Category: Pharmacology & Therapeutics
Keywords: clindamycin, MRSA, SSTI (PubMed Search)
Posted: 7/1/2014 by Bryan Hayes, PharmD
(Updated: 7/5/2014)
Click here to contact Bryan Hayes, PharmD
Clindamycin used to be a first-line agent for many SSTIs, particularly where MRSA was suspected. With growing resistance to staph species, the 2014 IDSA Guidelines recommend clindamycin as an option only in the following situations:
* Clindamycin may be used if clindamycin resistance is <10-15% at the institution.
Stevens DL, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014;59(2):e10-52. [PMID 24947530]
Follow me on Twitter (@PharmERToxGuy) or Google Plus (+bryanhayes13)
Category: International EM
Keywords: Geriatric, Global, Emergency Care (PubMed Search)
Posted: 7/3/2014 by Jon Mark Hirshon, MPH, MD, PhD
(Updated: 5/4/2026)
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
Background:
Relevance to the EM Physician:
Bottom Line:
University of Maryland Section of Global Emergency Health Author: Terrence Mulligan DO, MPH
Samaras N, Chevalley T, Samaras D, et al. “Older Patients in the Emergency Department: A Review” Annals of EM Vol 56:3, Sept 2010, p 261-269.
WHO Global Burden of Disease. 2010. www.who.int/healthinfo/global_burden_disease/GBD_report_2010update_full.pdf
United Nations. “World Population Ageing 1950-2050” 2011. www.esa.un.org/wpp/
Category: Critical Care
Keywords: blood, anemia, infection, blood transfusions (PubMed Search)
Posted: 7/1/2014 by Feras Khan, MD
(Updated: 5/4/2026)
Click here to contact Feras Khan, MD
Risk of infection from Blood transfusions
JAMA Meta-Analysis
What they found
Bottom Line
Rohde J, et al. Health Care Associated Infection after Red Blood Cell Transfusion. A systematic Review adn Meta-Analysis. JAMA 2014; 311(13): 1317-1326.
Category: Visual Diagnosis
Posted: 6/30/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
49 year-old female on trimethoprim/sulfamethoxazole presents with a rash & lesions on her oral mucus membranes. What's the diagnosis?
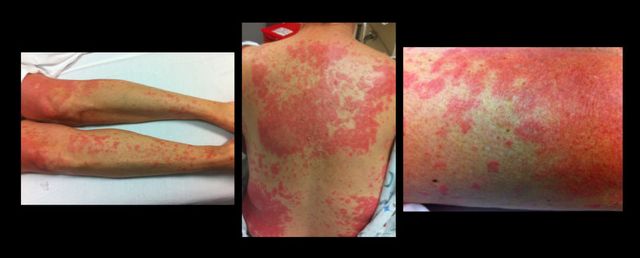
Answer: Steven-Johnson Syndrome (SJS)
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Keywords: IVUS, CAD, vulnerable plaques (PubMed Search)
Posted: 6/29/2014 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
IVUS Plaque Correlation to Cardiovascular Death
Several non-invasive studies are currently utilized for the identification of coronary artery disease (i.e. coronary CTA, intravascular ultrasound- IVUS, etc.)
Few studies have quantified which of those with CAD (i.e. coronary plaques) are considered high-risk or unstable plaques
A recent study utilizing IVUS looked at autopsies over a 2 year-period comparing near-infrared detection of high-risk plaques and cardiovascular related deaths
IVUS findings associated with CAD are classified into 3 categories: echo-attenuation, echolucent zone, and spotty calcification
Echo-attenuated plaques, especially superficial echo-attenuation, was found to be a significant and reliable finding suggestive of vulnerable plaques and future cardiovascular death
Pu J, Mintz G, et al. Insights into echo-attenuated plaques, echolucent plaques, and plaques with spotty calcification. JACC Vol 63, No 2, 2014.
Category: Toxicology
Keywords: Colchicine, Poisoning, Arrhythmia (PubMed Search)
Posted: 6/29/2014 by Kishan Kapadia, DO
Click here to contact Kishan Kapadia, DO
Colchicine tablets and injectable solution is frequently used for the treatment of gout and familial Mediterranean fever. An overdose is extremely serious, with considerable mortality that is often delayed. It is considered a cellular poison due to its inhibition of cellular mitosis of dividing cells.
