Category: Critical Care
Posted: 3/16/2021 by Lindsay Ritter, MD
Click here to contact Lindsay Ritter, MD
The PARAMEDIC2 trial in NEJM 2018 studied the outcomes of the use of epinephrine in outside hospital cardiac arrest (OHCA) on survival and neurological outcome.
Methods: Conducted in Britain, randomized 8007 patients to receive either epinepherine 1mg (n=4012) or placebo (n=3995) as part of standard CPR for out-of-hosptial arrest. Their primary outcome was survival at 30 days and their secondary outcomes included length of stay as well as neurological outcomes at 30 days and 3 months.
Results: The epinepherine group had improved survival to hospital admission (23% vs. 8%), at 30 days (3.2% vs. 2.4%) or at 3 months (3% vs. 2.2%). Favourable neurological outcomes, however, had no statistical difference at both hospital discharge and at 3 months.
Bottom line: Epinephrine improves ROSC, though with poor neurological outcomes.
Important facts:
Recently, a follow up of the PARAMEDIC2 trial was completed in Resuscitation.
They reported long-term survival, quality of life, functional and cognitive outcomes at 3, 6 and 12-months.
Results: At 6 months, 78 (2.0%) of the patients in the adrenaline group and 58 (1.5%) of patients in the placebo group had a favourable neurological outcome (adjusted odds ratio 1.35 [95% confidence interval: 0.93, 1.97]). 117 (2.9%) patients were alive at 6-months in the adrenaline group compared with 86 (2.2%) in the placebo group (1.43 [1.05, 1.96], reducing to 107 (2.7%) and 80 (2.0%) respectively at 12-months (1.38 [1.00, 1.92]). Measures of 3 and 6-month cognitive, functional and quality of life outcomes were reduced, but there was no strong evidence of differences between groups.
Bottom line: Epinephrine improves survival at 12 months, but poor neurological outcomes remain.
Haywood KL, Ji C, Quinn T, Nolan JP, Deakin CD, Scomparin C, Lall R, Gates S, Long J, Regan S, Fothergill RT, Pocock H, Rees N, O'Shea L, Perkins GD. Long term outcomes of participants in the PARAMEDIC2 randomised trial of adrenaline in out-of-hospital cardiac arrest. Resuscitation. 2021 Mar;160:84-93. doi: 10.1016/j.resuscitation.2021.01.019. Epub 2021 Jan 30. PMID: 33524488.
Perkins GD, Ji C, Deakin CD, Quinn T, Nolan JP, Scomparin C, Regan S, Long J, Slowther A, Pocock H, Black JJM, Moore F, Fothergill RT, Rees N, O'Shea L, Docherty M, Gunson I, Han K, Charlton K, Finn J, Petrou S, Stallard N, Gates S, Lall R; PARAMEDIC2 Collaborators. A Randomized Trial of Epinephrine in Out-of-Hospital Cardiac Arrest. N Engl J Med. 2018 Aug 23;379(8):711-721. doi: 10.1056/NEJMoa1806842. Epub 2018 Jul 18. PMID: 30021076.
Category: Critical Care
Keywords: sepsis recognition, antibiotics administration, mortality, (PubMed Search)
Posted: 3/10/2021 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Background:
The association between time intervals of ED antibiotic administration and outcome has been controversial. While single studies showed there was increased mortality associated with delayed antibiotic administration (1-3). A meta-analysis of 13 studies and 33000 patients showed that there was no mortality difference between septic patients receiving immediate Abx (< 1 hour) vs. those receiving early abx (1-3 hours) (4).
Since delay in recognition of sepsis (defined as ED triage to Abx order) and delay in antibiotics delivery (Abx order to administration) contribute to total delay of Abx administration, a new retrospective study (3) attempted to investigate the contributions of either factor to hospital mortality.
Results:
The study used generalized linear mixed models and involved 24000 patients.
For All patients and outcome of hospital mortality:
Recognition delay (ED triage to Abx order): OR 2.7 (95% CI 1.5-4.7)*
Administration delay at 2-2.5 hours (Abx order to administration): OR 1.5 (1.1-2.0)
These results was associated with non-statistical significance in patients with septic shocks.
