HRD <3.5 cm without active bleeding
III 3 – Parenchymal laceration length ?2.5 cm
– HRD ?3.5 cm without active bleeding
– Partial kidney infarction
– Vascular injuries without active bleeding
– Laceration extending into urinary collecting system and/or urinary extravasation
IV 4 – Active bleeding from kidney
– Pararenal extension of hematoma
– Complete/near-complete kidney infarction without active bleeding
– MFK without active bleeding
– Complete/near-complete ureteropelvic junction disruption
V 5 – Main renal artery or vein laceration or transection with active bleeding
– Complete/near-complete kidney infarction with active bleeding
– MFK with active bleeding
Keihani, Sorena MD, MSCI; Tominaga, Gail T. MD; Matta, Rano MD; Gross, Joel A. MD; Cribari, Chris
MD; Kaups, Krista L. MD, MSc; Crandall, Marie MD, MPH, FACS; Kozar, Rosemary A. MD; Werner,
Nicole L. MD, MS; Zarzaur, Ben L. MD; Coburn, Michael MD, FACS; Myers, Jeremy B. MD, FACS. Kidney
organ injury scaling: 2025 update. Journal of Trauma and Acute Care Surgery 98(3):p 448-451, March
2025. | DOI: 10.1097/TA.0000000000004509
Category: Trauma
Keywords: Sarcopenia, trauma, ct scan (PubMed Search)
Posted: 3/9/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Having a readily measurable variable to identify frailty on admission for critically injured patients would help prognosticate morbidity, mortality, and discharge destination. Sarcopenia has been used to prognosticate length of stay, discharge destination, and physical function recovery in oncology and general surgery patients. Sarcopenia is defined as “age-related progressive loss of muscle mass and strength. The main symptom of the condition is muscle weakness. Sarcopenia is a type of muscle atrophy primarily caused by the natural aging process. Scientists believe being physically inactive and eating an unhealthy diet can contribute to the disease.” 1. This study looked at admission CT scan psoas muscle sarcopenia in 197 critically injured patients. The authors concluded:
“For trauma critical care patients, sarcopenia on admission CT was associated with dependent discharge destination and therefore is unfavourable. Defining sarcopenia early in a trauma patient’s critical care admission may help to identify those at risk of poor outcomes.” 2
1. Sarcopenia (Muscle Loss): Symptoms & Causes
2. Badminton R, Christie R, Brohi K, Cole E. Pre-injury sarcopenia and the association with discharge destination in critical care trauma patients. Trauma. 2025;27(1):57-64. doi:10.1177/14604086231214878
Category: Trauma
Keywords: Male. Female, outcome, trauma (PubMed Search)
Posted: 3/6/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
The Pan-Asia Trauma Outcomes Study database was reviewed for differences in in-hospital mortality and functional capacity at discharge between male and female trauma patients. There were 76,000 trauma patients from 12 Asian countries in this study. The authors concluded: “This study indicates no difference in the general trauma outcomes in the Asia Pacific between females and males. Although younger females with less severe injuries had better functional outcomes, this advantage disappeared in severe injuries and those over 50 years.” There were several differences in mechanism of injury and age of presentation. “With females more frequently represented in the ??50 age group (60.13%) compared to males (44.87%) (p?<?0.001). Trauma type also varied between sexes; 95.51% of females experienced blunt trauma compared to 93.65% of males (p?<?0.001). Anatomically, males predominantly sustained injuries to the head, face, thorax, abdomen, and upper extremities, whereas females more frequently suffered injuries to the lower extremities and spine (p?<?0.001).” This is similar toEuropean and North American data
Bin Kunji Mohamad, M., Jamaluddin, S.F., Ahmad, N. et al. Trauma outcomes differences in females: a prospective analysis of 76 000 trauma patients in the Asia-Pacific region and the contributing factors. Scand J Trauma Resusc Emerg Med 33, 34 (2025). https://doi.org/10.1186/s13049-025-01342-1
Category: Trauma
Keywords: EMS, AlS, trauma, Bls, outcome (PubMed Search)
Posted: 3/5/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Large retrospective propensity matching study looking at mortality in trauma patients based on ALS vs. BLS transport crew found lower mortality in those attended by ALS crews. The matching was “based on patient age, sex, year, ICD-10-CM based injury severity score, mechanism of injury, AIS based body region of injury, EMS characteristics including time with patient and prehospital interventions performed, prehospital vital signs, and trauma center designation.”
This is different than other studies which showed limited difference. other studies have shown improved survival with police “scooping and running” with penetrating trauma patients.
