Category: Trauma
Keywords: Whole blood, trauma (PubMed Search)
Posted: 3/22/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
Achieving faster homeostasis in trauma patients leads to lower mortality, less coagulopathy, and lower total blood volume transfusion requirements. This study looked at time to achieving homeostasis as defined by transfusion requirements as well as laboratory measurements in critically ill trauma patients who either received whole blood or component therapy transfusion as part of their resuscitation. Those receiving whole blood achieved statistically significant faster homeostasis.
Chipman, Amanda M. MD; Luther, James F. MA; Guyette, Francis X. MD, MPH; Cotton, Bryan A. MD; Cannon, Jeremy W. MD; Schreiber, Martin A. MD; Moore, Ernest E. MD; Namias, Nicholas MD, MBA; Minei, Joseph P. MD; Yazer, Mark H. MD; Vincent, Laura MS, RN; Cotton, Abigail L. BS, MPH; Agarwal, Vikas MD; Brown, Joshua B. MD, MSc; Leeper, Christine M. MD; Neal, Matthew D. MD; Forsythe, Raquel M. MD; Wisniewski, Stephen R. PhD; Sperry, Jason L. MD, MPH; the SWAT Study Group. Early achievement of hemostasis defined by transfusion velocity: A possible mechanism for whole blood survival benefit. Journal of Trauma and Acute Care Surgery 98(3):p 393-401, March 2025. | DOI: 10.1097/TA.0000000000004507
Category: Pediatrics
Keywords: CPR, pediatric cardiac arrest, termination, TOR (PubMed Search)
Posted: 3/21/2025 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
This was a retrospective analysis of pediatric cardiac arrests that occurred out of hospital in Japan, where no pediatric termination of resuscitation is allowed. 1007 arrests were included. Patients that were placed on ECMO were excluded. This study included both medical and traumatic arrests looking at a primary outcome of 1 month moderate or better neurological disability. CPR time for both EMS and the hospital prior to ROSC were included. Bystander CPR was not included in these calculations. Possible downtime prior to CPR was not taken into consideration.
Overall, less than 1% of pediatric patients exhibited one-month moderate disability or better neurological outcome when total CPR duration is more than 64 minutes.
Yasuda M, Amagasa S, Kashiura M, Yasuda H, Uematsu S. Duration of prehospital and in-hospital cardiopulmonary resuscitation and neurological outcome in paediatric out-of-hospital cardiac arrest. Emerg Med J. Published online October 15, 2024. doi:10.1136/emermed-2023-213730
Category: EMS
Keywords: TOR, pediatric cardiac arrest (PubMed Search)
Posted: 3/19/2025 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
A few states have pediatric out of hospital termination of resuscitation protocols. This study used CARES data to create a termination protocol that was not only linked to ROSC, but also to neurological outcomes. This study only included medical arrests.
21240 children were included in the study where 2326 patients survived to hospital discharge. A total of 1894 survived with a favorable neurological outcome. The criteria developed for pediatric TOR in this study had a specificity of 99.1% and a PPV of 99.8% for patient death. Another set of criteria had a 99.7% specificity and PPV of 99.9% for predicting death or survival with poor neurological outcome.
TOR criteria of death consisted of:
unwitnessed arrest
asystole
arrest not due to drowning or electrocution
no sustained ROSC
TOR criteria of death or survival with poor neurological outcome:
unwitnessed arrest
asystole
arrest not due to drowning or electrocution
no sustained ROSC
no bystander CPR
Bottom line: Pediatric termination of resuscitation in the out of hospital setting can be appropriate under the right set of conditions.
Shetty P, Ren Y, Dillon D, et al. Derivation of a clinical decision rule for termination of resuscitation in non-traumatic pediatric out-of-hospital cardiac arrest. Resuscitation. Published online September 18, 2024. doi:10.1016/j.resuscitation.2024.110400
Category: Ultrasound
Keywords: POCUS; MSK; fracture (PubMed Search)
Posted: 3/17/2025 by Alexis Salerno Rubeling, MD
(Updated: 5/3/2026)
Click here to contact Alexis Salerno Rubeling, MD
On ultrasound, lipohemarthrosis—the presence of blood and fat in the joint cavity—is a key clinical indicator of an intra-articular fracture.
