Category: Pharmacology & Therapeutics
Keywords: thrombin,dabigatran,partial thromboplastin,bleeding (PubMed Search)
Posted: 9/1/2011 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Rye J, Stangier J, Haertter S, et al. Dabigatran etexilate - a novel, reversible, oral direct thrombin inhibitor: Interpretation of coagulation assays and reversal of anticoagulant activity. Thrombosis and Haemostasis 2010. 103;1116-27.
Category: Neurology
Keywords: delirium (PubMed Search)
Posted: 8/31/2011 by Aisha Liferidge, MD
(Updated: 5/4/2026)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Keywords: ultrasound, tracheal intubation, esophageal intubation, critical care, airway (PubMed Search)
Posted: 8/30/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Multiple methods of confirming endotracheal tube placement exist, however quantitative waveform capnography is the most reliable method. Unfortunately this may not be immediately available at all medical centers.
Recent studies demonstrate that bedside ultrasound may assist in the detection of proper endotracheal tube placement.
The T.R.U.E. (Tracheal Rapid Ultrasound Exam) was demonstrated to be 99% sensitive, 94% specific, 99% PPV, and 94% NPV during intubation.
The basic exam involves placing a high-frequency linear-array probe on the anterior neck above the sternal notch and identifying the trachea and esophagus during intubation.
The following video is an example of what you DO NOT want to see during an intubation: http://www.youtube.com/watch?v=LvfThxhQ93A
Chou, H. et al. Tracheal rapid ultrasound exam (T.R.U.E.) for confirming endotracheal tube placement during emergency intubation. Resuscitation. Jun 2011
Werner SL,et al. Pilot study to evaluate the accuracy of ultrasonography in confirming endotracheal tube placement. Ann Emerg Med 2007;49:75–80.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Visual Diagnosis
Posted: 8/29/2011 by Rob Rogers, MD
(Updated: 5/4/2026)
Click here to contact Rob Rogers, MD
Patient presents with right-sided chest and shoulder pain....
What's the diagnosis?
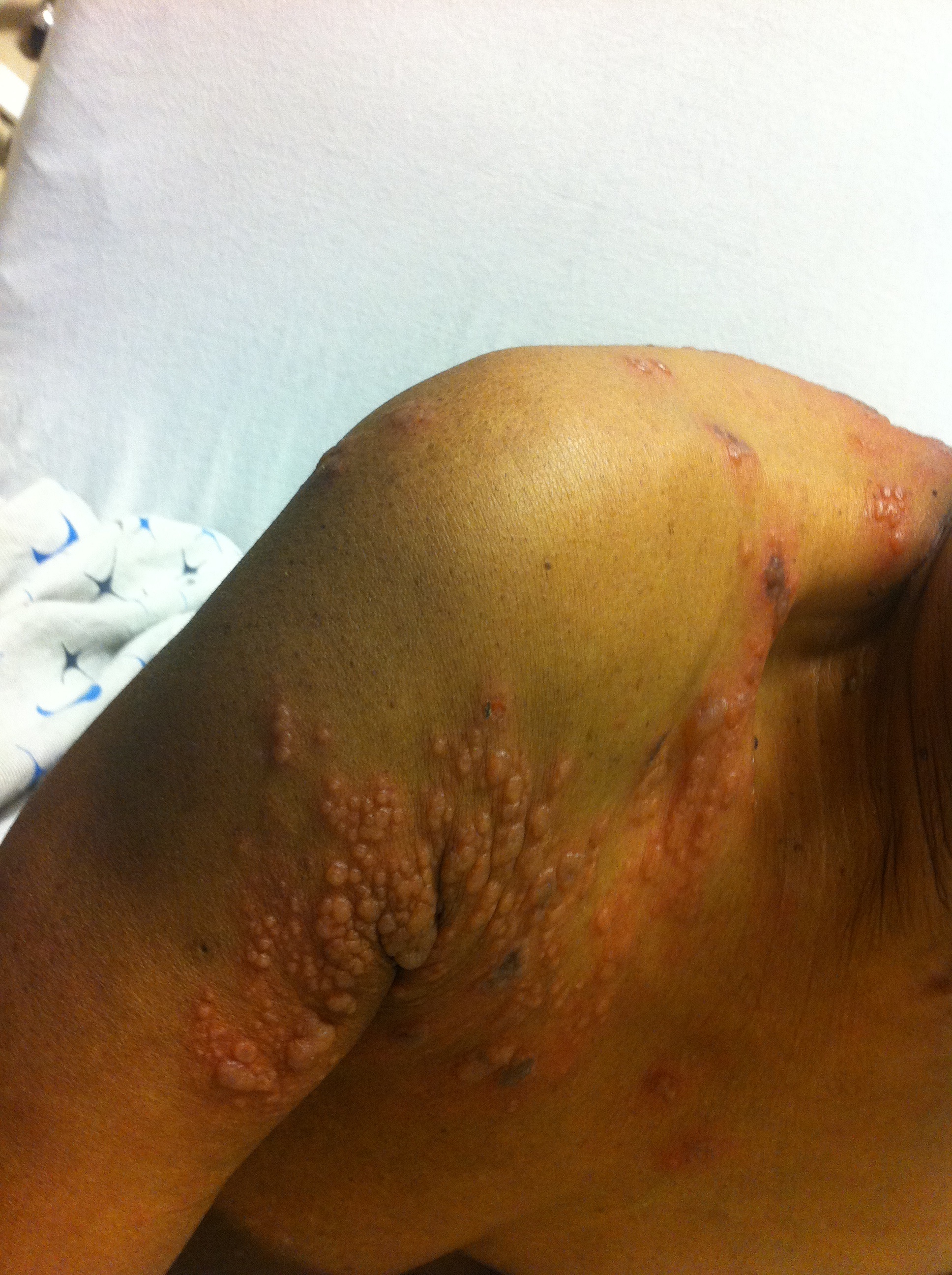
Herpes Zoster
Category: Cardiology