Conclusion:
Delayed recognition of sepsis was associated with higher hospital mortality. Longer delay of abx administration was also associated with increased risk of hospital mortality.
1.Kumar A, Roberts D, Wood KE, et al: Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit Care Med. 2006; 34:1589–1596
2. Ferrer R, Martin-Loeches I, Phillips G, et al: Empiric antibiotic treatment reduces mortality in severe sepsis and septic shock from the first hour: Results from a guideline-based performance improvement program. Crit Care Med 2014; 42: 1749–1755
3. Seymour CW, Gesten F, Prescott HC, et al: Time to treatment and mortality during mandated emergency care for sepsis. N Engl J Med 2017; 376:2235–2244.
4. Rothrock SG et al. Outcome of immediate versus early antibiotics in severe sepsis and septic shock: A systematic review and meta-analysis. Ann Emerg Med 2020 Jun 24; [e-pub]. (https://doi.org/10.1016/j.annemergmed.2020.04.042)
Category: Critical Care
Posted: 3/2/2021 by Caleb Chan, MD
(Updated: 5/6/2026)
Click here to contact Caleb Chan, MD
Clinical Question:
Methods:
Results:
Take-home points:
Hughes CG, Mailloux PT, Devlin JW, et al. Dexmedetomidine or propofol for sedation in mechanically ventilated adults with sepsis. N Engl J Med. Published online February 2, 2021:NEJMoa2024922.
Category: Critical Care
Keywords: HACOR, NIV, noninvasive ventilation, acute respiratory failure (PubMed Search)
Posted: 2/2/2021 by Kami Windsor, MD
(Updated: 2/23/2021)
Click here to contact Kami Windsor, MD
Background: In respiratory failure due to COPD and cardiogenic pulmonary edema, noninvasive positive pressure ventilation decreases need for intubation and improves mortality,1 while its utility in other scenarios such as ARDS and pneumonia has yet to be proven.1,2 We know that patients on NIV with delays to needed intubation have a higher mortality,1,3 but intubation and mechanical ventilation come with risks that it is preferable to avoid if possible.
So how and when can we determine that NIV is not working?
The HACOR (Heart rate, Acidosis, Consciousness, Oxygenation, Respiratory rate) score at 1 hour after NIV initiation has been demonstrated to be highly predictive of NIV failure requiring intubation.4,5
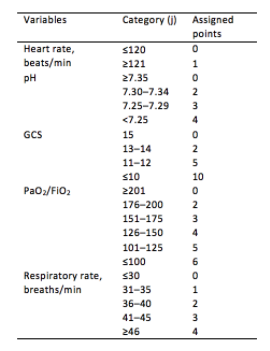

Initial development/validation: Score > 5 after 1 hour of NIV corresponds to >80% risk of NIV failure4
Earlier intubation (before 12 hours) in these patients = better survival
External validation: Score > 8 after 1 hour of NIV most predictive of eventual NIV failure 5
Average score @ 1-hour of patients with NIV success = 3.8
Score remained predictive at 6, 12, 24, 48 hours as well & mortality worsened as delay to intubation time increased
Baseline, pre-NIV score not predictive
Better predictive agreement in pneumonia and ARDS
Bottom Line:
Patients on NIV require close reassessment to prevent worsened survival due to intubation delay should invasive mechanical ventilation be indicated.
A HACOR score >8 after 1 hour of NIV should prompt intubation in most instances, with strong consideration given to a score >5.
*Note: ABGs were obtained for PaO2 assessment in the above studies -- the use of SpO2 was not evaluated -- but we are often not obtaining ABGs in our ED patients with acute respiratory failure. The following chart provides an estimated SpO2 to PaO2 conversion.
