Category: Critical Care
Posted: 8/31/2021 by Lucas Sjeklocha, MD
Click here to contact Lucas Sjeklocha, MD
Background: Interest in moving to balanced fluid administration has grown after publication of the SPLIT trial and SALT-ED/SMART trials, which showed respectively evidence of benefit to balanced crystalloid over normal saline on mortality and major adverse kidney events at 30 days.
Population/Intervention: The BaSICs trial is an RCT in 75 ICUs in Brazil, testing P-Lyte versus NS (with each arm getting two different infusion rates that were analyzed as a separate trial) for volume administration per protocol.
--10,520 ICU patients requiring fluid expansion, expected ICU stay >1 day, and 1 additional risk factor for AKI (age>65, hypotension, sepsis, MV, NIV, oliguria, elevated creatinine, cirrhosis, or acute liver failure).
--Exclusions: severe dysnatremia, expected RRT within 6 hours, expected death.
--Average age was 61, with a SOFA score of 4, and 48% on were elective surgical admissions.
Outcome:
--No difference in 90 days mortality (P-Lyte 26.4% v NS 27.2, aHR p=0.47), AKI or RRT out to 7-days, or in duration of MV, ICU LOS or hospital LOS
--Median study fluid by day 3 was 2.9L in each group
--Higher neurological SOFA score observed in P-Lyte group
--Higher mortality seen with P-Lyte in TBI subgroup (P-Lyte 31.3% vs NS 21.1%, p=0.02)
Discussion:
--Adds contrasting negative data to previous large positive RCTs showing benefit of balanaced fluids
--Expect further reanalysis/metanalysis of BSS versus NS trials
--Signal for harm in TBI pts with P-Lyte correlates with SMART point estimates that were not significant
--Compared to SMART trial population BaSICs had: 2x higher mortality, more planned surgery, received about 1L more study fluid in the first 3ds
Takeaway:
--Balanced crystalloid versus normal saline debate will continue considering this large negative trial
--Signal for possible harm in TBI population with balanced crystalloids compared to normal saline
References:
Category: Critical Care
Keywords: SOFA, sepsis, oxygen saturation (PubMed Search)
Posted: 8/25/2021 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Background: SOFA score has been used as a predictor for poor outcomes in patients with sepsis. However, the original SOFA score utilizes PaO2/FiO2 ratio to calculate the SOFA’s respiratory component. When there are no ABG, thus no PaO2, we have to convert patients’ spO2 to PaO2, and the amount of oxygen support to FiO2 (for example, 2 liters of oxygen via nasal cannula = 0.27). This is cumbersome.
Objective: This study assessed whether spO2 can be used instead of PaO2/FiO2 ratio for SOFA’s respiratory score.
Settings: 8 hospitals across Sweden and Canada
Patients: Adults with sepsis. 19396 patients were included for the derivation group while there were 10586 patients for the validation cohort.
Study Results:
Discussion:
Valik JK, Mellhammar L, Sundén-Cullberg J, Ward L, Unge C, Dalianis H, Henriksson A, Strålin K, Linder A, Nauclér P. Peripheral Oxygen Saturation Facilitates Assessment of Respiratory Dysfunction in the Sequential Organ Failure Assessment Score With Implications for the Sepsis-3 Criteria. Crit Care Med. 2021 Aug 18. doi: 10.1097/CCM.0000000000005318. Epub ahead of print. PMID: 34406170.
Category: Critical Care
Keywords: IVF, intravenous fluids, resuscitation, infusion rates (PubMed Search)
Posted: 8/18/2021 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Background:
There are also no clear guidelines regarding how fast fluid boluses should be administered, and there has been debate about whether different infusion rates could lead to different outcomes in patients receiving intravenous fluid (IVF) boluses (i.e. fast infusions may cause more third spacing due to the rapidity of the expansion of the intravascular space compared to fluid administered more slowly). A recent study compared IVF infusion rates in ICU patients.