Keywords: therapeutic hypothermia, induced hypothermia, cardiac arrest, post arrest care (PubMed Search)
Posted: 8/28/2011 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
If you're like me, you've been a bit confused about what exactly defines "coma" in the current recommendations for post-arrest hypothermia in "comatose" patients with return of spontaneous circulation. Fortunately, a recent NEJM article has helped clarify this by suggesting that hypothermia should be induced in these post-arrest patients with either:
Naturally, if the patient was comatose before the arrest, don't bother.
Holzer M. Targeted temperature management for comatose survivors of cardiac arrest. N Engl J Med 2010;363:1256-1264.
Category: Orthopedics
Keywords: knee dislocation (PubMed Search)
Posted: 8/27/2011 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Stability from 4 major ligaments (ACL, PCL, MCL and LCL)
Knee dislocation causes injury to multiple ligaments (usually 3 of the above).
Many of these dislocation spontaneously reduce prior to medical evaluation. Therefore, consider knee dislocation in a patient with multi ligament injury, significant hemarthrosis and bruising.
Vascular injury in up to 40% (popliteal artery)
Nerve injury in up to 23% (peroneal nerve) ((ankle dorsiflexion and sensation to the first web space of the foot))
After reduction, immobilize knee in 15-20 degrees flexion.
The degree of initial deformity, presence of strong pulses, or warm skin cannot be used to rule out popliteal injury.
Category: Pediatrics
Keywords: severe asthma, decreased hospitalization (PubMed Search)
Posted: 8/26/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Toxicology
Keywords: propofol (PubMed Search)
Posted: 8/25/2011 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
End Tidal CO2 continuous capnography is being utilized more in the ED for procedural sedation. One of the best studies is a randomized control trial using propofol that showed you could see signs of hypoventiliation prior to hypoxia by about 60 seconds - which can be plenty of time to get your BVM and airway cart ready.
Deitch K, Miner J, Chudnofsky CR, Dominici P, Latta D.
Ann Emerg Med. 2010 Mar;55(3):258-64. Epub 2009 Sep 24.