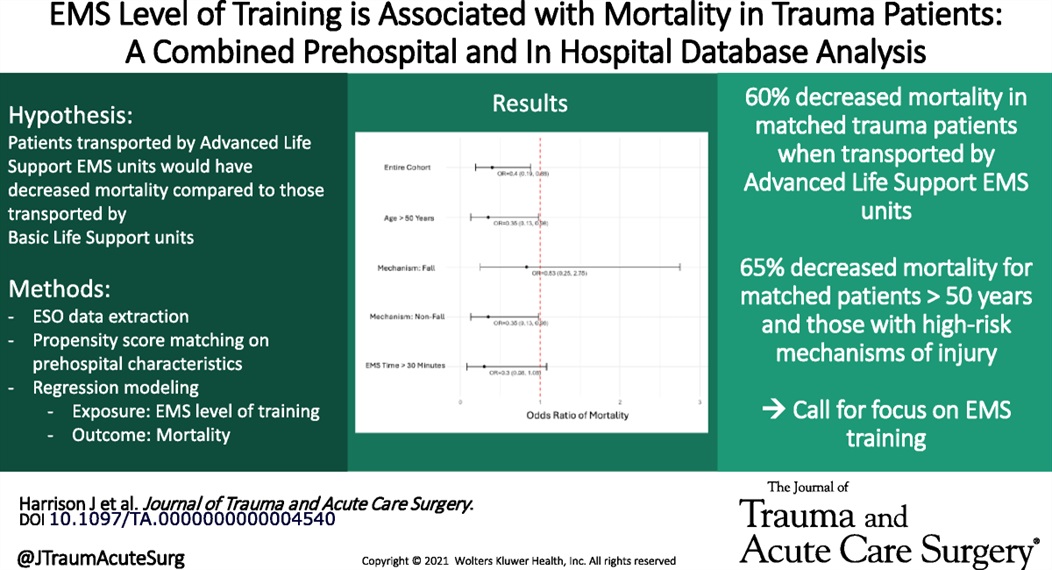
Harrison, Julia MD; Bhardwaj, Akshay MS; Houck, Olivia MPH; Sather, Kristiana MD; Sekiya, Ayako MPH; Knack, Sarah MD; Saarunya Clarke, Geetha PhD; Puskarich, Michael A. MD, MSCR; Tignanelli, Chris MD, MSc; Rogers, Lisa MPH; Marmor, Schelomo PhD; Beilman, Greg MD. Emergency medical services level of training is associated with mortality in trauma patients: A combined prehospital and in hospital database analysis. Journal of Trauma and Acute Care Surgery 98(3):p 402-409, March 2025. | DOI: 10.1097/TA.0000000000004540
Category: Trauma
Keywords: Trauma, geriatric, fall, pain management, fracture, rib, pelvis (PubMed Search)
Posted: 3/1/2025 by Robert Flint, MD
(Updated: 3/2/2025)
Click here to contact Robert Flint, MD
Rib and pelvic fractures are common findings in geriatric trauma patients, even in low impact trauma such as falls from standing. Pain management is vital for improving morbidity and mortality. The IFEM White Paper suggests:
“Use multimodal pain management strategies, including regional anesthesia and non-opioid analgesics, to control pain without compromising recovery.
Monitor closely for complications such as pneumonia or hemodynamic instability, intervening promptly to mitigate risks.
Collaborate with physiotherapists to implement early mobility programs, reducing the risk of deconditioning and promoting recovery.”
A multidisciplinary team proficient in geriatric trauma care leads to better outcomes. This may require transfer to a trauma center.
Trauma in Older Adults: Evidence-Based Guidelines for Optimized Care White Paper
Trauma Special Interest Group and Geriatric Emergency Medicine Special Interest Group
https://assets.nationbuilder.com/ifem/pages/1768/attachments/original/1740084007/IFEM_Trauma_in_Older_Adults_Evidence-Based_Guidelines_for_Optimized_Care_White_Paper_December_2024.pdf?1740084007
Published: December 2024
Category: Trauma
Keywords: Trauma, geriatrics, frailty (PubMed Search)
Posted: 3/1/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
This white paper reminds us that age is just a number; frailty is a better predictor of morbidity and mortality after trauma.
“Frailty, characterized by reduced physiological reserve and increased vulnerability to stressors, is a significant factor influencing recovery from trauma. Individuals with frailty may experience slower healing, higher rates of complications, and longer hospital stays. Tools such as the Clinical Frailty Scale (CFS) and the Trauma-Specific Frailty Index (TSFI) have been developed to assess frailty systematically, enabling clinicians to predict outcomes and guide treatment decisions.”
Trauma in Older Adults: Evidence-Based Guidelines for Optimized Care White Paper
Trauma Special Interest Group and Geriatric Emergency Medicine Special Interest Group
https://assets.nationbuilder.com/ifem/pages/1768/attachments/original/1740084007/IFEM_Trauma_in_Older_Adults_Evidence-Based_Guidelines_for_Optimized_Care_White_Paper_December_2024.pdf?1740084007
Published: December 2024
Category: Trauma
Keywords: Ems, trauma, arrest, resuscitation (PubMed Search)
Posted: 2/23/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
This position paper from American College of Surgeons, NAEMSP, and ACEP outlines a literature based approach to prehospital care of traumatic circulatory arrest. It logically could be applied to care in the hospital as well. Care of a traumatic arrest is different than a medical etiology arrest.
“Emphasize the identification of reversible causes of traumatic circulatory arrest and timely use of clinically indicated life-saving interventions (LSIs) within the EMS clinician’s scope of practice. These include:
Epinephrine should not be routinely used, and if used should not be administered before other LSIs.
External chest compressions may be considered but only secondary to other LSIs.
