Category: Toxicology
Keywords: poinsettia (PubMed Search)
Posted: 12/20/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Myth: The ornamental red plant - poinsettia - gained a reputation as a poisonous plant from a case report. In 1919, a 2-year-old child reportedly died from an ingestion and later an 8-month-old developed mucosal burns. These anectdotal case reports perpetuated the myth that poinsettia plants are poisonous. In the modern literature there is one single case of anaphylaxis(1) due to poinsettia ingestion/exposure, an allergic dermatitis(2) and one case of dermatitis(4).
Krenzelok et al.(3) showed there were 22,793 cases of poinsettia exposure and there were no fatalities reported to poison centers. 96.1% were kept at home without sequelae.
1: Kimata H. Anaphylaxis by poinsettia in infants with atopic eczema. Allergy. 2007 Jan;62(1):91-2. 2: Bala TM, Panda M. No poinsettia this Christmas. South Med J. 2006 Jul;99(7):772-3. 3: Krenzelok EP, Jacobsen TD, Aronis JM. Poinsettia exposures have good outcomes...just as we thought. Am J Emerg Med. 1996 Nov;14(7):671-4. 4: Edwards N. Local toxicity from a poinsettia plant: a case report. J Pediatr.1983 Mar;102(3):404-5.
Category: International EM
Keywords: trypanosomiasis, Human African Trypanosomiasis, sleeping sickness, international (PubMed Search)
Posted: 12/19/2012 by Walid Hammad, MD, MBChB
Click here to contact Walid Hammad, MD, MBChB
· A parasitic disease transmitted by the bite of the 'Glossina' insect (tsetse fly.)
· The disease is most prevalent in rural areas of Africa. Untreated, it is usually fatal. Infection with the genus Trypanosoma brucei gambiense may lead to chronic asymptomatic illness.
· Travelers to endemic areas in Africa are risk becoming infected.
· Symptoms resemble a viral illness; headaches, fever, weakness, pain in the joints, and stiffness. The parasite is able to crosses the blood-brain barrier and causes neurological symptoms, mainly psychiatric disorders, seizures, coma and ultimately death.
· Diagnosis is by serological tests (Card Agglutination Trypanosomiasis Test or CATT). Confirmation of infection requires the performance of parasitological tests to demonstrate the presence of trypanosomes in the patient.
· Treatment: four drugs are registered for the treatment of HAT: pentamidine, suramin, melarsoprol and eflornithine.
World Health Organization. (2010). Working to overcome the global impact of neglected tropical diseases. First WHO report on neglected tropical diseases. Available: http://whqlibdoc.who.int/publications/2010/9789241564090_eng.pdf. Last accessed 12/17/2012
Category: Critical Care
Posted: 12/18/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Management of patients with severe traumatic brain injury (TBI) typically involves the use of invasive intra-parenchymal pressure monitors. Although use of these monitors is recommended by TBI management guidelines, good quality evidence of benefit is lacking.
A recently published study evaluated the outcomes of TBI patients using a management protocol incorporating either an intracranial pressure (ICP) monitor compared to use of the clinical exam PLUS serial neuroimaging; a total of 324 patients were prospectively randomized into either group.
The primary study outcome was a composite of survival, impaired consciousness, and functional status at both three and six months.
The results of the study did not show a significant difference in the:
Bottom line: This study suggests that clinical exam PLUS serial neuroimaging may perform as well as invasive intra-parenchymal monitors for guiding therapy in TBI patients.
Chestnut, R. et al. A Trial of Intracranial-Pressure Monitoring in Traumatic Brain Injury. NEJM 2012 Dec 12. http://www.ncbi.nlm.nih.gov/pubmed/23234472
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Visual Diagnosis
Posted: 12/17/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
50 year-old man with presents with acute-onset sharp left-sided chest pain and dyspnea. What's the diagnosis and the name of the abnormality on chest x-ray?
