Category: Trauma
Keywords: Reverse shock index, Peds trauma, prediction (PubMed Search)
Posted: 11/18/2023 by Robert Flint, MD
Click here to contact Robert Flint, MD
This small study suggests using reverse shock index times the Glasgow Comma Scake score may give a prognostication on pediatric trauma severity and resource utilization.
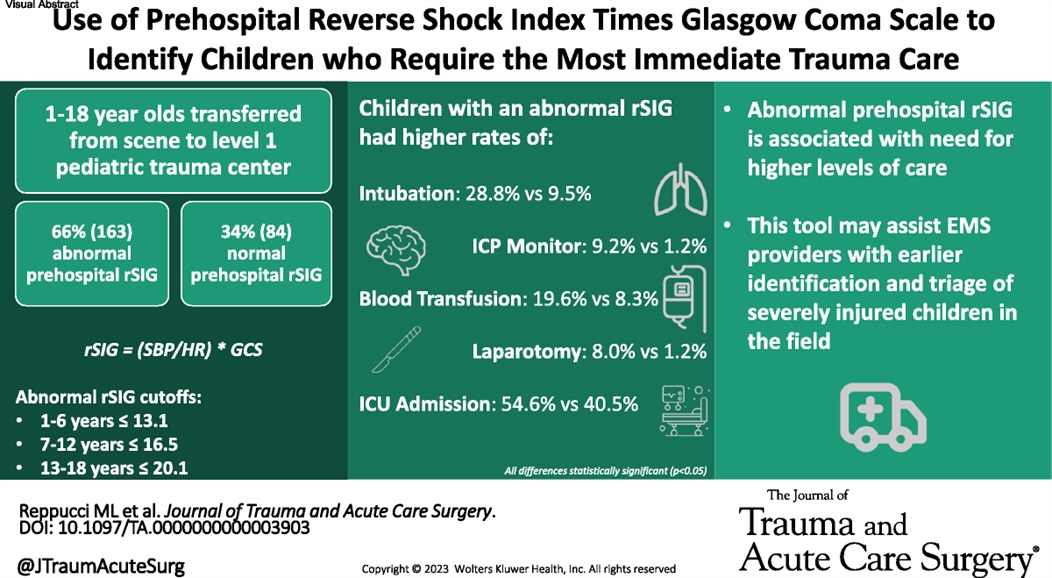
Reppucci, Marina L. MD; et al.
Journal of Trauma and Acute Care Surgery 95(3):p 347-353, September 2023. | DOI:
Category: Pediatrics
Keywords: pediatric trauma, transport, time to destination (PubMed Search)
Posted: 11/17/2023 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
Hosseinpour H. Interfacility Transfer of Pediatric Trauma to Higher Levels of Care: The Effect of Transfer Time and Level of Receiving Trauma Care. Journal of Trauma and Acute Care Surgery. Epub ahead of print.
Category: EMS
Keywords: mental health, excited delirium, agitation, sedation, ketamine (PubMed Search)
Posted: 11/15/2023 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
Bourke et al. Acute Severe Behavioral Disturbance Requiring Parenteral Sedation in Pediatric Mental Health Presentations to Emergency Medical Services: A Retrospective Chart Review. Annals of Emergency Medicine. 2023; 1-13. epub ahead of print.
Category: Trauma
Keywords: Brain injury, ketamine ICP (PubMed Search)
Posted: 11/12/2023 by Robert Flint, MD
Click here to contact Robert Flint, MD
This pediatric ICU study measured ICP during and after ketamine infusion. There was no increase in ICP associated with the ketamine infusion. This small study adds to the data that ketamine is safe in pediatric brain injured patients.