After an acute overdose, symptoms typically are delayed for 2-12 hours and include nausea, vomiting, abdominal pain, and severe bloody diarrhea.
Chronic poisoning presens with a more insidious onset.
Late complications include bone marrow suppression, particularly leukopenia and thrombocytopenia (4-5 days) and alopecia (2-3 weeks).
Treatment includes aggressive supportive care, monitoring and treatment of fluid and electrolyte disturbances.
The usual cause of death from acute poisoning is due to hemodynamic collapse and cardiac arrhythmias (typically 24-36 hours after ingestion or could be sudden) or from infectious or hemorrhagic complications.
1) Finkelstein Y et al. Colchicine poisoning: the dark side of an ancient drug. 2010 Clin Tox 48(5):404-414.
2) Olson KR, ed. Poisoning & Drug Overdose. 5th ed. New York: McGraw Hill; 2007.
Category: Orthopedics
Keywords: Elbow extension test (PubMed Search)
Posted: 5/27/2014 by Brian Corwell, MD
(Updated: 6/28/2014)
Click here to contact Brian Corwell, MD
Jie KE et al. Extension test and ossal point tenderness cannot accurately exclude significant injury in acute elbow trauma. Ann Emerg Med 2014
Category: International EM
Keywords: tetanus, global, international, infectious disease (PubMed Search)
Posted: 6/25/2014 by Andrea Tenner, MD
(Updated: 5/4/2026)
Click here to contact Andrea Tenner, MD
General Information: Tetanus is caused by the toxin of Clostridium tetani--a gram-positive bacillus found in soil and animal excrement. It is a life-threatening but preventable disease. Cases have declined by > 95% in the past 65 years, but dozens of cases still occur annually in the US and it is still frequently seen in developing countries.
Clinical Presentation:
Diagnosis:
Clinical Case Definition: In the absence of a more likely diagnosis, an acute illness with muscle spasms or hypertonia. There is no diagnostic laboratory test for tetanus.
Treatment:
Bottom Line:
Tetanus is not as rare as we would like to think. Acute diagnostic acumen and assertive clinical management can help save the life of someone with this potentially deadly disease
University of Maryland Section for Global Emergency Health
Author: Jon Mark Hirshon, MD, MPH, PhD
http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6012a1.htm
http://www.cdc.gov/vaccines/pubs/surv-manual/chpt16-tetanus.html
http://emedicine.medscape.com/article/229594-treatment
Category: Critical Care
Posted: 6/24/2014 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Prophylactic FFP for Procedures?
Category: Visual Diagnosis
Posted: 6/22/2014 by Haney Mallemat, MD
(Updated: 6/23/2014)
Click here to contact Haney Mallemat, MD
35 year-old female presents with nausea and vomiting 1 week post-op for an abdominal surgery. Abdominal ultrasound is below; what's the diagnosis?
