Category: Visual Diagnosis
Posted: 4/8/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
64 year-old female presents with chest pain following an argument with her husband. Her echocardiogram (apical four-chamber view) and ECG are shown. Her initial troponin is 10. What's the diagnosis?
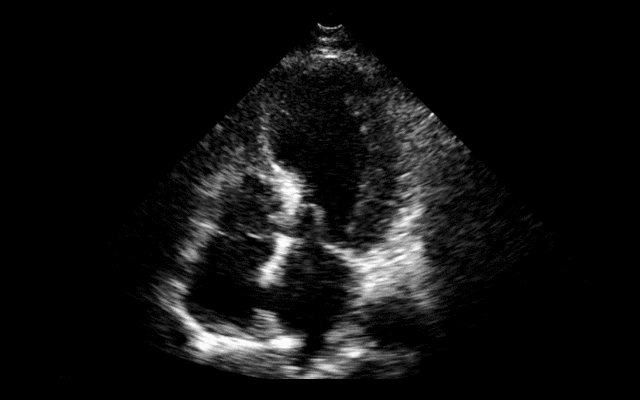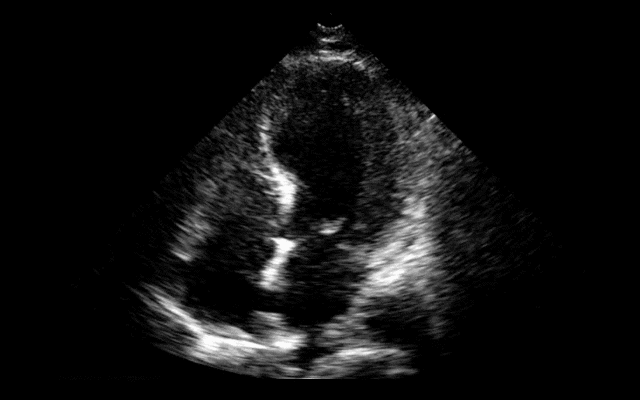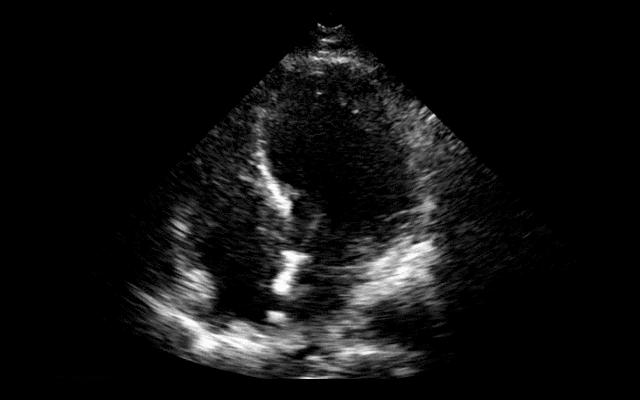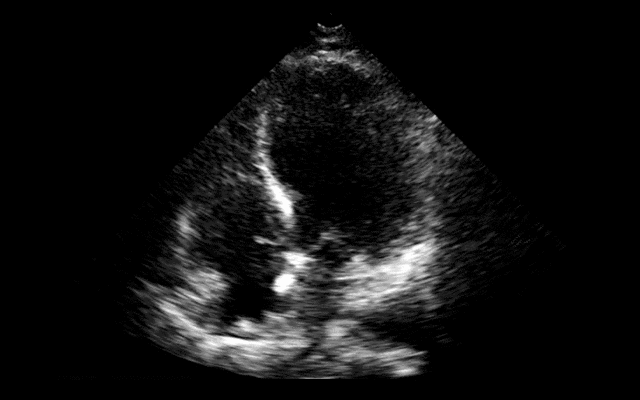
Answer: Takotsubo (a.k.a Stress) cardiomyopathy (TC)
TC is left ventricular dysfunction (hypokinesia, akinesia, or dyskinesia) secondary to catecholamine surge (e.g., physical / emotional stress) causing myocardial stunning; it is not due to acute coronary occlusion. TC disproportionately affects postmenopausal women, occurring in up to 90% of cases.
Patients often present with chest pain or dyspnea; 85% of patients will have an abnormal ECG (e.g., ST elevation or T wave inversions), making diagnosis difficult to differentiate between TC and acute coronary syndrome (ACS). TC has been found to be the diagnosis in 2.5% of patients initially worked up for ACS.
Diagnosis can usually be confirmed with echocardiography but cardiac catheterization (with ventriculogram) is sometimes performed if ACS is strongly suspected. Catheterization demonstrates normal coronary arteries with an abnormal ventriculogram (click for video), typically in mid-to apical portion of the left ventricle.
