Category: Pharmacology & Therapeutics
Keywords: Cephalosporin,penicillin,anaphylaxis,urticaria,cross sensitivity (PubMed Search)
Posted: 11/7/2013 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
When patients with severe allergies to penicillin (urticarial, bronchospasm, anaphylaxis, angioedema) are excluded, the cross reactivity to cephalosporins is very low (approximately 0.1%)
The reaction is related to structures in the side chain, not the cyclical structure as thought in the past.
There are several cephalosporins with IDENTICAL side chains that should not be given to patients with allergies to specific penicillins, namely:
The Medical Letter on Drugs and Therapeutics • December 24, 2012 (Issue 1406) p. 101.
Category: International EM
Keywords: MERS-CoV, Viral Illness, Respiratory (PubMed Search)
Posted: 11/6/2013 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation:
A 56y/o man with diabetes presents with fever, cough, and diarrhea x 2 days.
V/S: T:38.7 BP:165/88 P: 105 R:24 O2 sat:91% on room air
CXR: left lower lobe infiltrate.
On further history you learn he has just returned from visiting family in Saudi Arabia 7 days ago. While there, he visited a cousin that was ill.
Clinical Question:
Should this patient be isolated for Middle Eastern Respiratory Syndrome – Corona Virus (MERS-CoV)?
Answer:
Yes, there are 150 cases to date and 64 have died. None confirmed in the US yet but 6 confirmed in Europe.
Patients who should be isolated in an airborne iso room with N95 mask use (similar to TB) are:
Patients with fever + pneumonia/ARDS AND one of the following:
Bottom Line:
In patients with febrile respiratory illness requiring hospitalization and recent travel to the Arabian Peninsula: isolate for MERS-CoV and contact the health department.
University of Maryland Section of Global Emergency Health
Author: Jenny Reifel Saltzberg
Assiri A, et al. Epidemiological, demographic, and clinical characteristics of 47 cases of Middle East respiratory syndrome coronavirus disease from Saudi Arabia: a descriptive study. Lancet Infect Dis. 2013 Sep;13(9):752-61.
Category: Critical Care
Keywords: Mechanical ventilation, Critical Care, Intubation (PubMed Search)
Posted: 10/29/2013 by John Greenwood, MD
(Updated: 11/5/2013)
Click here to contact John Greenwood, MD
Ineffective triggering is the most common type of ventilator dyssynchrony. The differential diagnosis includes:
Auto peep is the most common cause of ineffective triggering and will often occur as a patient cannot create enough inspiratory force to overcome their own intrinsic peep (PEEPi). Patients who are severely tachypnic or those with obstructive lung disease are at high risk for auto peep (not enough time to exhale).
Ineffective triggering can also occur if the patient cannot create enough of a negative inspiratory force to trigger the vent to deliver a positive pressure breath. Prolonged period of mechanical ventilation, over sedation, high cervical spine injuries, or diaphragmatic weakness are common causes.
Lastly, improper trigger sensitivities may make it difficulty for the ventilator to sense when the patient is attempting to take a spontaneous breath.
For an example of a patient with ineffective triggering, check out: http://marylandccproject.org/2013/10/28/vent-problems1/
Category: Visual Diagnosis
Posted: 11/4/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
This week's visual pearl reviews the structures of the heart when being viewed in a parasternal long-axis view. What do the labels correspond to in the clip below (note: "E" and "F" are valves) and do you see any obvious abnormalities?