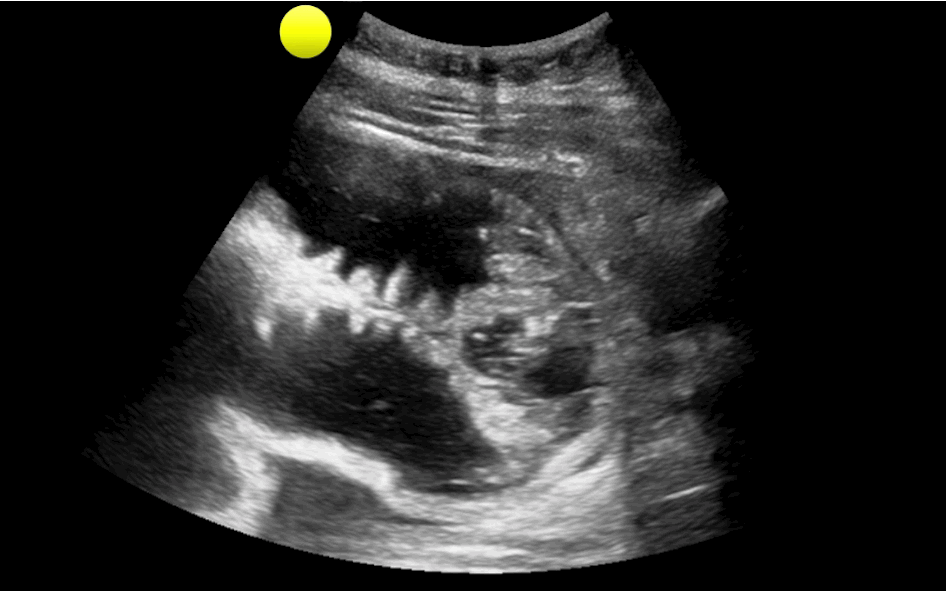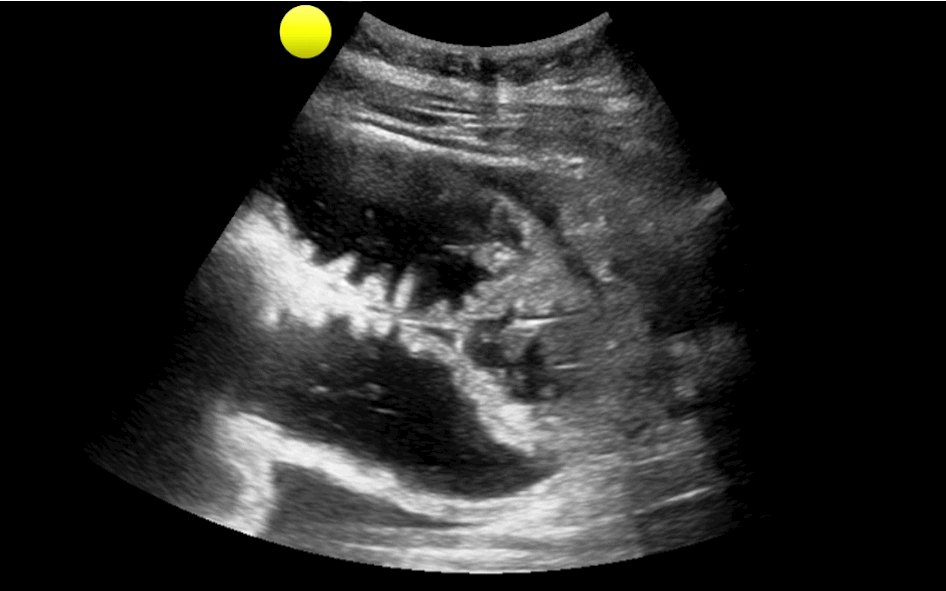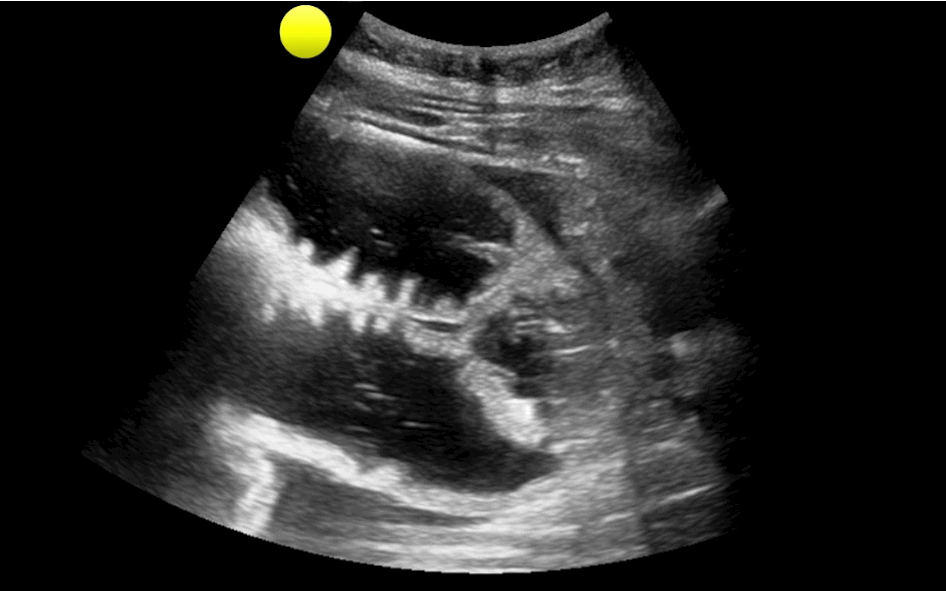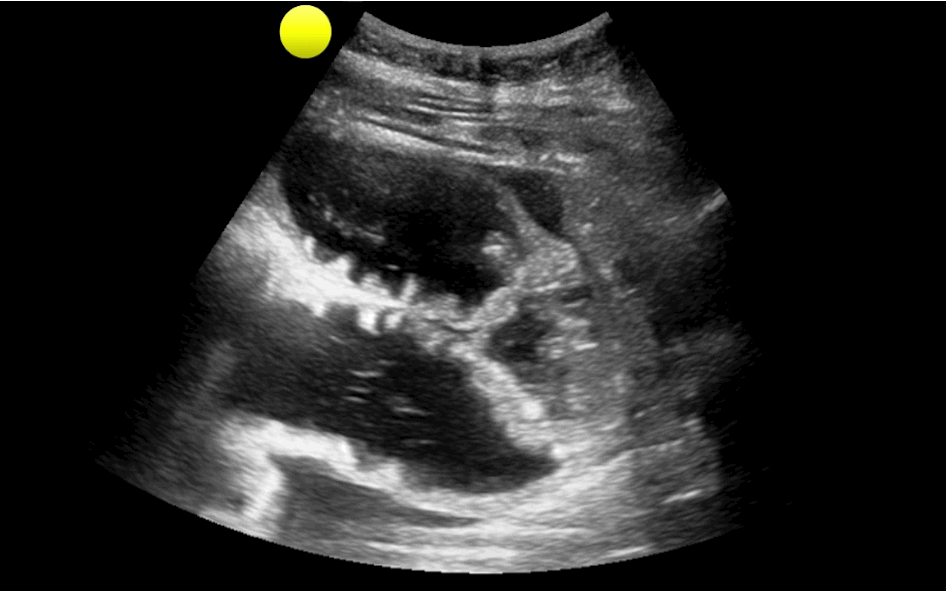
Small bowel obstruction (SBO)
Ultrasound for Small bowel obstruction (SBO)
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Orthopedics
Keywords: knee, injury, dislocation (PubMed Search)
Posted: 6/21/2014 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
Some quick facts about Knee Injuries:
Category: Pediatrics
Keywords: Ultrasound, pediatrics, appendicitis (PubMed Search)
Posted: 6/20/2014 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Category: Toxicology
Keywords: NAC, acetaminophen (PubMed Search)
Posted: 6/19/2014 by Hong Kim, MD
Click here to contact Hong Kim, MD
NAC is an effective antidote against acetaminophen (APAP) toxicity in preventing acute hepatotoxicity. It provides cysteine that is essential for glutathione synthesis and its availability is rate limiting.
Currently, PO and IV formulation is available in the U.S. Regardless of the route, NAC is equally effective in preventing APAP induced acute hepatotoxicity when administered within 8 hours after single acute ingestion. 1
Adverse effects of NAC
1. Anaphylactoid reaction
a. More frequently reported with IV administration and during the first regimen of NAC (150 mg/kg over 60 min) administration. (dose and rate dependent)
b. Higher risk of anaphylactoid reaction in patients with negative APAP vs. patients with elevated APAP level.2
c. Management: Benadryl as needed and slow infusion rate.