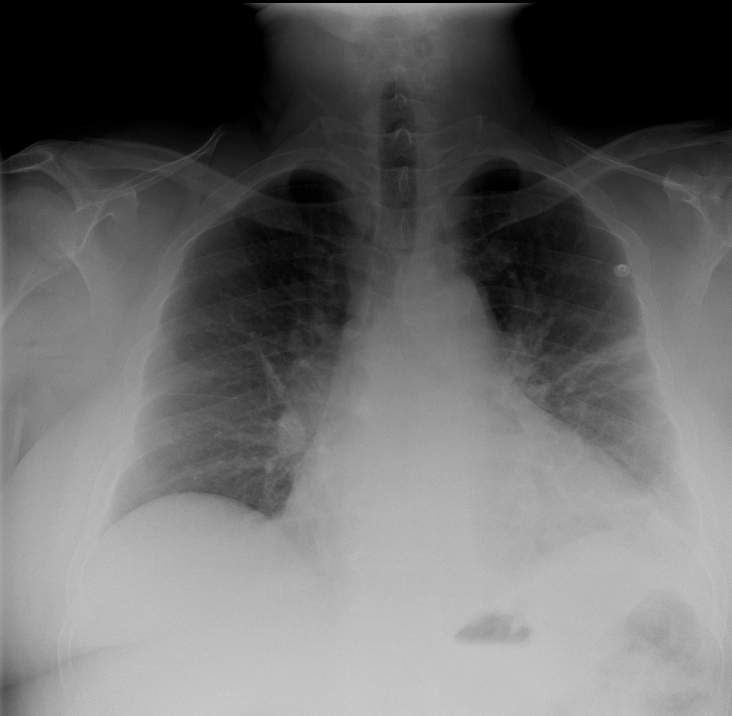
Answer: Pulmonary embolism with CXR demonstrating "Hampton Hump".
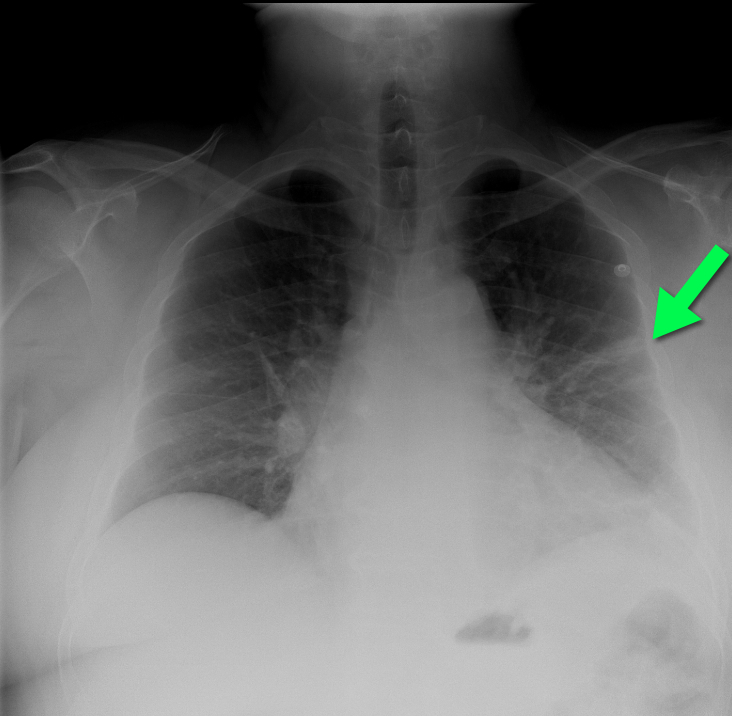
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: Pulmonary Arterial Hypertension (PAH) (PubMed Search)
Posted: 12/17/2012 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
A. Yao. Journal of Cardiology 60 (2012) 344–349
Category: ENT
Keywords: epistaxis (PubMed Search)
Posted: 12/15/2012 by Michael Bond, MD
Click here to contact Michael Bond, MD
Epistaxis can be a difficult thing to control in the ED, but there are several techniques you can learn that will make your life easier.
The majority of epistaxis cases are from kiesselbach's plexus therefore you can control it with:
Direct Pressure: Can be held with two fingers pinching the nares, or you can tape 4 tongue blades together and make your own "clothes pin" that can then be used to pinch the nares.
Vasoconstrictor and Anesthesia: A 1:1 mixture of topical lidocaine 4% and oxymetazoline can often be mixed together in the same oxymetazoline spray container enabling you to just spray it into the nares. This will often slow or stop the bleeding and provides anesthesia in case you need to cauterize the bleeding site. Some IV/IM narcotic pain medication will also help increase patient cooperation.