Treatment is symptomatic and similar to congestive heart failure (e.g., diuretics, beta-blockers, etc.); 95% of patients have full recovery within one month.
Refer to this prior PEARL by Dr. Tewelde for additional information
Reference
T Pilgrima, T Wyss, Takotsubo cardiomyopathy or transient left ventricular apical ballooning syndrome: A systematic review, Int J Card 2008 Mar 14;124(3):283-92
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 4/7/2013 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Weiss P, et al. Pediatric vasculitis. The Pediatric clinics of North America. April 2012:59;2:407-423.
Category: Critical Care
Keywords: Resuscitation, ventricular fibrillation, cardiac arrest, emergency, cardiology (PubMed Search)
Posted: 4/6/2013 by Ben Lawner, MS, DO
(Updated: 5/4/2026)
Click here to contact Ben Lawner, MS, DO
Recent advances in resuscitation science have enabled emergency physicians to identify factors associated with good neurologic and survival outcomes. Cases of persistent ventricular dysrhythmia (VF or VT) present a particular challenge to the critical care provider. The evidence base for interventions in shock refractory ventricular VF mainly consists of case reports and retrospective trials, but such interventions may be worth considering in these difficult resuscitation situations:
1. Double sequential defibrillation
-For shock-refractory VF, 2 sets of pads are placed (anterior/posterior and on the anterior chest wall). Shocks are delivered as "closely as possible."1,2
2. Sympathetic blockade in prolonged VF arrest
-"Eletrical storm," or incessant v-fib, can complicate some arrests in the setting of VF. An esmolol bolus and infusion may be associated with improved survival.3 Left stellate ganglion blockade has been identified as a potential treatment for medication resistant VF.4
3. Don't forget about magnesium!
-May terminate VF due to a prolonged QT interval
4. Invasive strategies
-Though resource intensive, there is limited experience with intra-arrest PCI and extracorporeal membrane oxygenation. Preestablished protocols are key to selecting patients who may benefit from intra-arrest PCI and/or ECMO. 5
5. Utilization of mechanical CPR devices
-Though mechanical CPR devices were not officially endorsed by the AHA/ECC 2010 guidelines, there's little question that mechanical compression devices address the complication of provider fatigue during ongoing resuscitation.
Category: Pharmacology & Therapeutics
Keywords: alteplase, tPA, dabigatran, anticoagulant, apixaban, rivaroxaban (PubMed Search)
Posted: 4/3/2013 by Bryan Hayes, PharmD
(Updated: 4/5/2013)
Click here to contact Bryan Hayes, PharmD
A new recommendation in the 2013 Ischemic Stroke Guidelines provides guidance on what to do in patients taking new oral anticoagulants who are deemed eligible for IV fibrinolysis. Here is what the guidelines say:
Until further data are available, a history consistent with recent use of new oral anticoagulants generally precludes use of IV tPA.
Jauch EC, et al. Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2013;44(3):870-947. PMID 23370205
Follow me on Twitter (@PharmERToxGuy)
Category: Pediatrics
Keywords: Conjunctivitis (PubMed Search)
Posted: 4/5/2013 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Children frequently present with "pink eye" to the ED. When they do, parents often expect antibiotics. How many of these kids actually need them? Previous studies have shown approximately 54% of acute conjunctivitis was bacterial, but antibiotics were prescribed in 80-95% of cases.
A prospective study in a suburban children's hospital published in 2007, showed that 87% of the cases during the study period were bacterial. The most common type of bacteria was nontypeable H. influenza followed by S. pneumoniae.
Topical antibiotic treatment has been shown to improve remission rates by 6-10 days.
Patel et al. Clinical Features of Bacterial Conjunctivitis in Children. Academic Emergency Medicine 2007; 14:1-5.
Category: Pharmacology & Therapeutics
Keywords: Status epilepticus, Keppra, seizures, valproic acid, levetiracetam (PubMed Search)
Posted: 4/4/2013 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Trinka E. What is the evidence to use new intravenous AED in status epilepticus? Epilepsia 2011 52(Suppl 8):35-8.
Zelano J, Kumlien E. Levetiracetam as alternative stage two antiepileptic drug in status epilepticus: A systematic review. Seizure 2012. 21:233-6.
Category: International EM
Posted: 4/3/2013 by Walid Hammad, MD, MBChB
Click here to contact Walid Hammad, MD, MBChB
Spring is in the air... and so is rotavirus.
Area of the world affected:
· Diarrheal illnesses were responsible for 1.6 million deaths for children under 5 globally in 2002.
· This number has improved over the years, in part due to oral rehydration salts (ORS) which were developed for cholera.
