Category: Critical Care
Keywords: peripheral pressors, central line, CVC, CLABSI (PubMed Search)
Posted: 10/4/2023 by William Teeter, MD
Click here to contact William Teeter, MD
Bottom line: As part of a systematic protocol, peripheral pressors administered through a peripheral line greater 22Ga or larger reduced the number of days of central venous catheter (CVC) use in a MICU population at an academic medical center. 35 (5.5%) patients had an extravasation event all with “minimal” tissue injury complications. None required surgery. 51.6% of patients did not require a CVC as a result of the protocol
Details
Notes on protocol
PIV were placed and confirmed with US, were between wrist and AC fossa with q2h patency checks. Max allowable dose of NE 15 mcg/min with requirement that patients be able to report pain at site. Initially, max infusion time was set at 48h but was eventually liberalized to indefinite use.
https://pubmed.ncbi.nlm.nih.gov/37611862/
Category: Critical Care
Keywords: BRASH, shock, av nodal blockers (PubMed Search)
Posted: 9/20/2023 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
The BRASH syndrome (Bradycardia, Renal failure, AV nodal blockade, Shock, Hyperkalemia) has been increasingly described in the literature in the past 3-5 years.
The inciting factor is generally considered to be something that prompts acute kidney injury, often hypovolemia of some sort. Rather than AV nodal blocker overdose or severe hyperkalemia causing conduction problems, the combination of AV nodal blocker use (most often beta-blockers, but can be any type) and hyperkalemia (often only moderate) has a synergistic effect on cardiac conduction with ensuing bradycardia that can devolve into a cycle of worsening renal perfusion and shock.
Treatment is supportive, but most effective when the syndrome is recognized and all parts simultaneously managed. ED physicians should be familiar with its existence for targeted whole-syndrome stabilization and to avoid diagnostic delay.
Category: Critical Care
Keywords: NIPPV, CPAP, HFNC, High Flow, Respiratory Failure (PubMed Search)
Posted: 9/12/2023 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
When patients fail simple respiratory support therapies like nasal cannula or non-rebreather, it is often a point of debate whether to move next to High Flow Nasal Cannula (HFNC) or Noninvasive Positive Pressure Ventilation (NIPPV). This study randomized patients in acute respiratory failure (ARF) to CPAP, a form of NIPPV, vs HFNC. They looked at all comers in ARF, and primary outcome was need for intubation. Importantly, they excluded asthma/COPD exacerbation, for which BiPAP is typically considered the first line therapy due to improved CO2 clearance.
They found a significantly lower number of patients required intubation in the CPAP (28.9%) group than the HFNC (42.6%) group (p=0.006). They hypothesized that the enhanced PEEP improved oxygenation (hypoxia being a common trigger for moving to intubation), but as opposed to BiPAP, the lack of additional driving pressure limited tidal volumes and Patient Self-Inflicted Lung Injury (P-SILI), which is a known mechanism of ARDS and mortality. They use this argument to explain why trials like FLORALI, pitting HFNC vs BiPAP, tend to not find an advantage for the NIPPV arm. While this rationale makes sense, it should be noted that the study does not directly investigate if this was the reason for the difference, and for what its worth the inverse argument that using driving pressure to reduce respiratory rate, hypercarbia, and work of breathing (other very common indications for intubation) would also theoretically reduce intubations. Furthermore, it's not clear why reducing P-SILI, which tends to cause mortality on a much longer duration, would improve the short-term outcome of need for intubation.
Bottom Line: This study demonstrated a benefit to CPAP over HFNC in terms of decreasing need for intubation amongst non-asthma/non-COPD patients with acute respiratory failure, and offered a physiologic rationale but one that requires further verification and discussion. While it may be reasonable to choose CPAP instead of HFNC in marginal patients at risk of intubation (but stable enough to trial noninvasive support first), in my opinion more studies are likely needed before a wholesale change in practice. The study also does not take into consideration the enhanced comfort and compliance we tend to see with HFNC over NIPPV, which should be considered as well.
Nagata K, Yokoyama T, Tsugitomi R, Nakashima H, Kuraishi H, Ohshimo S, Mori Y, Sakuraya M, Kagami R, Tanigawa M, Tobino K, Kamo T, Kadowaki T, Koga Y, Ogata Y, Nishimura N, Kondoh Y, Taniuchi S, Shintani A, Tomii K; JaNP-Hi Study Investigators. Continuous positive airway pressure versus high-flow nasal cannula oxygen therapy for acute hypoxemic respiratory failure: A randomized controlled trial. Respirology. 2023 Aug 30. doi: 10.1111/resp.14588. Epub ahead of print. PMID: 37648252.
