Category: Toxicology
Keywords: idiopathic intracranial hypertension, pseudotumor cerebri, tetracycline, vitamin a (PubMed Search)
Posted: 10/11/2011 by Bryan Hayes, PharmD
(Updated: 11/10/2011)
Click here to contact Bryan Hayes, PharmD
Several medications have been linked to causing idiopathic intracranial hypertension (pseudotumor cerebri). Be sure to record an accurate medication history in patients you suspect of having this diagnosis.
Withdrawal of the offending agent will generally resolve the symptoms.
Category: Neurology
Keywords: lithium toxicity, hemodialysis, whole bowel irrigation (PubMed Search)
Posted: 11/9/2011 by Aisha Liferidge, MD
(Updated: 5/4/2026)
Click here to contact Aisha Liferidge, MD
Perrone J, Chatterjee P. "Lithium Poisoning." UpToDate. May 2011. Retrieved from: http://www.uptodate.com/contents/lithium-poisoning?source=search_result&search=lithium+tocity&selectedTitle=2%7E150#H24.
Category: Critical Care
Keywords: tamponade, critical care, intubation, positive pressure, PEA arrest (PubMed Search)
Posted: 11/8/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Positive-pressure ventilation (e.g., mechanical ventilation) increases intrathoracic pressure potentially reducing venous return, right-ventricular filling, and cardiac output.
Pericardial tamponade similarly causes hemodynamic compromise through increased pericardial pressure which reduces right-ventricular filling and cardiac output.
When mechanically ventilating a patient with known or suspected pericardial tamponade the mechanisms above may be additive, causing cardiovascular collapse and possibly PEA arrest.
For the patient with known or suspected pericardial tamponade consider draining the pericardial effusion prior to intubation or delaying intubation until absolutely necessary.
If intubation is unavoidable, consider maintaining the intrathoracic pressure as low as possible (by keeping the PEEP and tidal volumes to a minimum) to ensure adequate cardiac filling and cardiac output.
Ho, A. et. al. Timing of tracheal intubation in traumatic cardiac tamponade: A word of caution. Resuscitation, 80(2), 272–274.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: obesity, shock, blood pressure (PubMed Search)
Posted: 11/6/2011 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
Blood pressure cuffs tend to OVERESTIMATE true blood pressure in obese patients. Even larger cuffs tend to do this as well. While low blood pressures are often reliable in diagnosing shock, be wary of assuming a "normal" blood pressure (e.g. SBP 100-120s) rules out shock in an obese patient who is sick. A-lines might be necessary to accurately assess the blood pressure.
[adapted from ACEP talk by Dr. Tiffany Osborn]
Category: Pharmacology & Therapeutics
Keywords: nicardipine, labetalol, blood pressure (PubMed Search)
Posted: 10/30/2011 by Bryan Hayes, PharmD
(Updated: 11/5/2011)
Click here to contact Bryan Hayes, PharmD
A recent randomized trial compared nicardipine as a continuous infusion to labetalol boluses to determine which one was more effective at lowering blood pressure to a target range within 30 minutes.
Median initial SBP for the 226 patients was 212 mm Hg. Within 30 minutes, nicardipine patients more often reached target range than labetalol (91.7 vs. 82.5%, P = 0.039). Of 6 BP measures (taken every 5 minutes) during the study period, nicardipine patients had higher rates of five and six instances within target range than labetalol (47.3% vs. 32.8%, P = 0.026).
What this means: Nicardipine is a reasonable choice for patients needing acute lowering of blood pressure (e.g., ischemic stroke with tPa). Nicardipine seems to achieve faster and smoother lowering of blood pressure than labetalol therapy with less blood pressure readings outside the target range.
Peacock WF, Varon J, Baumann BM, et al. CLUE: a randomized comparative effectiveness trial of IV nicardipine versus labetalol use in the emergency department. Crit Care 2011;15(3):R157. Epub 2011 Jun 27.
Category: Toxicology
Keywords: salicylate, aspirin, alkalosis, acidosis (PubMed Search)
Posted: 11/3/2011 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Salicylates:
Overall, this results in a mixed respiratory alkalosis and metabolic acidosis.
Micromedex; Poisindex, salicylate poisoning.