-- Unblinded, randomized
-- 10,520 patients clinically requiring a fluid challenge, from 75 ICUs in Brazil
-- Infusion rate 333 mL/hr vs 999 mL/hr
* (Trial also compared plasmalyte vs 0.9% saline, analyzed in separate study)
-- Some notable exclusion criteria: severe hypo/hypernatremia, AKI or expected to need RRT 6 hrs after admission
--Other caveats:
* Faster infusion rates allowed at physician discretion in patients with active bleeding or severe hypotension (SBP < 80 or MAP < 50 mmHg); patient was returned to assigned rate after condition resolved
* Almost 1/2 the patients received at least 1L of IVF in 24 hours prior to enrollment
-- Results: No sig difference in 90-day survival, use of RRT, AKI, mechanical ventilator free days, ICU/hospital mortality/LOS
Bottom Line: There is not yet compelling evidence that there are differences in patient outcomes in patients receiving fluid boluses given at 333 cc/hr vs. 999 cc/hr.
1. Zampieri FG, Machado FR, Biondi RS, et al. Effect of slower vs faster intravenous fluid bolus rates on mortality in critically ill patients: the basics randomized clinical trial. JAMA. Published online August 10, 2021.doi:10.1001/jama.2021.11444
2. Zampieri FG, Machado FR, Biondi RS, et al. Effect of intravenous fluid treatment with a balanced solution vs 0. 9% saline solution on mortality in critically ill patients: the basics randomized clinical trial. JAMA. Published online August 10, 2021.
Category: Critical Care
Keywords: cardiac arrest, IHCA, resuscitation, epinephrine, pediatrics (PubMed Search)
Posted: 8/11/2021 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Approximately 15,000 children experience an in hospital cardiac arrest (IHCA) with little improvement in outcomes over the last two decades. During that time, epinephrine has been the constant basis for resuscitation of these patients. Current recommendations by the AHA recommend bolus dosing of epinephrine every 3-5 minutes in a pediatric cardiac arrest. Animal studies suggest that more frequent dosing of epinephrine may be beneficial.
This was a retrospective study of 125 pediatric IHCAs with 33 receiving “frequent epinephrine” interval (≤2 minutes). Pediatric CPC score 1-2 or no change from baseline was used as primary outcome to reflect favorable neurologic outcome, with frequent dosing associated with better outcome (aOR 2.56, 95%CI 1.07 to 6.14). Change in diastolic blood pressure was greater after the second dose of epinephrine among patients who received frequent epinephrine (median [IQR] 6.3 [4.1, 16.9] vs. 0.13 [-2.3, 1.9] mmHg, p=0.034).
This study is subject to all sorts of confounding and should be studied more rigorously, but suggests that more frequent dosing for pediatric IHCA may be of benefit.
Kienzle MF, Morgan RW, Faerber JA, et al. The Effect of Epinephrine Dosing Intervals on Outcomes from Pediatric In-Hospital Cardiac Arrest. Am J Respir Crit Care Med. 2021. doi: 10.1164/rccm.202012-4437OC.
Category: Critical Care
Keywords: Modified Clamshell thoracotomy, resuscitative thoracotomy, randomized control trial (PubMed Search)
Posted: 8/3/2021 by Kim Boswell, MD
Click here to contact Kim Boswell, MD
Resuscitative thoracotomy is a dramatic and heroic procedure used in the emergency department in an attempt to resuscitate a patient in arrest due to trauma. There are a few techniques commonly used, but due to the extreme nature of the procedure no prior randomized controlled trials (RCTs) have been done.
The modified clamshell thoracotomy (MCT) is a technique in which the standard left anterolateral thoracotomy (LAT) is extended across the sternum, but does not involve surgical opening of the right chest. The MCT allows for increased visualization of the mediastinum and thoracic cavity structures.
Sixteen Emergency trained physicians (approximately half attending and half senior residents) from a level 1 trauma center underwent didactic and skill based training on both the MCT and LAT techniques using fresh, human cadavers. Following training they were randomized based on order of intervention, performing both techniques.
Their thoracotomies were assessed by a board certified surgeon and “success” was determined based on the complete delivery of the heart and cross clamping of the descending aorta.
Primary outcome: time to successful completion of procedure
Secondary outcomes: successful delivery of the heart from the pericardial sac (as well as time to delivery), cross clamping of the aorta (and time to clamping), procedural completion and number of iatrogenic injuries.
Overall, there was no statistical difference in primary outcome or successful completion between the MCT compared to the LAT (67% vs. 40%). However, 100% of the LAT resulted in some form of iatrogenic injury (rib fractures, lacerations of the diaphragm,/esophagus/heart/lung) compared to 67% of the MCT technique. There was no associated difference in success when previous experience (attending vs. senior resident) were compared. Lastly, MCT was the favored technique of the majority of the study subjects.