Category: Critical Care
Posted: 9/5/2023 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Pearls for the Patient in Cardiogenic Shock
Jentzer JC, et al. Advances in the management of cardiogenic shock. Crit Care Med. 2023; 51:1222-1233.
Category: Critical Care
Keywords: arterial cannulation, axillary artery, femoral artery, infraclavicular (PubMed Search)
Posted: 8/21/2023 by Quincy Tran, MD, PhD
Click here to contact Quincy Tran, MD, PhD
Settings: Single ICU in Poland, randomized trial
Participants: intubated patients who needed arterial catheter placement. Patients who had adequate access to one axillary and one femoral artery were eligible.
Patients were randomized 1:1 for axillary or femoral artery cannulation.
Outcome measurement: Primary outcome was cannulation success rate. Secondary outcomes were first pass success rate, number of attempts.
Study Results:
Discussion:
Conclusion:
Ultrasound-guided cannulation of the axillary artery via the infraclavicular route is non-inferior to the cannulation of the common femoral artery. When cannulation of the radial or femoral artery is not available, we can consider axillary artery via the infraclavicular approach.
Reference:
Gawda, Ryszard MD, PhD; Marszalski, Maciej MD; Piwoda, Maciej MD; Molsa, Maciej MD; Pietka, Marek MD; Filipiak, Kamil MD; Miechowicz, Izabela PhD; Czarnik, Tomasz MD, PhD1. Infraclavicular, Ultrasound-Guided Percutaneous Approach to the Axillary Artery for Arterial Catheter Placement: A Randomized Trial. Critical Care Medicine ():10.1097/CCM.0000000000006015, August 07, 2023. | DOI: 10.1097/CCM.0000000000006015
Category: Critical Care
Posted: 8/15/2023 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Background:
There has been interest in vitamin C as an adjunctive therapy in patients with systemic inflammation and vasoplegia to reduce inflammation. While it was suggested that vitamin C may have some benefit (along with hydrocortisone and thiamine) in septic shock, the LOVIT trial showed possible harm from high-dose vitamin C administration in septic ICU patients. The VALENCIA trial sought to evaluate whether vitamin C could reduce the duration of vasopressor therapy in patients with moderate vasoplegic shock.
Study:
-double-blinded RCT at two tertiary centers, 71 patients (36 to placebo, 35 to vitamin C)
-adult patients with vasoplegic shock of any cause
-vasopressor requirement >10 μg/min of norepi after hypovolemia was excluded
-notable exclusion criteria: end-stage renal failure and expected survival <12 hrs
Results:
-65 pts with septic shock, 6 pts with non-infectious cause
-no significant difference in the duration of vasopressors between the treatment group (median, 44 h [95% CI, 37-54 hrs]) and the control group (55 hrs [95% CI, 33-66 hrs])
-also no statistically significant difference in the vasopressor dose at 12 hourly time points, ICU or 28-day mortality and ICU or hospital length of stay
Take-home points:
Small study that ultimately may be under-powered but did not show that vitamin C reduces vasopressor duration in moderate vasoplegic shock
Anstey MH, Aljeaidi MS, Palmer R, et al. Intravenous vitamin C for vasoplegia: A double-blinded randomised clinical trial (VALENCIA trial). Journal of Critical Care. 2023;78:154369.
Category: Critical Care
Posted: 8/8/2023 by William Teeter, MD
Click here to contact William Teeter, MD
Targeted Therapeutic Mild Hypercapnia after Resuscitated Cardiac Arrest (TAME)
Current guidelines recommend normocapnia for out-of-hospital cardiac arrest (OHCA), the TAME Study asked is mild hypercapnia better?
Conclusion: "In patients with coma who were resuscitated after out-of-hospital cardiac arrest, targeted mild hypercapnia did not lead to better neurologic outcomes at 6 months than targeted normocapnia."
https://www.nejm.org/doi/full/10.1056/NEJMoa2214552
https://clinicaltrials.gov/study/NCT03114033
https://www.thebottomline.org.uk/blog/ebm/tame/
Category: Critical Care
Keywords: OHCA, ROSC, cardiac arrest, resuscitation, CT, pan-scan, computed tomography (PubMed Search)
Posted: 7/25/2023 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Background: Prior evidence1,2 has suggested that early “pan-scan” after ROSC provides clinically-relevant information that assists in the care of the patient in question, when the cause of OHCA is unclear.