Lipohemarthrosis appears as three distinct layers near the joint line.
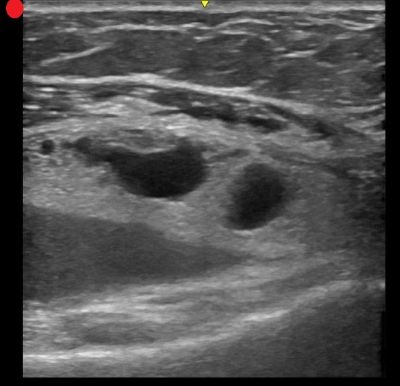
Salerno A. Lipohemarthrosis. Floating fat in an intra-articular fracture. Visual Journal of Emergency Medicine. 2022, 26:101236.
Category: Trauma
Keywords: kidney trauma, grading, (PubMed Search)
Posted: 3/16/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
Unless a patient is unstable, renal injuries are managed non-operatively or endovascularly. Here is the
2025 Kidney Injury Grading Scale from AAST.
AAST AIS
Grade Severity Imaging Criteria
I 2 –Subcapsular hematoma <3.5 cm without active bleeding
– Parenchymal contusion without laceration
II 2 – Parenchymal laceration length <2.5 cm
– HRD <3.5 cm without active bleeding
III 3 – Parenchymal laceration length ?2.5 cm
– HRD ?3.5 cm without active bleeding
– Partial kidney infarction
– Vascular injuries without active bleeding
– Laceration extending into urinary collecting system and/or urinary extravasation
IV 4 – Active bleeding from kidney
– Pararenal extension of hematoma
– Complete/near-complete kidney infarction without active bleeding
– MFK without active bleeding
– Complete/near-complete ureteropelvic junction disruption
V 5 – Main renal artery or vein laceration or transection with active bleeding
– Complete/near-complete kidney infarction with active bleeding
– MFK with active bleeding
Keihani, Sorena MD, MSCI; Tominaga, Gail T. MD; Matta, Rano MD; Gross, Joel A. MD; Cribari, Chris
MD; Kaups, Krista L. MD, MSc; Crandall, Marie MD, MPH, FACS; Kozar, Rosemary A. MD; Werner,
Nicole L. MD, MS; Zarzaur, Ben L. MD; Coburn, Michael MD, FACS; Myers, Jeremy B. MD, FACS. Kidney
organ injury scaling: 2025 update. Journal of Trauma and Acute Care Surgery 98(3):p 448-451, March
2025. | DOI: 10.1097/TA.0000000000004509
Category: Administration
Keywords: Ramadan, fasting (PubMed Search)
Posted: 3/15/2025 by Hanna Hussein, MD
(Updated: 5/3/2026)
Click here to contact Hanna Hussein, MD
Ramadan is the holy month in the Islam faith, where observers will fast from sunrise to sunset. This includes food, water, some medications, smoking and sex. This can obviously have some impact on patients' health, especially when presenting to the ED. Here are some considerations to keep in mind:
As with everything, maintaining cultural awareness and compassion will help to
M Nadir Bhuiyan 1,?, Rayya A Saadiq 1, Michael R Mueller 1, Ahmed D Abdalrhim 1, Joshua Overgaard 1
PMCID: PMC11268016 PMID: 39050928
Category: Pediatrics
Keywords: pediatrics, fever, seizure (PubMed Search)
Posted: 1/9/2025 by Kathleen Stephanos, MD
(Updated: 3/14/2025)
Click here to contact Kathleen Stephanos, MD
Simple Febrile Seizures are a very common cause for presentation to the Emergency Department.
Up to 5% of children will have one in their lifetime, and a single febrile seizure increases risk of recurrence.