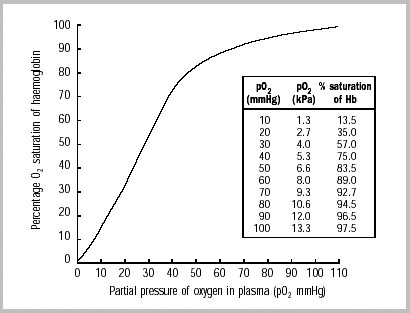
WHO 2001
Caveats:
Category: Critical Care
Keywords: Oxygenation, Mechanical Ventilation, Critical Care (PubMed Search)
Posted: 2/9/2021 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Optimal oxygenation targets and the possible, theoretical, benefits of hyperoxygenating critically ill patients have long been points of controversy. Multiple studies have suggested harm in pursuing aggressive hyperoxygenation amongst critical patients with various conditions ranging from myocardial infarction to sepsis to neurologic conditions. In addition, oxygen toxicity is a known mechanism causing ARDS.
The HOT-ICU trial adds to the list of arguments against hyperoxygenation, by looking at 2928 ICU patients on high levels of supplemental oxygen and targeting a paO2 of 60 mm Hg (low oxygen group) vs paO2 of 90 mm Hg (high oxygen group). There was no difference in mortality, or other significant difference in outcomes.
Bottom Line: A lower paO2 goal of 60 (correlates to an O2 sat of 90%) is noninferior to a higher paO2 goal of 90 (O2 sat of approximately 96%). When titrating oxygen, targeting a pulse ox of 90-96% is reasonable in critically ill patients. Be sure to include an upper limit on the sat goal, beware an O2 sat of 100%, and titrate down supplemental oxygen when the spO2 is above goal, as the paO2 may be dangerously high.
Schjørring OL, Klitgaard TL, Perner A, Wetterslev J, Lange T, Siegemund M, Bäcklund M, Keus F, Laake JH, Morgan M, Thormar KM, Rosborg SA, Bisgaard J, Erntgaard AES, Lynnerup AH, Pedersen RL, Crescioli E, Gielstrup TC, Behzadi MT, Poulsen LM, Estrup S, Laigaard JP, Andersen C, Mortensen CB, Brand BA, White J, Jarnvig IL, Møller MH, Quist L, Bestle MH, Schønemann-Lund M, Kamper MK, Hindborg M, Hollinger A, Gebhard CE, Zellweger N, Meyhoff CS, Hjort M, Bech LK, Grøfte T, Bundgaard H, Østergaard LHM, Thyø MA, Hildebrandt T, Uslu B, Sølling CG, Møller-Nielsen N, Brøchner AC, Borup M, Okkonen M, Dieperink W, Pedersen UG, Andreasen AS, Buus L, Aslam TN, Winding RR, Schefold JC, Thorup SB, Iversen SA, Engstrøm J, Kjær MN, Rasmussen BS; HOT-ICU Investigators. Lower or Higher Oxygenation Targets for Acute Hypoxemic Respiratory Failure. N Engl J Med. 2021 Jan 20. doi: 10.1056/NEJMoa2032510. Epub ahead of print. PMID: 33471452.
Category: Critical Care
Posted: 2/2/2021 by Mike Winters, MBA, MD
(Updated: 5/6/2026)
Click here to contact Mike Winters, MBA, MD
Mechanical Ventilation in COPD
Demoule A, et al. How to ventilate obstructive and asthmatic patients. Intensive Care Med. 2020; 46:2436-2449.