Relevance to the US physician:
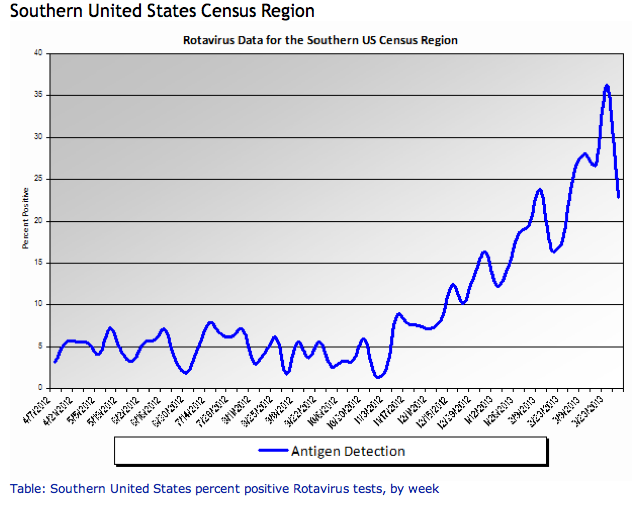
http://www.cdc.gov/surveillance/nrevss/rotavirus/region.html#top
· ORS are also important for rotavirus treatment and uncomplicated gastroenteritis in children and adults.
· Commercially prepared solutions have different concentrations of ingredients, but all will work as better treatment and rehydration than common household products like sports drinks and juice.
Bottom line:
Consider ORS in patients with uncomplicated acute gastroenteritis.
University of Maryland Section of Global Emergency Health
Author: Jennifer Reifel Saltzberg, MD, MPH
Atia AN, Buchman AL. Oral rehydration solutions in non-cholera diarrhea: a review. Am J Gastroenterol 2009;104(10):2596-604.
Sentongo, TA. The Use of Oral Rehydration Solutions in Children and Adults. Current Gastroenterology Reports 2004; 6:307–313.
Category: Critical Care
Posted: 4/2/2013 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Hormonal Dysfunction in Neurologic Injury
Vespa PM. Hormonal dysfunction in neurocritical patients. Curr Opin Crit Care 2013; 19:107-12.
Category: Visual Diagnosis
Posted: 4/1/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
What's the Diagnosis?
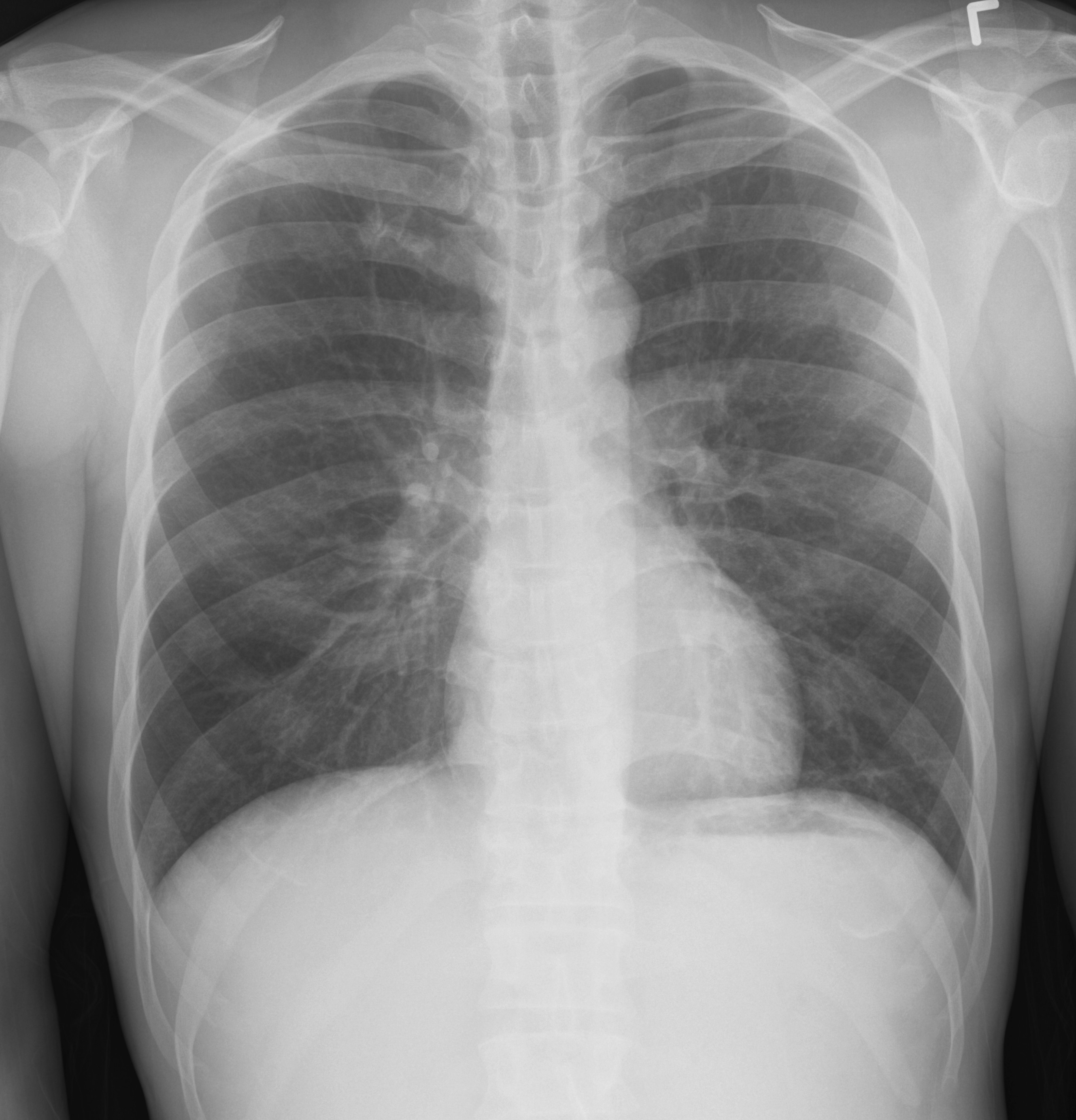