Definition:
While not part of the formal definition, the following details are critical to obtain on history, and high risk features that should not be missed on initial evaluation:
Evaluation and Management:
Consider a finger stick
Most patients can be discharged to home after a period of observation - most use a 2-4 hour minimum. More recent literature suggests considering a longer observation period in patients who have seizures at lower core body temperatures (<39°C) or those with a history of recurrent simple febrile seizures (2 simple febrile seizures within 24 hours with return to baseline in between)
Obtain a lumbar puncture in all patients with symptoms of meningitis
Consider a lumbar puncture, lab evaluation, and prolonged observation in patients who are under-vaccinated/unvaccinated/unknown vaccination status between 6 months and 12 months of age, or received antibiotics within the last 48 hours
Eilbert W, Chan C. Febrile seizures: A review. J Am Coll Emerg Physicians Open. 2022 Aug 23;3(4):e12769. doi: 10.1002/emp2.12769. PMID: 36016968; PMCID: PMC9396974.
Category: Pharmacology & Therapeutics
Keywords: tenecteplase, alteplase, stroke (PubMed Search)
Posted: 3/10/2025 by Ashley Martinelli
(Updated: 3/13/2025)
Click here to contact Ashley Martinelli
On March 3, 2025, the FDA approved tenecteplase to treat acute ischemic stroke. Historically, only alteplase was FDA-approved, but the stroke guidelines suggest tenecteplase as a reasonable alternative and many centers have made the change to use tenecteplase.
The EXTEND-IA TNK trial showed benefit of tenecteplase over alteplase in patients who were candidates for mechanical thrombectomy. The newer AcT trial found that tenecteplase was non-inferior to alteplase for patients eligible for thrombolysis, regardless of thrombectomy candidacy. There was no difference in safety outcomes, specifically ICH or angioedema in either trial.
Tenecteplase will soon be available in a new 25 mg vial with stroke-specific packaging (potentially as early as June 2025). Currently, there is only a 50 mg vial that is used for STEMI and PE which has higher maximum dosing compared to stroke.
The dosing is now recommended in weight-based groupings based on the supplemental appendix from the AcT trial. This is likely a change in practice for most centers that previously implemented tenecteplase for stroke before the FDA approval. Consult with your stroke and pharmacy team to discuss potential protocol changes at your institution.

Campbell BCV, et al. NEJM 2018;378:1573-1582.
Menon BK, et al. Lancet 2022;400:161-69.
TNKase [package insert]. South San Francisco, CA. Genetech, Inc. 2025.
Genetech Press Release: https://www.gene.com/media/press-releases/15053/2025-03-03/fda-approves-genentechs-tnkase-in-acute-#:~:text=South%20San%20Francisco%2C%20CA%20%2D%2D,stroke%20(AIS)%20in%20adults.
Category: Gastrointestional
Keywords: Droperidol, abdominal pain (PubMed Search)
Posted: 3/13/2025 by Neeraja Murali, DO, MPH
(Updated: 5/3/2026)
Click here to contact Neeraja Murali, DO, MPH
Many of us probably use droperidol for pain relief in the ED. If you don't, two recent studies highlight it's use in multimodal pain control:
-In the DRUGS study (2023), droperidol reduced opiod use (46% vs 60%), lowered pain scores (median of 9 vs 5), and decreased the need for antiemetics (60% vs 73%). Before you ask - mean pain score wasn't reported!
-This study evaluated gastroparesis patients, with most common dose of droperidol being 1.25 mg IV
-the DREAMER study (2024) showed that pateitns receiving droperidol required fewer opiods (median 10 Morphine Milligram Equivalents vs 19.4 MME). No significant different in need for antiemetics
-This study evaluated abdominal pain patients, with 2.5 mg IV being the most common dose
Neither study found statistically significant differences in length of stay. Additionally, neither study reported major adverse effects or healthcare costs. Note that these were both single center trials as well.
With droperidol shortages ongoing, suggestions were made to directly compare droperidol to haloperidol, with hopefully more research coming soon!
-Stirrup N, Jones G, Arthur J, Lewis Z. Droperidol undermining gastroparesis symptoms (DRUGS) in the emergency department. Am J Emerg Med. 2024 Jan;75:42-45. doi: 10.1016/j.ajem.2023.10.030. Epub 2023 Oct 21. PMID: 37897920.
