Category: Critical Care
Keywords: Intracerebral hemorrhage, intraparenchymal hemorrhage, ICH, IPH, hypertensive emergency, blood pressure, neurocritical care, nicardipine (PubMed Search)
Posted: 8/15/2016 by Daniel Haase, MD
(Updated: 9/6/2016)
Click here to contact Daniel Haase, MD
--Aggressive BP management (SBP <140) in atraumatic intracerebral hemorrhage (ICH) does NOT signifcantly improve mortality or disability compared with traditional goal (SBP <180) [1]
--However, a lower goal (SBP <140) has been shown to decrease hematoma size and be safe compared to a higher goal (SBP <180) [2]
The recently published ATACH-2 study investigated aggressive BP control in hypertensive acute atraumatic ICH/IPH (intraparenchymal hemorrhage). [1]
--Control group SBP 140-179 mmHg vs. intervention group SBP 110-139 mmHg with nicardipine infusion (control group actually had SBP 140-150 vs. intervention group SBP 120-130 most of the time).
--Study stopped early for futility. No difference in mortality or modified Rankin.
Previously, INTERACT2 demonstrated that aggressive SBP management (<140) was safe, decreasing hematoma expansion leading to a change in some individuals' practice. [2]
1. Qureshi AI, Palesch YY, et al; ATACH-2 Trial Investigators and the Neurological Emergency Treatment Trials Network. Intensive Blood-Pressure Lowering in Patients with Acute Cerebral Hemorrhage. N Engl J Med. 2016 Jun 8. [Epub ahead of print] PubMed PMID: 27276234.
2. Anderson CS, Heeley E, et al; INTERACT2 Investigators. Rapid blood-pressure lowering in patients with acute intracerebral hemorrhage. N Engl J Med. 2013 Jun 20;368(25):2355-65. doi: 10.1056/NEJMoa1214609. Epub 2013 May 29. PubMed PMID: 23713578.
Category: Critical Care
Keywords: refractory status epilepticus, ketamine, propofol, siezure, midazolam (PubMed Search)
Posted: 8/30/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Ketamine for RSE?
Legriel S, et al. What's new in refractory status epilepticus? Intensive Care Med 2016. [Epub ahead of print]
Category: Critical Care
Keywords: DKA (PubMed Search)
Posted: 8/23/2016 by Rory Spiegel, MD
Click here to contact Rory Spiegel, MD
Is it possible to have a patient present in diabetic ketoacidosis (DKA) with both negative serum and urinary ketone levels?
A case report published in American Journal of Emergency Medicine by Jehle et al provides a helpful reminder of this phenomenon (1). The degree of acidosis is directly related to the ratio of the various ketones/ketone metabolites: acetone, acetoacetate and beta-hydroxybutyrate present in the serum. The proportion of each respective substance is determined by the existing redox state in the blood. At any given time, acetoacetate and beta-hydroxybutyrate exist in an equilibrium dependent upon the ratio of NAD+ and NADH(fig.1). These substances freely convert with the assistance of the enzyme beta-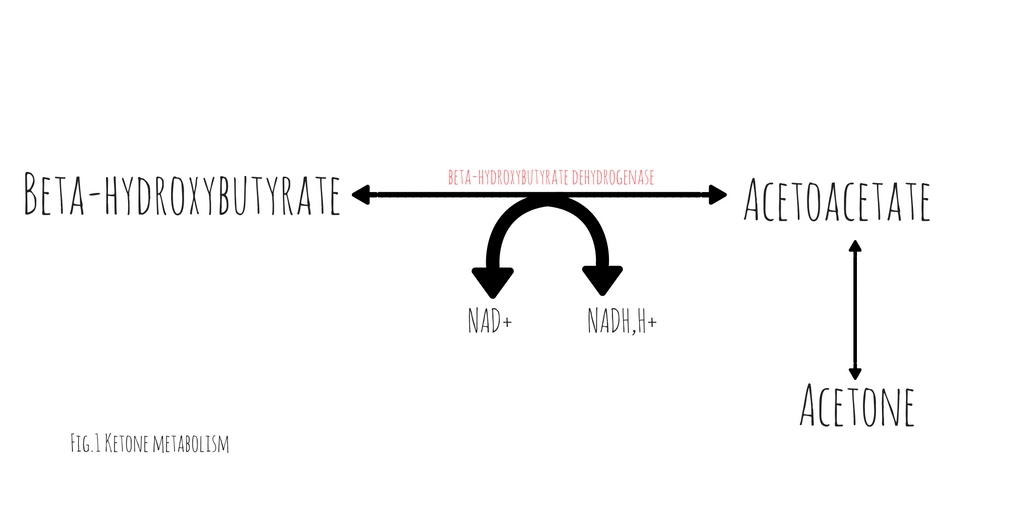 hydroxybutyrate dehydrogenase (2). This conversion requires the donation of a hydrogen atom from NADH. The balance between beta-hydroxybutyrate and acetoacetate, is determined by the ratio of NADH to NAD+. Acetoacetate will freely degrade into acetone through non-enzymatic decarboxylation. Early in DKA, acetoacetate is the most prevalent substance. As the disease progresses and the serum ratio of NADH to NAD+ increases, the proportion of beta-hydroxybutyrate rises, decreasing the quantity of acetoacetate and acetone.
