Category: Pediatrics
Keywords: pediatric, code, resuscitation, medication error (PubMed Search)
Posted: 10/3/2015 by Christopher Lemon, MD
Click here to contact Christopher Lemon, MD
A group from Colorado identified the high-stress of pediatric resuscitation as a high-risk setting for possible medication error. As such, they performed a prospective, block-randomized, crossover study with two mixed teams of docs (ABEM certified) and nurses, managing 2 simulated peds arrest scenarios using either:
1) conventional “draw-up and push” drug administration methods [control] or
2) prefilled medication syringes labeled with color-coded volumes correlating to the weight-based Broselow Tape dosing [intervention].
The objective was to compare the time of preparation and administration of a medication, as well as to assess dosing errors. Participants were blinded to the purpose during recruitment but unblinded just prior to running the scenarios.
The scenarios included advanced airway management and hemodynamic life support efforts to care for an 8-year-old or 8-month-old manikin. The intervention group received a standard 3-minute tutorial on the use of prefilled color-coded syringes just prior to their scenario. After completing the first scenario, the groups switched, utilizing the other sim with the other method of medication administration. After a 4-16 week “wash out” period, the groups reconvened to reverse the medication administration technique across the same 2 scenarios.
Each Broselow tape color zone corresponds to a narrow range of weights. The authors opted to designate medication dosing errors >10% above or below the correct range as critical dosing errors.
The results? Median time to delivery of all conventionally administered medication doses was 47 seconds versus the prefilled color-coded administration system-- 19 seconds. The conventional administration system saw 17% of doses with critical errors versus none for the prefilled color-coded syringe group.
These prefilled color-coded syringes are not currently manufactured. Should they go into commercial production, the hope is that such syringes would be longer and more narrow than conventional syringes to effectively elongate each color-coded section (the delineations for red and purple on a standard syringe differ by as little as 1/8-3/32 of an inch if you want to make your own!-- see picture).
Color-Coded Prefilled Medication Syringes Decrease Time to Delivery and Dosing Error in Simulated Emergency Department Pediatric Resuscitations. Moreira, Maria E. et al. Annals of Emergency Medicine, Volume 66 , Issue 2 , 97 - 106.e3.
Category: Toxicology
Keywords: Odansetron, Zofran (PubMed Search)
Posted: 10/2/2015 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
Category: International EM
Keywords: international, American College of Emergency Physicians, emergency medicine (PubMed Search)
Posted: 9/30/2015 by Jon Mark Hirshon, MPH, MD, PhD
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
If you are interested in learning about the current status of emergency medicine in a specific country, it can be difficult to find up-to-date information. One excellent resource for country specific details is the American College of Emergency Physicians’ (ACEP) International Ambassador Program.
This program has Emergency Medicine Ambassadors (U.S. emergency physicians), Liaisons (in-country emergency physicians) and Representatives (U.S. emergency physicians in training) for many countries around the world. Additionally, there are country specific reports that give annually updated information about emergency medicine in each country.
Included on the website are links to send emails to the Ambassadors, Liaisons and Representatives in order to request more detailed information.
To learn more, see: http://www.acep.org/IntlAmbassador/
Category: Critical Care
Keywords: Aortic dissection, STEMI, cardiac tamponade, aortic insufficiency, echocardiography (PubMed Search)
Posted: 9/30/2015 by Daniel Haase, MD
Click here to contact Daniel Haase, MD
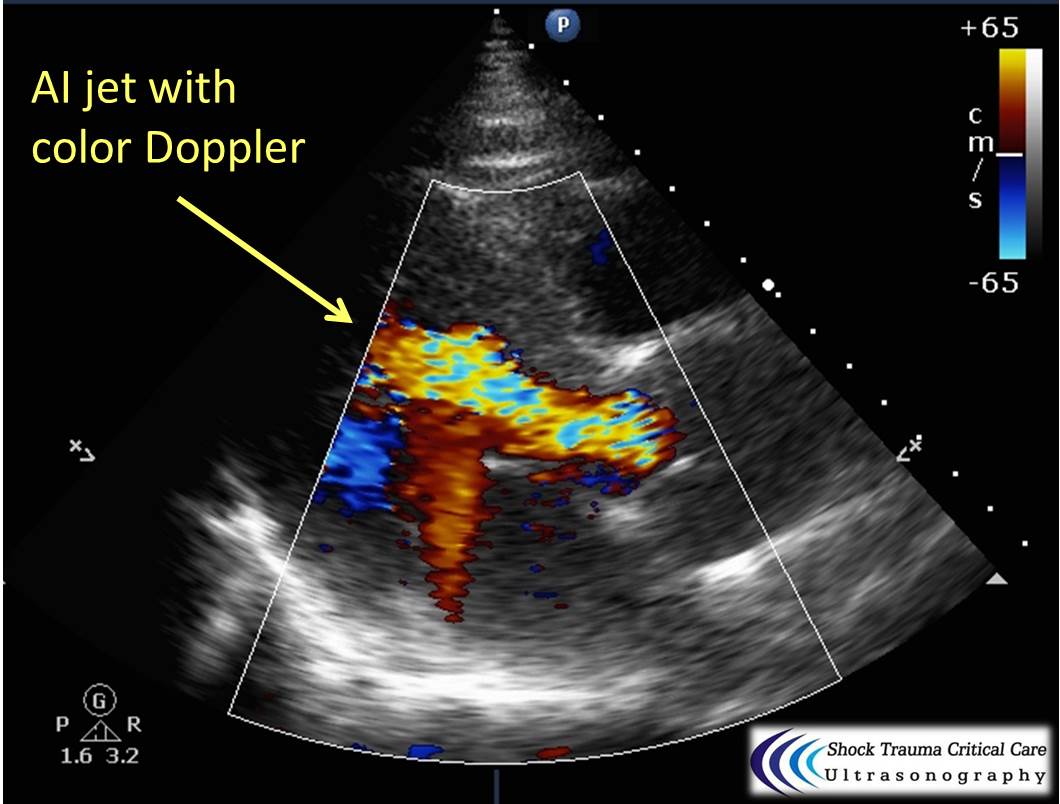
Classically, aortic dissection presents as tearing or ripping chest pain that radiates to the back in a HYPERtensive patient.