-Townsend BR, Malka ST, Di Paola SG, Nisly AE, Gilbert BW. DRopEridol for Abdominal pain in the emergency department for Morphine Equivalent Reduction. The DREAMER study. Am J Emerg Med. 2025 Jan 4;90:31-34. doi: 10.1016/j.ajem.2024.12.082. Epub ahead of print. PMID: 39798184.
Category: Obstetrics & Gynecology
Posted: 2/25/2025 by Jennifer Wang, MD
(Updated: 3/10/2025)
Click here to contact Jennifer Wang, MD
So you have a patient who is pregnant and has abdominal pain. You, as the astute provider you are, decide to do an ultrasound to rule out an ectopic, and low and behold! You see a gestational sac and a yolk sac within the uterus! You show your patient, you both breathe a sigh of relief, and you discharge them…
But they return two weeks later, now hypotensive, excruciating pain, and extremely pale. On an emergent bedside ultrasound, you see copious amounts of free fluid, and OBGYN tells you, after they rush your patient to the OR, that it was an ectopic - but how? The pregnancy was in the uterus!
Welcome everyone to the world of interstitial and angular pregnancies, pregnancies that are much closer to the endometrium than normal ectopic pregnancies and therefore have a much higher chance of progressing further before they rupture, meaning that when they do, they are devastating!
To evaluate for these ectopics, make sure that you get a mantle distance on every pregnancy ultrasound you do looking for an ectopic. Mantle distance is measured from the end of the gestational sac to the outer edge of the thinnest side of endometrium. If your value is >0.8cm, you should be okay. If it's less than <0.5cm, you most likely have an ectopic. Between 0.5cm and 0.8cm, consult OB urgently or have extremely close follow up for your patient.

Doane B, Perera P. Emergency ultrasound identification of a cornual ectopic pregnancy. West J Emerg Med. 2012;13(4):315. doi:10.5811/westjem.2011.10.6912
https://radiopaedia.org/articles/interstitial-ectopic-pregnancy?lang=us
Category: Trauma
Keywords: Sarcopenia, trauma, ct scan (PubMed Search)
Posted: 3/9/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
Having a readily measurable variable to identify frailty on admission for critically injured patients would help prognosticate morbidity, mortality, and discharge destination. Sarcopenia has been used to prognosticate length of stay, discharge destination, and physical function recovery in oncology and general surgery patients. Sarcopenia is defined as “age-related progressive loss of muscle mass and strength. The main symptom of the condition is muscle weakness. Sarcopenia is a type of muscle atrophy primarily caused by the natural aging process. Scientists believe being physically inactive and eating an unhealthy diet can contribute to the disease.” 1. This study looked at admission CT scan psoas muscle sarcopenia in 197 critically injured patients. The authors concluded:
“For trauma critical care patients, sarcopenia on admission CT was associated with dependent discharge destination and therefore is unfavourable. Defining sarcopenia early in a trauma patient’s critical care admission may help to identify those at risk of poor outcomes.” 2
1. Sarcopenia (Muscle Loss): Symptoms & Causes
2. Badminton R, Christie R, Brohi K, Cole E. Pre-injury sarcopenia and the association with discharge destination in critical care trauma patients. Trauma. 2025;27(1):57-64. doi:10.1177/14604086231214878
Category: Orthopedics
Posted: 3/8/2025 by Brian Corwell, MD
(Updated: 5/3/2026)
Click here to contact Brian Corwell, MD
Lidocaine transdermal patches
Frequently used for lower back pain.
A single 5% patch contains 700mg of lidocaine.
There is low systemic absorption.
Data supporting efficacy for lower back pain are limited.
Best benefit in other neuropathic conditions such as post herpetic neuralgia.
Topical capsicum
Underused, safe, non-sedating.
Potential treatment option for acute and subacute back pain (<3 months duration).
Can be OTC or via prescription.
Available in cream, lotion and patches.
Best used 3-4 times per day for maximal effectiveness.
Grade A recommendation from North American Spine Society.