Prospective Randomized Trial of Standard Left Anterolateral Thoracotomy Versus Modified Bilateral Clamshell Thoracotomy Performed by Emergency Physicians. Ann Emerg Med. 2021 Mar;77(3):317-326 doi: 10.1016/j.annemergmed.2020.05.042nnemergmed.2020.05.042Prospective Randomized Trial of Standard Left Anterolateral Thoracotomy Versus Modified BiProspective Randomized Trial of Standard Left Anterolateral Thoracotomy Versus Modified Bilateral Clamshell Thoracotomy Performed by Emergency Physicians. Ann Emerg Med. 2021 Mar;77(3):317-326 doi: 10.1016/j.annemergmed.2020.05.042lateral Clamshell Thoracotomy Performed by Emergency Physicians. Ann Emerg Med. 2021 Mar;77(3):317-326 doi: 10.1016/j.annemergmed.2020.05.042
Category: Critical Care
Keywords: COVID-19, Antiviral, Hydroxychloroquine (PubMed Search)
Posted: 7/27/2021 by Mark Sutherland, MD
(Updated: 5/6/2026)
Click here to contact Mark Sutherland, MD
The much anticipated REMAP-CAP trial was epublished ahead of print July 12th in Intensive Care Medicine. It was an RCT investigating four antiviral strategies in critically ill adults with COVID-19: lopinavir-ritonavir, hydroxychloroquine, a combination of the two, and no antiviral therapy (control group).
Despite the hype around protease inhibitors, hydroxychloroquine, and other unproven therapies in COVID (lookin at you next, Ivermectin...), all three strategies had WORSE outcomes than placebo. They all decreased organ-support-free days (all reaching statistical significance), which was the primary outcome. They also all led to longer ICU time, longer time to hospital discharge, and reduced 90 day survival. Not only does this study show no benefit, it shows fairly convincing signs of harm to these therapies.
Bottom Line: Protease inhibitors (e.g. lopinavir-ritonavir) and hydroxychloroquine are unproven therapies for critical COVID-19 infection, and are not recommended. Providers should focus on interventions with demonstrated benefit, most notably steroids and good supportive/critical care.
Arabi YM, Gordon AC, Derde LPG, Nichol AD, Murthy S, Beidh FA, Annane D, Swaidan LA, Beane A, Beasley R, Berry LR, Bhimani Z, Bonten MJM, Bradbury CA, Brunkhorst FM, Buxton M, Buzgau A, Cheng A, De Jong M, Detry MA, Duffy EJ, Estcourt LJ, Fitzgerald M, Fowler R, Girard TD, Goligher EC, Goossens H, Haniffa R, Higgins AM, Hills TE, Horvat CM, Huang DT, King AJ, Lamontagne F, Lawler PR, Lewis R, Linstrum K, Litton E, Lorenzi E, Malakouti S, McAuley DF, McGlothlin A, Mcguinness S, McVerry BJ, Montgomery SK, Morpeth SC, Mouncey PR, Orr K, Parke R, Parker JC, Patanwala AE, Rowan KM, Santos MS, Saunders CT, Seymour CW, Shankar-Hari M, Tong SYC, Turgeon AF, Turner AM, Van de Veerdonk FL, Zarychanski R, Green C, Berry S, Marshall JC, McArthur C, Angus DC, Webb SA; REMAP-CAP Investigators. Lopinavir-ritonavir and hydroxychloroquine for critically ill patients with COVID-19: REMAP-CAP randomized controlled trial. Intensive Care Med. 2021 Aug;47(8):867-886. doi: 10.1007/s00134-021-06448-5. Epub 2021 Jul 12. PMID: 34251506; PMCID: PMC8274471.
Category: Critical Care
Posted: 7/20/2021 by Mike Winters, MBA, MD
(Updated: 5/6/2026)
Click here to contact Mike Winters, MBA, MD
Hemophagocytic Lymphohistiocytosis (HLH)
Morrissette K, et al. Hemophagocytic lymphohistiocytosis in the emergency department: recognizing and evaluating a hidden threat. J Emerg Med. 2021;60:743-751.