hydroxybutyrate dehydrogenase (2). This conversion requires the donation of a hydrogen atom from NADH. The balance between beta-hydroxybutyrate and acetoacetate, is determined by the ratio of NADH to NAD+. Acetoacetate will freely degrade into acetone through non-enzymatic decarboxylation. Early in DKA, acetoacetate is the most prevalent substance. As the disease progresses and the serum ratio of NADH to NAD+ increases, the proportion of beta-hydroxybutyrate rises, decreasing the quantity of acetoacetate and acetone.
Traditional serum and urinary ketone assays react strongly to acetoacetate but neither reliably react with beta-hydroxybutyrate. Patients in whom the majority of their anion gap is filled by beta-hydroxybutyrate, urinary or serum ketone levels may be negative. In such cases, serum beta-hydroxybutyrate assays would be positive but are not universally available.
It is important to note, with resuscitation and insulin therapy, the ratio of NADH/NAD+ will start to normalize causing an increase in the quantity of acetoacetate. As the patient improves and the anion gap clears, the degree of ketones detected in the serum and urine will paradoxically increase.
1. Jehle D, et al, Severe diabetic ketoacidosis presenting with negative serum ketones: First case report and a review of the mechanism, Am J Emerg Med (2016)
2. Konijn, Abraham M., Naama Carmel, and Nathan A. Kaufmann. The redox state and the concentration of ketone bodies in tissues of rats fed carbohydrate free diets. The Journal of nutrition 10 (1976): 1507.
Category: Critical Care
Keywords: Zika Virus, Guillain-Barre (PubMed Search)
Posted: 8/9/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Zika Virus-associated GBS
Thiery G, et al. Zika virus-associated Guillain-Barre syndrome: a warning for critical care physicians. Intensive Care Med 2016; epub ahead of print.
Category: Critical Care
Keywords: ROSC, Cardiac Arrest, ETCO2 (PubMed Search)
Posted: 8/2/2016 by Rory Spiegel, MD
Click here to contact Rory Spiegel, MD
Despite a lack of prospective data, end-tidal CO2 (ETCO2) is often proposed as a viable replacement for the traditional pulse check to identify return of spontaneous circulation (ROSC) in patients presenting to the Emergency Department in Cardiac Arrest. A recent study by Tat et al examined this very question. The authors prospectively enrolled 178 patients suffering out-of-hospital cardiac arrest (OHCA) and examined the accuracy of a rise in ETCO2 at predicting ROSC. The authors examined both a rise of 10 and 20 mm Hg in ETCO2. Of the 178 patients included in this cohort, 60 (34%) experienced ROSC. The sensitivity and specificity of ETCO2 to predict ROSC at a threshold of 10 mm Hg was 33% and 97% respectively. At a threshold of 20 mm Hg ETCO2 performed no better with a sensitivity and specificity of 20% and 99% respectively.
What this data suggests is while a rise of ETCO2 of greater than 10 is highly suggestive of ROSC, the contrary cannot be said. The absence of a spike in ETCO2 does not rule out ROSC, as the large majority of patients experiencing ROSC in this cohort did so without demonstrating a significant rise in ETCO2. This evidence suggests that ETCO2 is a poor surrogate for a pulse check.