However, type A aortic dissections can quickly become HYPOtensive due to any the primary cardiac complications from retrograde dissection into:
Bedside echo can't rule out aortic dissection, but it can help rule in the diagnosis (figure 1) or complications (figure 2) at times.
Category: Visual Diagnosis
Posted: 9/28/2015 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
26 year-old male presents with a swollen 4th digit and pain during extension, what’s the diagnosis?
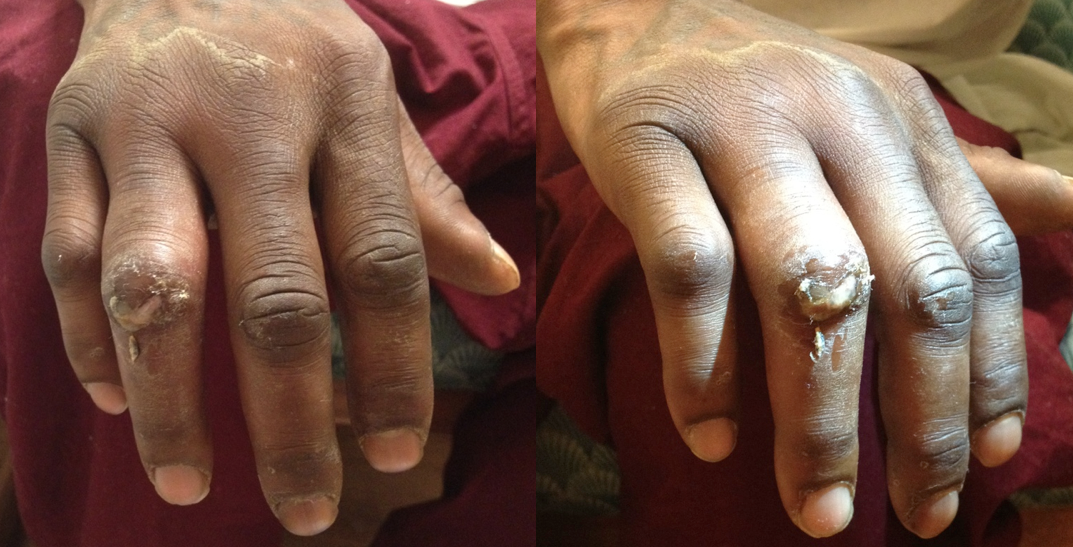
Answer: Infectious Flexor Tenosynovitis
Infectious Flexor Tenosynovitis
Follow me on Twitter (@criticalcarenow)
Category: Orthopedics
Keywords: Popliteal cyst, knee swelling (PubMed Search)
Posted: 9/26/2015 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Most common mass in popliteal fossa
Incidence 10 to 58%
Intra-articular pathology results in flow of synovial fluid from the joint into the bursa, forming a cyst
Association with concomitant intra-articular disorders 94%
Possible pathology - Meniscus, ligamentous, arthritis, other osteochondral defects
In children this is not a pathologic finding
Symptoms - Posterior knee bulging, posterior tightness/stiffness esp. with knee flexion
Ultrasound - 100% sensitive/specific
DDx: DVT
Tx: Refer for ultrasound guided aspiration, fenestration and steroid injection
http://www.caringmedical.com/wp-content/uploads/2013/11/Bakers-Cyst-treatment.jpg
Smith, Lesniak et al. 2015 Treatment of popliteal cysts with ultrasound-guided aspiration, fenestration and injection: long term follw-up
Category: Neurology
Keywords: SAH, cerebral venous thrombosis, head CT (PubMed Search)
Posted: 9/23/2015 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
A thunderclap headache is defined as a very severe headache that reaches its maximum intensity within 1 minute.
One of the most common causes (and the one associated with this buzzword on board questions!) is subarachnoid hemorrhage, but what else can cause a it?