Category: Critical Care
Posted: 1/19/2021 by Lindsay Ritter, MD
Click here to contact Lindsay Ritter, MD
| Ever wonder what to tell the families regarding prognosis of the sickest COVID-19 patients you intubate in the ED or ICU? Introduction: Case fatality rates (CFR) for COVID-19 patients requiring invasive mechanical ventilation have been widely variable. A study in the Blue Journal (AJRCCM) examined patients requiring intubation in a systemic review and meta-analysis. The case fatality risk of an infection is represented by the proportion of patients who die among all infected cases in a population over a period of time. Methods: 69 studies axross 23 countries for a total of 57,420 patients with COVID-19 who required mechanical ventilation were included in analysis. Results: Overall case fatality rate was 45%, or about 1 death for every two intubated patients.. Among studies that included age stratification, pooled estimates of CFR were 47.9% in patients <40 (CI 46.4-49.4%) and 84.4% in patients >80 (CI 83.3-85.4%). Overall heterogeneity is high (I 2 .90%), In early COVID epicenters, CFR was 70% among patients aged more than 60 years of age. CFR increased exponentially with increasing age. Specifically in the US across 21 studies (3,811 intubated patients), CFR was 47% (95% CI, 36–57%). Studies from New York reported a CFR of 54% (95% CI, 36–72%) whereas other regions in the United States reported a CFR of 41% (95% CI, 30–53%). Definitive hospital CFR (aka for those with hospital discharge outcomes, 13,120 patients) was 56% (CI 47-65%). Conclusion: Almost half of patients with COVID-19 receiving IMV died based on the reported CFR. The reported CFR was higher in older patients and in early pandemic epicenters, which may be influenced by limited ICU resources. Limitations: Overall CFR of 45% still included patients in the hospital. Definitive hospital outcomes were only for 13,120 patients (36.6%). Significant variation in CFR exists between studies. |
Lim ZJ, Subramaniam A, Ponnapa Reddy M, Blecher G, Kadam U, Afroz A, Billah B, Ashwin S, Kubicki M, Bilotta F, Curtis JR, Rubulotta F. Case Fatality Rates for Patients with COVID-19 Requiring Invasive Mechanical Ventilation. A Meta-analysis. Am J Respir Crit Care Med. 2021 Jan 1;203(1):54-66.
Angriman F, Scales DC. Estimating the Case Fatality Risk of COVID-19 among Mechanically Ventilated Patients. Am J Respir Crit Care Med. 2021 Jan 1;203(1):3-4.
Category: Critical Care
Keywords: COVID-19, Awake proning, intubation (PubMed Search)
Posted: 1/12/2021 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
A single center (Nebraska, USA), retrospective analysis investigated the prevalence of intubation during hospital stay for 105 patients who had COVID-19 between March 24 to May 5, 2020 (1). 40 patients underwent awake proning vs. 60 patients did not undergo awake proning.
After adjusting for either SOFA or APACHE scores, patients with awake proning were associated with lower Hazard Ratios of intubation for SOFA (HR 0.30, 95% CI 0.09-0.96, p=0.043) and APACHE (HR 0.30, 95%CI 0.1-0.91, p=0.034).
Discussion
While this US study seemed promising, another Brazilian study being published earlier in July 2020 showed no difference in the prevalence of intubation between COVID-19 patients with proning or without proning (2).
These 2 studies highlighted the nature of this disease: high practice variability, uncertainty of therapeutic modalities. However, the complications from awake proning had been very low.
Conclusion:
Awake proning for hypoxic COVID-19 patients is a promising intervention but we will need more studies. In the meanwhile, we can try this therapeutic modality as the risk is low.
Category: Critical Care
Posted: 1/6/2021 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Study Question: What is the association of relative hypotension (degree and duration of MPP deficit) in patients with vasopressor-dependent shock with the incidence of new significant AKI and major adverse kidney events (MAKE)?
Methods:
Results:
Take-aways:
Panwar R, Tarvade S, Lanyon N, et al. Relative hypotension and adverse kidney-related outcomes among critically ill patients with shock. A multicenter, prospective cohort study. Am J Respir Crit Care Med. 2020;202(10):1407-1418.
Category: Critical Care
Posted: 12/8/2020 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
PEEP in the Intubated Obese Patient
De Jong A, et al. How to ventilate obese patients in the ICU. Intensive Care Med. 2020; 46:2423-35.
Category: Critical Care
Keywords: vasopressor, peripheral IV, safety (PubMed Search)
Posted: 11/17/2020 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Summary
Our group performed a meta-analysis to assess whether it is safe to infuse vasopressor through peripheral venous catheters. We identified 9 studies with a total of 1835 patients. The prevalence of complications among the pooled patient population was 9%. Up to 96% of the complications was extravasation and almost no complications required any treatment.