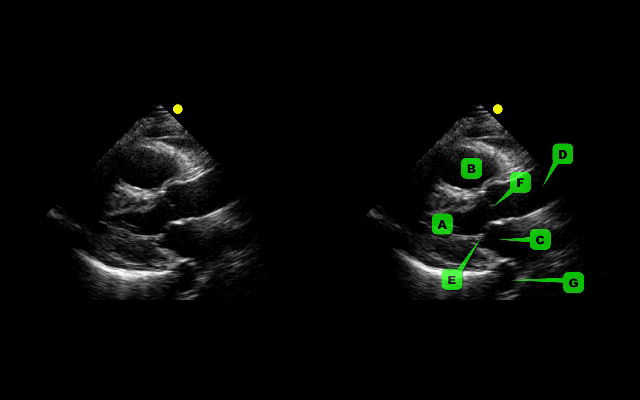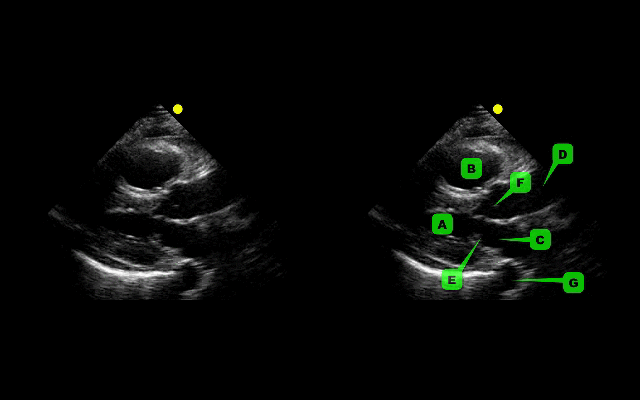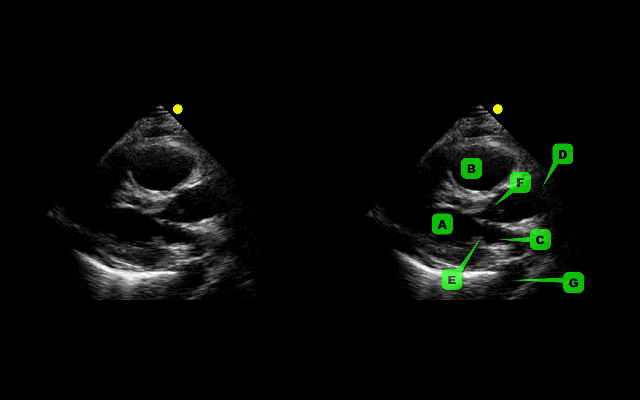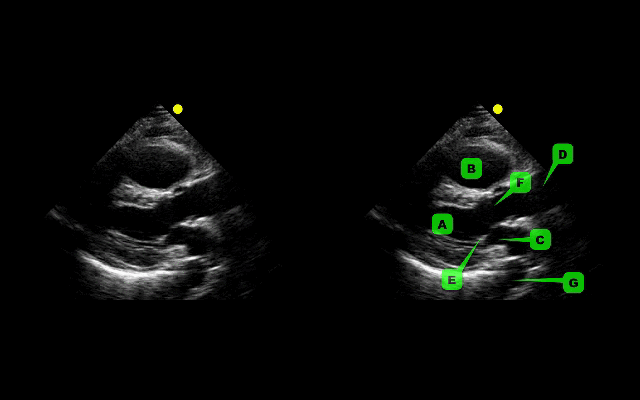
The parasternal long-axis is obtained by scanning to the left (patient's left) of the sternum through the 2nd-5th intercostal space. Click here for a tutorial on the technique.
Answer to Bonus Question: Dilation of the RVOT
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 11/3/2013 by Semhar Tewelde, MD
(Updated: 11/16/2013)
Click here to contact Semhar Tewelde, MD
Secondary Prevention in AMI
Just as aspirin is pivotal in the treatment of acute coronary syndrome, medications such as beta-blocker, statins, and angiotensin-converting enzyme inhibitors have been proven to be essential in secondary prevention of AMI.
Patients after AMI are typically discharged on appropriate secondary prevention medications; however the prescribed doses are often far below the proven efficacy based on clinical trials.
A review of 6,748 patients from 31 hospitals enrolled in 2 U.S. registries (2003 to 2008) illustrated that only 1 in 3 patients were prescribed these medications at goal doses.
Of patients not discharged on goal doses, up-titration during follow-up occurred infrequently ~25%.
Optimal medication dosing and appropriate titration is integral to prevention of further morbidity and mortality.