Visualize the bleeding site: Use a HEAD LAMP with an appropriate sized nasal speculum. You may look like Marcus Welby, MD but nothing works as well to see into the nose.
Cauterization It is best to cauterize circumferential around the bleeding site prior to directly cauterizing the actual site. Be careful with electrical cautery so has not to perforate the septum.
Nasal Packing: Instead of using surgilube to lubricate the packing; use Muprion, Bactroban or Bacitracin ointment to lubricate the packing. This will reduce the chance of Toxic Shock Syndrome.
Category: Toxicology
Keywords: aspirin, salicylate, thyroid, levothyroxine, hyperthermia, isoniazid, theophylline (PubMed Search)
Posted: 12/4/2012 by Bryan Hayes, PharmD
(Updated: 12/13/2012)
Click here to contact Bryan Hayes, PharmD
The more well known causes of toxin-induced hyperthermia include sympathomimetics and anticholinergics. In addition, neuroleptic malignant syndrome, serotonin syndrome, and malignant hyperthermia are high on the differential.
Several other xenobiotics can cause hyperthermia in overdose as well:
In general, benzodiazepines should be considered first-line therapy, followed by barbiturates, propofol, or other sedative hypnotics. Phenytoin rarely has a role in the management of toxin-induced seizures. Extrenal cooling measures are also warranted. Specifically for isoniazid, pyridoxine should be administered immediately with a benzodiazepine.
Levy RP, Gilger WG. Acute thyroid poisoning. N Engl J Med. 1957;256:459-460.
Boyd RE, Brennan PT, Deng JF, Rochester DF, Spyker DA. Strychnine poisoning. Recovery from profound lactic acidosis, hyperthermia, and rhabdomyolysis. Am J Med. 1983;74:507-12.
Follow me on Twitter (@PharmERToxGuy)
Category: International EM
Keywords: dengue, fever, international, mosquito, vector (PubMed Search)
Posted: 12/12/2012 by Andrea Tenner, MD
(Updated: 5/4/2026)
Click here to contact Andrea Tenner, MD
Background:
Dengue is the most rapidly expanding mosquito-borne virus with an increasing incidence and geographical area. It is most commonly found in the tropics, but there are occasional outbreaks in other places, including Texas and Hawaii.
Clinical:
Three Phases:
1. The febrile phase lasts 2-7 dyas and is similar to other viral syndromes, often with high fever and nausea/vomiting. Petechiae may also be present which can be induced by the application of a tourniquet.
2. The critical phase occurs after defervescence and lasts only 24-48 hours. IT is marked by increased capillary permeability and can lead to severe pulmonary edema, shock, and multisystem organ failure.
3. The recovery phase is marked by hemodynamic improvement. Some patients have a rash described as "isles of white in a sea of red."
Some patients will develop bradycardia. Most patients have a self-limited form of the illness that is not severe, and consists of symptoms seen in the febrile phase. The patients that develop severe dengue can have markers in the febrile phase that are associated with organ dysfunction, GI bleeding, and increased capillary permeability. Other concerning symptoms early are abdominal tenderness and persistent vomiting.
Treatment:
Treatment is supportive, mostly consisting of IV fluids, which is very effective when started early in the patient's illness. For more information and maps of endemic areas check out the CDC or WHO websites: http://www.cdc.gov/travel/notices/in-the-news/dengue-tropical-sub-tropical.htm or http://www.who.int/denguecontrol/en/
University of Maryland Section for Global Emergency Health
Author: Jenny Saltzberg
Dengue: guidelines for diagnosis, treatment, prevention, and control -- New Edition. (2009) World Health Organization.
Chen LH, Wilson ME. Dengue and chikungunya in travelers: recent updates. Curr Opin Infect Dis. 2012 Oct;25(5):523-9.
Category: Critical Care
Posted: 12/11/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Ultrasound-Guided Pericardiocentesis
L'Italien AJ. Critical cardiovascular skills and procedures in the emergency department. Emerg Med Clin N Am 2013; 31:151-206.
Tirado A, Wu T, Noble VE, et al. Ultrasound-guided procedures in the emergency department - Diagnostic and therapeutic asset. Emerg Med Clin N Am 2013; 31:117-149.