Category: Neurology
Keywords: ROSIER scale, ischemic stroke (PubMed Search)
Posted: 8/24/2011 by Aisha Liferidge, MD
(Updated: 5/4/2026)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 8/23/2011 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Re-expansion Pulmonary Edema After Chest Tube Placement
Hsu KF, et al. Re-expansion pulmonary edema after insertion of chest tube for pneumothorax. J Trauma 2011;70(3):761.
Category: Visual Diagnosis
Posted: 8/22/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
79 y.o. male lung cancer patient with tachypnea, tachycardia, and normal blood pressure. Click here: http://vimeo.com/27973006
Possible diagnosis?
Answer: Right ventricular (RV) dysfunction secondary to submassive pulmonary embolism (PE).
Ultrasound for suspected PE
Consider bedside echo with PE and elevated troponin or BNP.
Recall the classes of PE:
Ultrasound “clues” of submassive / massive PE:
Lodato JA, Parker Ward RP, Lang RM. Echocardiographic Predictors of Pulmonary Embolism in Patients Referred for Helical CT. Echocardiography 2008;25:584-590.
McConnell MV, Solomon SD, Rayan ME, et. al. Regional Right Ventricular Dysfunction Detected by Echocardiography in Acute Pulmonary Embolism. Am J Cardiol. 1996; 78: 469-473.
ACEP. Critical Issues in the Evaluation and Management of Adult Patients Presenting to the Emergency Department With Suspected Pulmonary Embolism. http://www.acep.org/content.aspx?id=30060. [July 24, 2011].
John Griffiths. Respiratory: Management of small, submassive and massive pulmonary embolism. http://www.frca.co.uk/article.aspx?articleid=100750. [July 24, 2011].
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Geriatrics
Keywords: acute MI, MI, myocardial infarction, geriatrics, elderly, acute coronary syndrome (PubMed Search)
Posted: 8/21/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
Elderly patients are high risk for missed MI because of atypical presentations. Though this seems to be relatively common knowledge, it is not always remembered. So here's a reminder....
Samaras, N, Chevalley, T, et al. “Older patients in the emergency department: a review.” Ann Emerg Med. 2010;56:261-269.
Category: Pediatrics
Keywords: weakness, constipation (PubMed Search)
Posted: 8/20/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Infantile botulism
Category: Toxicology
Keywords: propofol, procedural sedation, fospropofol (PubMed Search)
Posted: 8/18/2011 by Fermin Barrueto
Click here to contact Fermin Barrueto
If you think the controversy was just heating up for propofol use in the Emergency Department, just wait until the new agent begins arriving to an ED near you - fospropofol. A new water soluble version of propofol, this agent will remove the problems of pain at the injection site, an easier/wider therapeutic window for sedation and allowing of long-term sedation without the heavy lipid load.
Currently, there is limited FDA approval in the US for monitored anesthesia care. I am waiting for the first paper showing its use in the ED for procedural sedation. Safety data is still growing.
Mini-pearl: Patients allergic to soybean should either avoid propofol or undergo skin testing since the emulsion is made of soybean oil and egg lecithin. There have been reported cases of anaphylaxis after administration of propofol in patients with food allergies, peanut and birch.
Fospropofol: a new sedative-hypnotic agent for monitored anesthesia care.
Moore GD, Walker AM, MacLaren R.
Ann Pharmacother. 2009 Nov;43(11):1802-8. Epub 2009 Oct 13. Review.
Possible anaphylaxis after propofol in a child with food allergy.
Hofer KN, McCarthy MW, Buck ML, Hendrick AE.
Ann Pharmacother. 2003 Mar;37(3):398-401.
Category: Neurology
Keywords: tumor, dandy-walker syndrome, craniosynostosis, increased intracranial pressure, spina bifida (PubMed Search)
Posted: 8/17/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
- Tumor - more likely if in lateral ventricles, posterior fossa, or intraspinal.
- Spina Bifida - blocked cerebrospinal fluid (CSF) flow may cause Chiari Malformation II.
- Congenital Aqueductal Stenosis - associated with mental retardation, abducted thumbs.
- Craniosynostosis - results from premature closure of skull sutures.
- Dandy-Walker Syndrome - cystic deformity of fourth ventricle, hypoplasia of cerebellar
vermis, and enlarged posterior fossa.