The recent CT FIRST trial looked at patients pre- and post- implementation of a protocol for head-to-pelvis CT within 6 hours of ROSC for adult patients without known cause or evidence of possible cardiac etiology, stable enough for scan. *Patients with GFR <30 were excluded from assignment to CT, although were included in the post/CT cohort if their treating doctors ordered CT scans based on perceived clinical need. To balance this, a similar number of patients with GFR <30 were included in the pre/“standard of care” cohort.
Outcomes After Protocol (Pre- vs. Post-):
Bottom Line: Early pan-CT allows for earlier definitive diagnosis and stabilization without increase in adverse events. While this earlier diagnosis does not seem to yield better survival, earlier stabilization may provide some benefits in terms of resource allocation and disposition, a notable benefit during our current crisis of staffing shortages and ED boarding.
Category: Critical Care
Keywords: Central Lines, Platelets, Bleeding (PubMed Search)
Posted: 7/18/2023 by Mark Sutherland, MD
(Updated: 5/6/2026)
Click here to contact Mark Sutherland, MD
Central Venous Catheter (CVC; aka central line) placement is a common procedure in both the ED and ICU, and while overall quite safe, does carry some risk. In particular, many of us regularly are confronted with the challenge of placing a line in a patient with profound thrombocytopenia, which can result in significant bleeding. In these cases, should we give platelets before we place the line?
Van Baarle et al published a randomized study in NEJM comparing an empiric 1u platelet transfusion vs no transfusion in patients with a platelet count of 10,000-50,000, prior to line placement. The study included both HD and non-HD (e.g. TLC) lines, from all three major access sites, in patients in their ICU or hematology ward. They found statistically fewer serious bleeding events in the transfusion group (4.8%) vs no transfusion group (11.9%). The study wasn't powered to look at more patient oriented outcomes like mortality, but I'm sure we can all agree less bleeding is probably a good thing. Also importantly, this study did not evaluate the risks/benefits of delaying line placement to obtain platelets when the line is urgently needed, so I would not recommend extending this to conclude platelets must be given before line placement if the line is needed for something highly time-sensitive (e.g. only available access to infuse pressors in a hypotensive patient).
Bottom Line: It is probably beneficial and appropriate to provide prophylactic platelet transfusion prior to CVC placement in patients with a platelet count less than 50,000, assuming circumstances allow.
van Baarle FLF, van de Weerdt EK, van der Velden WJFM, Ruiterkamp RA, Tuinman PR, Ypma PF, van den Bergh WM, Demandt AMP, Kerver ED, Jansen AJG, Westerweel PE, Arbous SM, Determann RM, van Mook WNKA, Koeman M, Mäkelburg ABU, van Lienden KP, Binnekade JM, Biemond BJ, Vlaar APJ. Platelet Transfusion before CVC Placement in Patients with Thrombocytopenia. N Engl J Med. 2023 May 25;388(21):1956-1965. doi: 10.1056/NEJMoa2214322. PMID: 37224197.
https://www.nejm.org/doi/10.1056/NEJMoa2214322
Category: Critical Care
Keywords: NEWS, MEWS, IEWS, international Early Warning Score, mortality (PubMed Search)
Posted: 6/27/2023 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Settings: Retrospective data from 3 Dutch EDs (development of the score), 2 Denmark ED (for validation of the score). The novel score (International Early Warning Score) will be composed of the National Early Warning Score (NEWS) + Age +Sex
Components of the National Early Warning Score:
Participants: All adult patients in the Netherlands Emergency department Evaluation Database (NEED) and Danish Multicenter Cohort (DMC).
Outcome measurement: in-hospital mortality, including death in EDs.
Study Results:
Discussion:
Conclusion:
This multicenter study showed that IEWS perform better than the NEWS for predicting in-hospital mortality for ED patients.
Candel BGJ, Nissen SK, Nickel CH, Raven W, Thijssen W, Gaakeer MI, Lassen AT, Brabrand M, Steyerberg EW, de Jonge E, de Groot B. Development and External Validation of the International Early Warning Score for Improved Age- and Sex-Adjusted In-Hospital Mortality Prediction in the Emergency Department. Crit Care Med. 2023 Jul 1;51(7):881-891. doi: 10.1097/CCM.0000000000005842. Epub 2023 Mar 23. PMID: 36951452; PMCID: PMC10262984.