Category: Critical Care
Keywords: cardiac arrest, CPR, cardiopulmonary resuscitation, hands-off time, CCF, chest compression fraction (PubMed Search)
Posted: 7/6/2021 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Despite the knowledge that minimizing interruptions in chest compressions during CPR is key to maintaing coronary perfusion pressure and chance of ROSC,1-4 difficulties in limiting hands-off time remain.
Dewolf et al.5 recently performed a prospective observational study using body cameras to find that 33% (623/1867) of their CPR interruptions were longer than the recommended 10 seconds:
Previous studies have shown an increase in hands-off time associated with the use of cardiac POCUS during rhythm checks as well.6,7
Bottom Line:
Category: Critical Care
Keywords: OHCA, hypothermia, normothermia (PubMed Search)
Posted: 6/29/2021 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Settings: International multicenter trials; 1:1 randomization, blinded assessment of outcomes.
Patients: adults with witnessed OHCA, regardless of initial rhythm. Patients had more than 20 minutes of CPR. Eligible patients were unconscious, not able to follow command, no verbal responses to painful stimuli.
Intervention: hypothermia to target of 33C for 28 hours, then rewarming at rate of 1/3C every hour until 37C.
Comparison: maintaining temperature at 37.5C or less. Cooling if body temperature reached 37.8C to 37.5C
Outcome: primary outcome was Any cause mortality at 6 months; secondary outcome was poor functional outcome at 6 months (modified Rankin Scale 4-6).
Study Results:
1. 930 hypothermia, mortality 465/925 (50%, RR 1.04, 95%CI 0.94-1.14); 488/881 (55%) had mRS 4-6 (RR 1.0, 95%CI 0.92-1.09).
2. 931 normothermia, mortality 446/925 (48%); 479/866 (55%) had mRS 4-6.
Discussion Points:
Conclusion:
Normothermia in coma patients after OHCA did not lead to higher morality or worse neurologic outcomes.
Dankiewicz J, Cronberg T, Lilja G, Jakobsen JC, Levin H, Ullén S, Rylander C, Wise MP, Oddo M, Cariou A, B?lohlávek J, Hovdenes J, Saxena M, Kirkegaard H, Young PJ, Pelosi P, Storm C, Taccone FS, Joannidis M, Callaway C, Eastwood GM, Morgan MPG, Nordberg P, Erlinge D, Nichol AD, Chew MS, Hollenberg J, Thomas M, Bewley J, Sweet K, Grejs AM, Christensen S, Haenggi M, Levis A, Lundin A, Düring J, Schmidbauer S, Keeble TR, Karamasis GV, Schrag C, Faessler E, Smid O, Otáhal M, Maggiorini M, Wendel Garcia PD, Jaubert P, Cole JM, Solar M, Borgquist O, Leithner C, Abed-Maillard S, Navarra L, Annborn M, Undén J, Brunetti I, Awad A, McGuigan P, Bjørkholt Olsen R, Cassina T, Vignon P, Langeland H, Lange T, Friberg H, Nielsen N; TTM2 Trial Investigators. Hypothermia versus Normothermia after Out-of-Hospital Cardiac Arrest. N Engl J Med. 2021 Jun 17;384(24):2283-2294. doi: 10.1056/NEJMoa2100591. PMID: 34133859.
Category: Critical Care
Keywords: cardiac arrest, ROSC, computed tomography, CT scan, imaging (PubMed Search)
Posted: 6/16/2021 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
A recent prospective observational study examined the diagnostic usefulness of head-to-pelvis sudden death computed tomography (SDCT) in 104 patients with ROSC and unclear OHCA etiology.
Diagnostic performance:
Safety:
Bottom Line: For OHCA without clear etiology, SDCT explicitly including a thoracic CTA may have diagnostic benefit over standard care alone with the added benefit of identification of resuscitation complications.
Branch KRH, Strote J, Gunn M, et al. Early head-to-pelvis computed tomography in out-of-hospital circulatory arrest without obvious etiology. Acad Emerg Med. 2021 Apr;28(4):394-403. doi: 10.1111/acem.14228.
Category: Critical Care
Keywords: midodrine; septic shock; vasopressors; ICU LOS (PubMed Search)
Posted: 6/8/2021 by Kim Boswell, MD
Click here to contact Kim Boswell, MD
A recent pilot study was conducted in two centers (Mayo Clinic & Cleveland Clinic Affiliate) and aimed to evaluate if the administration of oral midodrine in early septic shock could decrease the use of IV vasopressors and decrease ICU and hospital length of stay (LOS). The study was a placebo-controlled, double blinded randomized trial.
