Category: Orthopedics
Keywords: biceps, tendon, rupture (PubMed Search)
Posted: 12/24/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
The long head of the biceps originates from the glenoid tubercle and superior labrum.
Rupture of the proximal biceps tendon comprises 90-97% of all biceps ruptures
Often in men aged 40-60y
- Almost exclusively involves the long head.
- Aka "Popeye Arm" (distal contraction of the muscle belly)
- May be acutely traumatic or microtears & age associated degeneration
- Minimal loss of function because short head of biceps remains attached
- Many patients can be treated non operatively
- Most asymptomatic after 4-6 weeks
- Place in sling, ice, analgesia
- Refer to ortho for re-evaluation and determination of operative versus conservative management
http://imaging.birjournals.org/content/15/4/193/F7.large.jpg
Category: Orthopedics
Keywords: fractures, child abuse, radiology (PubMed Search)
Posted: 12/10/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Metaphyseal bucket handle and corner fractures are almost pathognomonic for child abuse
These injuries were originally identified by clinicians evaluating children with subdural hematomas
These injuries are typically seen in the ankles, knees, elbows and wrists
Violent twisting, shaking, or pulling across a joint creates shearing forces across the weak epiphyseal growth plate and metaphysis
This leads to
1) A thin rim of mineralized metaphyseal bone aka “bucket handle”
http://rad.usuhs.mil/rad/home/peds/bucketarrow.jpg
OR
2) Small flecks of bone from the metaphyseal corner adherent to periosteum
http://t2.gstatic.com/images?q=tbn:ANd9GcT0kZ3VR1f7MwRj7oIa6jaYVp_-f8kZ1NhSbw4kCTRGNLDJ1pKK9g
Category: Orthopedics
Keywords: Weber, ankle fracture, fibula (PubMed Search)
Posted: 11/26/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
The Weber classification system
A commonly used, simple, easily remembered system used to describe ankle fractures. The system focuses on the integrity of the syndesmosis.
http://www.accessemergencymedicine.com/loadBinary.aspx?fileName=simo_c017f013t.gif
- TYPE A: fibula fracture below the ankle joint/syndesmosis (which is intact). Deltoid ligament intact. Medial malleolus can be fractured. Usually treated with closed reduction.
http://www.gentili.net/image1.asp?ID=-241442344&imgid=AnkleWeberAAP600.jpg&Fx=Weber+A+Fracture
- TYPE B: is a transsyndesmotic fracture with usually partial rupture of the syndesmosis (though may be intact). No gross widening to the tib/fib articulation.. Deltoid ligament intact. Medial malleolus often fractured. Variable stability. Any clinical or radiographic injury to the medial joint complex make this an unstable fracture
http://www.gentili.net/image.asp?ID=145&imgid=AnkleWeberBmortise600.jpg&Fx=Weber+B+Fracture
- TYPE C: Fibular fracture above the level of the syndesmosis with usually a total rupture of the syndesmosis (seen as widening of the distal tib/fin articulation), resulting in instability of the ankle mortise. Associated with medial malleolus fracture or deltoid ligament injury. Unstable.
http://www.gentili.net/image1.asp?ID=146&imgid=anklewebcapoblx2600.jpg&Fx=Weber+C+Fracture
Category: Orthopedics
Keywords: Back Pain, Treatment, Guidlines (PubMed Search)
Posted: 11/19/2011 by Michael Bond, MD
Click here to contact Michael Bond, MD
Low Back is one of the most common complaints that we see in the Emergency Department. Our first priority is to rule out those causes that can lead to paralysis or death (i.e.: epidural abscess, pathological fracture, cauda equina syndrome, etc…). However, most of the back pain that we will see is musculoskeletal in origin.
The American College of Physicians (ACP) and the American Pain Society (APS) released joint recommendations on the evaluation of treatment of individuals with back pain in 2007.
In summary their key recommendations were:
Links to the Clinical Guidelines are listed below:
Category: Orthopedics
Keywords: wrist arthrocentesis radiocarpal joint (PubMed Search)
Posted: 11/12/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Arthrocentesis of the Wrist
First locate and feel comfortable identifying two important landmarks:
1) Lister's tubercle is an elevation found in the center of the dorsal aspect of the distal end of the radius
http://www.aafp.org/afp/2004/0415/afp20040415p1941-f2.jpg
2) The extensor pollicis longus (EPL) tendon runs in a grove just radially to Lister's tubercle. Active extension of wrist and thumb aid with identification.
http://www.rad.washington.edu/academics/academic-sections/msk/muscle-atlas/upper-body/extensor-pollicis-longus/atlasImage
A) Positioning: Place wrist in ulnar deviation and 20 - 30 degrees of flexion. Apply longitudinal traction to the fingers of the hand.