- Reversible cerebral vasoconstriction syndrome (RCVS): suggested by recurrent thunderclap headaches (2-10) over 1 to 2 weeks. Normal CT and LP, with vasoconstriction on angiography. Can lead to SAH, ICH or ischemic stroke.
- Cervical artery dissection
- Cerebral venous sinus thrombosis
- Spontaneous intracranial hypotension: characterized by orthostatic HAs and auditory muffling.
- Intracerebral hemorrhage
- “Primary”: a diagnosis of exclusion
Bottom line? All patients with thunderclap HA should have a stat head CT with no contrast, then have SAH excluded with an LP, CTA or MRI/MRA. Just because you excluded SAH in a patient with thunderclap headache does not mean you’re done with the emergency workup.
TJ Schwedt. Thunderclap Headache. Continuum 2015; 21(4): 1058-71
Category: Critical Care
Posted: 9/22/2015 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
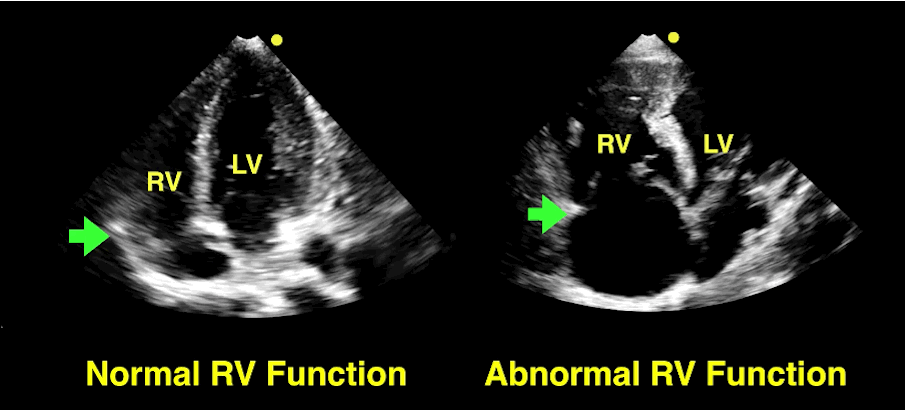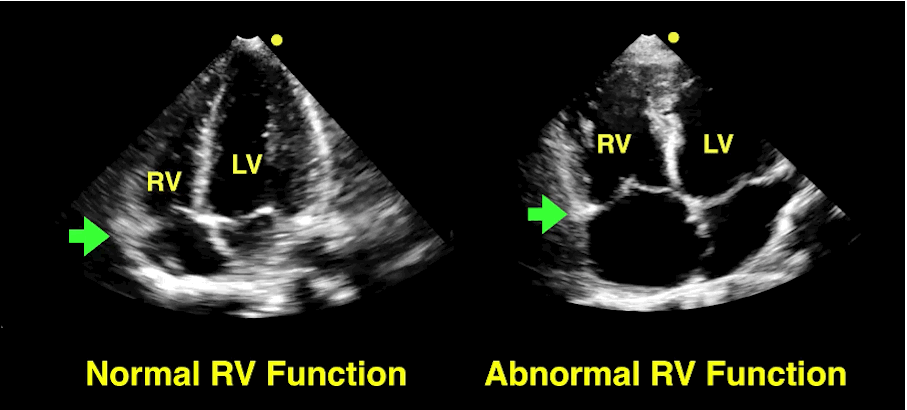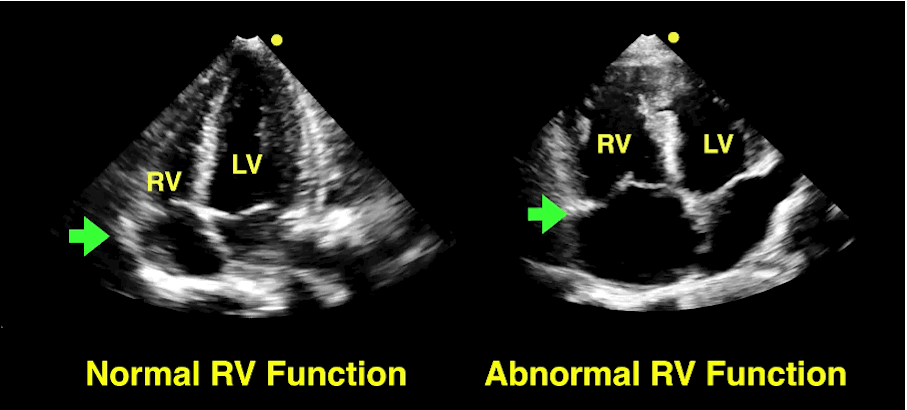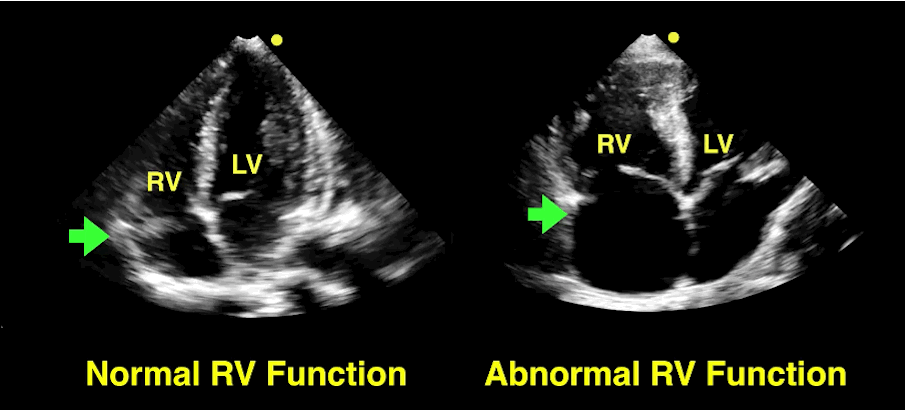
Follow me on Twitter (@criticalcarenow)
Category: Visual Diagnosis
Posted: 9/21/2015 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
30 year-old male with abdominal pain and diffuse tenderness on exam. Ultrasound is shown, what's the diagnosis?