This study enrolled:
The study did not find a statistical difference between the two groups in the use of vasopressors or ICU/Hospital LOS. However, there was a trend in the midodrine group which is suggestive of decreased vasopressor use and ICU/Hospital LOS.
It is Important to note the study was not powered to determine clinical significance. Overall the trend noted in the midodrine group should encourage further studies that are clinically powered to determine if there is a statistical difference and therefore a potential benefit to early initiation of oral midodrine in septic shock.
Lal, A, Trivedi, V, Rizvi, MS, et al. Oral Midodrine Administration During the First 24 Hours of Sepsis to Reduce the Need of Vasoactive Agents: Placebo-Controlled Feasibility Clinical Trial, Critical Care Explorations: May 2021 - Volume 3 - Issue 5 - p e0382
doi: 10.1097/CCE.0000000000000382
Category: Critical Care
Keywords: Pressors, Vasopressin, Sepsis, Septic Shock (PubMed Search)
Posted: 5/31/2021 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Norepinephrine is widely considered the first-line vasopressor for patients in septic shock. Vasopressin is often added to norepinephrine in patients requiring escalating doses, but when to add vasopressin, and what exactly the benefit is (as opposed to just further titrating up the norepinephrine) remain unclear. Given the limited evidence for a patient-oriented benefit and the increasing cost of vasopressin, some centers are becoming more judicious in the use of vasopressin. A systematic review in AJEM October 2021 examined the literature on early (< 6 hours of diagnosis) addition of vasopressin to the management of septic shock patients, compared to either no vasopressin or starting it after 6 hours.
Improved with early vasopressin: Need for renal replacement therapy (RRT; secondary outcome)
No difference: mortality, ICU length of stay, hospital length of stay, new onset arrhythmias
Bottom Line: When, and if, to start vasopressin in patients requiring escalating doses of norepinephrine remains controversial. Based on the prior VASST trial, many providers will start vasopressin when norepi doses reach ~ 5-15 mcg/min (approx 0.1-0.2 mcg/kg/min), but there remains limited data to support this practice, and either starting vasopressin or continuing to titrate the norepinephrine as needed are both reasonable approaches in most patients.
1) Huang H, Wu C, Shen Q, Xu H, Fang Y, Mao W. The effect of early vasopressin use on patients with septic shock: A systematic review and meta-analysis. Am J Emerg Med. 2021 May 6;48:203-208. doi: 10.1016/j.ajem.2021.05.007. Epub ahead of print. PMID: 33975132.
2) Russell JA, Walley KR, Singer J, Gordon AC, Hébert PC, Cooper DJ, Holmes CL, Mehta S, Granton JT, Storms MM, Cook DJ, Presneill JJ, Ayers D; VASST Investigators. Vasopressin versus norepinephrine infusion in patients with septic shock. N Engl J Med. 2008 Feb 28;358(9):877-87. doi: 10.1056/NEJMoa067373. PMID: 18305265.
3) Lam SW, Barreto EF, Scott R, Kashani KB, Khanna AK, Bauer SR. Cost-effectiveness of second-line vasopressors for the treatment of septic shock. J Crit Care. 2020 Feb;55:48-55. doi: 10.1016/j.jcrc.2019.10.005. Epub 2019 Oct 23. PMID: 31706118.
Category: Critical Care
Posted: 5/25/2021 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Refractory Anaphylaxis
Krishnaswamy G. Critical care management of anaphylaxis: A conside definitive review. Crit Care Med. 2021.
Category: Critical Care
Keywords: COVID-19, tocilizumab, ICU, mechanical ventilation (PubMed Search)
Posted: 5/11/2021 by Lindsay Ritter, MD
(Updated: 5/6/2026)
Click here to contact Lindsay Ritter, MD
RECAP: RECOVERY trial is a large, randomized, open label, adaptive trial studying different treatments on COVID-19. Most well known is the use of dexamethasone which reduced mortality by 1/3 in COVID patients requiring mechanical ventilation and by 1/5 in those requiring oxygen, with no benefit on those patients not requiring oxygen.
