Category: Geriatrics
Keywords: Prescribing cascade (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 4/30/2026)
Click here to contact Robert Flint, MD
The article outlines how instead of looking at medications as the cause of symptoms, we often add more medications to treat the medication induced symptoms. Here is an example of how we get to polypharmacy in older patients
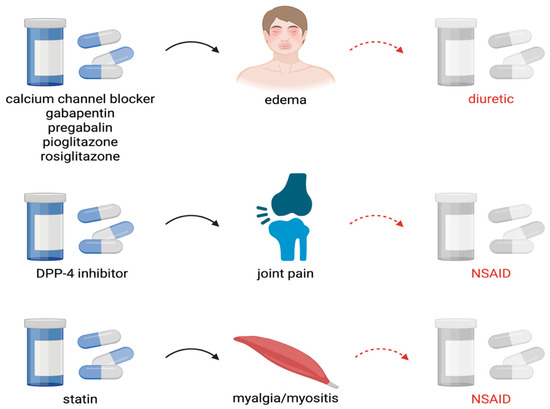
Bry?a A, Woro? J, Miedziaszczyk M, Lorkowska-Zawicka B, Bujak-Gi?ycka B, Orzechowski D, Po?etek P, Pa?ys W. Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity. Geriatrics. 2026; 11(2):37. https://doi.org/10.3390/geriatrics11020037
Category: Trauma
Keywords: Body armor, blunt injury, BABT (PubMed Search)
Posted: 4/26/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Body armor/ bullet resistant vests used by law enforcement are designed to stop penetration by handgun rounds. These rounds have less velocity than rifle rounds. When caring for someone who has been shot while wearing body armor, verify no penetration has occurred and then look for blunt injuries such as rib fractures, liver injuries, pneumothorax, cardiac contusion, vertebral injury, etc. Behind Armor Blunt Trauma (BABT) is the technical term for injuries caused by the transfer of kinetic energy that occurs when these vests are struck.
Volume 49, Issue 7, July 2018, Pages 1251-1257
Author links open overlay panelRosalind M. Jennings a, Chris Malbon b, Fiona Brock a, Stuart Harrisson c, Debra J. Carr b
Category: Trauma
Keywords: trauma, chronic pain, (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/23/2026)
Click here to contact Robert Flint, MD
This narrative review of the trauma literature looking at chronic pain after trauma found:
Kussé M, Hans G, Saldien V, Wildemeersch D. Chronic pain following major trauma: Prevalence, predictive models, and risk factors across common injury types. Trauma. 2026;0(0). doi:10.1177/14604086251404750
Category: Trauma
Keywords: obesity, trauma, mortality, organ failure, sepsis, ARDS (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/18/2026)
Click here to contact Robert Flint, MD
This German retrospective review of 1500 level one trauma center patients (ICU level or ISS over 9) found obesity was an independent predictor of ARDS, multisystem organ failure, and sepsis but not pneumonia or mortality.
Erdle, B., Mangold, J., Kalbhenn, J. et al. BMI is independently associated with ARDS, sepsis and multiorgan failure after major trauma—results of a high-volume retrospective observational cohort study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01603-7
Category: EMS
Keywords: prehospital, EMS, ultrasound (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/12/2026)
Click here to contact Robert Flint, MD
This German retrospective study compared the prehospital use of ultrasound by trained paramedics and compared their findings to in-hospital diagnosis and image results. The authors found:
“Diagnostic accuracy, defined as the concordance between prehospital POCUS-based working diagnoses and final in-hospital diagnoses, was particularly strong for lung ultrasound (pneumothorax, pulmonary edema, pneumonia and pleural effusion; sensitivity 91.7%, specificity 100%) and eFAST (sensitivity 100%, specificity 96.5%), while for the abdominal ultrasound examinations, the specificity was 70% and sensitivity was 71.43%.”
This study sets the stage for future prospective work looking at prehospital US use by paramedics.