Laws, Jennifer C. MD1; Vance, E. Haley DNP2; Betters, Kristina A. MD1; Anderson, Jessica J. PharmD3; Fleishman, Sydney BA4; Bonfield, Christopher M. MD2; Wellons, John C. III MD, MSPH2,5; Xu, Meng MS6; Slaughter, James C. DrPH6; Giuse, Dario A. Dr.Ing7; Patel, Neal MD, MPH5,7; Jordan, Lori C. MD, PhD8; Wolf, Michael S. MD1,2
Category: Orthopedics
Posted: 11/11/2023 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
https://prod-images-static.radiopaedia.org/images/626179/d58f35a8aa4a0a6750a6adce4087a4_gallery.jpg
"I was kicked in the inside of my knee while it was straight (extended). Look at the x-ray and tell me if its bad"
The arcuate sign
Avulsion fracture of the styloid of the proximal fibula. The fragment is usually small (less than 1 cm) and displaced superiorly and medially. This fracture pattern is pathognomonic for posterolateral corner (PLC) injury.
Treatment in ED is knee immobilization in full extension. Refer to orthopedics for PCL reconstruction.
Category: Critical Care
Keywords: Pneumonia, Corticosteroids, Steroids, Respiratory Failure, Infection (PubMed Search)
Posted: 11/9/2023 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
For the folks who have been in practice for a while, you may be aware of the roller-coaster evidence base looking at steroids for pneumonia. Once thought to be beneficial and clearly indicated, of late steroids for pneumonia have fallen out of favor. Hamad et al have published an excellent (and brief) review in Clinical Infectious Diseases which suggests the pendulum might be swinging back in favor of giving steroids to patients with pneumonia. It's a ~5 minute read, so I recommend glancing through it yourself, but below are my two cents (solely my opinion) on where we are with steroids for pneumonia.
Take Home Points (OPINION ALERT):
1) When you have a condition present that you consider an indication for steroids (e.g. severe COVID-19 for sure; septic shock, s. pneumo infection, and ARDS depending on how you feel about the existing literature) --> strongly consider giving steroids unless there's a contraindication
2) When you have an undifferentiated patient who MAY have one of these conditions (e.g. pneumonia with COVID pending, patient potentially in ARDS or high risk of going into ARDS, etc) who is very sick --> it is reasonable to give steroids (if no contraindication) or not give steroids. My tendency is to lean towards giving steroids in these cases, but do be aware that society guidelines recommend against steroids here (although debatable if they just haven't caught up to more recent literature)
3) When you have an undifferentiated patient who may have one of these conditions, but is NOT very sick --> I do not think there is significant enough evidence to support empiric steroids
4) Factors that might push you one way or another:
Category: Gastrointestional
Keywords: NG Tube (PubMed Search)
Posted: 11/9/2023 by Neeraja Murali, DO, MPH
Click here to contact Neeraja Murali, DO, MPH
Think before placing a nasogastric tube!
Multiple articles which discussed complications of NGT placement were included in this integrative review, with the majority (n=67) publishing results in English. The authors categorized adverse events into two broad categories:
1) Mechanical adverse events - including respiratory, esophageal, and pharyngeal complications, obstructed tube, intestinal and intracranial (!) perforation, and tube withdrawal
-The largest cohort (n=44) was respiratory, with displacement or placement of tube to the respiratory tract
2) Others - pressure injury and misconnection
-One study showed pressure related injury in 25%, and 5 articles discussed complications of misconnection (including extravasation of gastric fluids and inadvertent connection to central venous catheters)
16 of the 69 studies reported death as a consequence of improper placement.
One big takeaway: there is no universally accepted standard for verificaiton of tube placement. Xray is considered to be *most* accurate. Tubes should also be checked periodically and depth should be marked. Evidence-based guidelines need to be developed to improve patient safety, outcomes, and quality of care.
Motta APG, Rigobello MCG, Silveira RCCP, Gimenes FRE. Nasogastric/nasoenteric tube-related adverse events: an integrative review. Rev Lat Am Enfermagem. 2021 Jan 8;29:e3400. doi: 10.1590/1518-8345.3355.3400. PMID: 33439952; PMCID: PMC7798396.
Category: Trauma
Keywords: ECMO, Trauma, Survivial (PubMed Search)
Posted: 10/14/2023 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
This systematic review and analysis found in 1822 trauma patients treated with ECMO:
-Overall 66% survival to discharge
-VV ECMO was significantly superior to VA ECMO
-Mean age was 35 years. Typical of ECMO use in trauma is younger healthier patients are chosen to receive ECMO
“ECMO is not a routine life-saving intervention following trauma, but rather a salvage therapy that effectively replaces conventional treatment for young, healthy patients when conventional methods fail. Its complexity requires a multidisciplinary healthcare team and sufficient resources for optimal implementation.”