Answer: Normal CXR...April Fool's Day ;)
Our international friends can learn more about April Fool'sDay here
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 3/30/2013 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
Category: Orthopedics
Keywords: Ottawa, Knee, Pittsburgh (PubMed Search)
Posted: 3/30/2013 by Michael Bond, MD
Click here to contact Michael Bond, MD
Knee Pain Injuries are Radiographs needed?
Many people know that the folks in Ottawa have come up with a rule to determine whether radiographs are needed in patients complaining of knee pain. The Ottawa Knee rules that that radiographs are only required for knee injuries with any of the following:
• Age 55 years or older
• isolated tenderness of patella
• tenderness at head of fibula
• inability to flex to 90'
• inability to bear weight both immediately and in the emergency department (4 steps)
Well another group in Pittsburgh have their own set of rules that were recently shown to be more specific with equal sensitivity. The Pittsburgh decision rules state that radiographs are only needed if
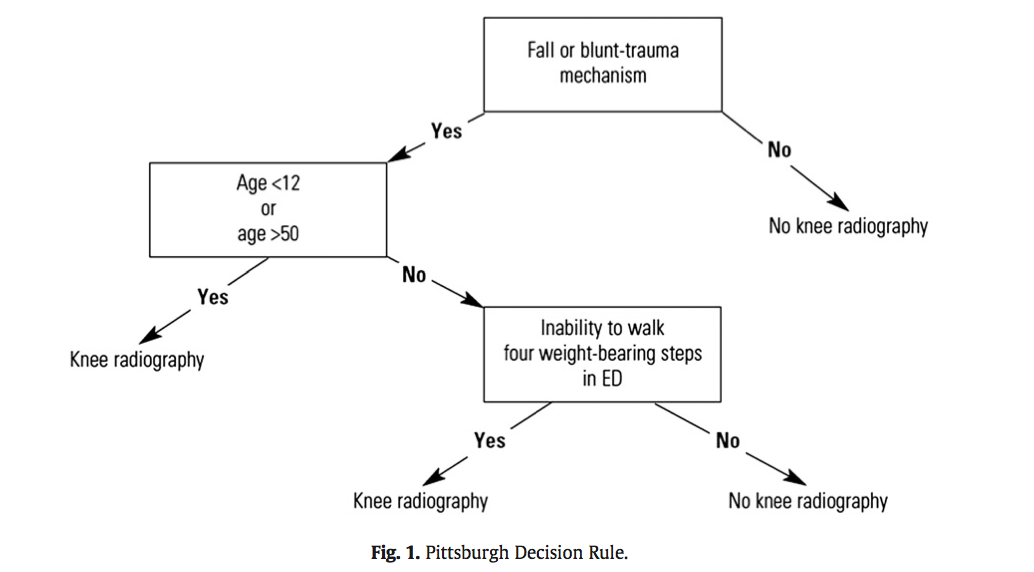
So consider using the Pittsburgh or Ottawa Knee rules the next time you have a patient with knee pain to determine if those radiographs are really needed.