Tat LC, Ming PK, Leung TK, Abrupt rise of end tidal carbon dioxide level was a specific but non sensitive marker of return of spontaneous circulation in patient with out-of-hospital cardiac arrest, Resuscitation (2016), http://dx.doi.org/10.1016/j.resuscitation.2016.04.018
Category: Critical Care
Posted: 7/26/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Predicting Fluid Responsiveness with ETCO2
Category: Critical Care
Posted: 7/20/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Bucher J, Koyfman A. Intubation of the neurologically injured patient. J Emerg Med 2016; 49:920-7.
Category: Critical Care
Posted: 7/12/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
LVADs and RV Failure
Sen A, et al. Mechanical circulatory assist devices: a primer for critical care and emergency physicians. Crit Care 2016; 20:153.
Category: Critical Care
Keywords: Respiratory failure (PubMed Search)
Posted: 6/21/2016 by Feras Khan, MD
Click here to contact Feras Khan, MD
There are 4 types of respiratory failure that all providers should be familiar with
Type 1: Hypoxemic, PaO2 <50; this can include shunt , V/Q mismatch, or high altitude. Pulmonary edema, ARDS, pneumonia are common causes of this type of failure.
Type 2: Hypercapnic respiratory failure; decreased RR or tidal volume. This includes neuromuscular disorders including GBS or Myasthenia Gravis, in addition to medication overdose. COPD and asthma can lead to this type of respiratory failure as well.
Type 3: Peri-operative; atelectasis; decreased FRC from being supine or obese during the operative period.
Type 4: Shock or hypoperfusion leading to increased work of breathing and respiratory failure.
Category: Critical Care
Posted: 6/15/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Heat Stroke
Gaudio FG, Grissom CK. Cooling methods in heat stroke. J Emerg Med 2016; 50:607-16
Category: Critical Care
Keywords: PPI, GI bleed, UGIB, GI hemorrhage (PubMed Search)
Posted: 6/7/2016 by Daniel Haase, MD
Click here to contact Daniel Haase, MD
1. Laine L, Jensen DM. Management of patients with ulcer bleeding. Am J Gastroenterol. 2012 Mar;107(3):345-60; quiz 361. doi: 10.1038/ajg.2011.480. Epub 2012 Feb 7. Review. PubMed PMID: 22310222.
2. Barkun AN, et al; International Consensus Upper Gastrointestinal Bleeding Conference Group. International consensus recommendations on the management of patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med. 2010 Jan 19;152(2):101-13. doi: 10.7326/0003-4819-152-2-201001190-00009. PubMed PMID: 20083829.
3. Sachar H, Vaidya K, Laine L. Intermittent vs continuous proton pump inhibitor therapy for high-risk bleeding ulcers: a systematic review and meta-analysis. JAMA Intern Med. 2014 Nov;174(11):1755-62. doi: 10.1001/jamainternmed.2014.4056. Review. PubMed PMID: 25201154; PubMed Central PMCID: PMC4415726.
4. Neumann I, et aI. Comparison of different regimens of proton pump inhibitors for acute peptic ulcer bleeding. Cochrane Database Syst Rev. 2013 Jun 12;(6):CD007999. doi: 10.1002/14651858.CD007999.pub2. Review. PubMed PMID: 23760821.
5. Pantoprazole. Micromedex 2.0. Truven Health Analytics, Inc. Available at http://micromedexsoultsions. Accessed June 7, 2016.
Category: Critical Care
Posted: 5/31/2016 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Follow me on Twitter (@criticalcarenow)a
Category: Critical Care
Keywords: ATS, non invasive ventilation, aspirin, nighttime extubation, dialysis (PubMed Search)
Posted: 5/24/2016 by Feras Khan, MD
(Updated: 5/6/2026)
Click here to contact Feras Khan, MD
American Thoracic Society (ATS) Conference Highlights
The ATS conference was last week in San Francisco and a few cool articles were presented. They are briefly summarized below:
1. Using a helmet vs face mask for ARDS: Non-invasive ventilation is not ideal for ARDS for a variety of reasons. At the same time, endotracheal intubation and ventilation carries some risks as well. Could a new design of a "helmet" device make a difference? This one center study from the Univ of Chicago suggests that it would: decreased rate of intubation, increase in ventilator free days, and decrease in 90 day mortality. http://jama.jamanetwork.com/article.aspx?articleid=2522693
2. Can aspirin prevent the development of ARDS in at risk patients in the emergency department? Unfortunately, it does not appear to help. http://jama.jamanetwork.com/article.aspx?articleid=2522739
3. Should you start renal-replacement therapy (HD, CRRT etc) in critically ill patients with AKI sooner or later? Seems to have no difference and may actually lead to patients not needing any dialysis. Really a great read if you have time. http://www.nejm.org/doi/full/10.1056/NEJMoa1603017?query=OF&
4. Should I extubate at night? Lastly, probably don’t extubate at night if you can avoid it. Or just be cautious. http://www.atsjournals.org/doi/abs/10.1164/ajrccmconference.2016.193.1_MeetingAbstracts.A6150
Category: Critical Care
Posted: 5/17/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Situations Where ECMO Will Likely Fail
Schmidt M, et al. Ten situations in which ECMO is unlikely to be successful. Intensive Care Med 2016; 42:750-752.