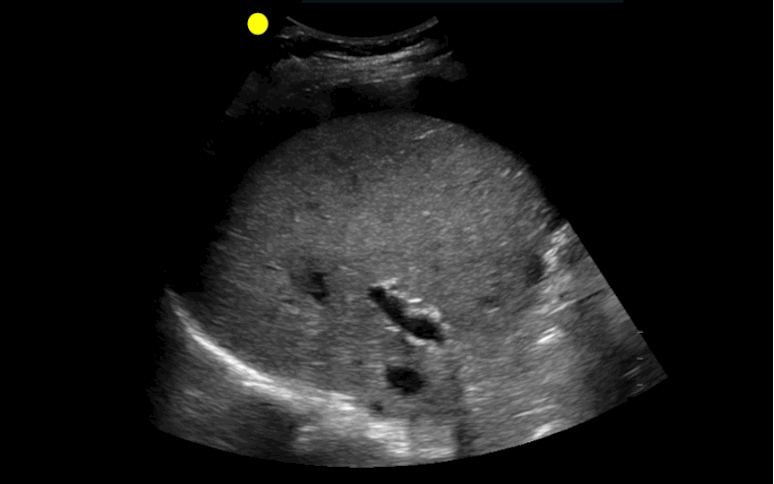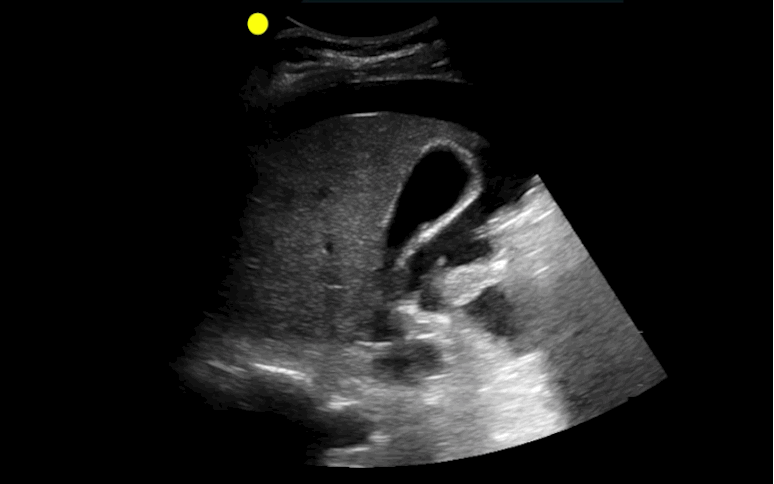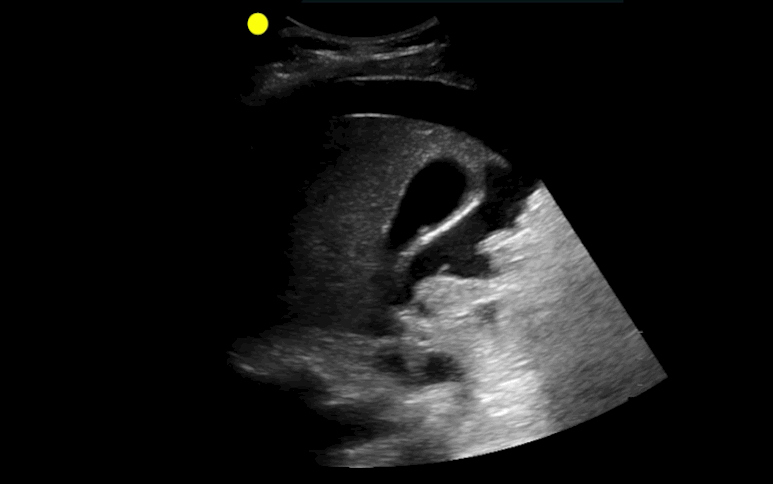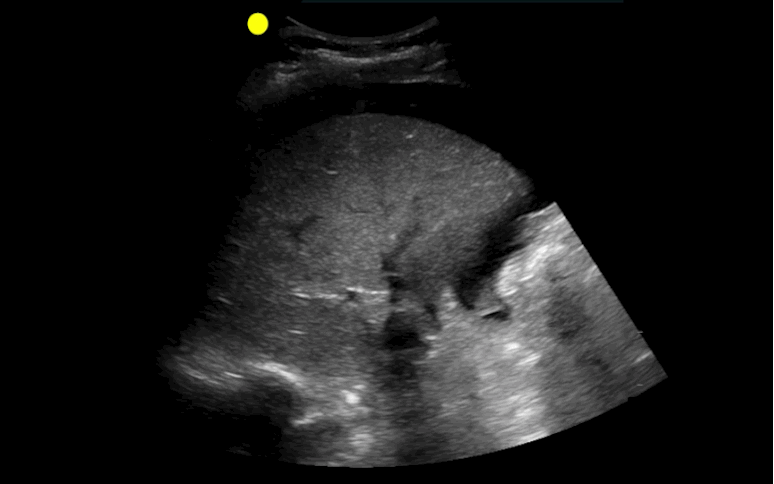
Free intra-abdominal fluid.