Category: Trauma
Keywords: Male. Female, outcome, trauma (PubMed Search)
Posted: 3/6/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
The Pan-Asia Trauma Outcomes Study database was reviewed for differences in in-hospital mortality and functional capacity at discharge between male and female trauma patients. There were 76,000 trauma patients from 12 Asian countries in this study. The authors concluded: “This study indicates no difference in the general trauma outcomes in the Asia Pacific between females and males. Although younger females with less severe injuries had better functional outcomes, this advantage disappeared in severe injuries and those over 50 years.” There were several differences in mechanism of injury and age of presentation. “With females more frequently represented in the ??50 age group (60.13%) compared to males (44.87%) (p?<?0.001). Trauma type also varied between sexes; 95.51% of females experienced blunt trauma compared to 93.65% of males (p?<?0.001). Anatomically, males predominantly sustained injuries to the head, face, thorax, abdomen, and upper extremities, whereas females more frequently suffered injuries to the lower extremities and spine (p?<?0.001).” This is similar toEuropean and North American data
Bin Kunji Mohamad, M., Jamaluddin, S.F., Ahmad, N. et al. Trauma outcomes differences in females: a prospective analysis of 76 000 trauma patients in the Asia-Pacific region and the contributing factors. Scand J Trauma Resusc Emerg Med 33, 34 (2025). https://doi.org/10.1186/s13049-025-01342-1
Category: Trauma
Keywords: EMS, AlS, trauma, Bls, outcome (PubMed Search)
Posted: 3/5/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
Large retrospective propensity matching study looking at mortality in trauma patients based on ALS vs. BLS transport crew found lower mortality in those attended by ALS crews. The matching was “based on patient age, sex, year, ICD-10-CM based injury severity score, mechanism of injury, AIS based body region of injury, EMS characteristics including time with patient and prehospital interventions performed, prehospital vital signs, and trauma center designation.”
This is different than other studies which showed limited difference. other studies have shown improved survival with police “scooping and running” with penetrating trauma patients.
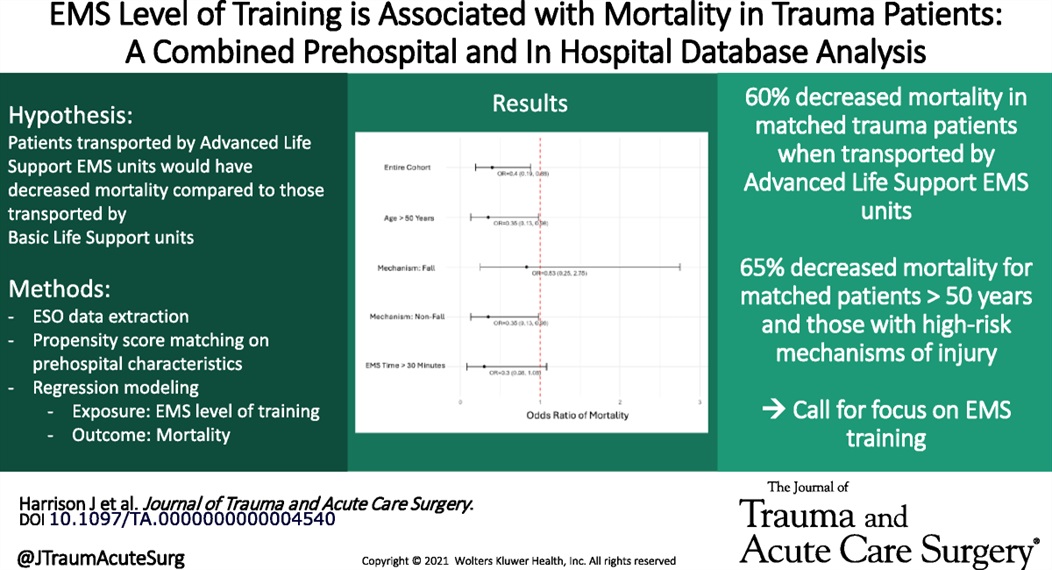
Harrison, Julia MD; Bhardwaj, Akshay MS; Houck, Olivia MPH; Sather, Kristiana MD; Sekiya, Ayako MPH; Knack, Sarah MD; Saarunya Clarke, Geetha PhD; Puskarich, Michael A. MD, MSCR; Tignanelli, Chris MD, MSc; Rogers, Lisa MPH; Marmor, Schelomo PhD; Beilman, Greg MD. Emergency medical services level of training is associated with mortality in trauma patients: A combined prehospital and in hospital database analysis. Journal of Trauma and Acute Care Surgery 98(3):p 402-409, March 2025. | DOI: 10.1097/TA.0000000000004540
Category: Critical Care
Keywords: Mechanical Ventilation, Brain Injury, ICH, Stroke, Hypercapnea, Hypoxia, Hyperoxia (PubMed Search)