Zhang et al. European Journal of Medical Research (2023) 28:412 https://doi.org/10.1186/s40001-023-01390-2
Category: Quality Assurance/Quality Improvement
Keywords: Medication Errors, Pharmacy (PubMed Search)
Posted: 11/4/2023 by Brent King, MD
(Updated: 5/3/2026)
Click here to contact Brent King, MD
Spanish investigators conducted a 6-month, prospective, observational study to determine the impact of emergency department pharmacists on medication errors. They specifically focused on so called "High Alert" medications and on errors that, if undetected prior to administration, were likely to have serious deleterious consequences.
Over the course of the study, the pharmacists reviewed the medication records and histories of nearly 3000 patients. The pharmacists intervened in the care of 557 patients. Errors were most often detected during the process of medication reconcilliation. Over half of the potential errors were considered "severe" and the majority of pharmacist interventions were deemed important to the patient's care. Many of the medication errors detected involved "High Alert" medications.
The Bottom Line: Pharmacists are integral members of a high-functioning emergency department team. Their specialized knowledge contributes to a safe and effective care environment.
Perez-Moreno MA, Rodriguez-Camacho JM, Calderon-Hernandez B, et al. Clinical relevance of pharmacist intervention in an emergency department. Emerg Med J. 2017;34:495-501. doi:10.1136/emermed-2015-204726.
Category: EMS
Keywords: Stroke, EMS, medical record linkage, prehospital (PubMed Search)
Posted: 11/3/2023 by Ben Lawner, MS, DO
Click here to contact Ben Lawner, MS, DO
BACKGROUND: Prehospital (EMS) clinicians are positioned on the front lines of health care. With respect to stroke identification and treatment, early recognition is essential to positive outcomes. Considerable variability exists within EMS documentation. Despite considerable variability in documentation, the establishment and tracking of core stroke metrics serves as a benchmark to gauge performance and outline strategies for improvement.
METHODS: Authors conducted a retrospective, observational analysis of EMS encounters (2018-2019) which ultimately received a diagnosis of an "acute cerebrovascular event." Hospital based diagnoses included: hemorrhagic stroke, ischemic stroke, or transient ischemic attack. The data set was comprised of a statewide EMS documentation and a state wide acute stroke registry. Authors examined compliance with six core performance metrics which included measurement of blood glucose, documentation of last known well time, and on-scene time < 15 mins for patients with suspected stroke. During the 18 month study, almost 6000 encounters met criteria for inclusion.
RESULTS: EMS documentation remains a significant source of variability. EMS crews were largely compliant with blood glucose measurement. However, last known well time had the lowest (24%) documentation rate. Patients diagnosed with subarachnoid hemorrhage had the lowest rate of compliance with metrics.
BOTTOM LINE: Accurate prehospital stroke diagnosis remains a challenge. Consistent data collection and benchmarking remains an important first step in the evaluation of performance. Higher NIHSS scores and ischemic strokes are linked to higher rates of metric compliance.
Oostema JA, Nickles A, Luo Z, Reeves MJ. Emergency Medical Services Stroke Care Performance Variability in Michigan: Analysis of a Statewide Linked Stroke Registry. J Am Heart Assoc. 2023 Jan 3;12(1):e026834. doi: 10.1161/JAHA.122.026834. Epub 2022 Dec 20. PMID: 36537345; PMCID: PMC9973590.
Category: Pediatrics
Keywords: Neonate, Newborn, resuscitation, NRP (PubMed Search)
Posted: 11/3/2023 by Kelsey Johnson, DO
(Updated: 5/3/2026)
Click here to contact Kelsey Johnson, DO
Term? Tone? Tantrum?
Immediately after delivery, your initial neonatal assessment should evaluate for:
- Appearance of full or late pre-term gestation (>34 weeks)
- Appropriate tone (flexed extremities, not floppy)
- Good cry and respiratory effort
Newborns meeting this criteria should not require resuscitation. They can be placed skin to skin on mother and allowed to breastfeed. Delayed cord clamping for 60 seconds is recommended, as data shows improved neurodevelopmental outcomes and iron stores in first year of life.