Boehm, A., Bexten, T., Stanley, M. et al. Feasibility and diagnostic accuracy of paramedic-performed prehospital point-of-care ultrasound: a retrospective observational study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01595-4
Category: Trauma
Keywords: trauma, treatment disparity, gender (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/8/2026)
Click here to contact Robert Flint, MD
This systematic literature review looking at gender differences in trauma care reveals:
Ghika-Nanchen, A., Marzorati, L., Merra, A. et al. Sex and gender bias in major trauma care: a scoping review. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01596-3
Category: Geriatrics
Keywords: prehospital, geriatric, education (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/5/2026)
Click here to contact Robert Flint, MD
A modified 2 round Delphi study was used to create 57 learning objectives in geriatric care for European prehospital providers. Based on in-hospital learning objectives and literature, these experts came up with what appears to be a very reasonable and helpful list of education objectives for pre-hospital providers that could easily apply to emergency medicine learners as a whole. Here is their table:
https://link.springer.com/article/10.1186/s13049-026-01550-3/tables/3
Krohn, JN., Barrett, J., Heeren, P. et al. A European paramedic curriculum for geriatric emergency medicine developed via a modified Delphi technique. Scand J Trauma Resusc Emerg Med 34, 14 (2026). https://doi.org/10.1186/s13049-026-01550-3
Category: Trauma
Keywords: splenic injury, geriatrics, mortality (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
In this retrospective cohort study looking at splenic injury management and outcomes in the UK, patients over age 65 had much higher mortality and were more often managed conservatively (vs splenectomy or embolization) despite having a lower splenic injury grade and lower overall injury severity score compared to those under 65. Many factors are possible here including frailty, reluctance to intervene in older patients, and lower mechanism of injury bias away from evaluation and management.
Jenkins P, Anton B, Blair G, et al. Traumatic splenic injury in the elderly population: Does management choice affect outcome? Trauma. 2026;0(0). doi:10.1177/14604086261430458
Category: Trauma
Keywords: Cervical immobilization, collar rigid, soft (PubMed Search)
Posted: 4/2/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Looking at trauma patients evaluated at a major trauma center before and after EMS switched from semi-rigid to soft cervical collars for immobilization found no difference in adverse outcomes. Add this to the mounting evidence that our current practice of spinal immobilization may not offer any benefit.
JACEP Open 2024;5:e13239. https://doi.org/10.1002/emp2.13239
Category: Trauma
Keywords: Shock, bradycardia, Hemoperitoneum, hypotension, (PubMed Search)
Posted: 3/29/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Bradycardia accompanying hypotension can be found in spinal cord injury (loss of autonomic reflex), beta blocker and calcium channel blocker overdose, intrinsic cardiac electrophysiologic derangement, and, often forgotten, intrabdominal hemorrhage. In the appropriate setting (blunt trauma, ruptured ectopic pregnancy), bradycardic hypotensive patients should be considered the same as tachycardic hypotensive patients and get a work up and treatment focused on Hemoperitoneum.
Category: Geriatrics
Posted: 3/26/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
Using a database of 300,000 patients and applying a predictive measure for mortality, these authors found that patients over 66 with a high likelihood of 6 month mortality at the time of presentation were more likely to be admitted to an ICU when they presented to an ED. The authors conclude there is much work to be done regarding discussion of goals of care based on this information.
Adeyemi O, Hill J, Siman N, Goldfeld KS, Cuthel AM, Grudzen CR. Acute Care Use and Prognosis in Older Adults Presenting to the Emergency Department. J Pain Symptom Manage. 2025;69(6):559-568. doi:10.1016/j.jpainsymman.2025.01.006
Category: Trauma
Keywords: Whole blood, trauma center level (PubMed Search)
Posted: 3/22/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Looking at a national database, this study concluded the use of low titer O whole blood during trauma resuscitations was increasing at level one centers but not at level 2 and 3 centers. Is this a representation of the national blood supply as whole blood is harder to stock? We need to understand this trend to assure equal and appropriate care to trauma patients across the country.