Category: Visual Diagnosis
Posted: 12/10/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
64 year-old male with no past medical history presents complaining of chronic weight-loss and diffuse chest pain; CXR is shown below. What's the diagnosis, and what other disease(s) may present this way?
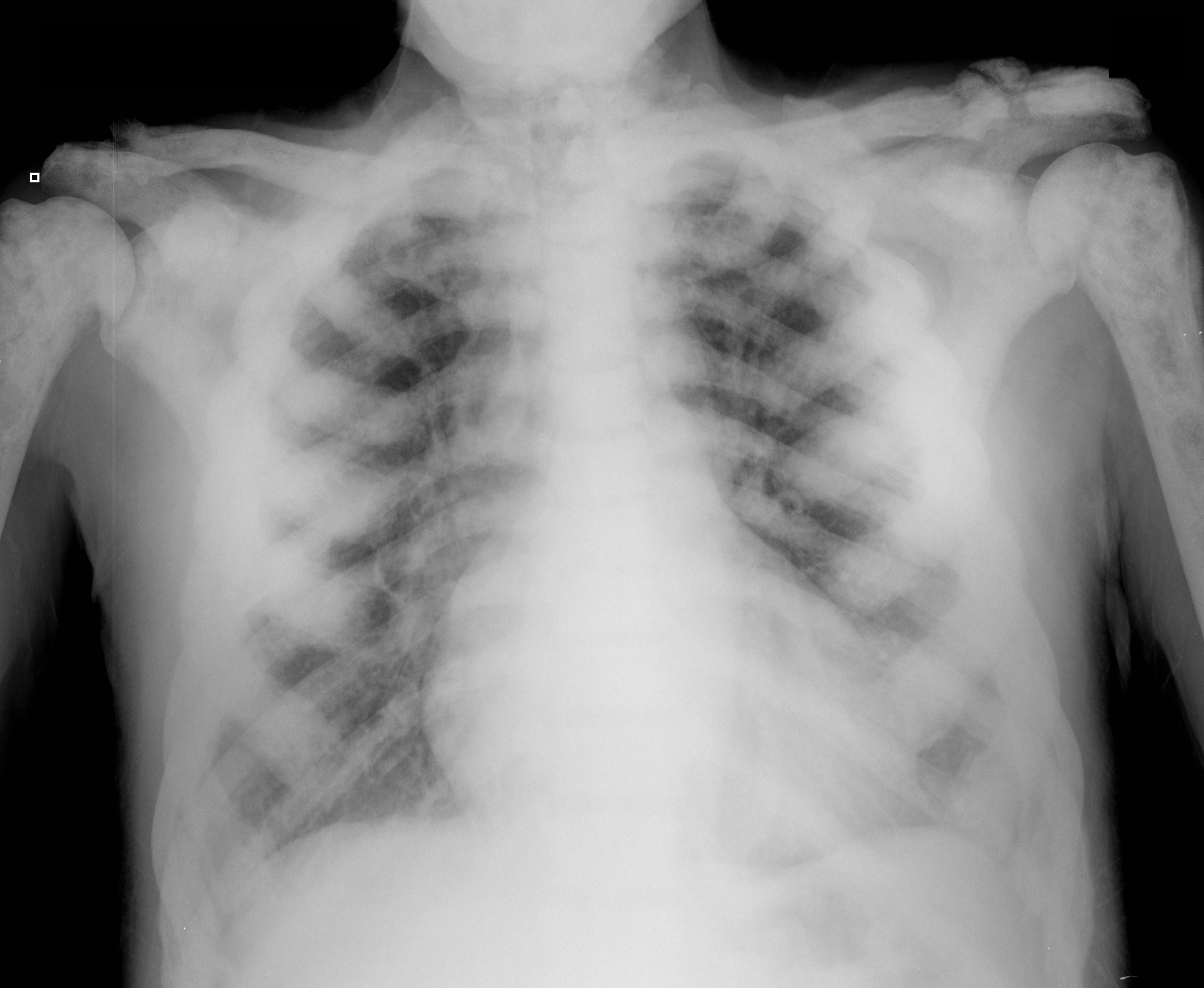
Answer: Sclerotic bone (osteoblastic) metastasis secondary to prostate cancer. The patient's CXR from 2 years prior is shown below for comparison.