A few studies reported safe infusion of norepinephrine up to 0.1 mcg/kg/min for up to 24 hours.
In exploratory meta-regression, catheter size 20 or larger was negatively associated with the rate of complications.
We also observed that studies that were published within the past 5 years reported significantly lower rate of complications from older studies. This suggested that with careful planning and monitoring, it is safe to start vasopressor through peripheral IV.
Limitation
most of the included studies were observational. No studies had enough power to statistically analyze any variables that could predict complications.
Bottom line: we should start vasopressor as soon as indicated, if we have good, reliable IV access.
Complication of vasopressor infusion through peripheral venous catheter: A systematic review and meta-analysis
Quincy K Tran, Gaurika Mester, Vera Bzhilyanskaya, Leenah Z Afridi, Sanketh Andhavarapu, Zain Alam, Austin Widjaja, Brooke Andersen, Ann Matta, Ali Pourmand.
Am J Emerg Med. 2020 Sep 28;S0735-6757(20)30842-1. doi: 10.1016/j.ajem.2020.09.047. Online ahead of print.
Category: Critical Care
Keywords: Hyponatremia (PubMed Search)
Posted: 11/12/2020 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Baek SH, Jo YH, Ahn S, et al. Risk of overcorrection in rapid intermittent bolus vs slow continuous infusion therapies of hypertonic saline for patients with symptomatic hyponatremia: the salsa randomized clinical trial. JAMA Intern Med. Published online October 26, 2020.
Category: Critical Care
Keywords: airway management, cardiac arrest, COVID-10, SARS-CoV-2, cardiopulmonary resuscitation, CPR (PubMed Search)
Posted: 11/3/2020 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
As the number of COVID-19 cases rises worldwide, prehospital and emergency department healthcare workers remain at high risk of exposure and infection during CPR for patients with cardiac arrest and potential SARS-CoV-2.
Existing evidence supports similar cardiac arrest outcomes in airways managed with a supraglottic airway (SGA) compared to endotracheal intubation (ETT).1 It is generally accepted that the best airway seal is provided with endotracheal intubation + viral filter, but how well do SGAs prevent spread of aerosols?
In CPR simulation studies:
Category: Critical Care
Keywords: NAC, Liver Failure, n-acetylcysteine (PubMed Search)
Posted: 10/20/2020 by Mark Sutherland, MD
(Updated: 5/6/2026)
Click here to contact Mark Sutherland, MD
N-acetylcysteine (NAC) is well known as the accepted antidote for acute acetaminophen (tylenol/paracetamol) overdose and is well studied for this indication. While the literature base is not nearly as strong in other causes of acute liver failure, NAC is increasingly used in these scenarios as well. In the emergency department in particular, the cause of fulminant hepatic failure is often not known. NAC may have some protective benefit in non-acetaminophen acute liver failure. Existing data do not show a mortality benefit to NAC in non-acetaminophen acute liver failure, but do show improvement in transplant-free survival. The AASLD guidelines (last revised in 2011) do not comment on NAC in non-acetaminophen acute liver failure. A common practice is to continue NAC until the INR is < 2 and AST/ALT have decreased at least 25% from their peak values.
Patients in fulminant liver failure should also be strongly considered for transfer to a center that does liver transplant, if presenting to a non-transplant center. The King's College criteria is the most commonly used prognostic score for determining need of transfer to a transplant center, but in addition to calculating a King's College score providers should generally consider consultation with a transplant hepatologist for any fulminant liver failure patient to discuss the risks/benefits of transfer for transplant evaluation.
Bottom Line: While not as strongly indicated as it is in acute acetaminophen induced liver failure, NAC should be considered in both non-acetaminophen liver failure and liver failure of unknown etiology. In addition, strongly consider consultation with a transplant hepatologist in any case of fulminant hepatic failure.
Teriaky A. The role of N-acetylcysteine in the treatment of non-acetaminophen acute liver failure. Saudi J Gastroenterol. 2017;23(3):131-132.