LETTER TO THE EDITOR
Steven G. Schauer, Mark H. Yazer
First published: 01 February 2026
Category: Trauma
Keywords: Trauma, geriatric, undertriage (PubMed Search)
Posted: 3/15/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Another study, this one from New Zealand, showing older trauma patients with similar injury severity score had less trauma team activations and higher mortality.
M.Nonis, A.McCombie, C.Wakeman, J.Geddes, and L. R.Joyce, “The Effect of Increasing Age on Outcomes in Major Trauma: A Retrospective Cohort Study,” Emergency Medicine Australasia38, no. 1 (2026): e70226, https://doi.org/10.1111/1742-6723.70226.
Category: Infectious Disease
Keywords: vasculitis, IgA, drug induced (PubMed Search)
Posted: 3/8/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
This case report reminds us that vasculitis is an inflammatory process that attacks blood vessels leading to organ dysfunction. The etiology can be a hypersensitivity reaction (think drugs) or an IgA mediated process secondary to infection (Strep or Mycoplasma). In this case, concomitate use of NSAIDS (very common etiology of hypersensitivity) and Mycoplasma lead to vasculitis. Treatment ranges from supportive care, to steroids to immunosuppressive agents such as azathioprine.
Elaine Yu, Akousa Osei-Tutu, Rachna Subramony,
Small Vessel Vasculitis from Mycoplasma Infection and Concurrent Topical Nonsteroidal Anti-Inflammatory Drug (NSAID) Medication,
The Journal of Emergency Medicine,
Volume 82,
2026,
Pages 88-93,
ISSN 0736-4679,
https://doi.org/10.1016/j.jemermed.2025.12.003.
Category: Pharmacology & Therapeutics
Keywords: Drug reaction. (PubMed Search)
Posted: 3/5/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Of 925 ED headache patients in this meta analysis comparing extrapyramidal side effects of bolus vs. continuous infusion of metoclopremide the majority of the reactions occurred in the bolus group.
Ryuta Onodera, Yusuke Ito, Takahiro Itaya, Yoshie Yamada, Taku Iwami, Yusuke Ogawa,
Extrapyramidal symptoms and effectiveness of continuous vs bolus intravenous metoclopramide: A systematic review and meta-analysis,
The American Journal of Emergency Medicine,
Volume 103,
2026,
Pages 36-44,
ISSN 0735-6757,
https://doi.org/10.1016/j.ajem.2026.01.051.
Category: Trauma
Keywords: Ketamine, pain control, trauma (PubMed Search)
Posted: 3/1/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
When compared to saline(!) trauma patients with a high injury severity score who received ketamine via pca for pain control had better quality of life indicators at 1,3, and 6 months post injury.
Trevino, C. , Carver, T. , Tomas, C. , Larson, C. , Mantz-Wichman, M. , Peppard, W. & deRoon-Cassini, T. (2026). Acute traumatic pain treatment with ketamine decreased PTSD and anxiety symptoms 6 months post hospital discharge. Journal of Trauma and Acute Care Surgery, 100 (2), 215-220. doi: 10.1097/TA.0000000000004835.
Category: Geriatrics
Keywords: Sepsis, geriatric, temperature (PubMed Search)
Posted: 2/26/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
Bottom Line: arrival temperature had no prognostic value in non-septic older patients. Hypothermia in sepsis, but not fever, predicted mortality.
Finn Erland Nielsen, Osama Bin Abdullah, Lana Chafranska, Thomas Andersen Schmidt, Rune Husås Sørensen,
Temperature at admission and mortality in older adults with infection: Limited prognostic value in non-sepsis cases,
The American Journal of Emergency Medicine,
Volume 103,
2026,
Pages 1-8,
ISSN 0735-6757,
https://doi.org/10.1016/j.ajem.2026.01.045.