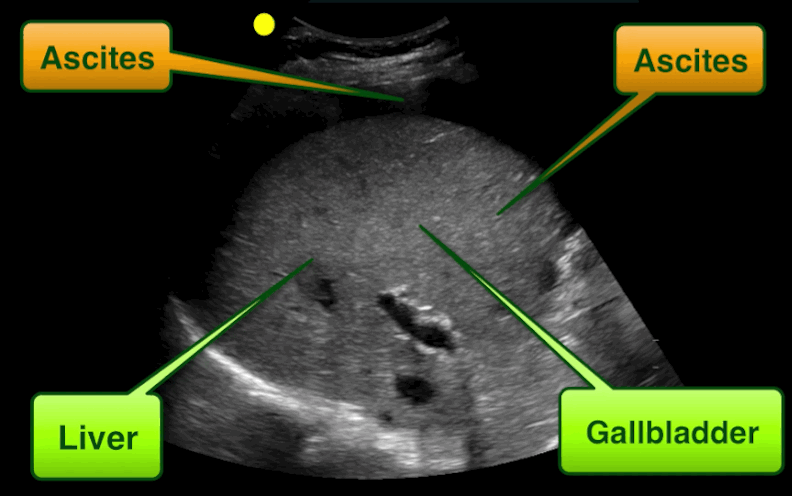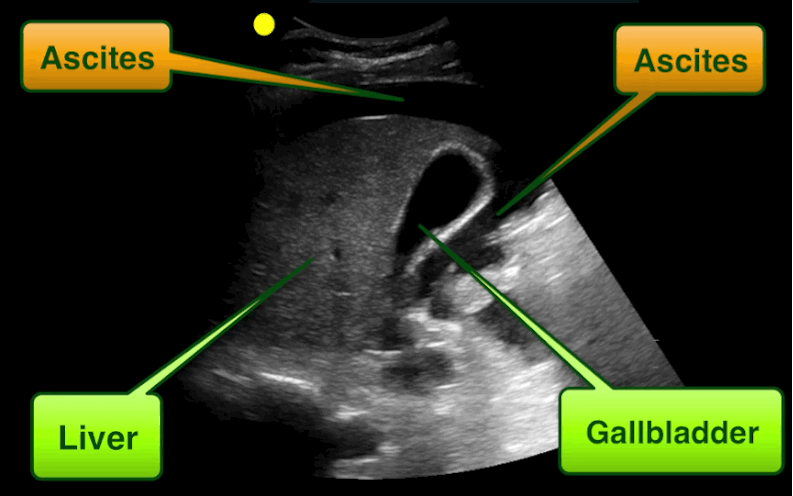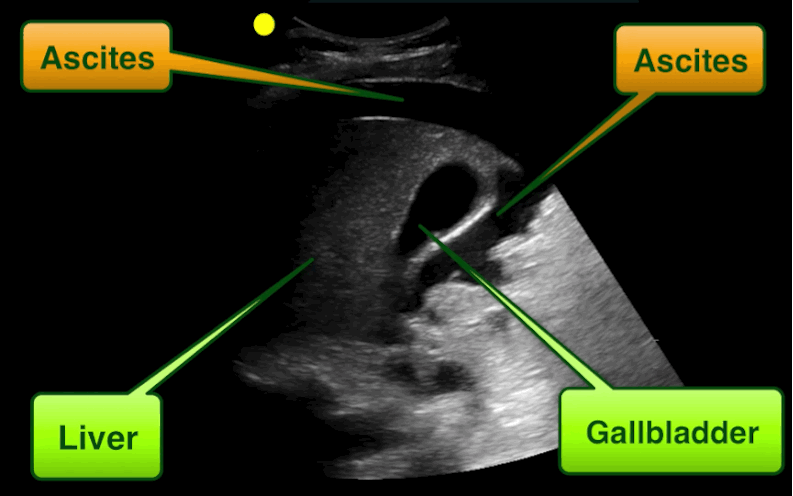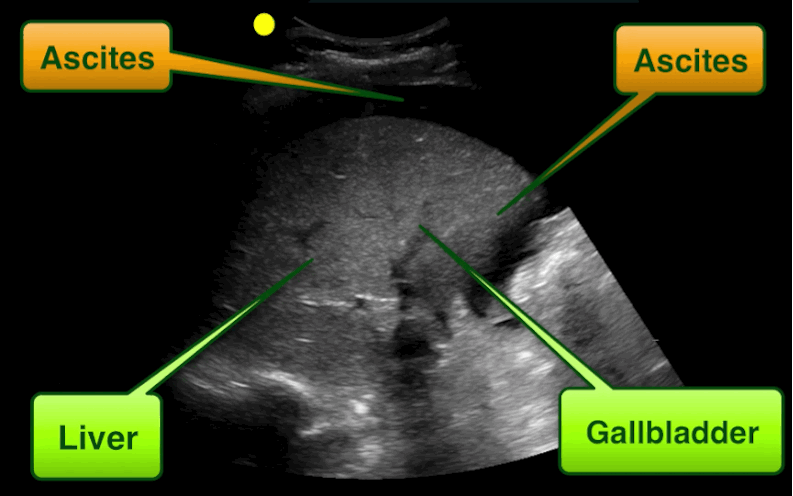
Follow me on Twitter (@criticalcarenow)
Category: Orthopedics
Keywords: shoulder, dislocation, GONAIS (PubMed Search)
Posted: 9/19/2015 by Michael Bond, MD
Click here to contact Michael Bond, MD
Shoulder Dislocation Reduction
Do you have a chronic dislocated that frequents your ED? Are you interested in teaching them a way to relocate their shoulder without looking like Mel Gibson from Lethal Weapon, https://youtu.be/Igrdi_lhhW4, then the newly described GONAIS method might be what you are looking for.
This technique has the patient grab the top of a chair with the hand on the affected side, and then slowly equating, effectively bringing the hand and arm above their head. Once in the full squat position the patient can step backwards which should reduce the shoulder. If not they can use the opposite hand to apply pressure to push the humerus backward and reduce the location.
The full article can be found at http://bit.ly/1iZ8a9z
Gonai S, Kamio Y, Matsuoka T, Harunari M, Saito Y, Takuma K. A new autoreduction method for anterior shoulder dislocation: the GONAIS method. Am J Emerg Med. 2015 Jun 14. pii: S0735-6757(15)00492-1. doi: 10.1016/j.ajem.2015.05.053. [Epub ahead of print]
Category: Pediatrics
Keywords: wrist, fracture, trauma (PubMed Search)
Posted: 9/18/2015 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Is there a set of criteria similar to the Ottawa Ankle or Knee Rule that can be applied to the wrist in children?
The Amsterdam Pediatric Wrist Rules are as follows:
-Swelling of distal radius
-Visible deformity