Category: Critical Care
Keywords: Upper GI Hemorrhage, Cirrhosis, Antibiotic Prophylaxis, SBP, ceftriaxone (PubMed Search)
Posted: 6/6/2023 by Zach Rogers, MD
(Updated: 5/6/2026)
Click here to contact Zach Rogers, MD
Prophylactic antibiotic use in cirrhotic patients with an upper GI bleed has been demonstrated to have a mortality benefit in multiple randomized clinical trials. Some trials as well demonstrated a decreased risk of rebleeding as well as a shorter hospital length of stay (1,2).
The exact means of protection is not entirely clear and its benefit is seen in both variceal and nonvariceal hemorrhages as well as in cirrhotic patient both with and without ascites.
There does appears to be a close interplay between cirrhosis bleeding risk and infection, with infection being a common precipitating factor for upper GI bleed.
The antibiotic of choice is ceftriaxone 1 gram IV daily for seven days. Although in case of allergy/intolerance, fluoroquinolones or aminoglycosides may be used as alternatives (3).
Bottom line:
All forms of upper GI hemorrhage in cirrhotic patients warrant prophylactic antibiotic use (regardless of the presence of ascites) as well as a diligent search and exclusion of possible infectious sources.
1. Chavez-Tapia NC, Barrientos-Gutierrez T, Tellez-Avila FI, Soares-Weiser K, Uribe M. Antibiotic prophylaxis for cirrhotic patients with upper gastrointestinal bleeding. Cochrane Database Syst Rev. 2010 Sep 8;2010(9):CD002907. doi: 10.1002/14651858.CD002907.pub2. PMID: 20824832; PMCID: PMC7138054.
2. Wong YJ, Tan CK, Yii YL, et al. Antibiotic prophylaxis in cirrhosis patients with upper gastrointestinal bleeding: An updated systematic review and meta?analysis. Portal Hypertension & Cirrhosis. 2022;1(3):167-177. doi:10.1002/poh2.35
3. Sanchez?Jimenez B, Chavez?Tapia NC, Jakobsen JC, Nikolova D, Gluud C. Antibiotic prophylaxis for people with cirrhosis and variceal bleeding. Cochrane Database Syst Rev. 2018 Dec 4;2018(12):CD013214. doi: 10.1002/14651858.CD013214. PMCID: PMC6517118.
Category: Critical Care
Keywords: thrombocytopenia, bleeding, hemorrhage, platelets, transfusions, central lines, CVCs (PubMed Search)
Posted: 5/30/2023 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Background: In general practice, platelets are typically transfused for invasive procedures when the platelet count falls below 50 x 109/L. Regarding the placement of central venous catheters (CVCs), there is minimal data to support or refute decisions to transfuse platelets in these patients, although the 2015 Clinical Practice Guideline from the AABB (formerly, the American Association of Blood Banks) recommends deferring platelet transfusion until a platelet count of 20 x 109/L for CVC placement [weak recommendation, low quality evidence].1
In a study published this month in NEJM,2 van Baarle et al. performed a multicenter randomized controlled noninferiority trial comparing platelet transfusion to no transfusion in patients with platelets 10 to 50 x 109/L prior to US-guided CVC insertion. The primary outcome was the occurrence of catheter-related bleeding Grades 2-4 (Grade 1 = oozing; managed with <20 min of manual compression, not requiring RBC transfusion, & Grades 2-4 is everything else up to death) within 24 hours post-procedure.
Bottom Line: The jury is still out on best platelet transfusion practices prior to CVC placement, but I would strongly consider prophylactic platelet transfusion in patients with platelets < 30 x 109/L, those with underlying hematologic malignancy, and patients receiving larger CVCs such as dialysis lines. How much to transfuse in those with more severe thrombocytopenia is uncertain.
Separately, I would also strongly recommend use of US-guidance for any CVC placement in this population as well, based on practical common sense and some supportive literature as well.5
Additional Background: Data in pediatric oncology patients indicates that CVC placement with platelets <50 x 109/L is associated w/ increased occurence of minor but not major post-procedure bleeding,3 while adult data indicates that CVC placement can be performed until a threshold of 20 x 109/L before transfusions are needed to prevent severe bleeding.4
Additional Study Data:
Category: Critical Care
Keywords: Intubation, Trauma, Cervical Spine, Laryngoscopy (PubMed Search)
Posted: 5/23/2023 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Ability to move the head and neck freely can be clutch in endotracheal intubation, so in patients such as certain trauma patients who may have c-spine instability and need to be immobilized, it's all the more important to choose the optimal intubation approach to maximize success and minimize head movement.