Category: Neurology
Keywords: stroke, iPhone, NIH Stroke Scale (PubMed Search)
Posted: 11/2/2011 by Aisha Liferidge, MD
(Updated: 5/4/2026)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 11/1/2011 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Mechanical Ventilation in Patients with Pulmonary HTN
Category: Visual Diagnosis
Posted: 10/30/2011 by Haney Mallemat, MD
(Updated: 10/31/2011)
Click here to contact Haney Mallemat, MD
72 year-old man, one-week post right fem-pop bypass presents with painful blue and black toe. Diagnosis?
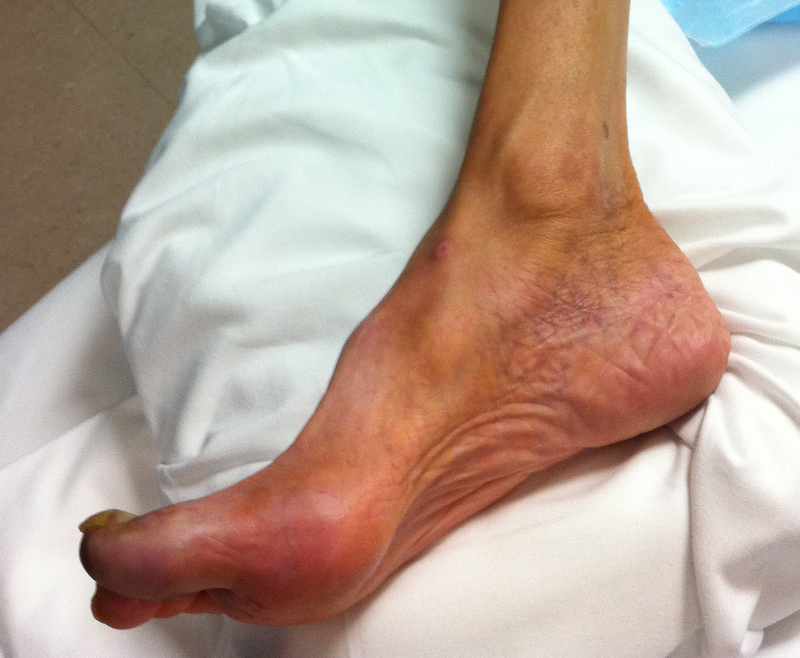
Answer: Blue-Toe Syndrome
Hirschman, J. et al. Blue (or purple) toe syndrome. J Am Acad Dermatol.2009 Jan;60(1):1-20
O'Keeffe S, et al. Blue toe syndrome: Causes and management.Arch Intern Med. 1992 Nov;152(11):2197-202.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: defibrillation, tachydysrhythmia, ventricular fibrillation (PubMed Search)
Posted: 10/30/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
Today's cardiology pearl provided by EMS guru Dr. Ben Lawner. Consider this one if you are caring for a patient with what appears to be shock-resistant VFib.
An intervention that has its roots in the electrophysiology lab has now gained traction on the front lines of resuscitation: double sequential defibrillation. Prospective studies are currently underway to examine the feasibility of this technique. New Orleans (LA) EMS boasts several anectodal accounts of survival, with neurologically intact recovery, from refractory ventricular fibrillation. The next time you can’t stop the fibbing, consider this:
· Apply TWO sets of defibrillator pads to the patient; one in traditional sternum/apex configuration and the other in anterior/posterior configuration
· If ventricular fibrillation persists despite several shocks, coordinate the simultaneous firing of BOTH defibrillators
Some caveats:
This treatment is based upon EP lab data; each MONOPHASIC defibrillator was set at 360J. EMS services in New Orleans and Wake County (NC) have used two biphasic defibrillators, each set a 200J. There is not sufficient data to make any widespread recommendation, but the idea of double sequential defibrillation may be another tool in a limited ACLS bag of tricks for patients who simply cannot come out of V-fib. New Orleans EMS has initiated the double-defib protocol after four shocks, and Wake County’s protocol recommends initiation after five. Wake's protocol also recommends firing the defirbillators "as synchronously as possible."
DH Hoch, WP Batsford, SM Greenberg, CM McPherson, et al. Double sequential defibrillation for refractory ventricular defibrillation. J. Am Cardiol. 1994;23:1141-45.