They recently published results in the Lancet on the use of tocilizumab.
Population:
Inclusion:
Outcomes:
Results:
Conclusion:
RECOVERY Collaborative Group Tocilizumab in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label, platform trial. Lancet. 2021; 397: 1637-1645
Category: Critical Care
Keywords: cardiac arrest, massive pulmonary embolism, Venoarterial, ECMO (PubMed Search)
Posted: 5/4/2021 by Quincy Tran, MD, PhD
(Updated: 5/6/2026)
Click here to contact Quincy Tran, MD, PhD
Background:
Cardiac arrest from massive pulmonary embolism (PE) can be up to 90% (1). A recent systemic review evaluated the efficacy of Venoarterial-Extracorporeal Membrane Oxygenation (VA-ECMO) for PE-related cardiac arrest.
Results:
The authors screened 1115 articles and included 77 articles, including gray literature. The authors performed a quantitative analysis of a total of 301 patients.
Overall, 183/301 (61%) patients survived to hospital discharge, a significant improvement from 90%.
Patients who were cannulated during chest compression were associated with 7x higher odds of death (OR, 6.84; 95% CI, 1.53–30.58; p = 0.01), compared to those who were cannulated after ROSC. However, cannulation in the ED was not associated with improved outcomes, compared with other cannulation site.
No increased risk of death among patients who received tPA prior to VA-ECMO vs. those who did not (OR, 0.78; 95% CI, 0.39–1.54; p = 0.48).
Patients whose age > 65 years of age were associated with 3X risk of death, compared to those with age < 65 years (OR, 3.56; 95% CI, 1.29–9.87; p = 0.02).
Take-home points
Please consider “early” VA-ECMO for eligible patients who have cardiac arrest from massive PE. However, it will take great convincing to push the PERT team to cannulate for VA-ECMO while the patient is still receiving chest compression.
1.Lavonas EJ, Drennan IR, Gabrielli A, et al: Part 10: Special circumstances of resuscitation: 2015 American Heart Association guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 2015; 132:S501–S518.
2. Scott JH, Gordon M, Vender R, Pettigrew S, Desai P, Marchetti N, Mamary AJ, Panaro J, Cohen G, Bashir R, Lakhter V, Roth S, Zhao H, Toyoda Y, Criner G, Moores L, Rali P. Venoarterial Extracorporeal Membrane Oxygenation in Massive Pulmonary Embolism-Related Cardiac Arrest: A Systematic Review. Crit Care Med. 2021 May 1;49(5):760-769. doi: 10.1097/CCM.0000000000004828. PMID: 33590996.
Category: Critical Care
Keywords: cardiac arrest, massive pulmonary embolism, Venoarterial, ECMO (PubMed Search)
Posted: 5/4/2021 by Quincy Tran, MD, PhD
Click here to contact Quincy Tran, MD, PhD
Background:
Cardiac arrest from massive pulmonary embolism (PE) can be up to 90% (1). A recent systemic review evaluated the efficacy of Venoarterial-Extracorporeal Membrane Oxygenation (VA-ECMO) for PE-related cardiac arrest.
Results:
The authors screened 1115 articles and included 77 articles, including gray literature. The authors performed a quantitative analysis of a total of 301 patients.
Overall, 183/301 (61%) patients survived to hospital discharge, a significant improvement from 90%.
Patients who were cannulated during chest compression were associated with 7x higher odds of death (OR, 6.84; 95% CI, 1.53–30.58; p = 0.01), compared to those who were cannulated after ROSC. However, cannulation in the ED was not associated with improved outcomes, compared with other cannulation sites.
No increased risk of death among patients who received tPA prior to VA-ECMO vs. those who did not (OR, 0.78; 95% CI, 0.39–1.54; p = 0.48).
Patients whose age > 65 years of age were associated with 3X risk of death, compared to those with age < 65 years (OR, 3.56; 95% CI, 1.29–9.87; p = 0.02).
Take-home points
Please consider “early” VA-ECMO for eligible patients who have cardiac arrest from massive PE. However, it will take great convincing to push the PERT team to cannulate for VA-ECMO while the patient is still receiving chest compression.
1.Lavonas EJ, Drennan IR, Gabrielli A, et al: Part 10: Special circumstances of resuscitation: 2015 American Heart Association guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 2015; 132:S501–S518.