Choi et al recently published a study in Anesthesia looking at:
-Video laryngoscopy with a standard geometry Mac blade
vs
-Fiberoptic intubation
as the initial method for intubating patients in c-collars about to undergo spinal surgery. This is an interesting contrast between two extremes, as standard geometry is the most "traditional" approach, whereas fiberoptic is kind of the opposite end of the spectrum, jumping to a more advanced method which might be more flexible (no pun intended) but also introduces new complexities.
All outcomes actually favored standard geometry VL over fiberoptic, including first pass success (98% vs 91%), time to intubation (50s vs 81s) and need for additional airway maneuvers (18% vs 56%). There was no difference in complication rates, although a bigger study might be needed to find rare complications (this study had 330 patients).
In my opinion, it's unfortunate they didn't include hyperangulated VL, as it would be interesting to see how this approach compares. Personally I think of hyperangulated VL in these patients as a nice blend of the two methods, bringing the familiarity and speed of typical VL intubation, but often requiring less neck movement like fiberoptic.
Bottom Line: This study does not support a fiberoptic first approach to intubating patients with cervical spine instability. In fact, it may cause harm.
Choi S, Yoo HK, Shin KW, Kim YJ, Yoon HK, Park HP, Oh H. Videolaryngoscopy vs. flexible fibrescopy for tracheal intubation in patients with cervical spine immobilisation: a randomised controlled trial. Anaesthesia. 2023 May 5. doi: 10.1111/anae.16035. Epub ahead of print. PMID: 37145935.
Category: Critical Care
Posted: 5/16/2023 by Mike Winters, MBA, MD
(Updated: 5/6/2026)
Click here to contact Mike Winters, MBA, MD
Bicarbonate Use for Lactic Acidosis?
Wardi G, et al. A review of bicarbonate use in common clinical scenarios. J Emerg Med. 2023; online ahead of print.
Category: Critical Care
Keywords: OHCA, Critical Care, Whole Body CT, Post Cardiac Arrest Care (PubMed Search)
Posted: 5/9/2023 by Lucas Sjeklocha, MD
Click here to contact Lucas Sjeklocha, MD
Just scan ‘em? Should everyone with unexplained out-of-hospital cardiac arrest get whole-body CT/CTA?
Background: Determination of the cause and subsequent management of out-of-hospital cardiac arrest is clinically challenging in those patients who survive to hospital admission without a clear diagnosis. CT imaging is often used to ascertain the cause of an arrest, find potentially intervenable etiologies, and assess for neurological injury but this practice and diagnostic yield are inconsistent and not well studied.
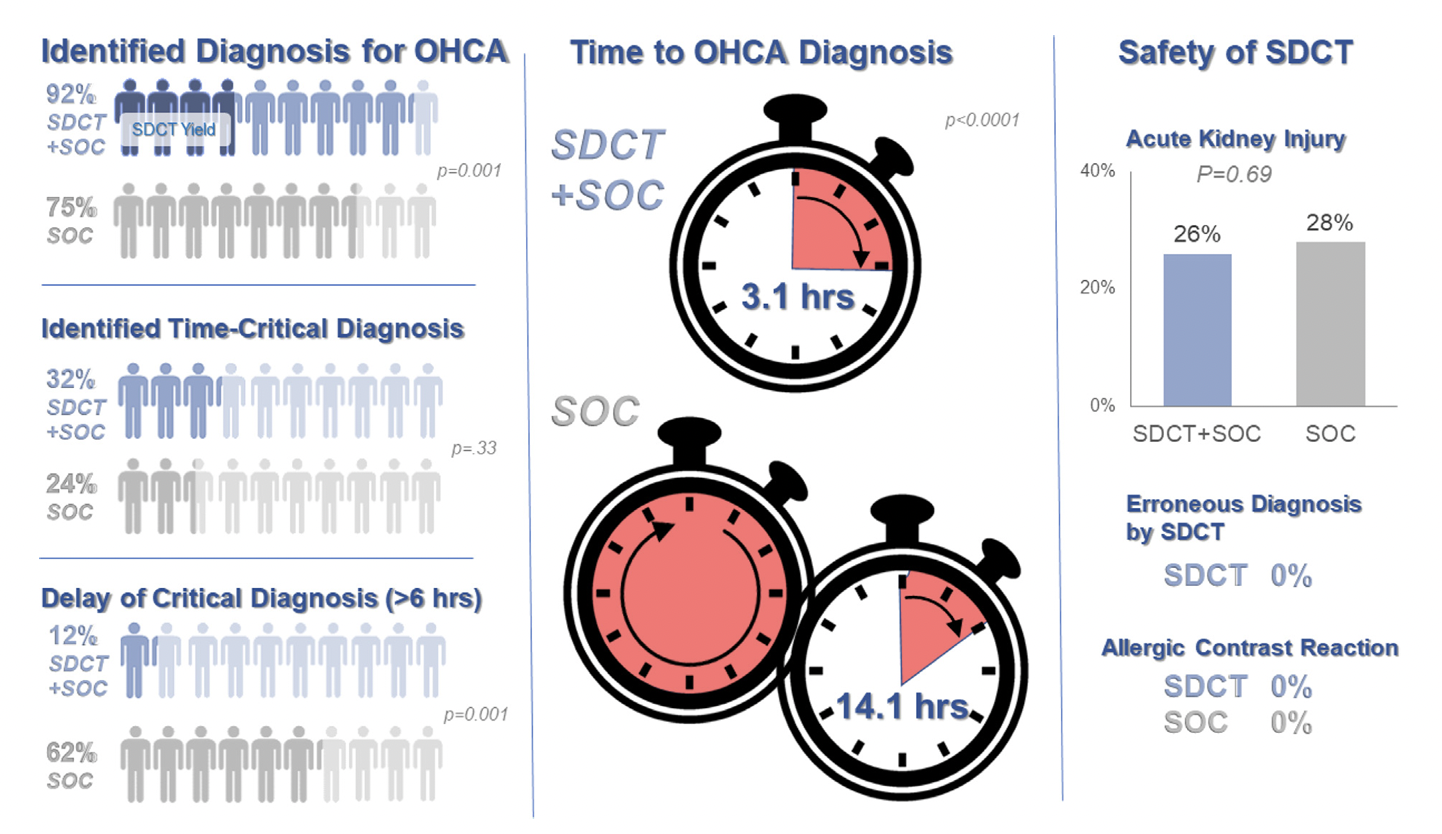