Chest decompression if there is clinical concern for a tension pneumothorax. Empiric bilateral decompression, however, is not indicated in the absence of suspected chest trauma.
Airway management using the least-invasive approach necessary to achieve and maintain airway patency, oxygenation, and adequate ventilation.
External hemorrhage control with direct pressure, wound packing, and tourniquets.”
Amelia M. Breyre, Nicholas George, Alexander R. Nelson, Charles J. Ingram, Thomas Lardaro, Wayne Vanderkolk, John W. Lyng,
Prehospital Management of Adults With Traumatic Out-of-Hospital Circulatory Arrest—A Joint Position Statement,
Annals of Emergency Medicine,
Volume 85, Issue 3,
2025,
Pages e25-e39,
ISSN 0196-0644,
https://doi.org/10.1016/j.annemergmed.2024.12.015.
Category: Trauma
Keywords: Peds, trauma, centers, adolescents (PubMed Search)
Posted: 2/16/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Looking at 416 patients aged 12-16, 48% at a Peds trauma center vs 20% at adult Level 1 center vs 34% at an adult level 2 center, there was no difference in in hospital mortality between adult and pediatric centers.
The authors conclude “These findings suggest that severely injured adolescents aged 12 to 16 years may be safely treated at either adult or pediatric trauma centers.”
Muttalib F, Tillmann B, Ernst G, Murthy S, Bhutta Z, Hansen B, Adhikari NKJ. Mortality Among Severely Injured Adolescents Admitted to Pediatric vs Adult Trauma Centers. JAMA Netw Open. 2024 Dec 2;7(12):e2450647. doi: 10.1001/jamanetworkopen.2024.50647.
Category: Cardiology
Keywords: Hypertension, as needed, acute kidney injury (PubMed Search)
Posted: 2/9/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
A retrospective look at veterans who received oral and/or IV as needed blood pressure medications while hospitalized in a non-ICU setting found an association with as needed meds and acute kidney injury, greater than 25% blood pressure drop in 3 hours, and death, stroke and MI while hospitalized. IV medications had a higher association.
While needing prospective validation, this appears to be more evidence to treat the patient not the number.
Canales MT, Yang S, Westanmo A, Wang X, Hadley D, Ishani A, Mohandas R, Shorr R, Lo-Ciganic W. As-Needed Blood Pressure Medication and Adverse Outcomes in VA Hospitals. JAMA Intern Med. 2025 Jan 1;185(1):52-60. doi: 10.1001/jamainternmed.2024.6213. PMID: 39585709; PMCID: PMC11589853.
Category: Infectious Disease
Keywords: Risk, soft tissue, infection (PubMed Search)
Posted: 1/30/2025 by Robert Flint, MD
(Updated: 2/2/2025)
Click here to contact Robert Flint, MD
Risk factors for necrotizing soft tissue infections include: obesity, diabetes mellitus, peripheral vascular disease, immunosuppression, injection drug use, and deep traumatic wounds.
“Any anatomical site can be involved, but the most common sites are perineal, anorectal, foot, or lower extremities.”
Category: Trauma
Keywords: Cervical sound, age, geriatric, trauma, clearance (PubMed Search)
Posted: 2/1/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
Not based on currently available literature.
This editorial reminds us that the only evidenced based screening criteria we have for C-spine clearance in those over age 65 after trauma is the Canadian C-Spine Rule (2002). This rule recommends imaging for all patients over age 65. No large, well done study indicates physical exam or other means can be used to clear C-Spines in those over age 65.
Rodriguez R, Greenberg S. Is older age an appropriate criterion alone for ordering cervical spine CT after trauma. Acad Emerg Med. 2024; 00: 1-2. doi:10.1111/acem.15001
Category: Infectious Disease
Keywords: Soft tissue infection (PubMed Search)
Posted: 1/30/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
These infections remain difficult to diagnose early and early diagnosis is key to limiting morbidity and mortality.
“The classic clinical signs and symptoms are rarely all present especially in early disease. Crepitus or gas in the soft tissues, while specific, is only present in approximately 10% of patients. More often, the presenting symptoms are nonspecific: fever, pain, induration, and edema. Pain out of proportion to examination is a more specific finding that may assist in differentiation of NSTI from cellulitis.”
Bisgaard, Erika K. MD; Bulger, Eileen M. MD
Journal of Trauma and Acute Care Surgery 97(5):p 678-686, November 2024. | DOI: 10.1097/TA.0000000000004351
Category: Trauma
Keywords: Chest trauma, ketorolac, ketamine (PubMed Search)
Posted: 1/26/2025 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
This small study randomized patients with 2 or greater rib fractures or requiring chest tube insertion into a kerorolac (30 mg) or ketamine (0.25 mg/kg) group and evaluated pain levels pre, 30 and 60 minutes post medication administration. They also looked at need for morphine rescue medication. The ketamine group had superior pain control and required less rescue medication.
Hossein Zabihi Mahmoodabadi MD, Zeynab Seyed Javadein MD, Fatemeh Moosaie MD, MPH, Ali Faegh, Maryam Bahreini MD
First published: 31 December 2024