October 2020 EMRAP: Critical Care Mailbag
MDCalc King's College Criteria: https://www.mdcalc.com/kings-college-criteria-acetaminophen-toxicity
Category: Critical Care
Posted: 10/13/2020 by Mike Winters, MBA, MD
(Updated: 5/6/2026)
Click here to contact Mike Winters, MBA, MD
Blood Pressure Management in Acute Ischemic Stroke
Herpich F, et al. Management of acute ischemic stroke. Crit Care Med. 2020; 48(11):1654-1663.
Category: Critical Care
Keywords: Cardiac arrest, transport, EMS (PubMed Search)
Posted: 9/29/2020 by Lindsay Ritter, MD
Click here to contact Lindsay Ritter, MD
Historically, there has been debate on transporting outside hospital cardiac arrests, as well a trauma, with the question of whether to "scoop and run" or "stay and play".
Could hasty transportation of cardiac arrest patients put a damper on resuscitation quality?
A recent propensity-matched study in JAMA analyzed 192 EMS agencies across 10 N American sites.
Methods:
-Resuscitation Outcomes Consortium Cardiac Epidemiologic Registry, which counted 43,969 consecutive cases of nontraumatic adult EMS-treated OHCA (median age 67, 37% of whom were women) in 2011-2015.
-25% of these patients were transported to the hospital
-Matched 1:1 with patients in refractory arrest who were resuscitated on scene
-Primary outcome was survival to hospital discharge, secondary outcome survival to hospital discharge with a favorable neurological status
Results:
-Duration of out-of-hospital resuscitation was only 6 minutes longer in the intra-arrest transport group (29.1 and 22.9 minutes; not a statistically significant difference)
-Survival to hospital discharge was 3.8% for patients who underwent intra-arrest transport and 12.6% for those who received on-scene resuscitation
-In the propensity-matched cohort, which included 27,705 patients, survival to hospital discharge occurred in 4.0% of patients who underwent intra-arrest transport vs 8.5% who received on-scene resuscitation (risk difference, 4.6% [95% CI, 4.0- 5.1])
-Favorable neurological outcome occurred in 2.9% of patients who underwent intra-arrest transport vs 7.1% who received on-scene resuscitation (risk difference, 4.2% [95% CI, 3.5%-4.9%])
-Intra-arrest transport during resuscitation was associated with worse odds of survival to hospital discharge compared to on-scene resuscitation (4% vs 8.5%, RR 0.48, CI 0.43-0.54)
-Findings persisted across subgroups of initial shockable rhythm vs. non-shockable rhythms (most common initial rhythm was aystole), as well as EMS witness arrests vs. unwitnessed arrests
Conclusion:
-This study does not support the routine transportation of patients in cardiac arrest during rescuscitation.
-The neurologically intact survival benefit associated with on-scene resuscitation is both impressive and intriguing.
-However, what implications could this have on ECPR?
Limitations:
-Potential bias due to observational nature of study
-Duration of resuscitations very similar, unknown exactly how long transport times were or if this was in urban or rural populations
-External validity not generalizable due to heterogeneity of patient populations and EMS systems
-Further randomized clinical trials are required
Grunau B, Kime N, Leroux B, et al. Association of Intra-arrest Transport vs Continued On-Scene Resuscitation With Survival to Hospital Discharge Among Patients With Out-of-Hospital Cardiac Arrest. JAMA. 2020;324(11):1058–1067. doi:10.1001/jama.2020.14185
Category: Critical Care
Keywords: IPH, blood pressure management, outcome (PubMed Search)
Posted: 9/22/2020 by Quincy Tran, MD, PhD
Click here to contact Quincy Tran, MD, PhD
A retrospective study analyzed data from 757 patients with spontaneous intraparenchymal hemorrhage.
Within the first 6 hours of admission, patients who had systolic blood pressure reduction between 40 – 60 mm Hg (OR 1.9, 95% CI 1.1-3.5) or reduction ≥ 60 mm Hg (OR 1.9, 95%CI 1.01-3.8) were associated with almost double likelihood of poor discharge functional outcome (defined as modified Rankin Scale 3-6).