Other malignancies associated with osteoblastic metastasis:
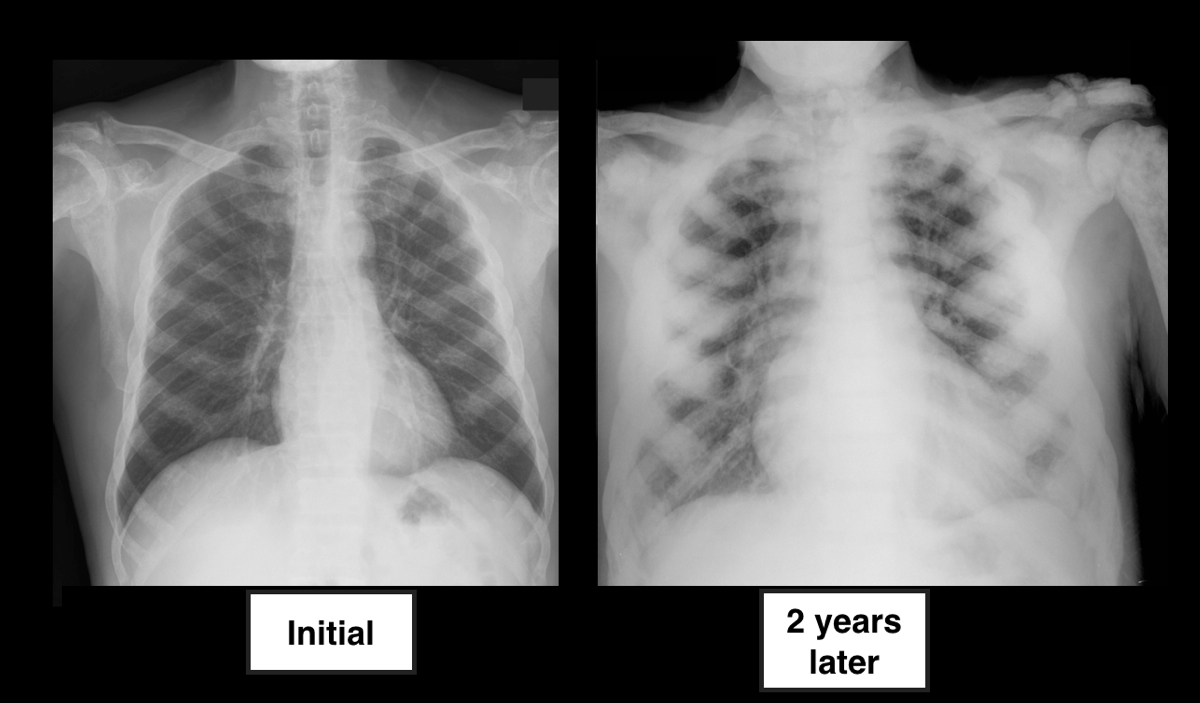
Follow me on Twitter (@criticalcarenow) or on Google+ (+haney mallemat)
Category: Cardiology
Posted: 12/8/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Hijazi K. Coarctation of the aorta: From fetal life to adulthood. Cardiology Journal. 18(5):487-95, 2011
Category: Orthopedics
Keywords: pneumonia, rib fracture, blunt chest trauma (PubMed Search)
Posted: 12/7/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Are discharged patients who suffer minor thoracic injury at risk of developing delayed pneumonia?
Prospective study of 1,057 patients age 16 and older with minor thoracic injury who were discharged from the ED.
32.8% had at least one rib fracture
8.2% had asthma
3.4% had COPD
Only 6 patients developed pneumonia!!
Sex, smoking, atelectasis on CXR, and alcohol intoxication were not significantly associated with delayed pneumonia.
However, for patients with preexistent pulmonary disease (asthma or COPD) AND rib fracture, the relative risk of delayed pneumonia was 8.6. Patients without either of these conditions are at extremely low risk of future development of pneumonia.