Posted: 3/4/2025 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Intubation and mechanical ventilation of brain injured patients, which is extremely common in the Emergency Department, can be very challenging and subject to significant practice variation. It is often said that brain injured patients “can't take a joke”, meaning that they are less tolerant to hemodynamic and metabolic perturbations, and these perturbations tend to be associated with very large swings in their clinical outcomes. For example, hypo/hyperglycemia, hypo/hypernatremia, hypo/hypertension, hypo/hyperoxia, hypo/hypercapnea, etc are all extremely important to avoid. This is probably the one patient population where “euboxia” (the notion that we obsess too much about making all the numbers pretty in the EMR) is probably not as applicable. As such, there is at least good physiologic rationale, and now increasing empirical evidence, that ventilating these patients very thoughtfully is extremely important and likely to have meaningful impact on patient-oriented outcomes (mortality, neurologic outcome, etc).
The VENTIBRAIN study was a prospective observation trial of 2,095 intubated patients in 26 countries who had TBI, ICH (including SAH), or acute ischemic stroke. Interestingly, they found that patients with lower tidal volume (TV) per predicted body weight had higher mortality (although the majority of their TVs were well controlled and in a fairly tight range), which is contrary to conventional thinking in pulmonary pathologies like ARDS. They also found that higher driving pressure (DP) was associated with higher mortality, which agrees with data from other conditions. PEEP and FiO2 had U-shaped curves, but FiO2 in particular tended to favor lower FIO2, also similar to current thinking for ICU patients in general.
Take Home Points:
Learning Driving Pressure/PEEP Titration:
Category: Ultrasound
Keywords: POCUS, OB, retained products of conception (PubMed Search)
Posted: 3/3/2025 by Alexis Salerno Rubeling, MD
Click here to contact Alexis Salerno Rubeling, MD
A recent study evaluated the accuracy of POCUS in detecting retained products of conception (RPOC) in the emergency department.
In this study, a patient was considered positive for RPOC if they had heterogenous material in the endometrium measuring 10 mm or more. Color Doppler was not used for further evaluation, though it has been cited in obstetric literature as a helpful tool.
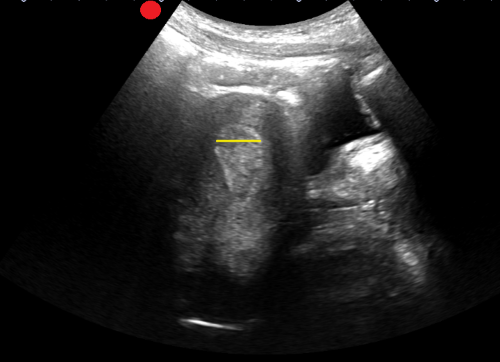
Among the 265 patients included, the prevalence of RPOC was 21.5%. POCUS had a sensitivity of 79.0 % and a specificity of 93.8 %.
The authors caution against the use of POCUS to diagnose RPOC in the setting of early pregnancy, as the endometrium can have a variable appearance, increasing the risk of a misdiagnosis. Of the 22 false positives identified, more than half were potentially viable pregnancies. Uterine fibroids can also lead to a heterogenous appearance of the uterus and can be another potential false positive.
Boivin Z, Barber D, Chimileski B, et al. Accuracy of point-of-care ultrasound in diagnosing retained products of conception. Am J Emerg Med. 2025;90:65-70. doi:10.1016/j.ajem.2025.01.032.