-Painful palpation of the distal radius
-Painful palpation at the anatomical snuff box
-Painful supination
A positive answer to any of these would indicate the need for an xray.
The study referenced attempted to validate these criteria. This criteria is inclusive of the distal radius in addition to the wrist. The sensitivity and specificity were 95.9% and 37.3%, respectively in children 3 years through 18 years. This model would have resulted in a 22% absolute reduction in xrays. In a validation study, 7/170 fractures (4.1%, 95% CI: 1.7- 8.3%) would have been missed using the decision model. The fractures that were missed were all in boys ages 10-15 and were all buckle fractures and one non displaced radial fracture.
Bottom line: This rule can serve as a guide for when to obtain an xray in the setting of trauma, but it is not perfect.
Slaar et al. A clinical decision rule for the use of plain radiography in children after acute wrist injury: development and external validation of the Amsterdam Pediatric Wrist Rules. Pediatr Radiol 2015; published online August 23, 2015.
Category: Toxicology
Keywords: flushed skin (PubMed Search)
Posted: 9/16/2015 by Hong Kim, MD
(Updated: 5/4/2026)
Click here to contact Hong Kim, MD
Monosodium glutamate
Metabisulfites (Na sulfite, Na/K bisfulfite, Na/K metabisulfite, etc.)
Tyramine reaction
Niacin
Trichloroethylene
Scrombroids
Hydroxocobalamin
Category: International EM
Keywords: anthrax, plague, tularemia, botulism, dengue, bioterror (PubMed Search)
Posted: 9/14/2015 by Jon Mark Hirshon, MPH, MD, PhD
(Updated: 9/16/2015)
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
Which infectious disease listed as Class A agents occur naturally, though sporadically within the U.S?