Additionally, large systolic blood pressure reduction ≥ 60 mm Hg in patients with large hematoma (≥ 30.47 ml) was associated with higher likelihood of very poor functional outcome (mRS 5-6).
Take home points: while more studies are still needed to confirm these observations, perhaps we may not want to drop blood pressure in patients with spontaneous intraparenchymal hemorrhage too much and too fast.
The Magnitude of Blood Pressure Reduction Predicts Poor In-Hospital Outcome in Acute Intracerebral Hemorrhage.
Afshin A Divani, Xi Liu, Alexander Petersen, Simona Lattanzi, Craig S Anderson, Wendy Ziai, Michel T Torbey, Tom J Moullaali, Michael L James, Alibay Jafarli, Stephan A Mayer, Jose I Suarez, J Claude Hemphill, Mario Di Napoli.
Neurocrit Care. 2020 Oct;33(2):389-398. doi: 10.1007/s12028-020-01016-z.
Category: Critical Care
Posted: 9/18/2020 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Systematic review and meta-analysis of 5 studies with a total of 929 patients comparing early vs. late initiation of norepinephrine in patients with septic shock
Primary outcome:
Secondary outcome:
Caveat:
Take home point:
Early norepinephrine usage may improve mortality in septic shock
Li Y, Li H, Zhang D. Timing of norepinephrine initiation in patients with septic shock: a systematic review and meta-analysis. Crit Care. 2020;24(1):488.
Category: Critical Care
Keywords: resuscitation, ultrasound, VExUS, venous congestion (PubMed Search)
Posted: 9/8/2020 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
While the invasive monitoring of central venous pressure (CVP) in the critically ill septic patient has gone the way of also transfusing them to a hemoglobin of 10 mg/dL, it remains that an elevated CVP is associated with higher mortality1,2 and renal failure.2,3
Extrapolating from existing data looking at hepatic vein, portal vein, and renal vein pulsatility as measures of systemic venous hypertension and congestion,4,5,6 Beaubien-Souligny et al. developed the venous excess ultrasound (VExUS) grading system incorporating assessment of all 3, plus the IVC, using US to stage severity of venous congestion in post-cardiac surgery patients.7 They evaluated several variations, determining that the VExUS-C grading system was most predictive of subsequent renal dysfunction.
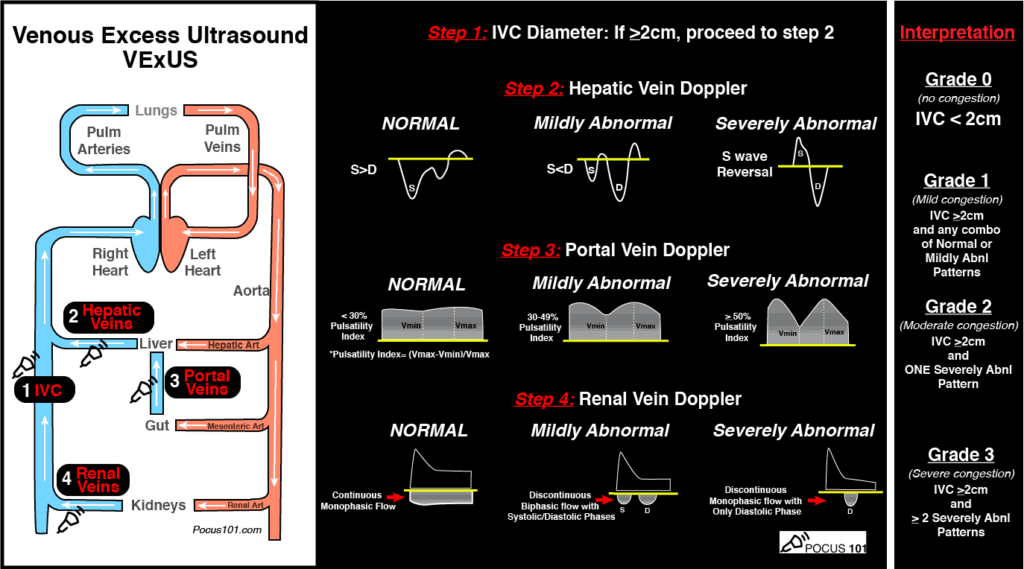
(Image from www.pocus101.com)
High Points
VExUS Grade 3 (severe) venous congestion:
Caveats
Clinical Uses
A great how-to can be found here:
https://www.pocus101.com/vexus-ultrasound-score-fluid-overload-and-venous-congestion-assessment/
1. Li DK, Wang XT, Liu DW. Association between elevated central venous pressure and outcomes in critically ill patients. Ann Intensive Care. 2017;7(1):83. doi:10.1186/s13613-017-0306-1
2. Chen KP, Cavender S, Lee J, et al. Peripheral Edema, Central Venous Pressure, and Risk of AKI in Critical Illness. Clin J Am Soc Nephrol. 2016;11(4):602-608.