- Arachnoid Cyst - common locations include middle and posterior fossa.
Category: Critical Care
Keywords: bougie, cricothyrotomy, trauma, critical care, intubation, failed airway (PubMed Search)
Posted: 8/16/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
The open cricothyrotomy technique is taught as the trauma airway standard when one “cannot intubate and cannot ventilate” however, it is not without difficulty and limitations. The B.A.C.T. (Bougie-Assisted Cricothyrotomy Technique) may improve the procedure by using a bougie to assist.
Steps for the B.A.C.T. (as described in the paper):
1. Stabilize the larynx with the thumb and middle finger, then identify the cricothyroid membrane.
2. Make a transverse stabbing incision with a scalpel through both skin and cricothyroid membrane.
3. Insert tracheal hook at the inferior margin of the incision and pull up on the trachea.
4. Insert a bougie through the incision with curved tip directed towards the feet
5. Pass 6-0 endotracheal tube or Shiley over bougie into trachea.
Advantages of a bougie:
1. Thin and easy to insert into incision
2. Tactile feedback from tracheal rings confirms proper placement
3. Ensures that stoma will not be lost during procedure
EMRAP.tv has a great video of Dr. Darren Braude demonstrating the procedure;
http://bit.ly/nB3BMG
Hill, C., et al. Cricothyrotomy Technique Using Gum Elastic Bougie Is Faster Than Standard Technique: A Study of Emergency Medicine Residents and Medical Students in an Animal Lab. Academic Emergency Medicine17(6), 666–669.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Geriatrics
Keywords: infection, sepsis, bacteremia, geriatrics, elderly (PubMed Search)
Posted: 8/14/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
The most common sources of bacteremia and serious bacterial infections in the elderly are the GU tract, the respiratory tract, and #3-the abdomen.
This third source is a bit of a surprise to many clinicians but worth remembering. Always consider the abdomen as the source of dangerous infections in the elderly when the source is not clearly the lungs or urine!
Caterino JM. Evaluation and management of geriatric infections in the emergency department. Emerg Med Clin N Am 2008;26:319-343.
Category: Orthopedics
Keywords: Brachial plexus neuritis, neck pain (PubMed Search)
Posted: 8/13/2011 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
Acute brachial plexus neuritis is an uncommon disorder that is easily confused with cervical radiculopathy.
Patients present with a characteristic pattern of acute onset of burning pain. Pain subsides in days to weeks and is then followed by profound weakness and muscle wasting changes affecting the shoulder and upper extremity. Weakness is best identified in the deltoid, biceps and rotator cuff muscles. Strength gradually recovers over 3-4 months.
DDX: The constellation of pain, weakness and sensory loss associated with cervical radiculopathy tend to occur simultaneously. Also cervical radiculopathy tends to involve only a single root.
ED treatment is with analgesics and physical therapy and PCP referral for outpatient MRI/EMG. Consider a sling in those with severe shoulder weakness.
Category: Toxicology
Keywords: adenosine, caffeine (PubMed Search)
Posted: 8/9/2011 by Bryan Hayes, PharmD
(Updated: 8/11/2011)
Click here to contact Bryan Hayes, PharmD
Caffeine can interfere with the successful reversion of paroxysmal supraventricular tachycardia (SVT) by adenosine.
Caffeine is an adenosine receptor blocker.
Ingestion of caffeine less than 4 hours before a 6-mg adenosine bolus significantly reduced its effectiveness in the treatment of SVT. Theophylline is similar but not many patients are prescribed it anymore.
An increased initial adenosine dose may be indicated for these patients. A first dose of 12 mg (instead of 6), followed by 2nd and 3rd doses of 18 mg (instead of 12) may be indicated.
Cabalag MS, et al. Recent caffeine ingestion reduces adenosine efficacy in the treatment of paroxysmal supraventricular tachycardia. Acad Emerg Med 2009;17(1):44-9.
Category: Neurology
Keywords: cerebrospinal fluid, meningitis, lumbar puncture (PubMed Search)
Posted: 8/10/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