The full article can be found at http://www.ajemjournal.com/article/S0735-6757%2812%2900566-9/abstract
Cheung TC, Tank Y, Breederveld RS, Tuinebreijer WE, de Lange-de Klerk ESM, MD RJD. Diagnostic accuracy and reproducibility of the Ottawa Knee Rule vs the Pittsburgh Decision Rule. Am J Emerg Med. Elsevier Inc; 2013 Feb 1;:1–5.
Category: Pediatrics
Posted: 3/29/2013 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
You have diagnosed an infant or child with pneumonia. How do you decide if they need admission?
The Pediatric Infectious Disease Society and the British Thoracic Society each have guidelines from 2011 to help with this decision.
Category: International EM
Posted: 3/28/2013 by Walid Hammad, MD, MBChB
(Updated: 5/4/2026)
Click here to contact Walid Hammad, MD, MBChB
Background Information:
Combination antiretroviral therapy (cART) reduces HIV-associated morbidities and mortalities but cannot cure infection. Recent literature has suggested that early initiation of cART with primary infection can lead to “functional cure” for HIV infected patients with suppressed viremia and delayed progression to clinical symptoms.
Pertinent Study Design and Conclusions:
- Researchers studied 14 patients whose treatment with combination antiretrovirals began soon after exposure to HIV. The patients' viral loads became undetectable within roughly 3 months, and treatment was interrupted after about 3 years.
- The patients were found to have very low viral loads and stable CD4-cell counts after several years without therapy. The researchers estimate that about 15% of those treated early could achieve similar results.
Bottom Line:
Have a high suspicion of acute anti-retroviral syndrome in the ED (fever, rash, pharyngitis, lymphadenopathy) and test properly (viral load NOT ELISA) to identify patients who may benefit from early, rapid initiation of cART.
University of Maryland Section of Global Emergency Health
Author: Emilie J. B. Calvello, MD, MPH
Sáez-Cirión A, Bacchus C, Hocqueloux L, Avettand-Fenoel V, Girault I, et al. (2013) Post-Treatment HIV-1 Controllers with a Long-Term Virological Remission after the Interruption of Early Initiated Antiretroviral Therapy ANRS VISCONTI Study. PLoS Pathog 9(3): e1003211.
Category: Critical Care
Posted: 3/26/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
There are several reasons why a mechanically ventilated patient may decompensate post-intubation. Immediate action is often needed to reverse the problem, but it can be difficult to remember where to start as the vent alarm is sounding and the patient is decompensating.