B) Technique: Insert a small needle (22g) just distal to the tubercle and on the ulnar side of the EPL tendon.
http://img.medscape.com/pi/emed/ckb/clinical_procedures/79926-79928-80032-1477044tn.jpg
http://www.youtube.com/watch?v=nlPdb_mymw4&feature=related
http://www.youtube.com/watch?v=UVG7fZvZD-s&feature=related
Roberts and Hedges Clinical Procedures in Emergency Medicine
Category: Orthopedics
Keywords: TFCC, triangular fibrocartilage complex, wrist (PubMed Search)
Posted: 10/23/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
The TFCC (triangular fibrocartilage complex) is a ligamentous/cartilage like complex similar to the meniscus of the knee located on the ulnar side of the wrist.
http://yanyanxu.com/wp-content/uploads/2008/01/trifibcc.gif
Hx: ulnar sided wrist pain following trauma and associated with activity related mechanical symptoms such as clicking.
PE: tenderness to palpation distal to ulnar head or at ulnar styloid . Tenderness against resisted radial deviation.
Plain film may show ulnar styloid avulsion or injury to carpal structures.
Refer to hand/wrist surgeon
Splint in ulnar gutter of long arm spica
MRI or arthrogram are studies of choice.
http://www.cobalthealth.co.uk/MImageGen.ashx?image=%2Fmedia%2F12951%2Fwrist-tfcc-tear-big.jpg&width=170&crop=true
Category: Orthopedics
Keywords: Sinus tarsi syndrome (PubMed Search)
Posted: 10/15/2011 by Michael Bond, MD
(Updated: 9/24/2013)
Click here to contact Michael Bond, MD
Sinus Tarsi Syndrome
Category: Orthopedics
Keywords: dislocation, fibula, reduction (PubMed Search)
Posted: 10/8/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Anterolateral dislocation is most common (>85%)
As the tib/fib joint has its own synovial cavity, a knee effusion will not be seen
Mechanism: fall on the flexed knee with foot/ankle inversion
Hx: swelling, variable amount of lateral knee pain (anywhere from mild discomfort to inability to bear weight)
PE: Prominence of the fibular head, ankle motion exacerbates knee pain. no associated neurovascular issues
However with less common dislocations (posterior and superior) peroneal nerve injury may occur
Reduction: Place patient supine with knee flexed to 90 degrees. Ankle should be dorsiflexed and externally rotated.
REVERSE THE INJURY: Apply firm posteriorly directed pressure to the fibular head. May head an audible pop as fibular head reduces. Reassess collateral ligament function.
Category: Orthopedics
Keywords: radial nerve, mononeuropathy (PubMed Search)
Posted: 9/24/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Saturday night palsy - radial nerve mononeuropathy due to improper arm positioning associated with inebriated sleep.
Physical examination - Wrist and finger drop.
Patients may have findings suggestive of ulnar nerve co-involvement (interossei testing) which may falsely lead the examiner to consider a more proximal location for the lesion such as the brachial plexus.
The finger drop caused by the radial nerve lesion places the hand at a mechanical disadvantage. Adjust for this by examining the hand on a flat surface (stretcher, counter top). With the fingers now supported in extension at the MCP joint (no longer "dropped"), the interossei can now be tested in isolation and will be normal.
Category: Orthopedics
Keywords: Posterolateral Corner, knee (PubMed Search)
Posted: 9/17/2011 by Michael Bond, MD
(Updated: 5/2/2026)
Click here to contact Michael Bond, MD
Posterolateral Corner Injuries
The posterolateral corner “PLC” of the knee is becoming increasingly recognized as an extremely important structure to maintain the stability of the knee joint.
PLC injuries occur with hyperextension, varus load and tibial external rotation. So the most common mechanism is a posterolaterally directed blow to the anteromedial tibia when the knee is hyperextended. PLC injuries are commonly associated with injury to other ligaments (ACL, PCL, LCL) and occur in isolation in <5% of cases. If suspected make sure to check for other ligamentous injuries.
Since this injury can be missed and is associated with significant disability it is important to test for it. This YouTube video, http://youtu.be/bnXaTdvZZ6o, demonstrates several examination techniques that can identify the injury.
Wheeless Online Ortho Reference http://www.wheelessonline.com/ortho/posterolateral_rotary_instability_of_the_knee
Category: Orthopedics
Keywords: knee dislocation, ABI, vascular (PubMed Search)
Posted: 9/10/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Evaluation of circulatory status is the most important aspect of post reduction care.
Look for hard findings such as cool/cold lower extremity, diminished or absent pulses, pale or dusky skin, paralysis, etc.
However, the absence of these findings should not lull the clinician into a false sense of security. The degree of initial joint deformity, presence of full bounding pulses and warm skin over the dorsum of the foot can all be present in the setting of vascular injury.
The next step will be to perform an ABI (ankle-brachial index).