Category: Toxicology
Keywords: overdose, methotrexate (PubMed Search)
Posted: 10/27/2011 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Methotrexate is a chemotherapeutic that is utilized in non-Hodgkin lymphoma and breast CA. It is also used as an immunosuppressant for rheumatoid arthritis and psoriasis. Finally, we see it used in the ED for the treatment of ectopic pregnancy. Overdose, often unintentional, can have a lethal outcome.
Toxicity: LFTs rise, N/V, stomatitis, mucositis, leukopenia, thrombocytopenia, renal failure
Antidote: Leukovorin (Folinic Acid)
Other Tx: Carboxypeptidase G2, Charcoal Hemoperfusion, HD (possible)
Category: Neurology
Keywords: myasthenia graves, MG (PubMed Search)
Posted: 10/26/2011 by Aisha Liferidge, MD
(Updated: 5/4/2026)
Click here to contact Aisha Liferidge, MD
- Mask-like face
- Eyelid weakness
-- leads to ptosis
-- exacerbated by sustained upward gaze
-- improved by closing the eyes for a short while
- Extraocular motion abnormality
-- usually affects more than one extraocular muscle
-- may be assymetrical
-- may result in mild proptosis
- Weak palatal muscles
-- nasal-sounding voice
-- nasal regurgitation of food
- Weak jaw muscles
- Absent gag reflex
- Pupils normal
Category: Critical Care
Keywords: xigris, activated protein C, sepsis, multi-organ failure, resuscitation (PubMed Search)
Posted: 10/25/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
On October 25, 2011, Eli Lilly announced a voluntary-recall of activated drotrecogin alfa (Xigris) following a recent trial (PROWESS-SHOCK), which demonstrated no survival benefit when using the drug when compared to placebo.
Activated drotrecogin alfa is a recombinant form of human activated protein C previously recommended for adults with severe sepsis and a high-risk of death (APACHE II > 25 or multi-organ failure); it is included in the 2008 International Sepsis Guidelines (Grade 2b recommendation).
The PROWESS-SHOCK trial reported an all-cause mortality rate of 26.4% in the drotrecogin alfa group compared with 24.2% in the placebo group; this difference was not statistically significant.
Interestingly, the study also found that severe bleeding (the drug's main side-effect) was found to be 1.2% in the activated drotrecogin alfa group compared to 1.0% for the placebo group (also non-significant) suggesting it does not increase the risk of bleeding as it had previously been reported.
Hospitals should revise their sepsis guidelines based on this recent news.
www.medscape.com/viewarticle/752169?sssdmh=dm1.728719&src=nl_newsalert
Dellinger, R. P., et al. Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Critical Care Medicine, 36(1), 296–327. doi:10.1097/01.CCM.0000298158.12101.41
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Misc
Posted: 10/24/2011 by Rob Rogers, MD
(Updated: 5/4/2026)
Click here to contact Rob Rogers, MD
Weird and Unusual Symptoms
Bet you didn't know that severe and intense pruritus of the nostrils, known as Wartenberg's symptom, is an uncommon but characteristic symptom of a brain tumor.
Etiologies include astrocytoma, glioblastoma, oligodendroglioma, medulloblastoma, and metastatic tumors.
1. Andreev VC, Petkov. Skin manifestations associated with tumors of the brain. Br J Dermatol 1975;92:675
2. Mark Marinella, Pocket Brain of 50 Unusual Symptoms. Blackwell Publishing
Category: Cardiology
Keywords: acute MI, MI, myocardial infarction, acute coronary syndrome, women (PubMed Search)
Posted: 10/23/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
"Women experience higher mortality rates and more adverse outcomes after acute MI than men, despite less obstructive CAD and plaque burden."(1)
How can this be explained? It turns out that women have more frequent coronary remodeling of vessels. "Remodeling" refers to the concept that as plaques grow, they tend grow into the vessel wall causing outward bulging of the wall, rather than growing into the vessel lumen. That means that standard coronary angiography and even stress testing often miss significant lesions because they only evaluate lumen obstruction....which is not directly reflective of plaque size/burden.