Consider using the mnemonic “D.O.P.E.S. like D.O.T.T.S.” to assist you in first diagnosing the problem (D.O.P.E.S.) and then fixing the problem (D.O.T.T.S.). You can view an entire lecture on the Crashing Ventilated Patient here.
Step 1: Could this decompensation be secondary to D.O.P.E.S.?
Step 2: Fix the problem with D.O.T.T.S.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 3/25/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
35 year-old male presents after a motor vehicle crash. No blood seen at the meatus of the penis and a Foley catheter is placed (see photo below). What's the next diagnostic step?
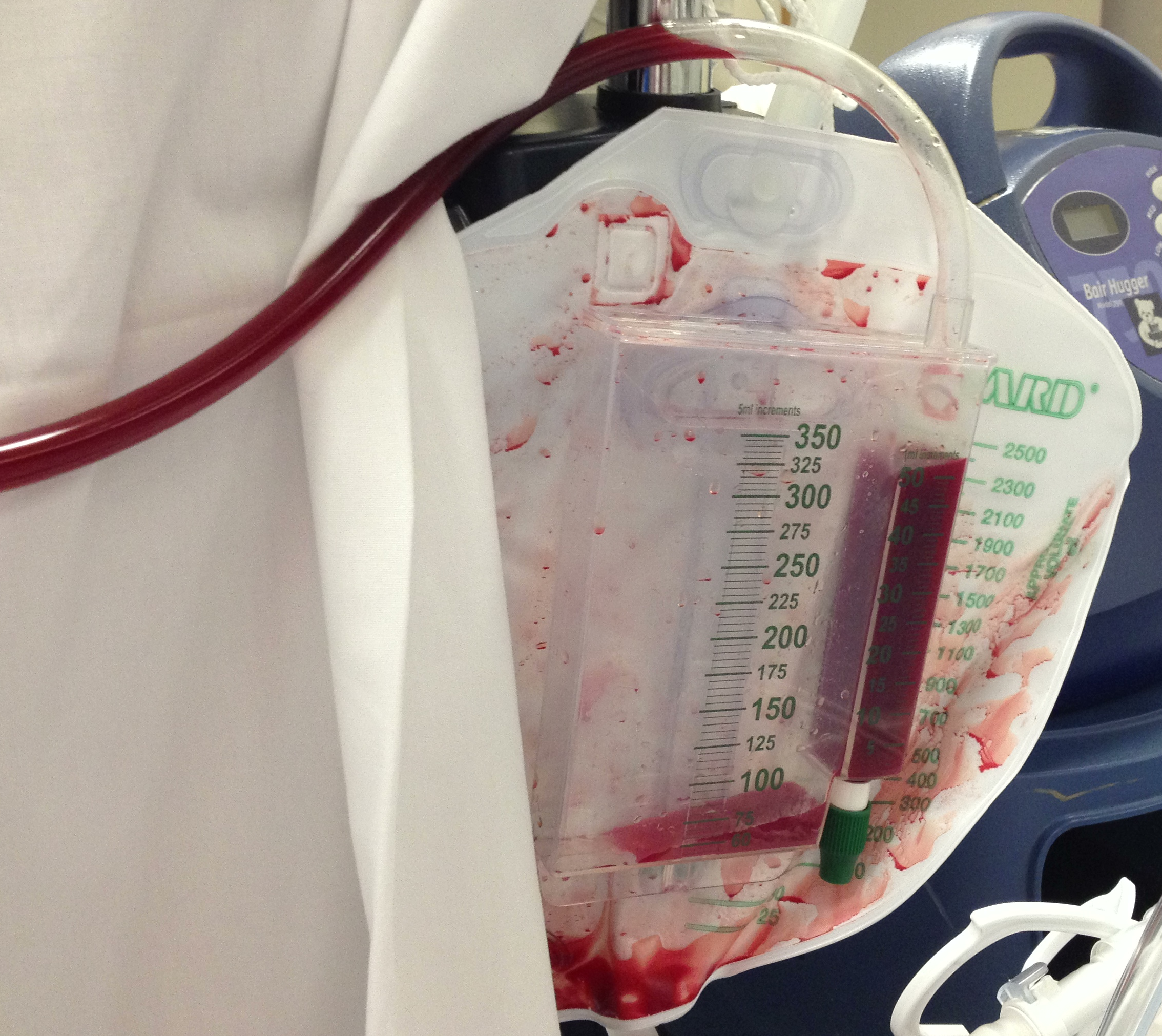
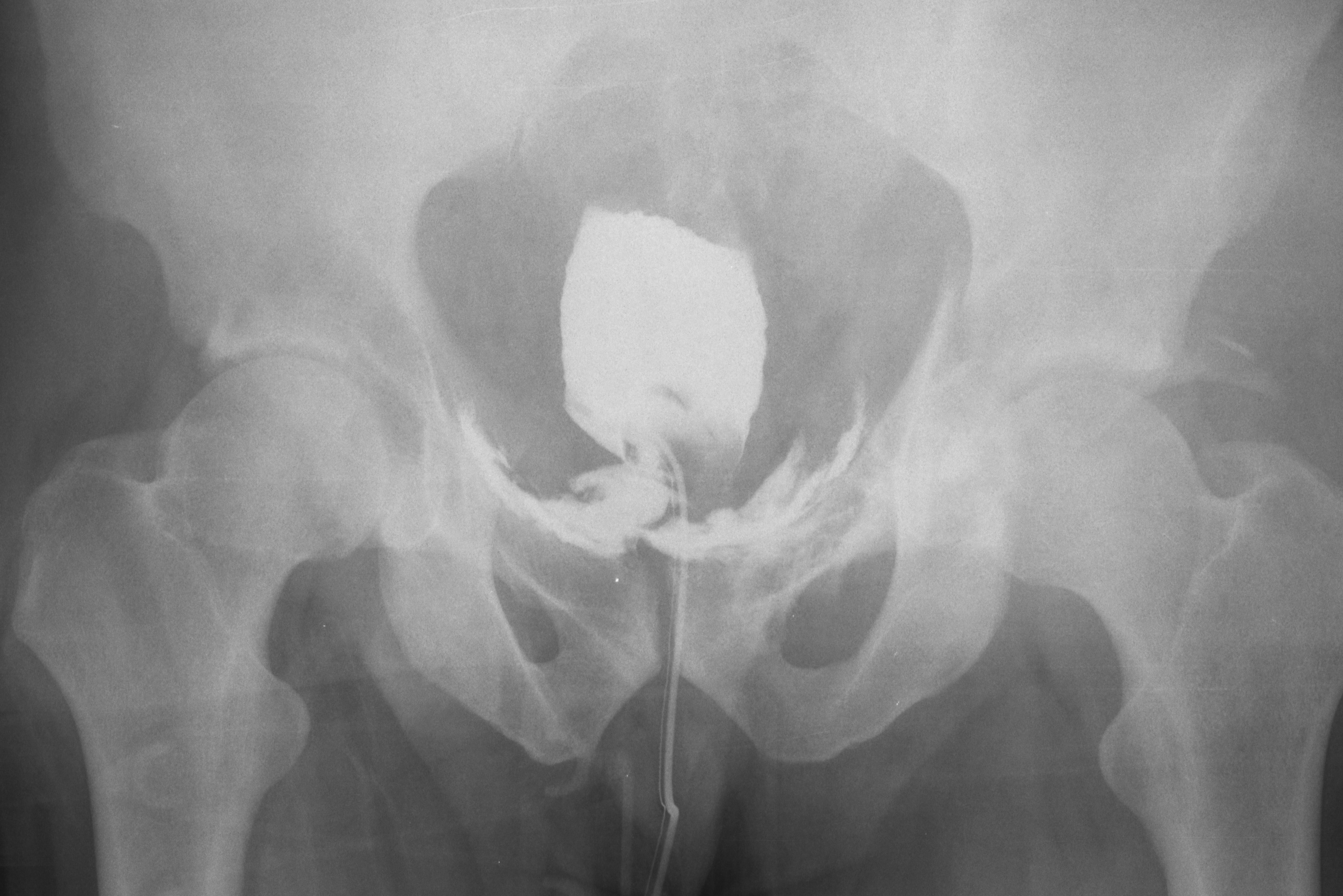
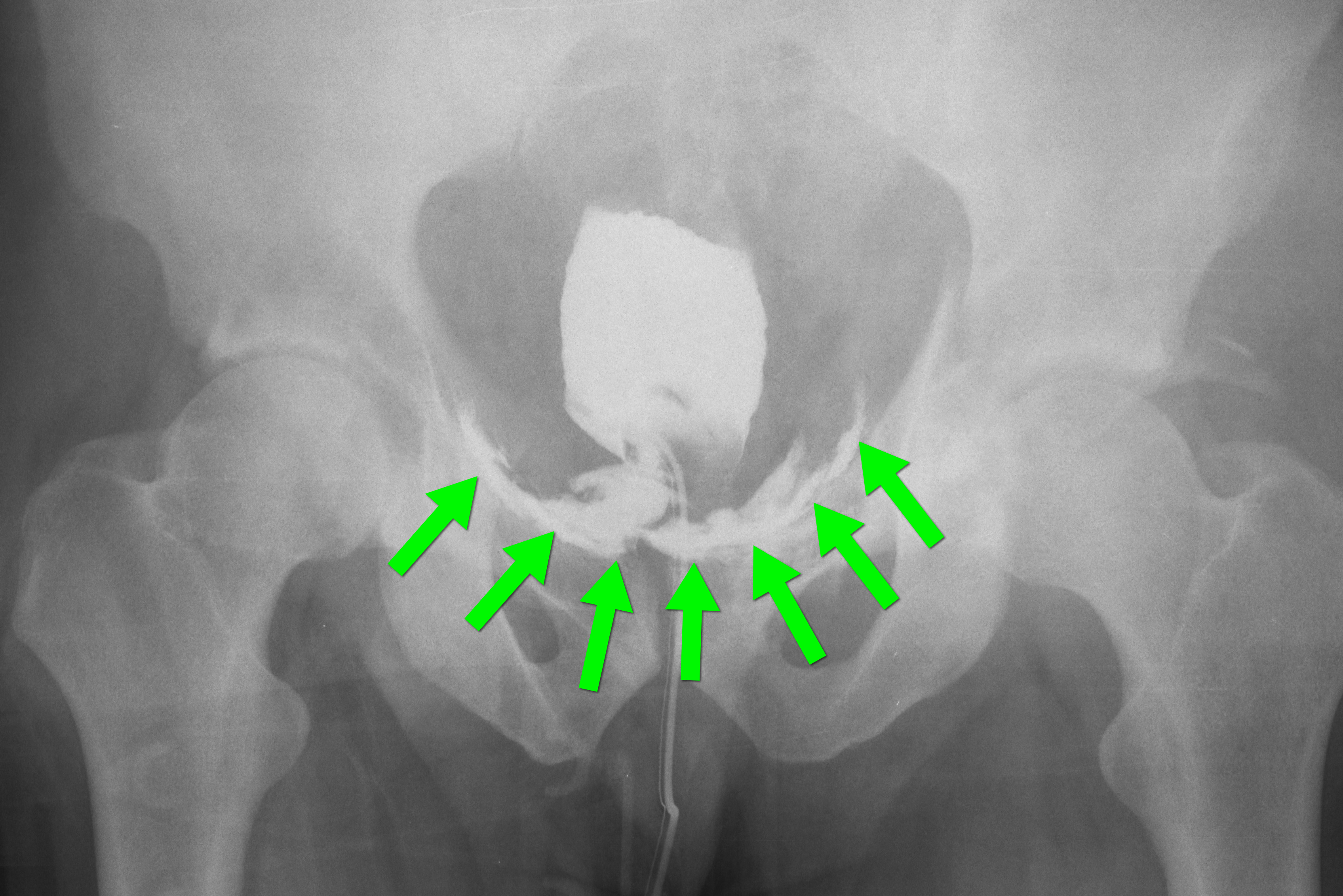
Answer: Retrograde cystogram
Traumatic bladder rupture
Gross or microscopic hematuria (>50 RBCs per high-power field) following blunt trauma requires a retrograde cystogram to evaluate for bladder injury. If blood is present at the meatus, however, urethral injury (not discussed) should be suspected and retrograde urethrogram should be performed before passing a Foley catheter.