Category: Critical Care
Keywords: Zika, Guillain-Barre, GBS, ITP, Critical Care (PubMed Search)
Posted: 5/10/2016 by Daniel Haase, MD
Click here to contact Daniel Haase, MD
Zika virus has received significant media attention in the US due to its recent link with teratogenicity. But Zika is also associated with critical and life-threatening complications, including death. Differentiating it from other Flavivirus diseases such as Dengue or Chikungunya can be challenging.
Diagnosis
Complications
1. Petersen LR, Jamieson DJ, Powers AM, Honein MA. Zika Virus. N Engl J Med. 2016 Apr 21;374(16):1552-63. doi: 10.1056/NEJMra1602113. Epub 2016 Mar 30. Review. PubMed PMID: 27028561.
2. LaBeaud, AD. Zika virus infection: An overview. uptodate.com. Accessed 5/10/2016.
3. Cao-Lormeau VM, et al. Guillain-Barr Syndrome outbreak associated with Zika virus infection in French Polynesia: a case-control study. Lancet. 2016 Apr 9;387(10027):1531-9. doi: 10.1016/S0140-6736(16)00562-6. Epub 2016 Mar 2. PubMed PMID: 26948433.
4. Centers for Disease Control and Prevention. Zika virus - What clinicians need to know? Clinician Outreach and Communication Activity (COCA) Call, January 26, 2016. Available at: http://emergency.cdc.gov/coca/ppt/2016/01_26_16_zika.pdf. Accessed May 10, 2016.
Category: Critical Care
Keywords: in hospital cardiac arrest, cardiac arrest (PubMed Search)
Posted: 4/26/2016 by Feras Khan, MD
Click here to contact Feras Khan, MD
A recent survey looked at resuscitation practices that could help improve survival during in-hospital cardiac arrest
Category: Critical Care
Posted: 4/19/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Can NIV be Used in ARDS?
Demoule A, et al. Can we prevent intubation in patients with ARDS? Intensive Care Med 2016; 42:768-771.
Category: Critical Care
Keywords: seizure, status epilepticus, pregnancy (PubMed Search)
Posted: 4/13/2016 by Daniel Haase, MD
Click here to contact Daniel Haase, MD
Disclaimer: Talking about seizures/status that is NOT due to eclampsia
TAKE HOME: While no AEDs are completely safe in pregnancy, treatment and stabilization of maternal status epilepticus is paramount for fetal health. Involve neurology/epileptology and OB/maternal-fetal medicine.
1. Hern ndez-D az S, et al; North American AED Pregnancy Registry; North American AED Pregnancy Registry. Comparative safety of antiepileptic drugs during pregnancy. Neurology. 2012 May 22;78(21):1692-9.
2. McElhatton PR. The effects of benzodiazepine use during pregnancy and lactation. Reprod Toxicol. 1994 Nov-Dec;8(6):461-75.
3. Lexicomp online accessed via uptodate.com.
Category: Critical Care
Posted: 4/5/2016 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Follow me on Twitter (@criticalcarenow)
Category: Critical Care
Keywords: cardiorenal syndrome, heart failure, kidney failure (PubMed Search)
Posted: 3/29/2016 by Feras Khan, MD
Click here to contact Feras Khan, MD
What is cardio-renal syndrome CRS?
There are 5 types
1. Acute CRS: abrupt worsening of heart function leading to kidney injury
2. Chronic CRS: chronic heart failure leads to progressive kidney disease
3. Acute renocardiac syndrome: abrupt kidney dysfunction leading to acute cardiac disorder
4. Chronic renocardiac syndrome: chronic kidney disease leading to decreased cardiac function
5. Systemic CRS: Systemic condition leading to both heart and kidney disease