Small pox no longer occurs naturally and other viral hemorrhagic fevers occur in tropical settings.
http://www.cdc.gov/nczved/divisions/dfbmd/diseases/anthrax/technical.html
http://www.cdc.gov/plague/maps/
http://www.cdc.gov/tularemia/statistics/map.html
http://www.cdc.gov/nationalsurveillance/botulism-surveillance.html
http://www.cdc.gov/dengue/epidemiology/
http://emergency.cdc.gov/agent/vhf/
Category: Critical Care
Keywords: Simv, critical care, ventilator (PubMed Search)
Posted: 9/15/2015 by Feras Khan, MD
(Updated: 5/4/2026)
Click here to contact Feras Khan, MD
SIMV (Synchronized intermittent mandatory ventilation)
Category: Visual Diagnosis
Posted: 9/14/2015 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
35 year-old female presents to the Emergency Room with cough and chest tightness. She was discharged from the hospital yesterday for an asthma exacerbation that was secondary to pneumonia. What's the diagnosis?
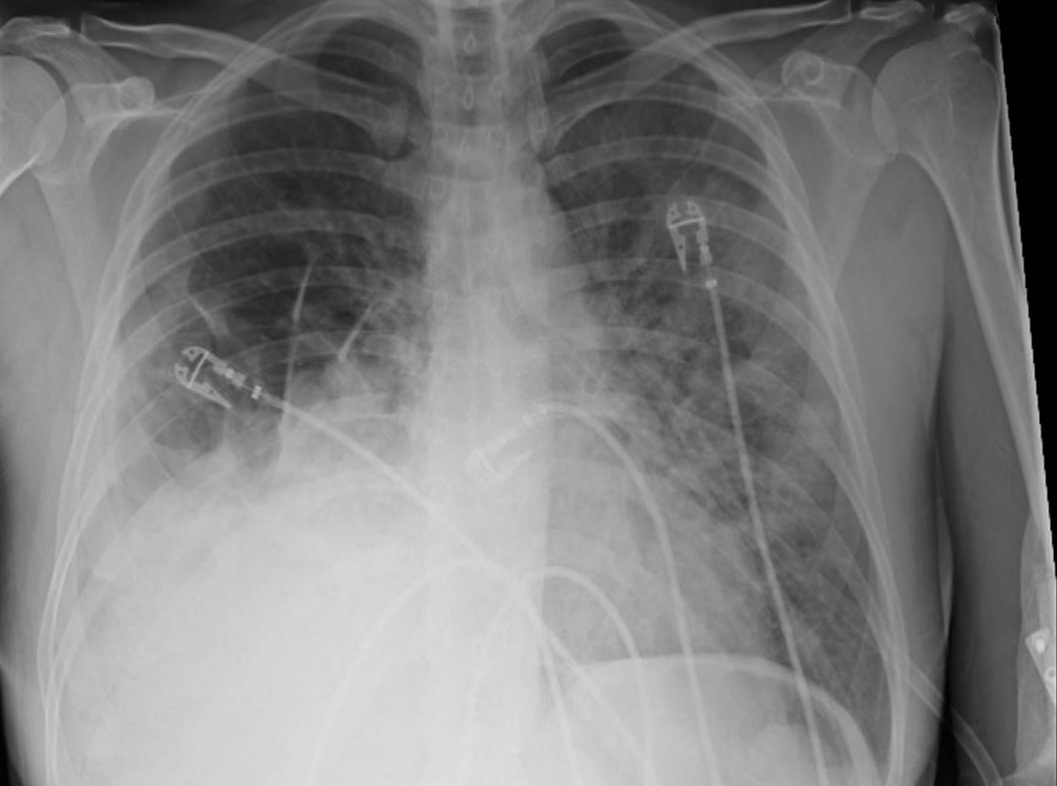
Diaphragmatic hernia
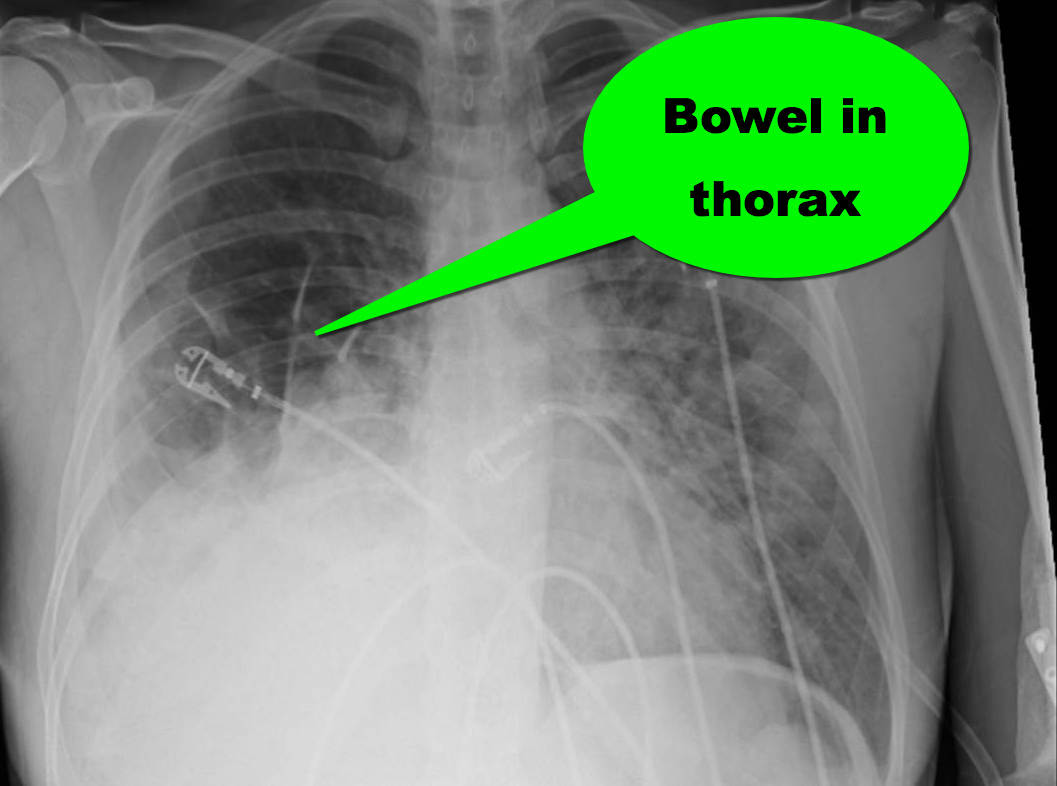
Follow me on Twitter (@criticalcarenow)
Category: Toxicology
Keywords: eye drops, pupil size, ophthalmic (PubMed Search)
Posted: 9/8/2015 by Bryan Hayes, PharmD
(Updated: 9/11/2015)
Click here to contact Bryan Hayes, PharmD
In the evaluation of ED patients, it may be important to understand the effect on pupil size from the ophthalmic medications they use. Here is a summary chart of common eye drops and their effect on pupil size.
Follow me on Twitter (@PharmERToxGuy)
Category: Neurology
Keywords: serotonin syndrome, SSRI, autonomic hyperactivity, hyperreflexia, clonus, Hunter Criteria (PubMed Search)
Posted: 9/9/2015 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Serotonin Syndrome - What is It?