Neonates not meeting these criteria should be brought to the warmer for resuscitation, with the focus being on:
- Warm - via radiant warmer. Maintain temps 36.5 C – 37.5 C
- Dry - Neonates have thin skin and lose heat readily from evaporative loses
- Stim - tactile stimulation on the head, midline of the back and extremities to provoke a cry and encourage respiratory effort
Avoid routinely bulb-suctioning unless there is significant obstructing mucous, as this can increase vagal tone and result in bradycardia. If bulb suctioning is used, first suction the mouth before the nose.
Majority of resuscitations do not require additional support, however if heart rate is <100 or there is poor respiratory effort, the physician should initiate PPV.
PPV settings: PIP 20 PEEP 5 FiO2 21% Rate of 60 breaths per minute
Improvement in the neonate’s HR is the primary indicator of effective PPV!
If HR poorly responding (remains <100), ensure appropriate mask size, reposition, suction, and increase PIP (max 35) and FiO2.
If HR drops below 60, intubate with uncuffed ETT
- Prioritize adequate ventilation as this is the highest priority in neonatal resuscitation
- Initiate compressions at rate of 120/min.
- Epi dosing is 0.01-0.03 mg/kg q3-5 min
- ETT size estimation by gestational age:
25 weeks = 2.5, 30 weeks = 3.0, 35 weeks = 3.5, 40 weeks = 4.0
Category: Critical Care
Posted: 10/31/2023 by Mike Winters, MBA, MD
(Updated: 5/3/2026)
Click here to contact Mike Winters, MBA, MD
IV Fluid Resuscitation
Kaufman DA, et al. The ins and outs of IV fluids in hemodynamic resucitation. Crit Care Med. 2023;51:1397-1406.
Category: Trauma
Keywords: transfusion, mass hemorrhage protocol, cryoprecipitate (PubMed Search)
Posted: 10/14/2023 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
This large UK and US study looked at the addition of high dose cryoprecipitate to mass transfusion protocols and found: “Among patients with trauma and bleeding who required activation of a major hemorrhage protocol, the addition of early and empirical high-dose cryoprecipitate to standard care did not improve all cause 28-day mortality.”
Davenport R, Curry N, Fox EE, et al. Early and Empirical High-Dose Cryoprecipitate for Hemorrhage After Traumatic Injury: The CRYOSTAT-2 Randomized Clinical Trial. JAMA. Published online October 12, 2023. doi:10.1001/jama.2023.21019
Category: Orthopedics
Keywords: Race day event, medical tent, endurance athlete (PubMed Search)
Posted: 10/28/2023 by Brian Corwell, MD
(Updated: 5/3/2026)
Click here to contact Brian Corwell, MD
The objective of a recent study was to analyze the injury and illness characteristics in Iron Man distance triathletes. This information is important for emergency providers who may be asked to directly assist or help coordinate race day medical care.
Intro: The Iron Man distance triathlon is one of the most challenging ultra endurance competitions in the world. 80,000 Iron Man triathletes compete internationally each year to qualify for the Ironman world championship. The race totals 140.6 miles across three legs, beginning with a 2.4 mile swim, followed by a 112 mile cycle, and is completed with a 26.2 mile run.
Retrospective cross-sectional study of medical records from Iron Man distance championship races across a 30-year period (1989-2019). The study population (10,533) consisted of all triathletes treated at mobile medical units along the race route or who presented to the medical tent for evaluation during and immediately after the event.
Mean population age of 37 with a range of 18 to 87 years.
Results: Female athletes were found to present to the medical tent more than males (P < 0.001).
The total incidence of medical encounters by age was found to be higher in both younger athletes (18 to 34 years old) and older athletes (greater than 70 years old) versus middle-aged athletes (35-69 years old) (P < 0.001).
Professional athletes have similar overall medical encounters compared with other athletes.
The busiest hours of the medical tent were between approximately 9 and 14 hours after start time (afternoon and early evening) in which approximately 73% of athletes presented for evaluation and treatment.