2. Scott JH, Gordon M, Vender R, Pettigrew S, Desai P, Marchetti N, Mamary AJ, Panaro J, Cohen G, Bashir R, Lakhter V, Roth S, Zhao H, Toyoda Y, Criner G, Moores L, Rali P. Venoarterial Extracorporeal Membrane Oxygenation in Massive Pulmonary Embolism-Related Cardiac Arrest: A Systematic Review. Crit Care Med. 2021 May 1;49(5):760-769. doi: 10.1097/CCM.0000000000004828. PMID: 33590996
Category: Critical Care
Keywords: COPD, emphysema, acute respiratory failure, hypoxia, oxygen saturation (PubMed Search)
Posted: 4/20/2021 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Supplemental oxygen therapy is frequently required for patients presenting with acute respiratory distress and COPD exacerbation. Over-oxygenation can derail compensatory physiologic responses to hypoxia,1 resulting in worsening VQ mismatch and, to a lesser degree, decreases in minute ventilation, that cause worsened respiratory failure.
The 2012 DECAF (Dyspnea, Eosinopenia, Consolidation, Acidaemia, and Atrial Fibrillation) score was found to predict risk of in-hospital mortality in patients admitted with acute COPD exacerbation.2,3 Data from the DECAF study’s derivation and external validation cohorts were examined specifically to look at outcome associated with varying levels of oxygen saturation.
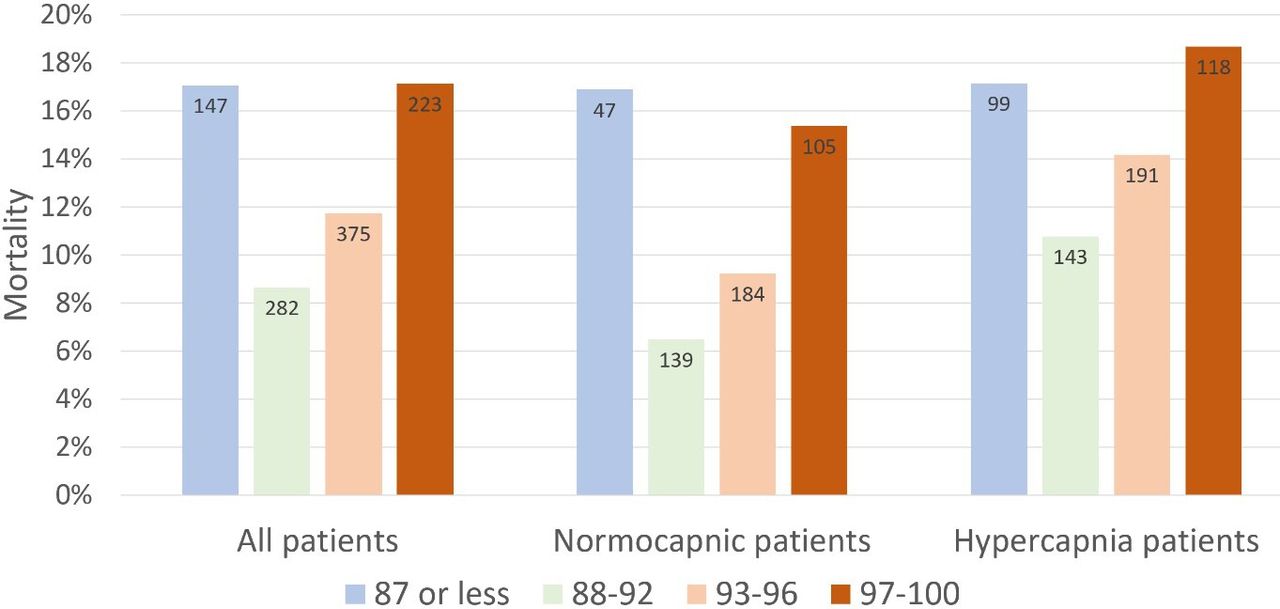
Bottom Line
In patients presenting to the ED with acute COPD exacerbation requiring oxygen supplementation, a target oxygen saturation of 88-92% is associated with the lowest in-hospital mortality, and higher oxygen saturations should be avoided independent of patients' PCO2 levels.