** Stay tuned for part 2 on what causes serotonin syndrome **
Follow me on Twitter @EM_NCC
Category: Critical Care
Posted: 9/8/2015 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Hyperoxia in the Critically Ill
Helmerhorst HJF, et al. Association between arterial hyperoxia and outcomes in subsets of critical illness: A systematic review, meta-analysis, and meta-regression of cohort studies. Crit Care Med 2015; 43:1508-19.
Category: Visual Diagnosis
Posted: 9/6/2015 by Haney Mallemat, MD
(Updated: 9/7/2015)
Click here to contact Haney Mallemat, MD
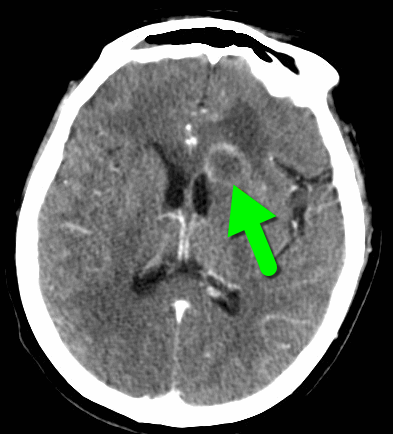
68 year-old man presents with a new-onset seizure. What's the diagnosis and what's in your differential diagnosis?
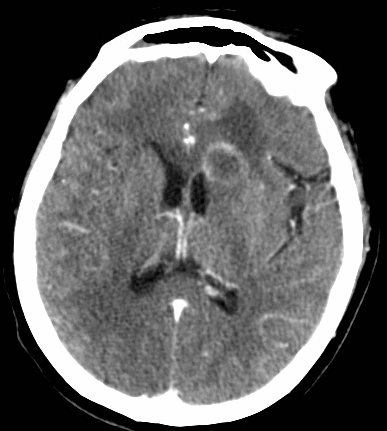
Ring-enhancing lesion
Differential diagnosis of a ring-enhancing lesion
| Neoplasm | Infectious | Neurologic |
| Primary brain tumor | Pyogenic Abscess | Multiple Sclerosis |
| Primary CNS lymphoma | Tuberculoma | Sarcoidosis |
| Metastatic disease | Syphilis | Vasculitis |
| Neurocysticercosis | Aneurysm | |
| Toxoplasmosis | Resolving hematoma | |
| Nocardiosis | Cerebral infarct | |
| Cyptococcocus | Post-op changes | |
| Aspergillosis |
Follow me on Twitter (@criticalcarenow)
Category: Pharmacology & Therapeutics
Keywords: ketamine, analgesia, morphine, pain (PubMed Search)
Posted: 8/30/2015 by Bryan Hayes, PharmD
(Updated: 9/5/2015)
Click here to contact Bryan Hayes, PharmD
A new prospective, randomized, double-blind trial compared subdissociative ketamine to morphine for acute pain in the ED.
What they did
What they found
Motov S, et al. Intravenous subdissociative-dose ketamine versus morphine for analgesia in the emergency department: a randomized controlled trial. Ann Emerg Med 2015;66:222-9. [PMID 25817884]
Follow me on Twitter (@PharmERToxGuy)