Study and Methods: The CT FIRST study is a single center cohort study using head-to-pelvis contrasted triple phase CT within 6 hours for cardiac arrest without obvious cause (sudden death CT or SDCT) studied in a before and after manner compared to usual care to determine the influence of early pan CT on diagnostic yield and outcomes. The primary outcome was diagnostic yield following SDCT and secondary outcomes include time to diagnosis of “time critical” findings and survival to discharge. 104 patients undergoing SDCT were compared to 143 historical controls after study implementation. Patients deemed to have a clear cause or are too unstable for CT were among exclusions.
Results: For the primary outcome of diagnostic yield: 92% of SDCT cohort received a separately adjudicated diagnosis for the arrest compared to 75% of the control cohort (p = 0.001). With time to such diagnosis of 3.1hrs in SDCT versus 14.1hrs of controls, with 39% versus 17% being made by CT. Time critical diagnoses including MI, PE, aortic dissection, pneumonia, embolic or hemorrhagic CVA and abdominal catastrophe were identified in 32% versus 24% (non significant) of the cohorts with delay greater than 6hrs to diagnosis reported in 12% in SDCT versus 62% in usual care (p=0.001).
There was no difference in survival to hospital discharge and no difference in safety measures and no evaluation reporting changes to and timing of patient managements.
The SDCT cohort had 100% scan rate compared to usual care where 81% received early head CT with chest CT and abdominal CT done in 36% and 18%, respectively. Notably there were no CT reported diagnoses that were later reversed on adjudication in either cohort. The planned economic and resource analysis was not reported in this study.
Discussion: There was a notable increase in diagnostic yield based on the study design with faster time to potentially time sensitive diagnoses. There were, however, no differences in mortality and it was not clear the degree to which these diagnoses influenced patient management given the limited numbers in this study and diverse set of diagnoses associated with cardiac arrest. Like previous studies of selective versus whole body CT in trauma populations, the increased diagnostic yield was not associated with reduced mortality or reported changes in management. The yield numbers suggest increased confidence by exclusion as much as positive findings of the cause. As always, the caveats of a relatively small single center before-and-after cohort study apply.
An interesting twist is that no CT diagnosis pointing to the cause of the arrest was reversed on subsequent review, this may speak to the accuracy of modern CT and radiology interpretation, but I sometimes worry that this can also be reflective of diagnostic fixation, especially with “objective” tests, as well as nihilism about the utility of clinical diagnosis.
That said, non-selective CT has many potential benefits for many critically ill and unexaminable populations with diagnostic uncertainty, as demonstrated here, which must be balanced against risks of intrahospital transport and of resource utilization as we do not yet have clear data that patients benefit from the practice despite increased diagnostic yield.