In one small study, no patient with an ABI greater than or equal to 0.9 had a vascular injury.
Patients with a reassuring physical exam and ABIs should be admitted for vascular checks without further imaging.
Patients with a reassuring physical examination but with an abnormal ABI should have an imaging study obtained (arteriogram/CT angiogram).
Patients with hard findings of a vascular injury should have an emergent vascular surgery consultation.
The value of the ankle-brachial index for diagnosing arterial injury after knee dislocation: a prospective study.
Category: Orthopedics
Keywords: Sugar Tong Splint (PubMed Search)
Posted: 9/3/2011 by Michael Bond, MD
Click here to contact Michael Bond, MD
Sugar Tong Splint
The sugar tong splint is ideal for splinting fractures of the radius, ulna, or wrist. It prevents flexion and extension at the wrist, limits flexion and extension at the elbow, and prevents supination and pronation. A posterior long arm splint does not prevent supinaton and pronation, therefore, it is of limited use for radius and ulna fractures.
The traditional sugar tong can be difficult to put on a patient without an assistant as it is often hard to hold the splint in position as you begin to ace wrap it. A variation on the sugar tong, the reverse sugar tong, prevents this frustration. The splinting material is cut so that a small piece suspends the splint from the web space between the thumb and index finger. The open ends at the elbow are also easily folded under each other, preventing any bulky splint material from extending out.
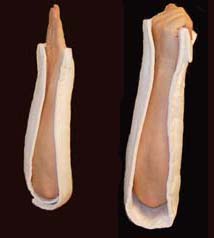
The reverse sugar tong is on the left, the original sugar tong on the right.
Check out this video showing how to place a reverse sugar tong splint.
http://www.youtube.com/watch?v=r-RHdttOMf0
Category: Orthopedics
Keywords: knee dislocation (PubMed Search)
Posted: 8/27/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Stability from 4 major ligaments (ACL, PCL, MCL and LCL)
Knee dislocation causes injury to multiple ligaments (usually 3 of the above).
Many of these dislocation spontaneously reduce prior to medical evaluation. Therefore, consider knee dislocation in a patient with multi ligament injury, significant hemarthrosis and bruising.
Vascular injury in up to 40% (popliteal artery)
Nerve injury in up to 23% (peroneal nerve) ((ankle dorsiflexion and sensation to the first web space of the foot))
After reduction, immobilize knee in 15-20 degrees flexion.
The degree of initial deformity, presence of strong pulses, or warm skin cannot be used to rule out popliteal injury.
Category: Orthopedics
Keywords: Brachial plexus neuritis, neck pain (PubMed Search)
Posted: 8/13/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Acute brachial plexus neuritis is an uncommon disorder that is easily confused with cervical radiculopathy.
Patients present with a characteristic pattern of acute onset of burning pain. Pain subsides in days to weeks and is then followed by profound weakness and muscle wasting changes affecting the shoulder and upper extremity. Weakness is best identified in the deltoid, biceps and rotator cuff muscles. Strength gradually recovers over 3-4 months.
DDX: The constellation of pain, weakness and sensory loss associated with cervical radiculopathy tend to occur simultaneously. Also cervical radiculopathy tends to involve only a single root.
ED treatment is with analgesics and physical therapy and PCP referral for outpatient MRI/EMG. Consider a sling in those with severe shoulder weakness.
Category: Orthopedics
Keywords: Osteomyelitis, hyperbaric oxygen (PubMed Search)
Posted: 7/23/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Refractory Osteomyelitis is defined as a chronic osteomyelitis that persists or recurs after appropriate interventions have been performed or where acute osteomyelitis has not responded to surgery and antibiotics.
Case series, animal data and non-randomized prospective trials suggest that the addition of Hyperbaric Oxygen therapy to routine surgical and antibiotic management of previously refractory osteomyelitis is safe and improves the rate of infection resolution.
In patients with osteomyelitis involving spine, skull, sternum, HBOT is recommended prior to surgical intervention.
Typically patients require 20-40 daily dives for sustained therapeutic benefit.
How does HBOT work in osteomyelitis?
1. Restoration of normal to elevated O2 level in infected bone.
2. Leukocyte mediated killing of aerobic bacteria is restored when low O2 tension intrinsic to osteomyolitic bone is restored to physiologic or supra-physiologic levels.
3. HBOT is noted to exert direct suppressive effects on anaerobic infections.
4. HBOT augment the transport of certain abx (aminoglycosides and cephalosporins) across bacterial cell wall.
5. Enhance osteogenesis
6. Enhance angiogenesis
thank you to Dr. Sethuraman for this pearl
“Refractory Osteomyelitis” written by Hart, Brett, MD In: Hyperbaric Oxygen Therapy Indications Editor: Gesell, Laurie, MD FACEP
Category: Orthopedics
Keywords: Electrolyte abnormalities, marathon runners, troponin (PubMed Search)
Posted: 7/9/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Emergency physicians are often called upon to provide event coverage for marathons.