Once inside the medical tent 71% of athletes were discharged within an hour and 87% were discharged within 1.5 hours. Athletes were dispatched to the hospital from the medical tent area at a rate of 17.1/1000 athletes (most athletes presenting to the medical tent finished the race and few required hospital transfer).
The most common medical complaints were dehydration and nausea followed by dizziness, exhaustion, muscle cramps, and vomiting.
Blood work was collected for 30% of athletes who entered the medical tent. Of these athletes, hyponatremia was the most prevalent diagnosis and most of whom were symptomatic with symptoms such as confusion, stupor, gait disturbance, muscle weakness, headache, dizziness, fatigue, nausea and vomiting.
Beyond basic medical care, intravenous fluids were the most common medical treatment.
Conclusion: Medical events were more frequent among female athletes as well as both younger and older age categories. Gastrointestinal and exertional related symptoms were the most common complaints in the medical tent. Besides basic medical care, IV infusions were the most common treatment. Most athletes presenting to the medical tent finished the race and only a small percentage were transferred to the hospital.
Nilssen PK, Connolly CP, Johnson KB, Cho SP, Cohoe BH, Miller TK, Laird RH, Sallis RE, Hiller WDB. Medical Encounters and Treatment Outcomes in Ironman-Distance Triathlon. Med Sci Sports Exerc. 2023 Nov 1;55(11):1968-1976.
Nilssen PK, Connolly CP, Johnson KB, Cho SP, Cohoe BH, Miller TK, Laird RH, Sallis RE, Hiller WDB. Medical Encounters and Treatment Outcomes in Ironman-Distance Triathlon. Med Sci Sports Exerc. 2023 Nov 1;55(11):1968-1976.
Category: Trauma
Keywords: trauma, pediatrics, resuscitation, MTP, MHP (PubMed Search)
Posted: 10/14/2023 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
This excellent review article discussing damage control resuscitation in traumatically injured children highlights several points including:
-”Damage-control resuscitation (DCR) consists of rapid control of bleeding, avoidance of hemodilution, acidosis, and hypothermia; early empiric balanced transfusions with red blood cells, plasma and platelets, or whole blood when available, and the use of intravenous or mechanical hemostatic adjuncts when indicated.”
-”he 30-day mortality in children with traumatic hemorrhagic shock is estimated to be 36% to 50% compared with the 25% reported mortality in similar adults. The early stages of hemorrhagic shock after injury in children can be more challenging to recognize because of their remarkable compensatory mechanisms. In children unlike adults, blood pressure alone is an insensitive indicator of hemorrhagic shock as hypotension is a late sign often not occurring until blood volume is reduced by >40%.”
-”Based on the current literature, the challenges health care providers must focus on are the early recognition of shock in the pediatric patient, moving the hemostatic resuscitation forward to the prehospital phase when feasible, improvement in times to first blood product, balanced resuscitation and efficiency of massive transfusion protocols (MTPs).”
Russell, Robert T. MD, MPH; Leeper, Christine M. MD; Spinella, Philip C. MD. Damage-control resuscitation in pediatric trauma: What you need to know. Journal of Trauma and Acute Care Surgery 95(4):p 472-480, October 2023. | DOI: 10.1097/TA.0000000000004081
Category: Pediatrics
Keywords: trauma arrest, ROSC, blunt, penetrating (PubMed Search)
Posted: 10/20/2023 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
Selesner L, Yorkgitis B, Martin M, et al. Emergency department thoracotomy in children: A Pediatric Trauma Society, Western Trauma Association, and Eastern Association for the Surgery of Trauma systematic review and practice management guideline. J Trauma Acute Care Surg. 2023;95(3):432-441. doi:10.1097/TA.
Category: EMS
Keywords: BVM, tidal volume, TV, ALS, BLS (PubMed Search)
Posted: 10/18/2023 by Jenny Guyther, MD
(Updated: 5/3/2026)
Click here to contact Jenny Guyther, MD
The typical bag valve mask ventilator (BVM) for adults has a reservoir volume between 1500-2000 mL depending on the manufacturer while the volume is between 500-1000 mL for a pediatric BVM. When trying to obtain the recommended tidal volume of 6-8 mL/kg (500-600 mL for the typical adult), one thought was that a pediatric BVM could be used with adult patients so as to avoid iatrogenic barotrauma. This has been studied on manakins using an oral pharyngeal airway, supraglottic airway and endotracheal tubes (ETT) and has been successful. This study attempted to obtain the same results in the back of a moving ambulance. Paramedics and EMTs, squeezing pediatric and adult BVMs with one hand, bagged adult manakins in the back of a moving ambulance (without lights and sirens). The average tidal volume was recorded using various types of airways (i-gel, King airway and ETT).