Kelley R.H. Branch, M.O. Gatewood, P.J. Kudenchuk et al., Diagnostic yield, safety, and outcomes of Head-to-pelvis sudden death CT imaging in post arrest care: The CT FIRST cohort study, Resuscitation, https://doi.org/10.1016/j. resuscitation.2023.109785
Category: Critical Care
Keywords: etomidate, intubation, critically ill, mortality (PubMed Search)
Posted: 5/2/2023 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
As emergency physicians, we use etomidate to intubate patients most of the time, although there was controversy whether etomidate would suppress critically ill patients’ cortisol production. Whether etomidate was associated with mortality was controversial. A recent meta-analysis investigated the issue again.
Methods: meta-analysis of randomized trials using etomidate for intubation versus other agents. Outcome = mortality as defined by the authors. Mortality was defined from 24 hours to 30 days by study’s authors.
Results: 11 RCTs, including one new RCT in 2022
319 (1359, 23%) patients received etomidate died vs. 267 (1345, 20%) receiving other agents died; Risk Ratio 1.16, 95% CI 1.01-1.33, P = 0.03.
Etomidate was also associated with higher risk ratio for adrenal insufficiency, when compared with other control agents (147/695, 21% vs. 69/686, 10%, RR 2.01, 95% CI (1.59-2.56), P < 0.01.
Etomidate was also associated with higher risk ratio of mortality, when compared with ketamine, for mortality, as defined by each study’s author (273/1201, 23% vs. 226/1198. 19%. RR 1.18, 95% CI 1.02-1.37, P = 0.03).
Discussion:
The authors used fixed effects model, as they claimed that their meta-analysis had low heterogeneity (I2 =0%). However, fixed effects model should only be used when there is no difference among patient population. In this study, the outcome definitions were different, the patient populations were different (trauma, pre-hospital, ED, ICU). Therefore, random effects model should be used. Random effects models tend to yield larger 95% CI, thus, more likely yield non-statistically significant results.
The authors claimed a Number Needed To Treat (NNT) for etomidate of 31, so basically many ED patients would die, while most of patients being intubated by Anesthesiology, regarding settings, would not die, as anesthesiologists mostly use propofol.
Category: Critical Care
Posted: 4/25/2023 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Hypoxemic respiratory failure is a common presentation of critically ill patients. If the degree of hypoxemia is severe and disproportionate to the patient's radiographic findings and not responding to increasing FiO2, a right-to-left shunt should be considered. To evaluate for an anatomic shunt, an intravenous agitated saline contrast (ASC) echocardiographic evaluation can be conducted by an ED provider at the bedside.
Technique:
Interpretation:
Millington SJ, Mayo-Malasky H, Koenig S. Agitated saline contrast injection in patients with severe hypoxemia. J Intensive Care Med. 2023;38(5):479-486.
Category: Critical Care
Posted: 4/20/2023 by William Teeter, MD
Click here to contact William Teeter, MD
CCM recently published Stanford's experience with their Emergency Critical Care Program (ECCP), an ED based intensivist consultation/management model staffed by EM/CC during peak hours with the "goals of improving care of the critically ill in the ED, offloading the ED team, and optimizing ICU bed utilization without the need for a dedicated physical space."
Conclusions:
This is the third group to document decrease in overall mortality utilizing an early or dedicated critical care consult model. EC3 and the CCRU here at UMMC have also both shown improvements in patient transfer and resource utilization metrics. As with all studies in this space, there are many limitations to these studies in both design and generalizability, even amongst each other. However, the literature is replete with data that increased boarding time in the ED for critically ill patients is associated with worse outcomes and these studies are now a body of complementary and growing evidence that teams such as this can perhaps bridge that gap. Hopefully come to an ED near you soon...
Study Details:
Objectives: To determine whether implementation of an Emergency Critical Care Program (ECCP) is associated with improved survival and early downgrade of critically ill medical patients in the emergency department (ED).
Design: Single-center, retrospective cohort study from a tertiary academic medical center using ED-visit data between 2015 and 2019 for adult medical patients presenting to the ED with a critical care admission order within 12 hours of arrival.
Pre and post intervention (2017) cohort analysis of patients when facility implemented dedicated bedside critical care by an ED-based intensivist "following initial resuscitation by the ED team". A difference-in-differences (DiD) analysis compared the change in outcomes for patients arriving during ECCP hours (2 pm to midnight, weekdays) between the preintervention period (2015–2017) and the intervention period (2017–2019) to the change in outcomes for patients arriving during non-ECCP hours (all other hours).