The net effect of the above is that women are more likely to have false negative stress tests and angiograms that appear to show non-significant occlusions. Until we have reliable tests that evaluate true plaque burden rather than just vessel occlusion, we can't completely rely on stress testing and angiography to rule out the the presence of significant plaques.
1. Della Rocca DG, Pepine CJ. What causes myocardial infarction in women without obstructive coronary artery disease? Circulation 2011;124:1404-1406.
2. Reynolds HR, Srichai MB, Iqbal SN, et al. Mechanisms of myocardial infarction in women without angiographically obstructive coronary artery disease. Circulation 2011;124:1414-1425.
Category: Orthopedics
Keywords: TFCC, triangular fibrocartilage complex, wrist (PubMed Search)
Posted: 10/23/2011 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
The TFCC (triangular fibrocartilage complex) is a ligamentous/cartilage like complex similar to the meniscus of the knee located on the ulnar side of the wrist.
http://yanyanxu.com/wp-content/uploads/2008/01/trifibcc.gif
Hx: ulnar sided wrist pain following trauma and associated with activity related mechanical symptoms such as clicking.
PE: tenderness to palpation distal to ulnar head or at ulnar styloid . Tenderness against resisted radial deviation.
Plain film may show ulnar styloid avulsion or injury to carpal structures.
Refer to hand/wrist surgeon
Splint in ulnar gutter of long arm spica
MRI or arthrogram are studies of choice.
http://www.cobalthealth.co.uk/MImageGen.ashx?image=%2Fmedia%2F12951%2Fwrist-tfcc-tear-big.jpg&width=170&crop=true
Category: Pediatrics
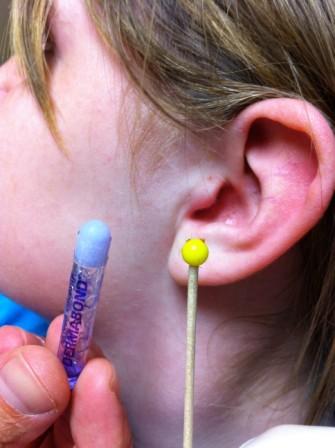
Keywords: dermabond, glue, foreign body, (PubMed Search)
Posted: 10/21/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Toxicology
Keywords: carbon monoxide (PubMed Search)
Posted: 10/20/2011 by Fermin Barrueto
Click here to contact Fermin Barrueto
Carbon Monoxide Toxicity and Hyperbaric Oxygen Treatment
CO disrupts cellular function by several mechanisms at a
cellular/mitochondrial level. Ultimately, these disruptions are
manifested as tissue hypoxia and hypoperfusion.
Initial symptoms may be subtle and nonspecific. Be sure to ask about
CO exposure when evaluating “viral syndrome” or patients that present
with non-specific neurological complaints especially during fall and
winter months, when people first start using their heating, or after
power outages and generator use. Dysrhythmias, cardiomopathy, MI and
sudden cardiac arrest are reported in severe CO poisoning.
Lab studies- COHb, base excess, lactate and any other studies based on
presentation.
Supplemental oxygen is the cornerstone of treatment. Oxygen
delivered at hyperbaric pressure (as opposed to sea-level) will
increase the rate of CO dissociation from hemoglobin, and mitigate
damage to cellular and mitochondrial function.
Definite Indications for HBOT: Current evidence supports the use for
HBOT to reduce cognitive sequelae in CO poisoned patients who have:
LOC , seizure, exposure >23 hours, COHb of 25% or more, and age >36.
Relative Indications: persistent symptoms after 100% O2 or change in
mental status, pregnancy, persistent cardiac ischemia, increased COHb
levels.
Disposition: Clinical judgment should guide your decision. Most
patients with mild symptoms can be discharged after treatment. If
patient has a more concerning presentation with several risk factors
(extremes of age, CAD, unconscious at arrival in the ED, etc…)
consider admission.
Category: Neurology
Keywords: fundoscopic examination, central retinal vein occlusion, central retinal artery occlusion (PubMed Search)
Posted: 10/19/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
Differentiating Central Retinal Artery vs. Vein Occlusion Fundoscopically
Category: Critical Care
Posted: 10/18/2011 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
SAH and Electrolyte Disorders
Wartenberg KE. Critical care of poor-grade subarachnoid hemorrhage. Curr Opin Crit Care 2011; 17:85-93