Category: Trauma
Keywords: Trauma, geriatric, fall, pain management, fracture, rib, pelvis (PubMed Search)
Posted: 3/1/2025 by Robert Flint, MD
(Updated: 3/2/2025)
Click here to contact Robert Flint, MD
Rib and pelvic fractures are common findings in geriatric trauma patients, even in low impact trauma such as falls from standing. Pain management is vital for improving morbidity and mortality. The IFEM White Paper suggests:
“Use multimodal pain management strategies, including regional anesthesia and non-opioid analgesics, to control pain without compromising recovery.
Monitor closely for complications such as pneumonia or hemodynamic instability, intervening promptly to mitigate risks.
Collaborate with physiotherapists to implement early mobility programs, reducing the risk of deconditioning and promoting recovery.”
A multidisciplinary team proficient in geriatric trauma care leads to better outcomes. This may require transfer to a trauma center.
Trauma in Older Adults: Evidence-Based Guidelines for Optimized Care White Paper
Trauma Special Interest Group and Geriatric Emergency Medicine Special Interest Group
https://assets.nationbuilder.com/ifem/pages/1768/attachments/original/1740084007/IFEM_Trauma_in_Older_Adults_Evidence-Based_Guidelines_for_Optimized_Care_White_Paper_December_2024.pdf?1740084007
Published: December 2024
Category: Trauma
Keywords: Trauma, geriatrics, frailty (PubMed Search)
Posted: 3/1/2025 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
This white paper reminds us that age is just a number; frailty is a better predictor of morbidity and mortality after trauma.
“Frailty, characterized by reduced physiological reserve and increased vulnerability to stressors, is a significant factor influencing recovery from trauma. Individuals with frailty may experience slower healing, higher rates of complications, and longer hospital stays. Tools such as the Clinical Frailty Scale (CFS) and the Trauma-Specific Frailty Index (TSFI) have been developed to assess frailty systematically, enabling clinicians to predict outcomes and guide treatment decisions.”
Trauma in Older Adults: Evidence-Based Guidelines for Optimized Care White Paper
Trauma Special Interest Group and Geriatric Emergency Medicine Special Interest Group
https://assets.nationbuilder.com/ifem/pages/1768/attachments/original/1740084007/IFEM_Trauma_in_Older_Adults_Evidence-Based_Guidelines_for_Optimized_Care_White_Paper_December_2024.pdf?1740084007
Published: December 2024
Category: Administration
Keywords: Nurse Practitioner, Physician Assistant, job satisfaction, burnout, longevity (PubMed Search)
Posted: 2/20/2025 by Steve Schenkel, MD, MPP
(Updated: 2/26/2025)
Click here to contact Steve Schenkel, MD, MPP
Nurse Practitioners and Physician Assistants practice alongside Physicians in Emergency Departments. In 2021, an estimated 17,679 NPs and PAs worked in EDs.
How long do NPs and PAs continue in Emergency Medicine practice?
An analysis of Medicare data reports that over the eight years of the study, the annual attrition rate averaged 13.8%, or almost 1 in 7 leaving Emergency Medicine practice every year. At the time of attrition, the median age for women was 40.2 years (IQR 33.8 to 49.9) and for men was 45.9 (IQR 37.8 to 56.3).
For additional breakdown and discussion of these numbers, see Gettel CJ, Chosh R, Rothenberg, et al. Workforce Attrition Among Emergency Medicine Non-Physician Practitioners. Ann Emerg Med, in press, https://www.annemergmed.com/article/S0196-0644(24)01294-0/fulltext.
Category: Critical Care
Keywords: Critically Ill, Intubated, Mechanical Ventilation, Ventilator-Associated Pneumonia (PubMed Search)
Posted: 2/25/2025 by Mike Winters, MBA, MD
(Updated: 5/3/2026)
Click here to contact Mike Winters, MBA, MD
Non-Pharmacologic Measures to Prevent VAP
Krone M, Seeber C, Nydahl P. What's New in Intensive Care: Preventing Ventilator-Associated Pneumonia Non-Pharmacologically. Intensive Care Med. 2024; 50:2185-2187.