Primary outcomes: In-hospital mortality and proportion of patients downgraded to non-ICU status while in the ED within 6 hours
Results:
Mitarai, Tsuyoshi; Gordon, Alexandra June; Nudelman, Matthew J et al. Association of an Emergency Critical Care Program With Survival and Early Downgrade Among Critically Ill Medical Patients in the Emergency Department. Critical Care Medicine ():10.1097/CCM.0000000000005835.
Gunnerson KJ, Bassin BS, Havey RA, et al.: Association of an emergency department–based intensive care unit with survival and inpatient intensive care unit admissions. JAMA Netw Open 2019; 2:e197584
Tran QK, O’Connor J, Vesselinov R, et al.: The critical care resuscitation unit transfers more patients from emergency departments faster and is associated with improved outcomes. J Emerg Med 2020; 58:280–289
Category: Critical Care
Keywords: Glucagon, Beta Blocker, Calcium Channel Blocker, Overdose (PubMed Search)
Posted: 4/11/2023 by Zach Rogers, MD
Click here to contact Zach Rogers, MD
Glucagon therapy in beta blocker and calcium channel blocker overdose is controversial and no high level evidence is available to support or refute its use in overdose treatment.
Glucagon has the ability to bypass adrenergic blockade from beta and calcium channel blocking agents and theoretically increase myocardial contraction, increase heart rate, and increase AV conduction through cyclic AMP production.
However, practically, the use of glucagon is limited due to high risk of vomiting and subsequent risk of aspiration with administration as well as the high cost and limited hospital stock available for continued use.
Given these limitations, glucagon therapy is no longer recommended for calcium channel blocker overdose in the 2017 Critical Care Medicine Expert Consensus*. The use in beta blocker therapy is still recommended. However, caution must be taken to ensure that more advanced (and possibly more efficacious) therapies such as vasopressors and high dose insulin are administered without delay.
The dose of glucagon therapy for this indication is 3-10 mg IV. You can repeat this dose a second time if no response is seen with the first dose. If clinical response is seen with bolus dosing, transition to continuous infusion at the dose of clinical response (eg. if two 5 mg boluses produced the desired response; start 10 mg/hr infusion). Antiemetic administration prior to initial bolus dose is highly recommended to avoid vomiting.
Peterson CD, Leeder JS, Sterner S. Glucagon therapy for beta-blocker overdose. Drug Intell Clin Pharm. 1984 May;18(5):394-8. doi: 10.1177/106002808401800507. PMID: 6144498.
*St-Onge M, Anseeuw K, Cantrell FL, Gilchrist IC, Hantson P, Bailey B, Lavergne V, Gosselin S, Kerns W 2nd, Laliberté M, Lavonas EJ, Juurlink DN, Muscedere J, Yang CC, Sinuff T, Rieder M, Mégarbane B. Experts Consensus Recommendations for the Management of Calcium Channel Blocker Poisoning in Adults. Crit Care Med. 2017 Mar;45(3):e306-e315. doi: 10.1097/CCM.0000000000002087. PMID: 27749343; PMCID: PMC5312725.
Khalid MM, Galuska MA, Hamilton RJ. Beta-Blocker Toxicity. [Updated 2023 Feb 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448097/
Category: Critical Care
Keywords: pneumonia, acute hypoxic respiratory failure, steroids (PubMed Search)
Posted: 4/5/2023 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Background: The use of steroids in pneumonia has long been controversial with conflicting data, and the recent ESCAPe randomized controlled trial by Meduri et al. showing no mortality benefit with their use, but likely underpowered due to recruitment issues. The recently published CAPE COD study by Dequin et al. may change the game.
Design: Double-blind, placebo-controlled, multicenter, RCT
Intervention: Early hydrocortisone within 24 hrs, 200mg/day x 4-8 days depending on improvement, then preset taper
Primary outcome: Death at 28 days
Secondary outcomes:
Bottom Line: The addition of hydrocortisone to antibiotics in severe CAP may decrease need for intubation and development of shock, and in this well-done study, decreased 28 and 90-day mortality.
Meduri GU, Shih MC, Bridges L, et al; ESCAPe Study Group. Low-dose methylprednisolone treatment in critically ill patients with severe community-acquired pneumonia. Intensive Care Med. 2022 Aug;48(8):1009-1023. doi: 10.1007/s00134-022-06684-3. Epub 2022 May 13. PMID: 35723686.
doi: 10.1056/NEJMoa2215145. Epub ahead of print. PMID: 36942789.