2. Hyponatremia in children if inappropriate volume of diluent (D5W) used. Dose calculator: http://acetadote.com/dosecalc.php
3. Laboratory: increase Prothrombin time (PT).3
4. Fatality from iatrogenic NAC overdose has been reported.
Advantage of IV NAC
1. Convenience
2. 100% bioavailability
3. Shorter hospital length of stay
4. Minimum GI symptoms (nausea & vomiting) compared to PO route
Indication of IV NAC
1. Severe hepatotoxicity or fulminant liver failure
2. APAP poisoning during pregnancy
3. Unable to tolerate PO intake (nausea, vomiting, altered mental status)
However many clinicians administer IV NAC for their advantages over PO NAC.
Take home message:
1. PO and IV NAC are equally effective when administered within 8 hours after single acute ingestion.
2. Anaphylactoid reaction is frequently encountered AE during the infusion of 1st NAC regimen and patients with negative/low APAP level may be at higher risk.
3. No emergent need to start NAC in presumed acetaminophen overdose patients prior to obtaining APAP level.
Category: International EM
Keywords: Schistosomiasis, parasites, international (PubMed Search)
Posted: 6/18/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Clinical Presentation:
A 35-year-old female presents to your emergency department complaining of fever, malaise, myalgias, headache and an urticarial rash. Her physical exam reveals a papular rash and hepatosplenomegaly. You also find out that she traveled to Sudan 6 weeks earlier. She stayed mostly in Kharotum, but while there, she swam in the Nile. You send a smear for malaria, which is negative. What other major parasite should you consider?
Diagnosis:
Discussion:
While the acute presentation is generally non-specific, chronic complications may be more serious. Many organ systems can be impacted and symptoms of chronic infection can include liver dysfunction, including portal hypertension and esophageal varacies or hematuria and renal failure.
Treatment:
Bottom Line:
Consider a broader differential in travelers. There are many infectious killers that can be easily treated.
University of Maryland Section of Global Emergency Health
Author: Jon Mark Hirshon, MD, MPH, PhD
Category: Critical Care
Keywords: Thrombelastography, TEG, ROTEM, Hemorrhagic Shock (PubMed Search)
Posted: 6/13/2014 by John Greenwood, MD
Click here to contact John Greenwood, MD
Thrombelastography for Management of Non-Traumatic Hemorrhagic Shock
The use of thrombelastography (TEG, ROTEM) has traditionally been utilized and studied in the management of acute coagulopathy of trauma (ACoT) developed by patients in hemorrhagic shock secondary to trauma.
Functional coagulation tests such as the TEG may provide valuable information when resuscitating the hemorrhaging patient, especially if there is any concern for an underlying coagulopathy.
The following is a TEG recently returned during the resuscitation of a 60 y/o male with a history of HCV cirrhosis presenting with hemorrhagic shock secondary to a massive upper GIB. The University's Massive Transfusion Protocol was promptly activated and at this point, the patient had received approximately 4 units of PRBCs & FFP along with 1 liter of crystalloid. His Hgb was 5, PT/PTT/INR were undetectable, and his fibrinogen was 80.
Below is a table that simplifies the treatment, based on the test's abnormalities:
After reviewing the initial TEG, all perameters were abnormal in addition to the presence of significant fibrinolysis. The patient was given an additional 4 units of FFP, DDAVP, cryoprecipitate, a unit of platelets, and aminocaproic acid. The patient still required significant resuscitation, however bleeding had significantly decreased as well has his pressor requirement. Below is the patient's follow-up TEG 2 hours later.
There is growing enthusiasm for the use of functional coagulopathy testing in the patient with hemorrhagic shock. Early resuscitation with blood products as your fluid of choice with limited fluid administration while arranging for definitive source control are critical, but also consider early thrombelastography to detect additional causes for uncontrolled hemorrhage.
References
Follow Me On Twitter: @JohnGreenwoodMD
email: johncgreenwood@gmail.com
Category: Visual Diagnosis
Posted: 6/15/2014 by Haney Mallemat, MD
(Updated: 6/16/2014)
Click here to contact Haney Mallemat, MD
41year-old male without past medical history presents with the image below. What's the diagnosis and what's the most likely causative organism?