Category: Critical Care
Keywords: COVID-19, Anticoagulation, Thromboembolism (PubMed Search)
Posted: 4/7/2021 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Two items from the recent INSPIRATION trial UMEM pearl were very well pointed out by our own Dr. Michael Scott and require clarification. Thank you to all our readers for their close attention, and please know that we always appreciate you reaching out with questions/comments.
Category: Critical Care
Keywords: COVID-19, Anticoagulation, Thromboembolism (PubMed Search)
Posted: 4/7/2021 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
COVID-19 is generally regarded as a hypercoagulable state, and the role of pulmonary emboli and other VTE in COVID remains unclear. As a result, how to optimally provide prophylactic anticoagulation in COVID-19 patients who are not known to have VTE has been a point of debate.
The INSPIRATION trial looked at 600 patients admitted to academic ICUs in Iran, and compared what is often-referred to as "intermediate-dose" prophylaxis (in this case 1 mg/kg daily of enoxaparin) to standard dose prophylaxis (40 mg/day of enoxaparin). The study utilized a combined endpoint of venous thromboembolism, arterial thromboembolism, need for ECMO, or mortality. As a reminder, composite endpoints can skew results. However, the dose and type of anticoagulant chosen is similar to many academic centers around the world, and pharmacy guidelines often recommend providing this type of "intermediate-dose" prophylaxis in COVID-19 patients, sometimes based on clinical status, d-dimer or other coagulation-related patient-data. As with many things with COVID-19, this practice is based on limited data.
There was no significant difference between groups in the primary outcome (45.7% in intermediate ppx group vs 44.1% in standard group), and while safety outcomes were similar (major bleeding in 2.5% in the intermediate ppx group vs 1.4% in standard group), the intermediate regimen failed to demonstrate non-inferiority to the standard regimen for major bleeding.
Intermediate vs standard-dose ppx was similar in this study with a small, but statistically significant increase in major bleeding in the intermediate-dose group.
Bottom Line: Although this study had methodologic flaws and there are external validity concerns, the INSPIRATION trial supports the notion that standard dose (e.g. 40 mg/g/kg/day enoxaparin) and intermediate-dose (e.g. 1 mg/kg/day enoxaparin) VTE prophylaxis are equivalent in critically ill COVID-19 patients who do not already have a known VTE in terms of preventing negative VTE outcomes. Intermediate-dose may be associated with increased bleeding. As more critically ill patients require ED boarding, the dose of VTE prophylaxis may remain controversial, but the need to start it remains an important consideration.
INSPIRATION Investigators, Sadeghipour P, Talasaz AH, Rashidi F, Sharif-Kashani B, Beigmohammadi MT, Farrokhpour M, Sezavar SH, Payandemehr P, Dabbagh A, Moghadam KG, Jamalkhani S, Khalili H, Yadollahzadeh M, Riahi T, Rezaeifar P, Tahamtan O, Matin S, Abedini A, Lookzadeh S, Rahmani H, Zoghi E, Mohammadi K, Sadeghipour P, Abri H, Tabrizi S, Mousavian SM, Shahmirzaei S, Bakhshandeh H, Amin A, Rafiee F, Baghizadeh E, Mohebbi B, Parhizgar SE, Aliannejad R, Eslami V, Kashefizadeh A, Kakavand H, Hosseini SH, Shafaghi S, Ghazi SF, Najafi A, Jimenez D, Gupta A, Madhavan MV, Sethi SS, Parikh SA, Monreal M, Hadavand N, Hajighasemi A, Maleki M, Sadeghian S, Piazza G, Kirtane AJ, Van Tassell BW, Dobesh PP, Stone GW, Lip GYH, Krumholz HM, Goldhaber SZ, Bikdeli B. Effect of Intermediate-Dose vs Standard-Dose Prophylactic Anticoagulation on Thrombotic Events, Extracorporeal Membrane Oxygenation Treatment, or Mortality Among Patients With COVID-19 Admitted to the Intensive Care Unit: The INSPIRATION Randomized Clinical Trial. JAMA. 2021 Mar 18. doi: 10.1001/jama.2021.4152. Epub ahead of print. PMID: 33734299.
Category: Critical Care
Posted: 3/30/2021 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Improving Compliance with Lung-Protective Ventilation
Tallman CMI, et al. Impact of provding a tape measure on the provision of lung-protective ventilation. West J Emerg Med. 2021; 22:389-93.