Category: Trauma
Keywords: substance use, falls, older, injury (PubMed Search)
Posted: 2/4/2026 by Robert Flint, MD
(Updated: 2/19/2026)
Click here to contact Robert Flint, MD
In a single level 1 trauma center there were 274 patients age over 55 evaluated for falls in a one year retrospective period. Their blood toxicology was reviewed for presence of alcohol, opioids, benzodiazepines and cannabinoids. The authors found:
“detection rates were 21.2% for opioids, 18.6% for ethanol, 13.9% for benzodiazepines, and 9.1% for cannabinoids. Injuries identified included 16.4% spinal fractures, 9.5% extremity fractures, 7.7% hip/thigh/pelvic fractures…In this study, nearly 20% of adults 55+ presenting for fall-related trauma recently used substances that impair psychomotor function.”
An area for injury prevention research and intervention would be to screen patients over age 55 for substance use, consider prescribing patterns in this age group (benzodiazepines) , and discuss with patients fall risk avoidance.
Babu, Kavita M. et al.
Journal of Emergency Medicine, Volume 0, Issue 0
Category: Trauma
Keywords: aajt, tourniquet (PubMed Search)
Posted: 2/4/2026 by Robert Flint, MD
(Updated: 2/14/2026)
Click here to contact Robert Flint, MD
A case report on use of the abdominal aortic and junctional tourniquet in a 27 year old female with hemorrhagic shock secondary to a pelvic fracture after a 10 meter fall demonstrated improved blood pressure and stabilized vasopressor use prior to operative intervention. This device has been used in battlefield situations, however very few reports of civilian use exist. Much more data is needed, however, it is a device to be aware of for future use.
From the manufacture's website:
"The AAJTS is an Abdominal Aortic Junctional Tourniquet that is designed to stop non-compressible hemorrhages wherever they occur on the body. FDA Certified for abdominal, axilla, inguinal and pelvic fractures, the AAJTS is battlefield tested and proven to be quick, easy, and effective to deploy.

1. Honnef, G., Freidorfer, D., Puchwein, P. et al. Bleeding control in catastrophic blunt pelvic trauma using the abdominal aortic and junctional tourniquet in a civilian level I trauma center: A case report. Scand J Trauma Resusc Emerg Med 34, 2 (2026). https://doi.org/10.1186/s13049-025-01517-w
2.https://www.life-assist.com/products/details/2848/abdominal-aortic-junctional-tourniquet/
Category: Vascular
Keywords: popliteal artery injury review (PubMed Search)
Posted: 2/4/2026 by Robert Flint, MD
(Updated: 2/8/2026)
Click here to contact Robert Flint, MD
Popliteal artery injuries are very rare (4% of all vascular injuries).
The majority of injuries are secondary to penetrating injury (70+%)
Blunt mechanism of injury has the higher rate of amputation.
Prolonged ischemia time (from injury to repair greater than 6 hours) leads to higher rates of amputation
Hard signs of vascular injury should prompt X-ray imaging of the knee, femur, and lower extremity and transfer to an operating room for repair.
Soft signs ("a history of significant bleeding which has ceased, nonexpanding hematomas, and the presence of an Ankle-Brachial Index of less than 0.9") and shotgun injury should prompt CT angiogram to evaluate arterial injury.
Asensio, Juan A. MD, PhD, DABS, FACS, FCCM, FRCS (England), FSVS, FAIM, FISS, KM; Ceron, Santiago A. MD; Inyang, Ime D. BA; Johnson, Sarah E. DHSc, MS; Williams, Mallory MD, MPH, FACS, FICS, FCCP, FCCM; Velasco, Jose M. MD, FACS, FCCM. Popliteal artery injuries: What you need to know. Journal of Trauma and Acute Care Surgery 100(2):p 162-172, February 2026. | DOI: 10.1097/TA.0000000000004752