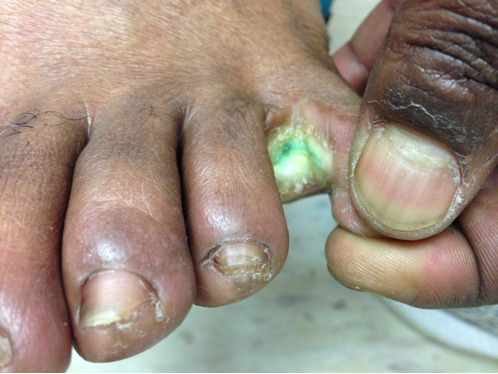
Gram-Negative web-space infection; most common etiologic organism is Pseudomonas
Gram Negative Web-space Infections
Gram-negative infections may occur in toe web-spaces of healthy patients, especially in areas with hyperhidrosis (excessive perspiration) and macerated skin.
Common organisms include Pseudomonas; others include Corynebacterium minutissimum (causes erythrasma, chronic superficial infection of the intertriginous areas of the skin), and other gram-negative bacteria
Woods-light examination may be clinically helpful if Pseudomonas is suspected (fluoresce green) and erythrasma will fluoresce coral red. KOH direct examination for fungal elements may show the presence of dermatophytes or Candida.
Treatment:
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Wolff, K., & Johnson, R. J. (2009). Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology. (6th ed., pp. 662-664;698). McGraw-Hill.
http://www.aafp.org/afp/2005/0901/p833.html
http://emedicine.medscape.com/article/1055306-overview
Category: Toxicology
Keywords: methadone, QTc, overdose (PubMed Search)
Posted: 6/9/2014 by Bryan Hayes, PharmD
(Updated: 6/21/2014)
Click here to contact Bryan Hayes, PharmD
Methadone prolongs the QTc interval. Is the degree of QTC widening correlated to worse outcomes after overdose?
The authors of a new study concluded the triage QTc can predict death, intubation, and respiratory arrest. QTc thresholds of 470, 447.5, and 450 msec had sensitivity (95 % CI) and specificity (95 % CI) of 87.5 (47.3-99.7), 86.8 (74.7-94.5), and 77.3 (62.2-88.5), respectively.
My Thoughts
Respiratory depression is the predominant cause of death in methadone overdoses. QTc interval prolongation may have the potential to help predict outcomes, but the QTc thresholds in this study were really not that prolonged. Patients on chronic methadone without overdose have baseline QTc intervals longer than those in this study after overdose.
Application to Clinical Practice
Many factors contribute to the ultimate disposition of methadone overdose cases. Even if QTc widening is correlated to outcomes, it really won't change our management.
Farsi D, et al. The correlation between prolonged corrected QTc interval with the frequency of respiratory arrest, endotracheal intubation, and mortality in acute methadone overdose. Cardiovasc Toxicol 2014 May 9. [Epub ahead of print] [PMID 24811951]
Follow me on Twitter (@PharmERToxGuy) or Google Plus (+bryanhayes13)
Category: International EM
Keywords: Malaria, International, Travel, fever (PubMed Search)
Posted: 6/11/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation:
A 64 yo male with a history of IDDM presents with generalized fatigue. He felt so weak last night that he missed his pm dose of Lantus and vomited this morning. He arrived with a critically elevated BG of 590. He flew to the US from Sierra Leone 3 days ago.
Labs include:
Wbc 3.5 Plt 34 Hb 12 Hct 36
Na 125 CL 93 Co2 14 K 4.5 BUN 25 Cr 1.9 Glu 590 AG 18
VBG pH 7.23
Clinical Question:
Other than treating his diabetic ketoacidosis and renal failure, would you send any further tests?
Answer:
Thick smear for Malaria.
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Bradford Schwartz, MD
Ansari, Khoharo, Akhund, and Qureshi. Thrombocytopenia in plasmodium falciparum malaria.J Ayub Med Coll Abbottabad. 2009 Apr-Jun;21(2):145-7.
Kumar and Shashirekha. Thrombocytopenia--an indicator of acute vivax malaria. Indian J Pathol Microbiol. 2006 Oct;49(4):505-8.
Lacerda, Mourao, Coelho, and Santos. Thrombocytopenia in malaria: who cares? Mem Inst Oswaldo Cruz. 2011 Aug;106 Suppl 1:52-63.
Category: Critical Care
Posted: 6/10/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 6/8/2014 by Haney Mallemat, MD
(Updated: 6/9/2014)
Click here to contact Haney Mallemat, MD
28 year-old female with history of chronic back pain presents with right-foot numbness and inability to move her foot at the ankle joint. What’s the diagnosis and what neurologic finding would you expect to find?
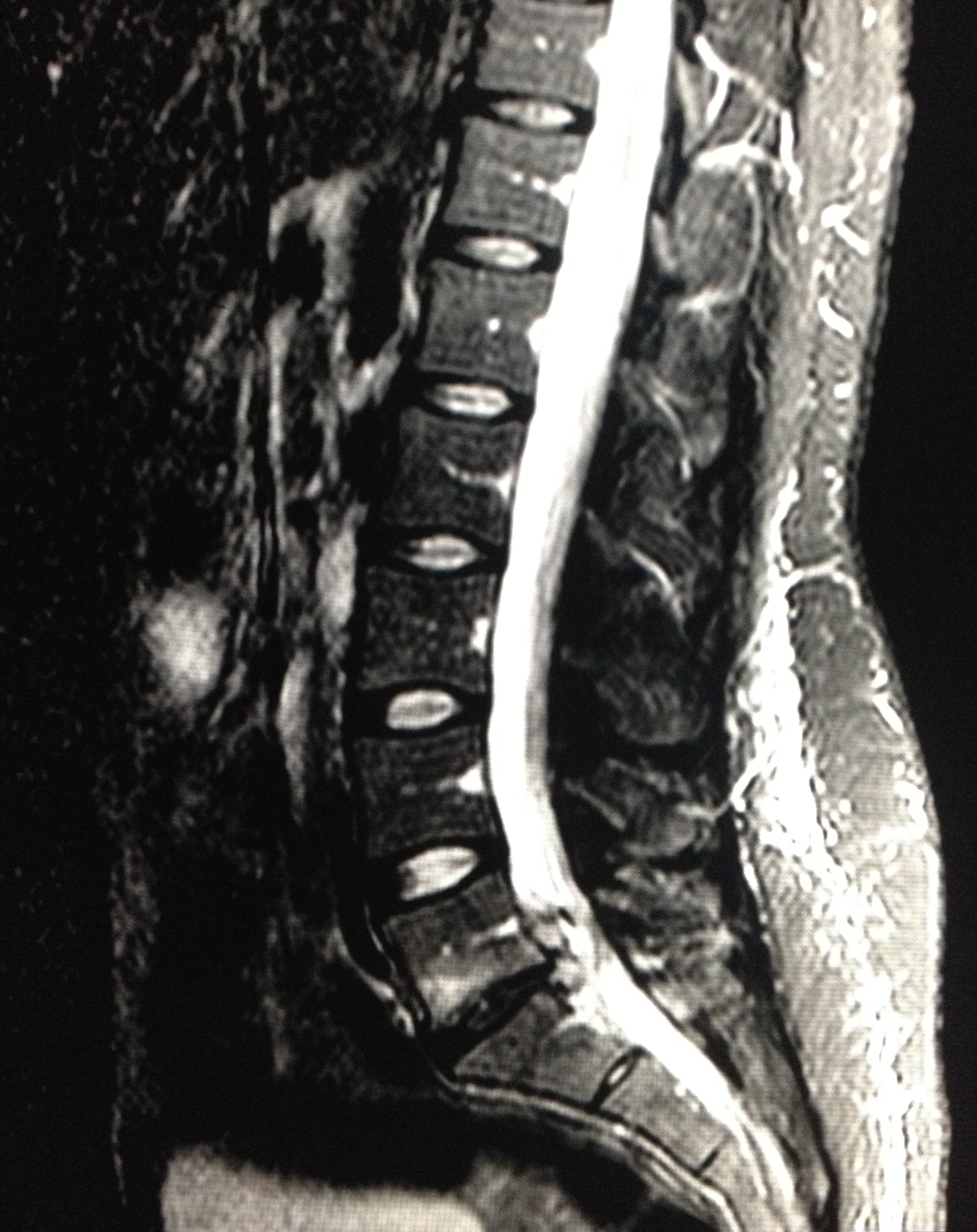
Large disc bulge at L5-S1
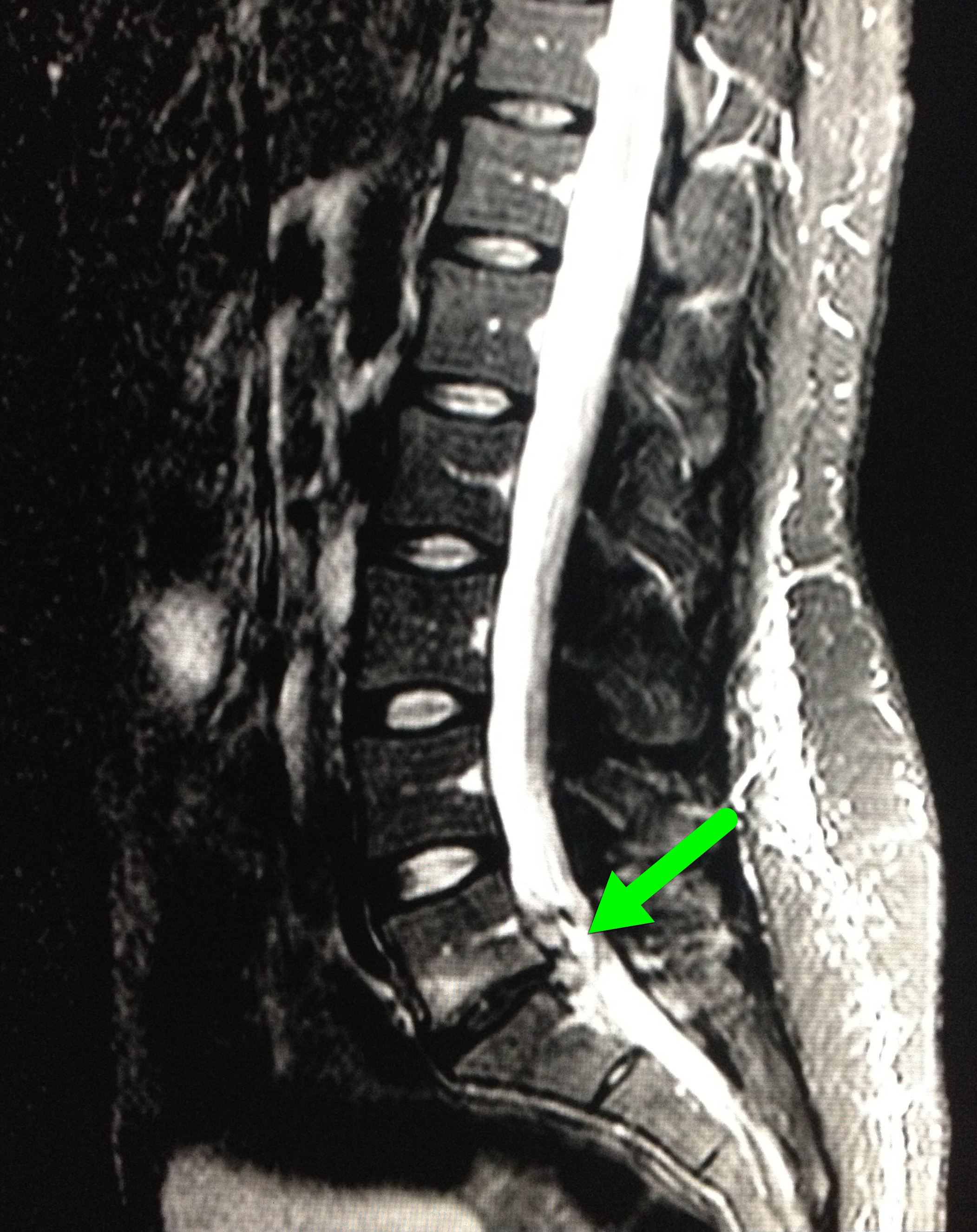
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