Arnold S, Spertus J, Masoudi F, et al. Beyond Medication Prescription as Performace Measure: Optimal Secondary Prevention Dosing After Acute Myocardial Infarction. JACC Nov 5, 2013 Vol 62:19;1791-1801
Category: Pharmacology & Therapeutics
Keywords: contrast-induced nephropathy, n-acetylcysteine, NAC (PubMed Search)
Posted: 10/31/2013 by Bryan Hayes, PharmD
(Updated: 11/2/2013)
Click here to contact Bryan Hayes, PharmD
A recent meta-analysis has called into question whether contrast-induced AKI even occurs after an IV dye load for radiologic imaging. [1] This conclusion is most certainly up for debate.
Irrespective of that conclusion, prevention of contrast-induced nephropathy is still important. Is there any benefit to using N-acetylcysteine over normal saline in the ED? Probably not according to a new study. [2]
Conclusions
Follow me on Twitter (@PharmERToxGuy)
Category: Pediatrics
Keywords: cough, upper respiratory infection, children, honey (PubMed Search)
Posted: 11/1/2013 by Danielle Devereaux, MD
Click here to contact Danielle Devereaux, MD
How many times have you been frustrated in the peds ED when you have a child with a URI that has a significant night time cough and you feel like you have nothing to offer them for symptom control? The parent is frustrated because the child is not sleeping which means they are not sleeping and they are looking at you for help. We all know that OTC cough and cold medications are not helpful and may be harmful in children <2 yrs old and should be used with caution in children <6 yrs old. So what can you do? You can recommend a course of HONEY at night. Of course this does not apply to children < 1 yr who are at increased risk of botulism. A recent double-blind placebo-controlled trial published in Pediatrics in 2012 demonstrated reduced night time cough and subjective improved sleep quality in children age 1-5 who were given honey compared to placebo. This study supports previous less rigorous publications that found honey was an effective remedy on cough in children. Mechanism for honey's beneficial effect on cough is unknown but possibly related to close anatomic relationship between sensory nerve fibers that initiate cough and gustatory nerve fibers that taste sweetness. Of note, a recently published survey in Pediatric Emergency Care revealed that 2/3 of parents were unaware of the FDA guidelines regarding OTC cough and cold remedies in children! After you recommend HONEY for night time cough, take an extra minute and educate your parents about the potential dangers of cough and cold medicines in small children!
Cohen A, Rozen J, Kristal H, et al. Effect of honey on nocturnal cough and sleep quality: a double-blind, randomized, placebo-controlled study. Pediatrics. 2012; 130(2): 465-471.
Varney SM, et al. Pediatr Emerg Care. 2012; 28(9): 883-885
Food and Drug Administration. Using Over-The-Counter Cough and Cold Products in Children. Available at http://www.fda.gov/ForConsumers/ConsumerUpdates/ucm048515.htm
Category: Toxicology
Keywords: glycyrrhizic acid, licorice (PubMed Search)
Posted: 10/31/2013 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
You have a treat bag full of candy, which one can cause hypertension, hyopkalemia, metabolic alkalosis, rhabdomyolysis, low renin activity, thrombocytopenia and hypoaldosteronism. (scroll down for answer)
Licorice syrup or licorice extract contains glycyrrhizic acid which has a mineralcorticoid-like effect and can cause of all of the effects. Don't worry, Twizzlers and other usual licorice candies do not have true licorice extract in them. It is found in herbal remedies and some "natural" candies and licorice flavored cigars. Don't pick the licorice !
Category: International EM
Keywords: international, EPTB, extrapulmonary, tuberculosis, ultrasound (PubMed Search)
Posted: 10/30/2013 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation: 28 year old woman from South Africa presents with 5 days of body weakness, nausea, vomiting and cough. BP 86/38, HR 142, RR 36, Temp 101.4 (oral) Sats 96% on RA. PMH: HIV+ last CD4=33, on HAART, history of pulmonary TB which was treated 2 years ago.
Clinical Question: The CT scanner, Xray and labs are down. What work-up can you do to best manage this patient?
Answer: The FASH Exam (Focused Assessment with Sonography for TB-HIV)
Technique: 6 probe positions--Similar to the FAST exam but with additional evaluation of the liver, the aorta, the spleen, as well as evaluation for pleural effusions over the diaphragm.
Evaluate for extrapulmonary TB (EPTB):
-Pericardial/Pleural effusion and ascites
-Periportal/para-aortic lymph nodes
-Focal liver and spleen lesions
(Go to http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3554543/ to view images of probe position.)
Bottom Line: The FASH exam can be taught to physicians with limited to no ultrasound experience. If there is concern for EPTB in an undifferentiated hypotensive patient, the FASH exam can performed in the emergency setting and treatment can be started.
University of Maryland Section of Global Emergency Health
Author: Laura Diegelmann, MD RDMS
Category: Critical Care
Posted: 10/29/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
The pregnant patient normally has increased cardiac output and minute ventilation by the third trimester. Despite this increase, however, these patients have little cardiopulmonary reserve should they become critically-ill.
Remember the mnemonic T.O.L.D.D. for simple tips that should be done for the pregnant patient who presents critically-ill or with the potential for critical illness:
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 10/27/2013 by Haney Mallemat, MD
(Updated: 10/28/2013)
Click here to contact Haney Mallemat, MD
15 year-old right-hand dominant male received a direct blow to the right arm with a hockey stick. What’s the diagnosis?
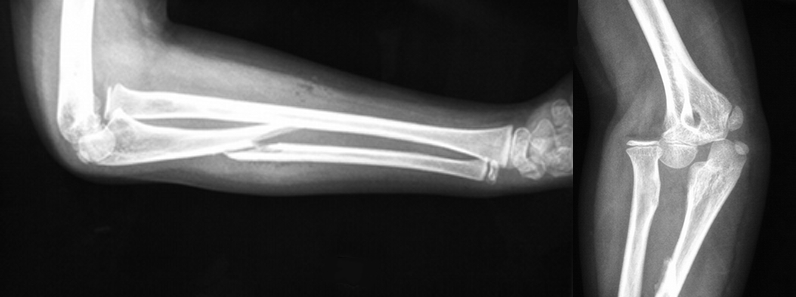
Monteggia Fracture
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Keywords: AV Block (PubMed Search)
Posted: 10/27/2013 by Ali Farzad, MD
(Updated: 3/10/2014)
Click here to contact Ali Farzad, MD
First-degree atrioventricular (AV) block is defined as an abnormally prolonged PR-interval >200ms. Although traditionally considered to be a benign clinical entity, not all first degree AV blocks are treated the same.
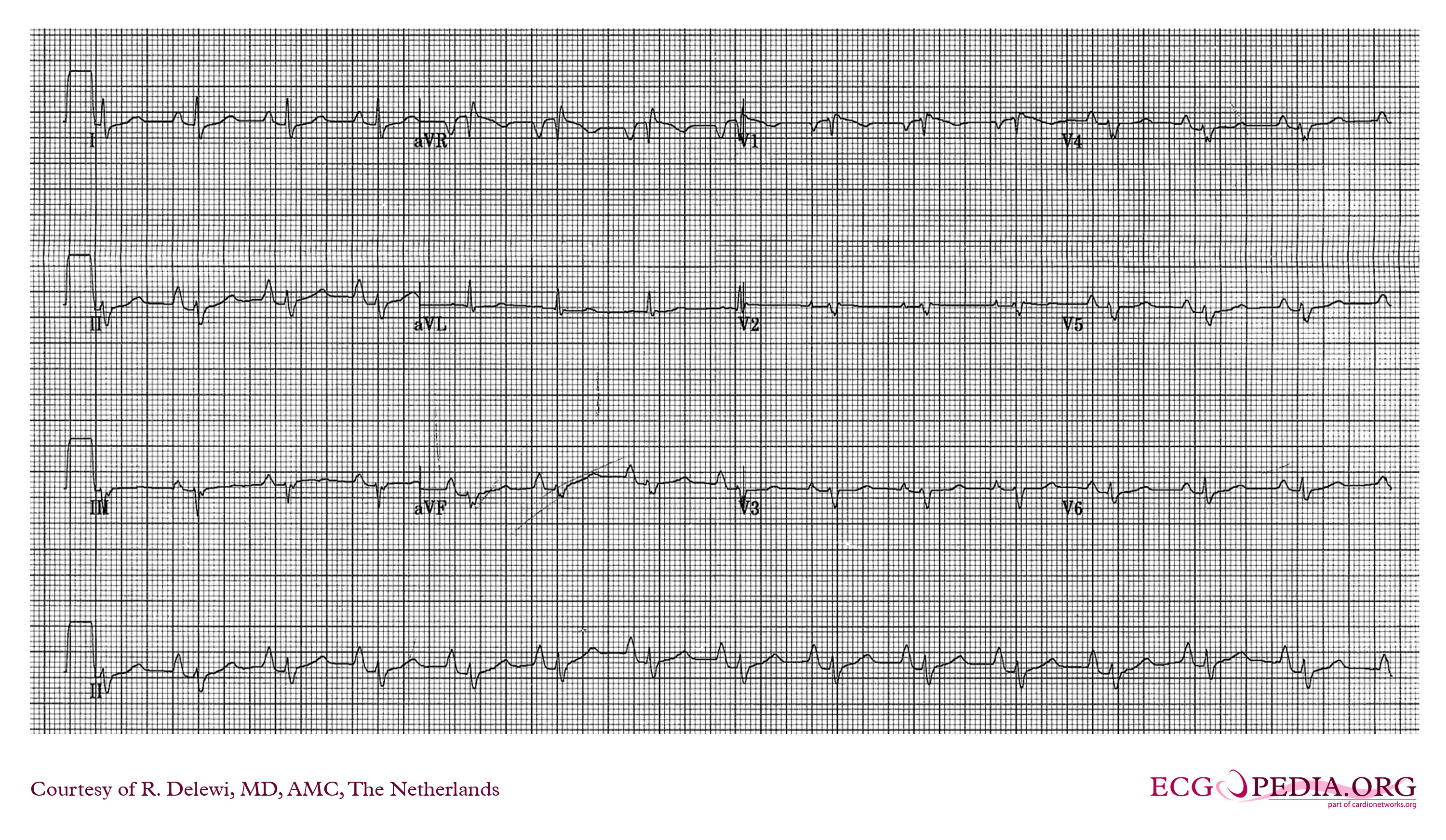
Markedly prolonged PR-intervals (PR >300ms) can cause symptoms and hemodynamic compromise due to inadequate timing of atrial and ventricular contractions. Consider the following ECG from a 32 YOF with intermittent episodes of syncope and dizziness…
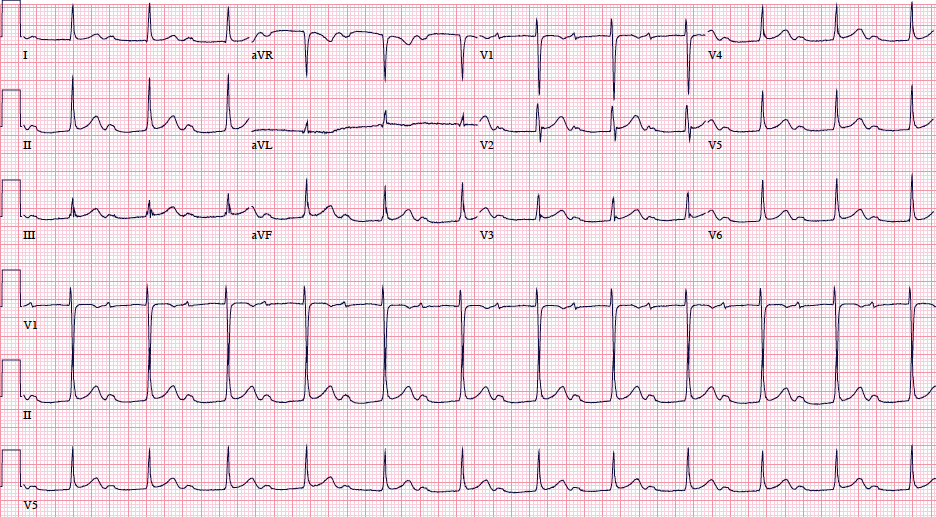
There is marked first degree AV block (PR=434 ms). When the PR-interval gets too long, AV dyssynchrony compromises ventricular filling and decreases cardiac output, similar to the so-called pacemaker syndrome.
Current ACC/AHA guidelines state that permanent pacemaker implantation is reasonable for marked first degree AV block with hemodynamic compromise or symptoms similar to those of pacemaker syndrome. (Class IIa, Level of Evidence B). The guidelines caution that pacemakers are not indicated in asymptomatic patients with isolated first degree AV block.
Want more emergency cardiology pearls? Follow me @alifarzadmd
Special thanks to Dr. Brandon Cole for submitting the ECG
References / Further Reading (Attached)
First-Degree AV Block-An Entirely Benign Finding or a Potentially Curable Cause of Cardiac Disease? Annals of Noninvasive Electrocardiology.2013;18(3):215–224. doi:10.1111/anec.12062.
ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2008;117(21):e350–e408. doi:10.1161/CIRCUALTIONAHA.108.189742.
Category: Orthopedics
Keywords: gluteus, trendelenberg test, hip pain (PubMed Search)
Posted: 10/26/2013 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
Lateral hip pain
Findings of weakness and/or pain while testing hip abduction may point to gluteus medius muscle dysfunction with associated with greater trochanteric pain syndrome.
The Trendelenburg test may help. The patient stands on the affected leg. A negative test result occurs when the pelvis rises on the opposite side. A positive test result occurs when the pelvis on the opposite side drops and indicates a weak or painful gluteus medius muscle.
http://www.youtube.com/watch?v=TY-G4ErruUA
Category: Toxicology
Keywords: promethazine (PubMed Search)
Posted: 10/25/2013 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Yesterday's pearl generated several questions that I thought were worth answering briefly:
1) Why give it IM? Absorption rate is faster than SQ infiltration though theoretically could still cause necrosis
2) Is it only infilitration? Gangrene has occurred with inadvertent intra-arterial injection, SQ infiltration and even regular IV administration
3) Mechanism? Appears to be the drug and not diluent, diluting down the concentration as well as decreasing dose appears to help if you are going to give it IV
Here is a website if you wish to read more details:
https://www.ismp.org/newsletters/acutecare/articles/20060810.asp
Category: Toxicology
Keywords: Promethazine (PubMed Search)
Posted: 10/24/2013 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
If you are still using IV Phenergan, you need to be aware of the necrotic effect that occurs if it infiltrates. EDs have even removed it from their drug dispensing machines. It appears to be the drug and not the diluent. Mechanism is not completely understood. Below is a picture the plaintiff attorney will use about this well know adverse effect. If so many alternatives for IV antiemetic it is wise to reconsider IV phenergan.
Category: International EM
Keywords: Pediatrics, Disaster (PubMed Search)
Posted: 10/23/2013 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Area of the world affected:
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Emilie J.B. Calvello, MD, MPH
Rothstein, D. Pediatric Care in Disasters. Pediatrics. 2013, 132;25.
Category: Critical Care
Keywords: TRALI, TACO, Transfusion, acute lung injury (PubMed Search)
Posted: 10/22/2013 by Feras Khan, MD
Click here to contact Feras Khan, MD
Background
Definition
Pathogenesis
Two-hit hypothesis: first hit is underlying patient factors causing adherence of neutrophils to the pulmonary endothelium; second hit is caused by mediators in the blood transfusion that activate the neutrophils and endothelial cells.
Differential
Can be confused or overlap with TACO or transfusion-associated volume/circulatory overload, which presents similarly but has evidence of increased BNP, CVP, pulmonary wedge pressure, and left sided heart pressures. Patients with TACO tend to improve with diuretic treatment
Supportive tests
Treatment
Lancet. 2013 Sep 14;382(9896):984-94. doi: 10.1016/S0140-6736(12)62197-7. Epub 2013 May 1.
Category: Visual Diagnosis
Posted: 10/20/2013 by Haney Mallemat, MD
(Updated: 12/5/2023)
Click here to contact Haney Mallemat, MD
55 year-old male presents with chest pain. You take a look at his cardiac function with ultrasound and here's the patient's apical four-chamber view. What's in his right ventricle and why would it be there?
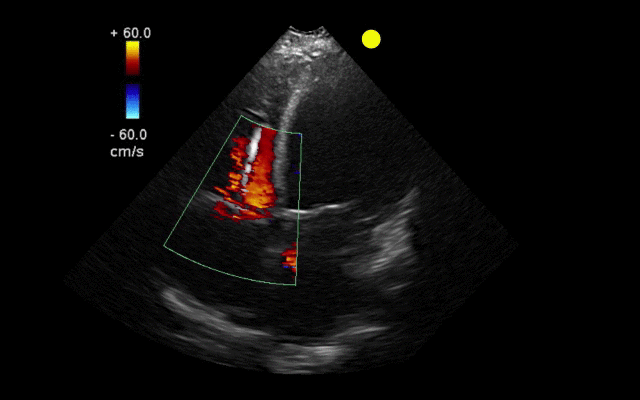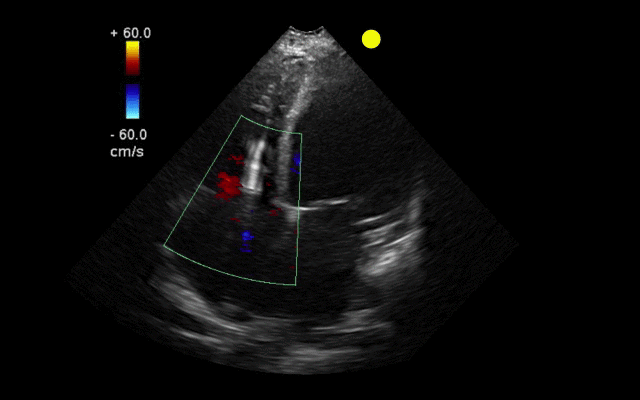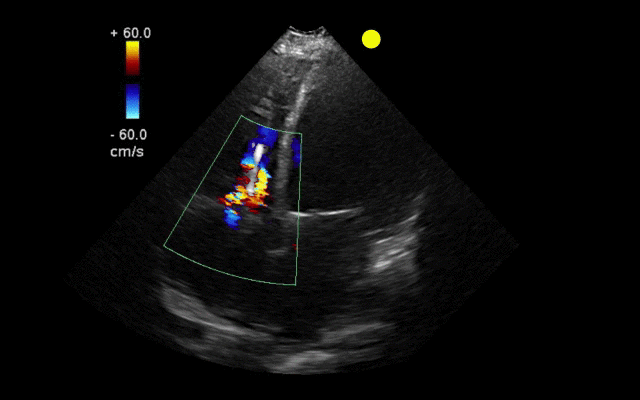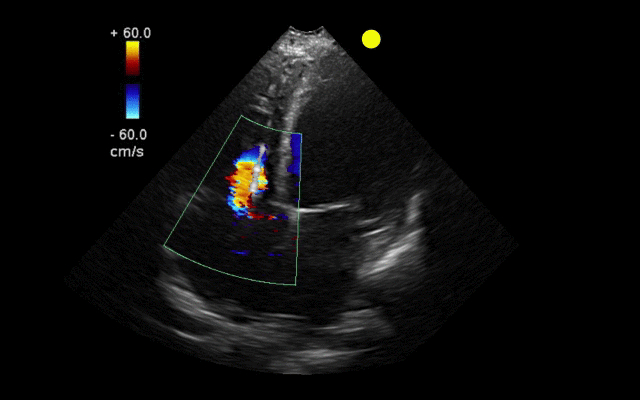
AICD
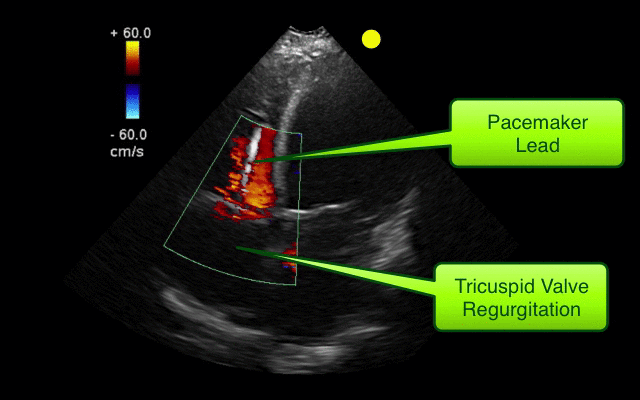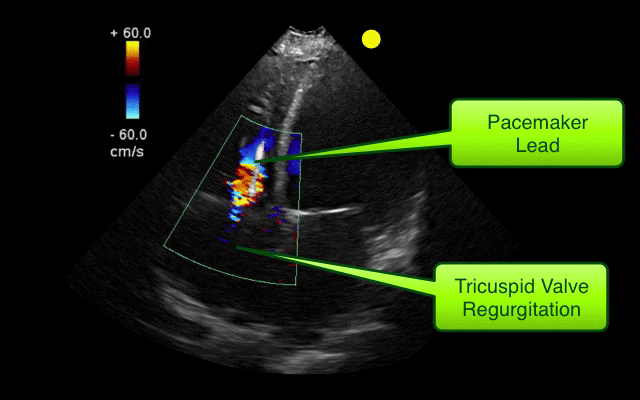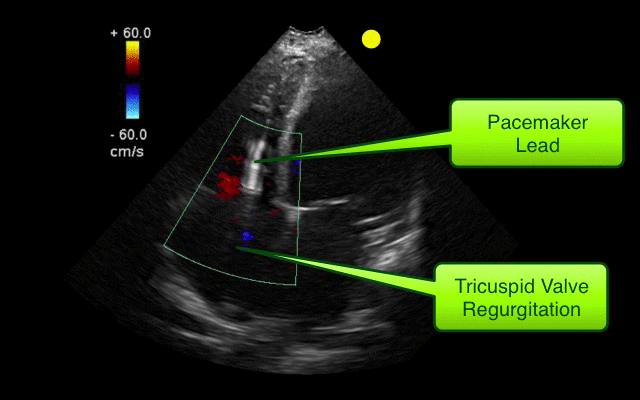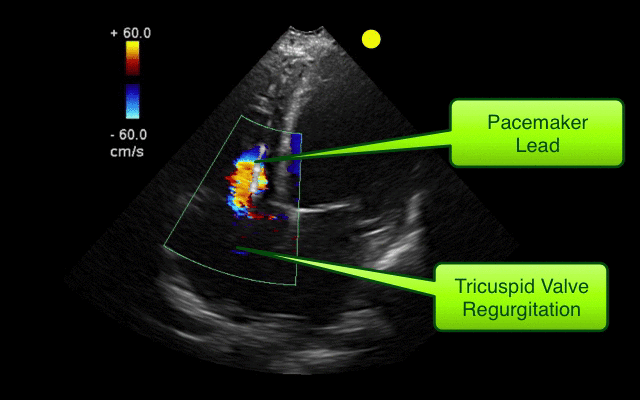
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 10/20/2013 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Ebstein's Anomaly
Osiro S, Tiwari K, Mathenge N, et al. When Lithum Hurts: A Look at Ebstein Anomaly. Cardiology in Review. Oct 2013, Vol 21(5); pgs 257-263.
Category: Pediatrics
Keywords: skull fracture (PubMed Search)
Posted: 10/18/2013 by Jenny Guyther, MD
(Updated: 5/4/2026)
Click here to contact Jenny Guyther, MD
Pediatric patients with an isolated skull fracture and normal neurological exam have a low risk of neurosurgical intervention and outpatient follow up may be appropriate (assuming no suspicion of abuse and a reliable family). In a study published in 2011, a retrospective review over a 5 year period at a level 1 trauma center showed that 1 out of 171 admitted patients with isolated skull fractures developed vomiting. This patient had a follow up CT showing a small extra-axial hematoma that did not require intervention. 58 patients were discharged from the ED within 4 hours.
You can also check out another recent article published in Annals of Emergency Medicine on the same topic this month!
Rollins et al. Neurologically intact children with an isolated skull fracture may be safely discharged after brief observation. Journal of Pediatric Surgery. Volume 26. Issue 7. 2011.
Mannix et al. Skull Fractures: Trends in Management in US Pediatric Emergency Departments. Annals of Emergency Medicine. Volume 64. Issue 4. 2013.