A retrograde cystogram is performed by infusing diluted contrast into the bladder (200-400 mL) to gently distend the bladder and allow visualization of potential rupture(s). A CT scan of the abdomen and pelvis is then performed to determine if any contrast has leaked from the bladder; alternatively an AP pelvis can also be used, but is not as sensitive as CT.
Traumatic bladder ruptures are categorized as either intra-peritoneal or extra-peritoneal (note: X-ray below demonstrates extra-peritoneal rupture).
Treatment for bladder rupture:
Prognosis is typically good for either injury.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Keywords: LVH (PubMed Search)
Posted: 3/25/2013 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Okin PM, Roman MJ, Devereux RB, Kligfield P. Electrocardiographic identification of increased left ventricular mass by simple voltage-duration products. J Am Coll Cardiol. 1995 Feb; 25(2):417-23.
Category: Pediatrics
Posted: 3/23/2013 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
In children, it is important to consider the maximum doses of local anesthetics when performing a laceration repair or painful procedure like abscess drainage. If there are multiple lacerations, or large lacerations, it may be possible to exceed those doses if one is not careful.
Max doses of common anesthetics
For example, in a 20 kg child (an average 5-6 year old), the maximum doses would be:
Pearls:
Category: Toxicology
Keywords: dexmedetomidine, cocaine (PubMed Search)
Posted: 3/21/2013 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Cocaine toxicity is characterized by the sympathomimetic toxidrome: tachycardia, hypertension, hyperpyrexia, diaphoresis as well as sodium channel blocking effects that can cause local anesthesia topically, QRS widening and even seizure.
Usual treatment for a cocaine toxic patient is benzodiazepines and cooling. Be wary of end organ damage, trauma and seizures.
There was a recent study that looked at dexmedetomidine to treat the sympathomimetic effects. Placebo-controlled trial used cocaine-addicted volunteer and applied intranasal cocaine. Measuring skin sympathetic nerve activity and skin vascular resistance, this study, unfortunately, showed as the dose increased MAP did not fall further and increased paradoxically in 4 of 12 subjects.
This highlights the incredible physiologic mechanism of catecholamine release from the CNS with cocaine. This mechanism overlaps some with the centrally acting alpha agonist - dexmedetomidine and was shown in the study by Kontak et al.
Kontak AC, Victor RG, Vongpatanasin W.
Hypertension. 2013 Feb;61(2):388-94
Category: International EM
Keywords: novel, coronavirus, International, infectious, SARS, pulmonary (PubMed Search)
Posted: 3/19/2013 by Andrea Tenner, MD
(Updated: 3/25/2013)
Click here to contact Andrea Tenner, MD
General Information:
14 cases of lower respiratory infection caused by a new coronavirus (not the original SARS virus, but with a similar picture) occurred in the past year. Mortality rate of this virus is >50%.
Area of the world affected:
Relevance to the US physician:
Bottom Line:
Consider this infection in patients with a lower respiratory tract infection who have traveled to or had contact with someone who traveled to the above regions in the past 10 days.
ASK ABOUT RECENT TRAVELS IN PATIENTS PRESENTING WITH SYMPTOMS OF SEVERE LOWER RESPIRATORY TRACT INFECTION!
University of Maryland Section of Global Emergency Health
Author: Veronica Pei MD, MPH
cdc.gov/mmwr/preview/mmwrhtml/mm6210a4.htm?s_cid=mm6210a4_w
Category: Critical Care
Posted: 3/19/2013 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Extubating in the ED
McConville JF, Kress JP. Weaning patients from the ventilator. NEJM 2012; 367:2233-9.