Prolonged endurance racing is safe for the majority of participants.
Hyponatremia (8.2% - 13.5%) - finishing times of greater than 4 hours is an independent risk factor
Hypokalemia – uncommon
Renal function – BUN > 30 or Cr > 1.4 mg/dL (23.6%). There is no data that this is of any clinical significance.
Cardiac Troponin - (11%) had significant increases (troponin T > or = 0.075 ng/mL or troponin I > or = 0.5 ng/mL). Elevations were more commonly seen with weight loss and increased Cr levels and may be associated with running inexperience (< 5 previous marathons) and young age (< 30 years) though interestingly not with race duration or traditional cardiac risk factors.
Findings are similar for men and women
Cardiac troponin increases among runners in the Boston Marathon.
.Ann Emerg Med. 2007 Feb;49(2):137-43
Prevalence of Hyponatremia, Renal Dysfunction, and Other Electrolyte Abnormalities Among Runners Before and After Completing a Marathon or Half Marathon
Sports Health 145 - 151.
Category: Orthopedics
Keywords: Pes Anserine, Bursitis, knee pain (PubMed Search)
Posted: 6/25/2011 by Brian Corwell, MD
(Updated: 5/2/2026)
Click here to contact Brian Corwell, MD
Pes Anserine Bursitis is an inflammatory condition of the medial knee
Occurs at the bursa of the pes anserinus which overlies the attachment of the 1) Sartorius 2) gracilis and 3) semitendinosis tendons
Note the location is 2-3 inches below the knee joint on the medial side
http://kneespecialistsurgeon.com/images/uploaded/Pes%20anserinus%20bursitis%20image.jpg
http://eso-cdn.bestpractice.bmj.com/best-practice/images/bp/en-gb/575-27_default.jpg
Patients complain of pain (especially with stair climbing)
PE: Tenderness to palpation of the bursa with mild swelling
DDx: MCL tear, medial meniscus injury, medial (knee) compartment arthritis
Treatment: Cessation/modification of offending activities, Icing and ice massage, NSAIDs, hamstring stretching and physical therapy. Failure of the above should prompt referral for bursal steroid injection.
Category: Orthopedics
Keywords: kocher, septic arthri (PubMed Search)
Posted: 6/18/2011 by Michael Bond, MD
(Updated: 5/2/2026)
Click here to contact Michael Bond, MD
Kocher Criteria for Septic Arthritis in Children:
Septic arthritis should be suspected in children that have a painful joint especially if they do not want to weight bear. Orthopedics uses the Kocher Criteria to determine the probability of whether the joint is infected.
Four elements make up the criteria:
If only one sign is present there is a 3% chance the child has a septic joint.
Category: Orthopedics
Keywords: Kienb ck's disease, wrist, avascular necrosis (PubMed Search)
Posted: 6/11/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Kienbock’s disease is a rare entity involving collapse of the lunate due to avascular necrosis and vascular insufficiency.
Occurs most commonly in young adults aged 15 to 40 years.
Cause is unknown but believed to be due to remote trauma or repetitive microtrauma in at risk individuals.
Patients complain of wrist pain, stiffness and swelling
On exam, limited range of motion, decreased grip strength and passive dorsiflexion of the 3rd digit produces pain.
Dx: plain film in the ED and with MRI as an outpatient.
Tx: Wrist immobilization with splint and refer to orthopedics. Ultimate treatment is individualized and there is no clear consensus.
Lunate sclerosis seen on plain film
http://orthoinfo.aaos.org/figures/A00017F02.jpg
AVN of the lunate seen on MRI
http://www.assh.org/Public/HandConditions/PublishingImages/KeinbocksMRI_figure3.JPG
Category: Orthopedics
Keywords: Brachial plexus, stinger, burner (PubMed Search)
Posted: 5/28/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Transient brachial plexopathies aka Burners and Stingers
Brachial plexus injuries are the most common peripheral nerve injuries seen in athletes.
49-65% of all college football players have experienced at least one burner with a 87% recurrence rate.
Injuries most commonly occur at C5-C6 but may involve any root level.
3 Mechanisms: Commonly due to
1) Traction caused by lateral flexion of the neck away from the involved side
2) Compression of the upper plexus between shoulder pads and scapula
3) Nerve compression caused by neck hyperextension and ipsilateral rotation.
CC: Burning or numbness in the neck, shoulder and/or arm
Symptoms are UNILATERAL and tend to usually last seconds to minutes
Symptoms are reproduced by the Spurling maneuver.
Function gradually returns from the proximal muscle groups to the distal muscle groups.
Because most burners are self-limited, the most important goal is to rule out an unstable cervical injury.