Volumes delivered with the pediatric BVM were significantly lower than the tidal volumes with adult BVMs across all airway types suggesting that in the moving ambulance, using pediatric BVMs on an adult patient would not be appropriate.
The I-Gel and King airway provided similar tidal volumes which were not statistically different than volume delivered through the ETT.
EMTs consistently delivered 50% less tidal volumes compared to paramedics. The authors suggested that perhaps the additional training and pathophysiology knowledge that paramedics have could also be important with a skill that is considered basic.
Sun et al. Are Pediatric Manual Resuscitators Only Fit for Pediatric Use? A Comparison of Ventilation Volumes in a Moving Ambulance. Prehospital Emergency Care 2023, 27:4, 501-505.
Category: Critical Care
Keywords: SOFA, admission unit, ICU, IMC, Ward, morality (PubMed Search)
Posted: 10/17/2023 by Quincy Tran, MD, PhD
(Updated: 5/3/2026)
Click here to contact Quincy Tran, MD, PhD
Settings: Retrospective study of a national inpatient database (Japan).
Participants:
Outcome measurement: Primary outcome was in-hospital mortality, after propensity score matching.
Study Results:
Discussion:
Conclusion:
Risk-stratifying patients according to SOFA score is a potential strategy for appropriate admission strategies.
1.Ohbe H, Sasabuchi Y, Doi K, Matsui H, Yasunaga H. Association Between Levels of Intensive Care and In-Hospital Mortality in Patients Hospitalized for Sepsis Stratified by Sequential Organ Failure Assessment Scores. Crit Care Med. 2023 Sep 1;51(9):1138-1147. doi: 10.1097/CCM.0000000000005886. Epub 2023 Apr 28. PMID: 37114933.
2.Corwin GS, Mills PD, Shanawani H, Hemphill RR. Root Cause Analysis of ICU Adverse Events in the Veterans Health Administration. Jt Comm J Qual Patient Saf. 2017 Nov;43(11):580-590. doi: 10.1016/j.jcjq.2017.04.009. Epub 2017 Jul 25. PMID: 29056178.
Category: Trauma
Keywords: REBOA, trauma, survival (PubMed Search)
Posted: 10/14/2023 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
This UK study randomized 90 trauma patients suspected of having major life threatening torso hemorrhage to receive standard resuscitative care vs. standard care plus resuscitative endovascular occlusion of the aorta (REBOA). Mortality was 54% in the REBOA group and 42% in the standard care group. This calls into question the routine use of REBOA in trauma resuscitations.
Jansen JO, Hudson J, Cochran C, et al. Emergency Department Resuscitative Endovascular Balloon Occlusion of the Aorta in Trauma Patients With Exsanguinating Hemorrhage: The UK-REBOA Randomized Clinical Trial. JAMA. Published online October 12, 2023. doi:10.1001/jama.2023.20850
Category: Pharmacology & Therapeutics
Keywords: epinephrine, anaphylaxis, allergy, digital ischemia, phentolamine, nitroglycerin ointment, terbutaline (PubMed Search)
Posted: 10/12/2023 by Alicia Pycraft
Click here to contact Alicia Pycraft
Background: It is estimated that nearly 6% of U.S. adults and children report having a food allergy.1,2 Epinephrine autoinjectors are used to provide life-saving pre-hospital treatment for patients experiencing anaphylaxis in the community, but can have serious consequences if administered incorrectly. Accidental finger-stick injuries with epinephrine auto-injector can result in significant pain and ischemia due to vasoconstriction and decreased blood flow to the digit. Treatments for digital epinephrine injection include supportive care, topical vasodilators, and injectable vasodilators.3
Supportive care3,4:
