Category: Visual Diagnosis
Posted: 2/3/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
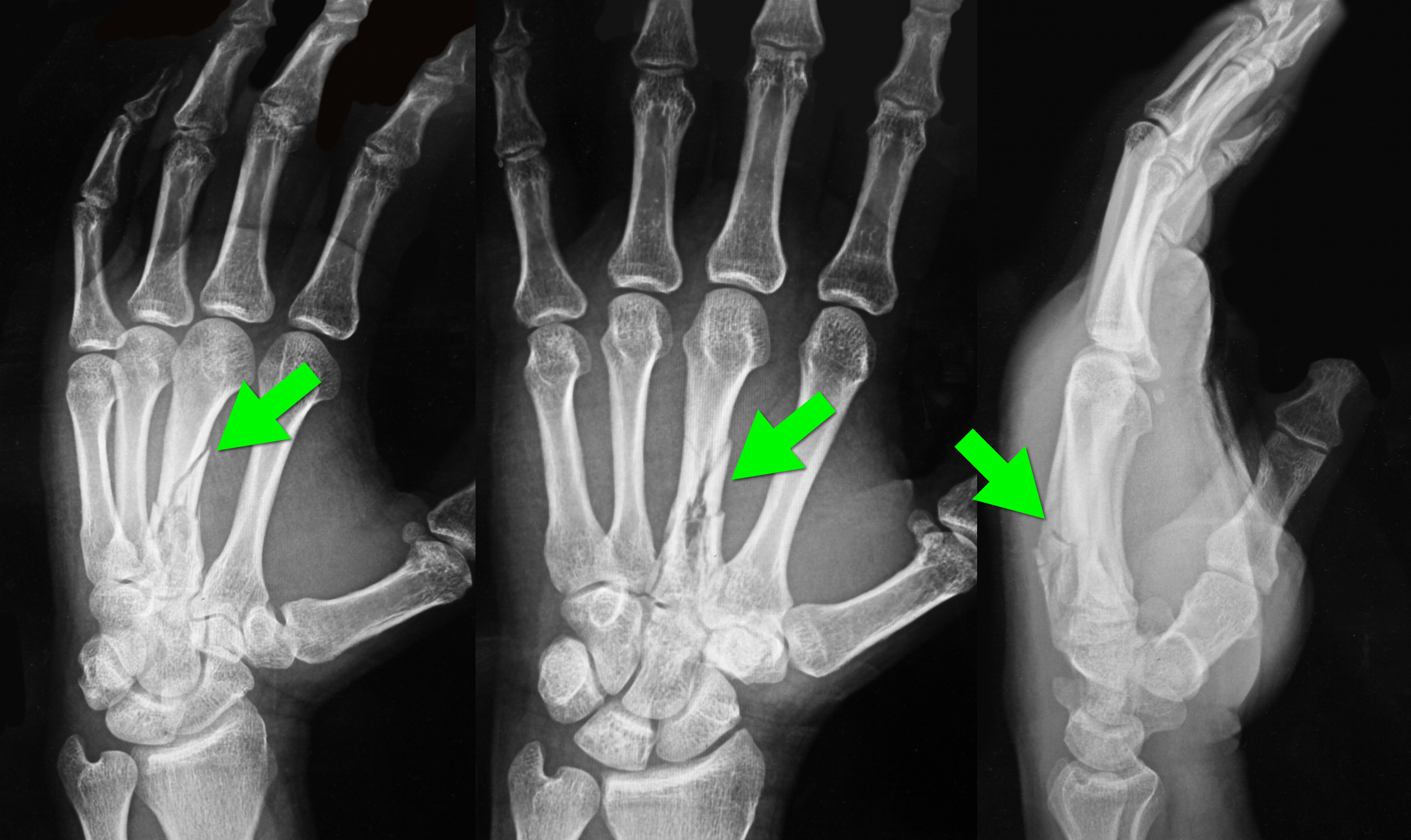
34 year-old left-hand dominant male sustained injury to left hand after his pressurized greasing-gun discharged into the palm of his hand. He has a small lac to the hand but is in extreme pain. On exam his hand is very puffy and he is neurovascularly intact (XR below) What is the next step in management?
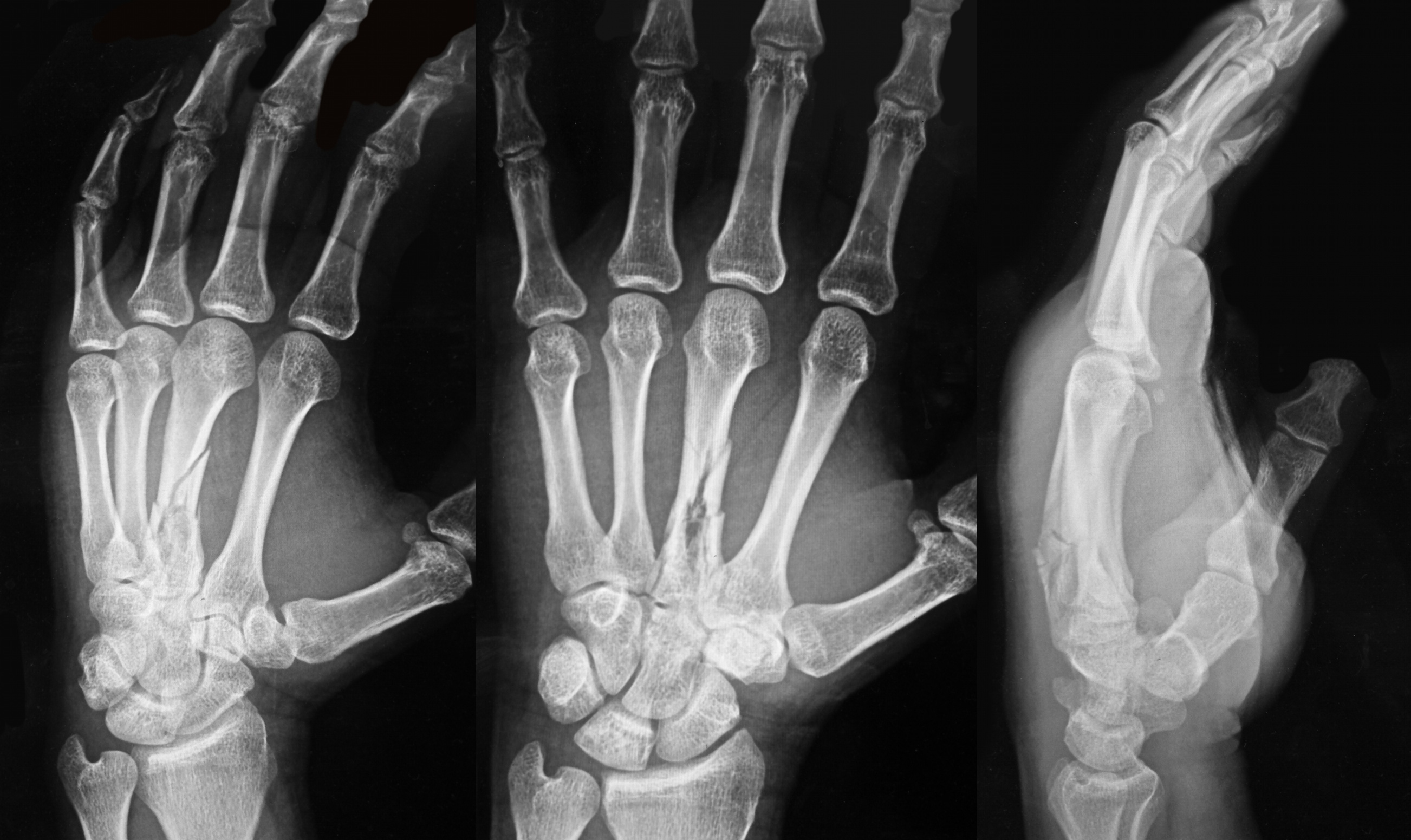
Metacarpal fracture; emergent surgical consult is required
High-Pressure Injection Injuries (HPI) injuries
HPI devices (e.g., grease, paint guns, etc.) may cause injury when the device accidently discharges, typically into the operator’s dominant hand during attempts to clean the nozzle.
Injuries may initially appear benign, however injuries should be considered surgical emergencies because they often require debridement / washout of materials injected into deeper tissues.
Tissue damage is multi-factorial and includes direct injury (e.g., high-pressure tissue damage, vascular compression, etc.) and indirect injury from material injected into tissues (e.g., chemical inflammation / injury, granuloma formation, deep-tissue infections, etc.).
Radiographs may assist surgical planning by identifying subcutaneous air, debris, or unanticipated fractures.
Treatment:
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 2/2/2014 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Myocardial Infarction in Women After Childbirth
World Health Organization reports that obesity is the 5th leading cause of global death with the highest impact on women <65 years of age
The association of obesity and cardiovascular risk in young women is currently being researched
A recent nationwide cohort looking at obesity and future cardiovascular risk looked at Danish women giving birth (2004-2009) and followed them a median time of 4.5 years
This study grouped women via pre-pregnancy body mass index (BMI)
1. Underweight (BMI <18.5)
2. Normal weight (BMI <25)
3. Overweight (BMI <30)
4. Obese (BMI >30)
Data revealed that healthy women of fertile age, pre-pregnancy obesity alone was associated with increased risk of myocardial infarction in the years after childbirth
Schmiegelow M, Andersson C, Kober L, et al. Prepregnancy Obesity and Associations With Stroke and Myocardial Infarction in Women in the Years After Childbirth. Circulation 2014;129:330-337.
Category: Pharmacology & Therapeutics
Keywords: methadone, withdrawal (PubMed Search)
Posted: 1/23/2014 by Bryan Hayes, PharmD
(Updated: 2/1/2014)
Click here to contact Bryan Hayes, PharmD
In most situations (dependant on state laws and institutional policies), methadone-maintained patients enrolled in a drug abuse program are best managed by continuing methadone at the usual maintenance levels with once-a-day oral administration.
Pearl: In the event the methadone clinic is closed and/or the dose cannot be verified, 30-40 mg (10-20 mg IM) is generally enough to prevent withdrawal in most patients.
This is only a short-term measure and some patients may require additional methadone. Full doses of methadone should be reinstituted as soon as possible.
Fultz JM, et al. Guidelines for the management of hospitalized narcotic addicts. Ann Intern Med 1975;82(6):815-8. [PMID 1138596]
Alford DP, et al. Acute pain management for patients receiving maintenance methadone or buprenorpine therapy. Ann Intern Med 2006;144(2):127-34. [PMID 16418412]
Freedman DX, et al. Methadone treatment of heroin addiction. Annu Rev Med 1973;24:153-64. [PMID 4575849]
Follow me on Twitter (@PharmERToxGuy) or Google Plus (+bryanhayes13)
Category: Toxicology
Keywords: dexmedetomidine, alcohol withdrawal (PubMed Search)
Posted: 1/30/2014 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Category: International EM
Keywords: Virus, Fever, West Nile, Dengue (PubMed Search)
Posted: 1/29/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation: A 63 year old woman from Texas with no recent international travel presents to the ED with persistent fatigue which onset a month ago and is associated with anorexia and occasional fevers and chills. She has been to her family doctor who tested her for a number of viral illnesses and was told she had West Nile virus.
Clinical Question:
What other febrile illness could this be?
Answer:
This patient had dengue. Dengue is now endemic in the US, and locally-acquired cases have been reported in Florida, Texas and Hawaii. The fatigue and anorexia are typical and can last for weeks after other symptoms have resolved.
West Nile virus testing may be falsely positive when another flavivirus is present such dengue, yellow fever or Japanese encephalitis.
Bottom Line:
Other possible illnesses like dengue should be considered in patients who have tested positive for West Nile virus.
University of Maryland Section of Global Emergency Health
Author: Jenny Reifel Saltzberg, MD, MPH
Sharp TM, et al. Fatal hemophagocytic lymphohistiocytosis associated with locally acquired dengue virus infection - New Mexico and Texas, 2012. MMWR Morb Mortal Wkly Rep. 2014 Jan 24;63(3):49-54. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6303a1.htm?s_cid=mm6303a1_w
Centers for Disease Control and Prevention. Dengue and Dengue Hemorrhagic Fever: Information for Health Care Practitioners. http://www.cdc.gov/dengue/resources/Dengue&DHF%20Information%20for%20Health%20Care%20Practitioners_2009.pdf
Category: Critical Care
Posted: 1/28/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
NSSTIs occur secondary to toxin-secreting bacteria; NSSTIs are surgical emergencies with a high-morbidity / mortality
Risk factors: immunocompromised host (DM, AIDS, etc.), intravenous drug use, malnourishment, peripheral vascular disease
Type I (polymicrobial; most common), Type II (monomicrobial; typically clostridia, streptococci, staph, or bacteroides), Type III (Vibrio vulnificus; seawater exposure)
Signs / Symptoms: pain out of proportion to exam (occasionally no pain at all), skin findings (blistering / bullae, gray-skin discoloration, or “Dishwater-like” discharge), or systemic toxicity (altered mental status, elevated lactate, etc.)
Diagnostic radiology
Treatment is emergent surgical debridement with simultaneous hemodynamic resuscitation PLUS broad-spectrum antibiotics; consider clindamycin becuase it has anti-toxin activity
Adjunctive therapies include Intravenous intraglobulin (neutralizes toxins secreted by bacteria) and hyperbaric oxygen

Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 1/27/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
32 year-old with diabetes presents with fever, erythema, and warmth of his lower extremity; his leg is not particularly painful. He is diagnosed with cellulitis, started on antibiotics, and admitted to the hospital. While boarding in the Emergency Department he becomes rigorous and hypotensive. An ultrasound of his cellulitis is performed and is shown below. What’s the diagnosis?

"Cobblestoning" of subcutaneous tissue consistent with cellulitis. There are also areas of subcutaneous air raising the concern for necrotizing fasciitis.
Special thanks to Dr. Mike Mallin from the Ultrasound Podcast for the clip. Want to see more amazing ultrasound clips? Check out Sonocloud

Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Keywords: Wide complex tachycardia, ventricular tachycardia (PubMed Search)
Posted: 1/26/2014 by Ali Farzad, MD
(Updated: 3/23/2014)
Click here to contact Ali Farzad, MD
A 48 year old woman has acute chest pain and palpitations over the past several hours. She has felt similar palpitations in the past but never sought medical attention. She arrives to your ED alert and anxious. HR = 270, BP=130/100. ECG is below. What’s the diagnosis and treatment?
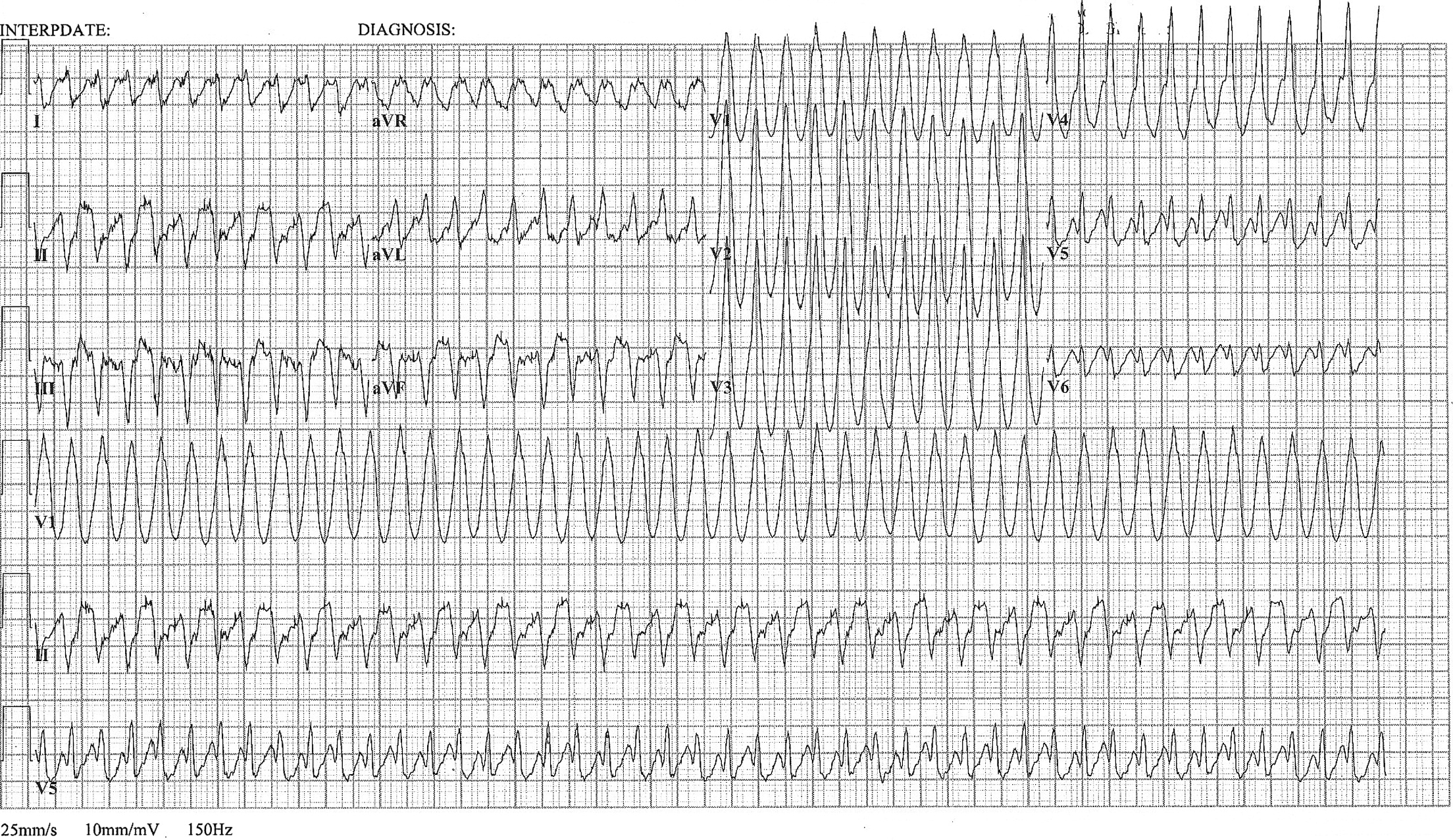
Most wide complex regular tachycardias are ventricular tachycardia (VT). However, supraventricular tachycardias can also cause wide complexes through aberrant conduction and accessory pathways.
Nelson JG, Zhu DW. Atrial Flutter with 1:1 Conduction in Undiagnosed Wolff-Parkinson-White Syndrome. The Journal of Emergency Medicine. January 2014. Pubmed Link
Category: Orthopedics
Keywords: MCL, knee, (PubMed Search)
Posted: 1/17/2014 by Brian Corwell, MD
(Updated: 1/25/2014)
Click here to contact Brian Corwell, MD
Pelllegrini-Stieda lesion
Ossified post-traumatic lesions at the MCL adjacent to the femoral attachment site of the medial femoral condyle.
Mechanism is likely from an avulsion injury that subsequently calcifies after the initial trauma.
Often an incidental finding on plain films.
If symptomatic, refer to ortho as an outpatient
If not symptomatic, no treatment is indicated
http://images.radiopaedia.org/images/30076/b62e61e83241e30f2da693901edcdc_gallery.jpg
http://www.imageinterpretation.co.uk/images/knee/PELLEGRINI%20STIEDA2.jpg
Category: Toxicology
Keywords: pharmacology (PubMed Search)
Posted: 1/23/2014 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Everyone has admitted an altered mental status, patient or bradycardic patient and all of your test results are coming back normal except for a mild increase in creatinine. Take a look at the medication list. Creatinine is a poor indicator of renal function and GFR may be severely impaired even with a mild elevation of creatinine. If you have a predominantly renally excreted drug, you can see toxic effects of a drug even if administered at therapeutic levels.
Common bradycardia inducing medication that is renally cleared: atenolol (very high renal excretion) and digoxin (70%).
Altered Mental Status and on Keppra? Keppra is 100% renally cleared!
Ask your pharmacist for help with the medication list with renal or hepatic insufficiency.
Category: International EM
Keywords: International, snake, venom, (PubMed Search)
Posted: 1/22/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
98% of venomous snake bites in the US are due to pit vipers. Occasionally a snake bite is from an exotic venomous snake being kept as a pet. In 2005, 142 exotic poisonous snakes were reported to poison control. It can be very challenging to find antivenom for these exotic animals.
Antivenom is usually specific to a family or subfamily, so the snake must be identified. Most exotic snake owners will know the common name and possibly the scientific name of the animal.
The WHO database of venomous snakes can help with identification of the species and will list antivenom available globally.
Poison centers are essential to help locate the antivenom and assist with treatment.
Relevance to the EM Physician:
When a patient presents with an exotic snake envenomation, the WHO website below can be helpful to identify the species and possible antivenom.
http://apps.who.int/bloodproducts/snakeantivenoms/database/
University of Maryland Section of Global Emergency Health
Author: Jenny Reifel Saltzberg
C Lubich and EP Krenzelok. Exotic snakes are not always found in exotic places: how poison centres can assist emergency departments.” Emerg Med J. 2007 November; 24(11): 796–797.
Melisa W. Lai, et al. 2005 Annual Report of the American Association of Poison Control Centers’ National Poisoning and Exposure Database. Clinical Toxicology, 44:803–932, 2006
http://www.who.int/neglected_diseases/diseases/snakebites/en/index.html
Category: Critical Care
Keywords: arterial line, catheter related blood stream infections (PubMed Search)
Posted: 1/20/2014 by John Greenwood, MD
(Updated: 1/21/2014)
Click here to contact John Greenwood, MD
Arterial Catheter-Related Blood Stream Infections
Whether arterial lines are a potential source of catheter-related blood stream infections (CRBSIs) is highly-debated; however, based on a recent systematic review they are an under recognized and significant source of CRBSIs.
Bottom Line(s)
Follow me on twitter @medicalgraffiti
Category: Visual Diagnosis
Posted: 1/20/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
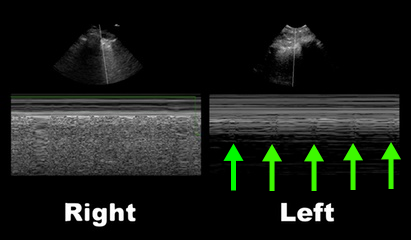
50 year-old male intubated for respiratory distress. Ultrasound is used post-intubation to confirm tube placement and the following images are obtained. What's the diagnosis?
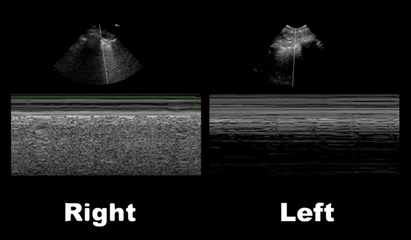
Right main-stem intubation as demonstrated by presence of lung-pulse on the left side
Lung-Pulse
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 1/19/2014 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Pacing Atrioventricular Block
- Atrioventricular (AV) block is classically treated with restoration of heart rate via right ventricular pacing, however high rates of right ventricular pacing is associated w/ left ventricular systolic dysfunction
- A recent multi-center randomized control trial (RCT) assessed the efficacy of right vs biventricular pacing in heart failure w/ AV block [BLOCK HF Trial]
- Primary outcomes of: morbidity, mortality, and adverse left ventricular remodeling were shown to be significantly lower in biventricular vs right ventricular pacing
- In patients with a high rate of pacing and/or an abnormally low left ventricular ejection fraction biventricular pacing may be more advantageous than conventional right ventricular pacing
Curtis A.B., Worley S.J., Adamson P.B.,et al: Biventricular pacing for atrioventricular block and systolic dysfunction. N Engl J Med 2013; 368: 1585-1593
Category: Misc
Keywords: Postoperative, fever, cause (PubMed Search)
Posted: 1/18/2014 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
Post Operative Fever is extremely common, and with the increase in same day surgery this is a common complaint presenting to the ED. The mnemonic "5Ws" are often taught to remember the causes. They are:
Though many surgical textbooks report that atelectasis is the most common cause of early post-operative fever, some even claiming that it is responsible for over 90% of febrile episodes in the first 48 hours after surgery; a recent review in CHEST (reference below) showed that there is no evidence to support this. We often see atelectasis in medical patients too, and few if any of them have fever. The CHEST review found that there was no clear evidence that atelectasis causes fever at all.
Pearl: Temperature >38.9C should raise concern for a true infection, where lower temperatures can be due to pulmonary embolism, DVT, drug fever, etc….
Mavros MN, Velmahos GC, Falagas ME.Atelectasis as a cause of postoperative fever: where is the clinical evidence? Chest. 2011 Aug;140(2):418-24. doi: 10.1378/chest.11-0127. Epub 2011 Apr 28. Review. PMID: 21527508
Category: Pediatrics
Keywords: hyponatremia, maintenance fluid (PubMed Search)
Posted: 1/17/2014 by Jenny Guyther, MD
(Updated: 5/4/2026)
Click here to contact Jenny Guyther, MD
Wang et al. Isotonic Versus Hypotonic Maintenance IV Fluids in Hospitalized Children: A Meta-Analysis. Pediatrics 2014; 133;105.
Category: International EM
Keywords: influenza, China, Asia, Avian, Swine, Global (PubMed Search)
Posted: 1/12/2014 by Andrea Tenner, MD
(Updated: 1/15/2014)
Click here to contact Andrea Tenner, MD
General Information:
The H’s and N’s refer to hemagglutinin and neuraminidase—two proteins on the surface of the Influenza A virus that help it attach. Here’s a quick breakdown of important emerging strains of influenza:
Avian flu:
Swine flu:
Relevance to the EM Physician:
As the frontline against the flu virus, we should know what to expect. H1N1 has predominated this flu season—so far 60% of hospitalizations occurred in patients aged 18-64, which is unusual. H7N9 is new on the scene but might be imported, and H5N1 has arrived.
Bottom Line:
Expect to see more severe illness in the 18-64 y/o age group due to H1N1. Watch for more deadly flu imports--obtain a travel history and notify the CDC of severe influenza-like illness in returned travellers.
University of Maryland Section of Global Emergency Health
Author: Andi Tenner, MD, MPH, FACEP
http://www.cdc.gov/flu/avianflu/h5n1-people.htm
http://www.cdc.gov/flu/weekly/summary.htm
http://www.cdc.gov/flu/avianflu/h7n9-virus.htm
Category: Critical Care
Keywords: brain death (PubMed Search)
Posted: 1/14/2014 by Feras Khan, MD
Click here to contact Feras Khan, MD
Determination of Brain Death
Clinical Examination
If apnea testing cannot be performed due to instability, hypoxia, or cardiac arrhythmias, then a confirmatory test should be performed (from highest to lowest sensitivity):
There is state to state variation on who can perform the test and how many separate examinations need to be performed before brain death can be legally declared.
For a great review on some of the pitfalls in making the diagnosis and difficulties with the examination, please see the attached article.
Category: Visual Diagnosis
Posted: 1/13/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
42 year-old male s/p assault complains of right sided facial pain, swelling, and decreased vision. Physical exam reveals subconjunctival hemorrhage, proptosis, afferent pupillary defect, and a firm globe. What's the diagnosis and what's the emergent treatment?
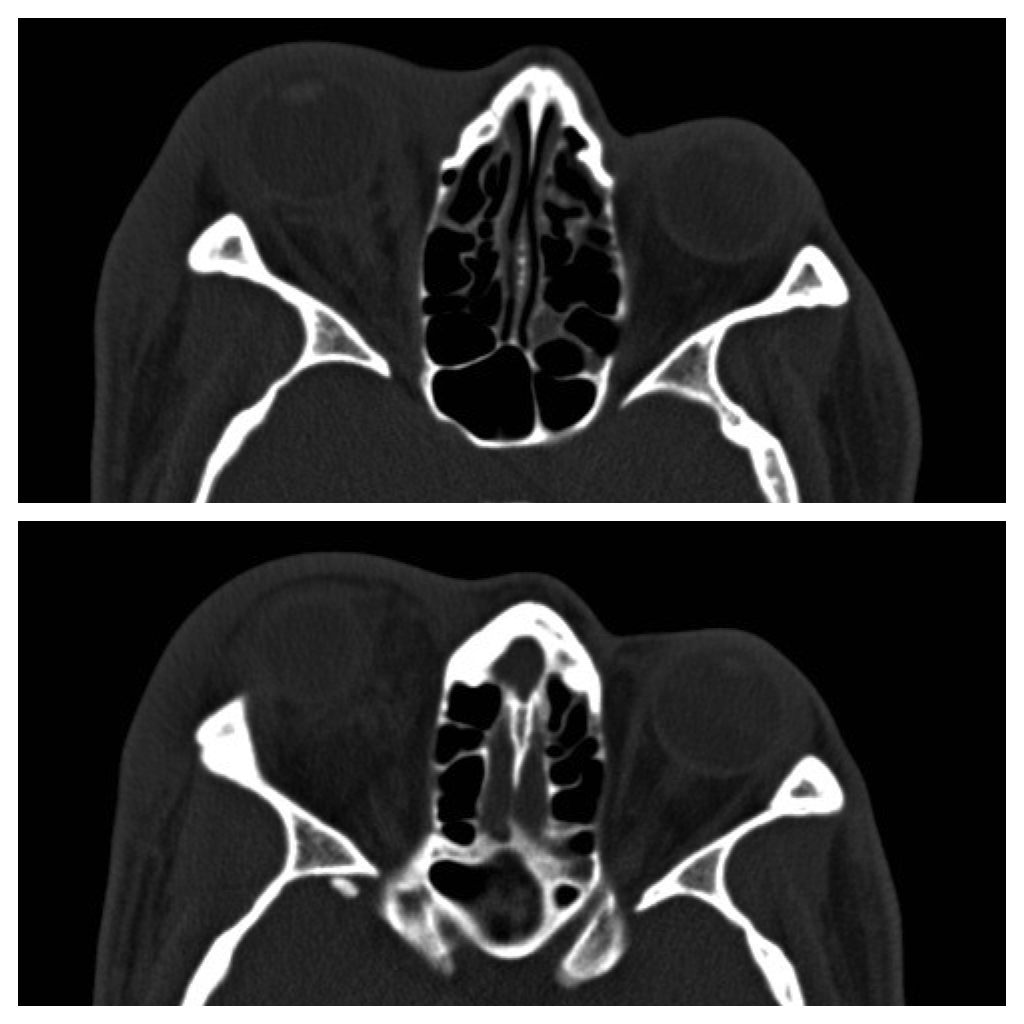
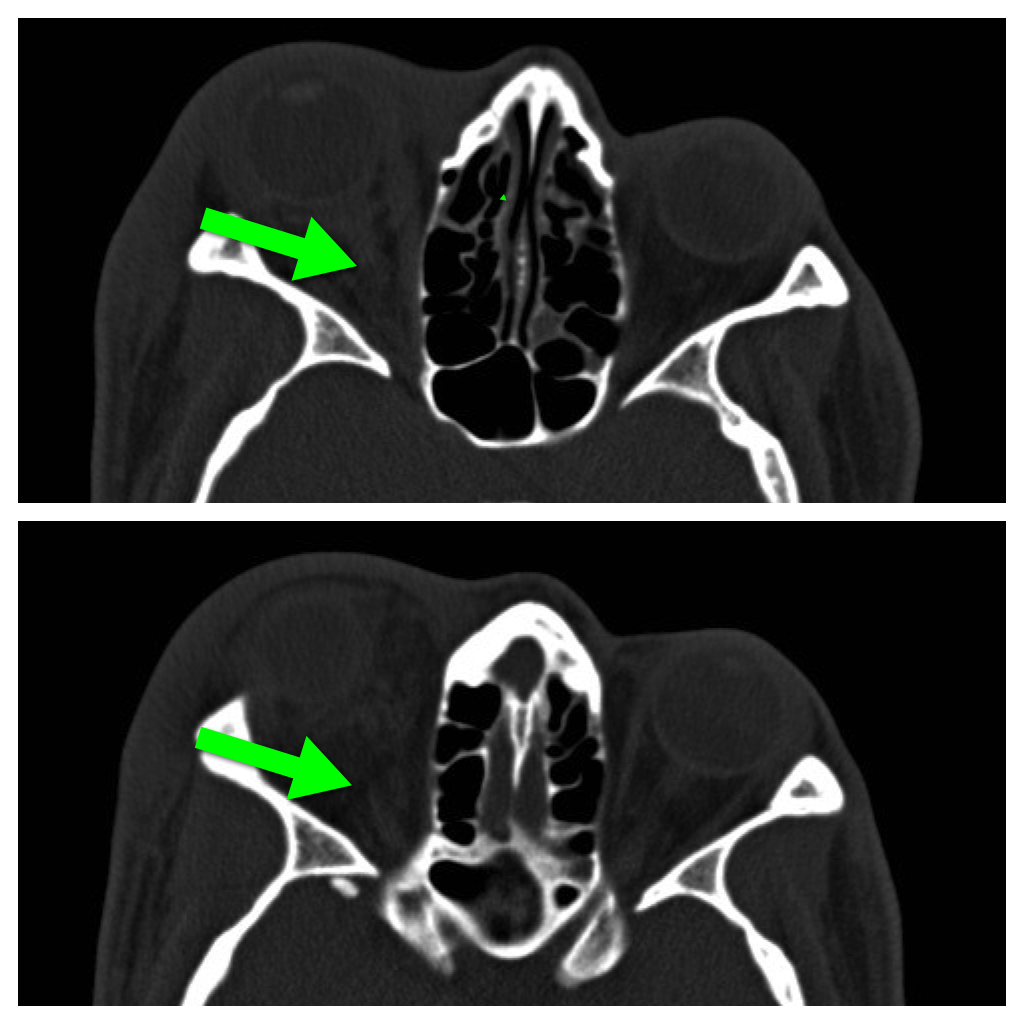
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Keywords: PVC, Premature ventricular beats, Premature ventricular complexes (PubMed Search)
Posted: 1/12/2014 by Ali Farzad, MD
(Updated: 3/10/2014)
Click here to contact Ali Farzad, MD
Differentiation between right and left ventricular origin of premature beats can be useful clinically.
PVCs arising from the right ventricle have a left bundle branch block morphology (dominant S wave in V1)
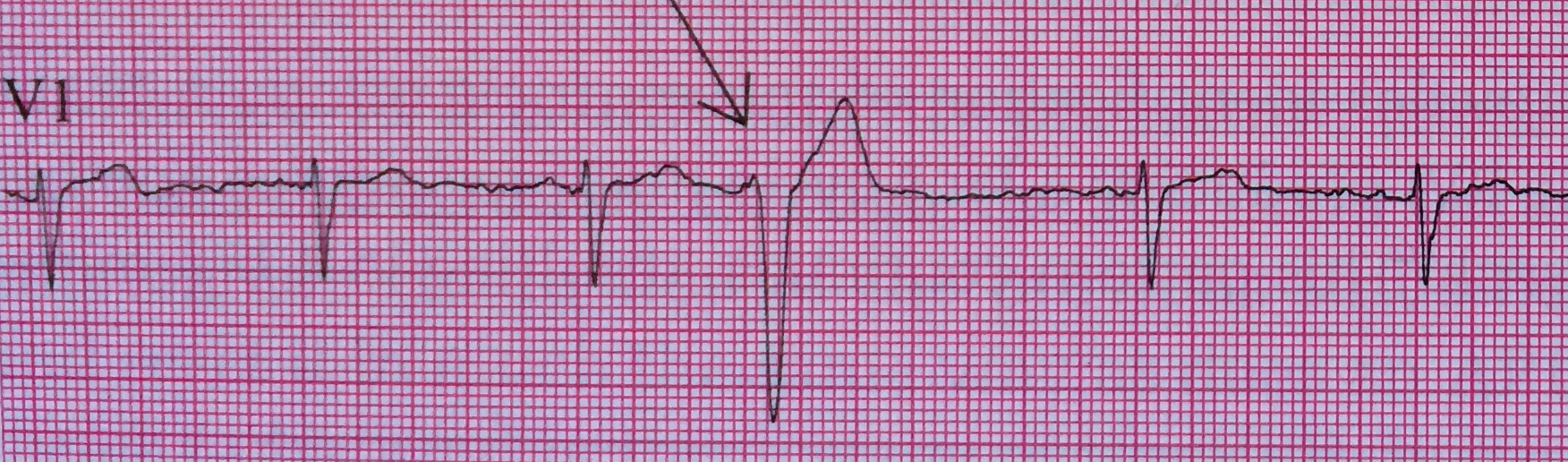
PVCs arising from the left ventricle have a right bundle branch block morphology (dominant R wave in V1)
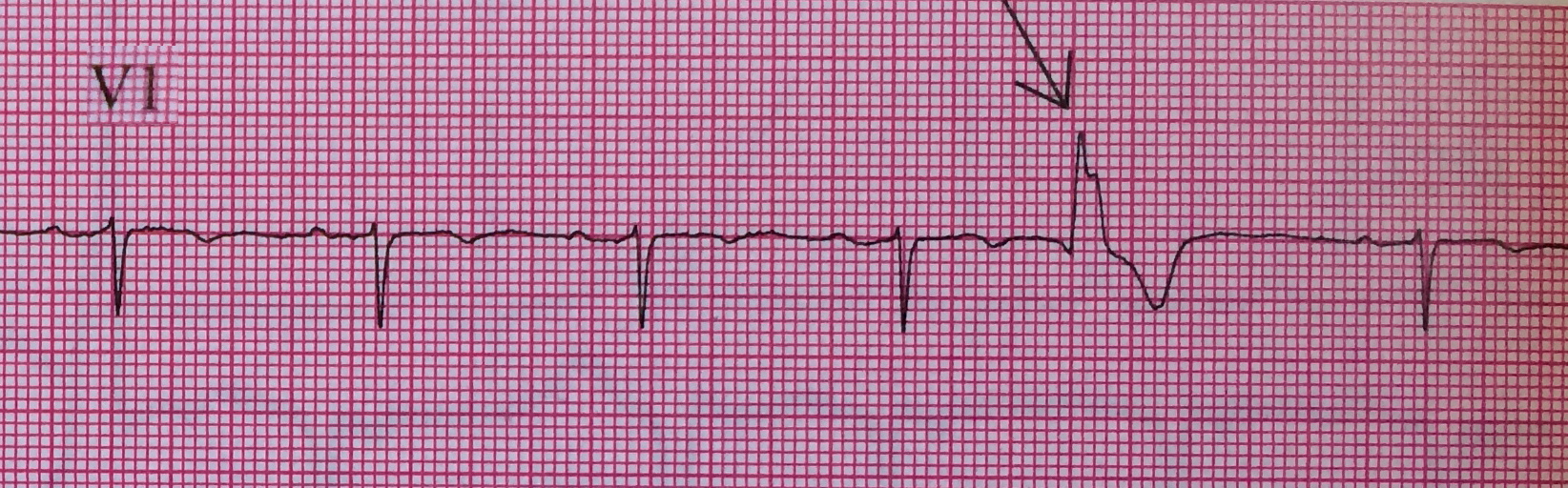
Left Ventricular premature beats are more often associated with heart disease and may precipitate ventricular fibrillation, whereas right ventricular premature beats are commonly seen in individuals with normal hearts.
Want more emergency cardiology pearls? Follow me @alifarzadmd
Wagner, Galen. Chapter 15 - Premature Beats. Marriott's Practical Electrocardiography, 12th Edition. 2013