3. Chen CY, Zhou Y, Wang P, Qi EY, Gu WJ. Elevated central venous pressure is associated with increased mortality and acute kidney injury in critically ill patients: a meta-analysis. Crit Care. 2020;24(1):80. doi:10.1186/s13054-020-2770-5
4. Iida N, Seo Y, Sai S, et al. Clinical Implications of Intrarenal Hemodynamic Evaluation by Doppler Ultrasonography in Heart Failure. JACC Heart Fail. 2016;4(8):674-682. doi:10.1016/j.jchf.2016.03.016
5. Ikeda Y, Ishii S, Yazaki M, et al. Portal congestion and intestinal edema in hospitalized patients with heart failure. Heart Vessels. 2018;33(7):740-751. doi:10.1007/s00380-018-1117-5.
6. Beaubien-Souligny W, Benkreira A, Robillard P, et al. Alterations in Portal Vein Flow and Intrarenal Venous Flow Are Associated With Acute Kidney Injury After Cardiac Surgery: A Prospective Observational Cohort Study. J Am Heart Assoc. 2018;7(19):e009961. doi:10.1161/JAHA.118.009961
7. Beaubien-Souligny W, Rola P, Haycock K, et al. Quantifying systemic congestion with Point-Of-Care ultrasound: development of the venous excess ultrasound grading system. Ultrasound J. 2020;12(1):16. doi:10.1186/s13089-020-00163-w
Category: Critical Care
Keywords: Renal Replacement Therapy (PubMed Search)
Posted: 9/1/2020 by Kim Boswell, MD
(Updated: 5/6/2026)
Click here to contact Kim Boswell, MD
STARRT-AKITrial
The Standard versus Accelerated initiation of Renal Replacement Therapy in Acute Kidney Injury
The development of acute kidney injury (AKI) in the critical care setting portends a greater morbidity and mortality for patients. Additionally, it places the patient at high risk of complications and requires a greater use of resources. Several studies in the past have examined if the timing of initiation of renal replacement therapy (RRT) would result in a mortality benefit, but have failed to demonstrate consistent outcomes.
The STARRT-AKI trial was a multinational, randomized controlled trial designed to determine if early initiation of RRT in critically ill adult patients with AKI lowered the risk of 90-day mortality. The Kidney Disease Improving Global Outcomes (KDIGO) classification was used to define AKI and over 2900 patients were randomly assigned to two groups over a 4 year period. Exclusion criteria included: recent RRT, a renal transplant within the preceding year, advanced CKD, an overdose necessitating RRT, or a strong suspicion of obstruction or autoimmune/vascular cause of their AKI.
Groups:
Outcomes/Results:
Take home points:
Timing of Initiation of Renal-Replacement Therapy in Acute Kidney Injury. STARRT-AKI Investigators; Canadian Critical Care Trials Group, the Australian and New Zealand Intensive Care Society Clinical Trials Group, the United Kingdom Critical Care Research Group, the Canadian Nephrology Trials Network, and the Irish Critical Care Trials Group, Bagshaw SM, Wald R, Adhikari NKJ, et al. N Engl J Med. 2020 Jul 16;383(3):240-251.