Patients with rib fractures do not develop delayed pneumonia: a prospective, multicenter cohort study of minor thoracic injury. Chauny JM, Emond M, Plourde M, Guimont C, Le Sage N, Vanier L, Bergeron E, Dufresne M, Allain-Boulé N, Fratu R. Ann Emerg Med. 2012 Dec;60(6):726-31.
Category: Pediatrics
Posted: 12/7/2012 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Epidemiology:
Trampoline injuries doubled between 1991 and 1996, increasing from 39,000 injuries per year to more then 83,000 injuries per year. Injury rates and trampoline sales peaked in 2004 and have been decreasing since; however, hospitalization rates are still between 3% and 14%.
Risk Factors:
¾ of injuries occur when multiple people are on the trampoline at once
Smaller participants were 14x more likely to be injured then their heavier playmates
Falls account for 27-39% of all injuries
Springs and frames account for 20% of injuries
Up to ½ of injuries occur despite adult supervision
Injury types:
Lower extremity injuries are more common than upper extremity
Head and neck injuries accounted for 10-17% of trampoline injuries
Unique Injuries:
Proximal tibial fractures
Manubriosternal dislocations and sternal injuries
Vertebral artery dissection
Atlanto-axial subluxation
Trampoline Saftey in Childhood and Adolescence. Pediatrics 2012; 130; 774-779.
Category: Critical Care
Keywords: anaphylaxis, tryptase, diagnosis (PubMed Search)
Posted: 12/6/2012 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Simons EF, Ardusso LE, Bilo MB, et al. 2012 Update: World Allergy Organization Guidelines for the assessment and management of anaphylaxis.
Category: Airway Management
Posted: 12/5/2012 by Walid Hammad, MD, MBChB
(Updated: 5/4/2026)
Click here to contact Walid Hammad, MD, MBChB
40 yo previously healthy male in China who presents with prolonged “seizure” after receiving a cut on his foot while fishing 5 days ago.
Dx: Tetanus
Clinical features:
· Incubation period 4-14 days
· 3 clinical forms:
1. Local spasm
2. Cephalic (rare) - cranial nerve involvement
3. Generalized (most common) - Descending spasm: facial sneer (risus sardonicus), “locked jaw” trismus, neck stiffness, laryngeal spasm, abdominal muscle spasm.
· Spasms continue to 3-4 weeks and can take months to fully recover
Complications: apnea, rhabodymyolysis, fracture/dislocations
Treatment: supportive, benzodiazepines, RSI, Tetanus IG (3000-5000 units IM), wound debridement
University of Maryland Section for Global Emergency Health
Author: Veronica Pei, MD
Category: Visual Diagnosis
Posted: 12/4/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
An 86 year-old nursing home resident presents to the ED with a urinary tract infection, four days after discharge from the inpatient service for the same diagnosis. She was discharged from the inpatient service with a prescription for ciprofloxacin to be given through her gastric feeding tube (she does not take anything orally). Could her tube feeds be playing a role in the relapse of her urinary tract infection?
Answer: Ciprofloxacin was not being properly absorbed secondary to enteral tube feeding.
Fluoroquinolones administered via enteral feeding tubes may have reduced efficacy and patient outcomes when given to patients simultaneously receiving tube feeds (e.g., PEG tube feeding).
The reduction in antimicrobial efficacy may be due to improper peak drug concentrations and variability in time to peak serum levels. Studies have demonstrated the bioavailability of Ciprofloxacin varies from 31-82% in patients receiving continuous enteral feeds.
The exact mechanism(s) responsible for the altered pharmokinetics are not completely understood but may involve the binding of divalent cations in the enteral feeds by fluoroquinolones, reducing its absorption and efficacy.
Clinicians should properly educate people who will be administering fluoroquinolones to the patient (e.g., nursing home staff, family, etc.). It is recommended that fluoroquinolones be given:
Perhaps easiest of all, is to consider discharging patients with a prescription for parenterally administered antibiotics for the duration of the infection.
Beckwith MF, Feddema SS, Barton RG, Graves C. A guide to drug therapy in patients with enteral feeding tubes: Dosage form selection and administration methods. Hosp Pharm. 2004;39:225–37
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Visual Diagnosis
Posted: 12/2/2012 by Haney Mallemat, MD
(Updated: 12/3/2012)
Click here to contact Haney Mallemat, MD
11 year-old boy presents with right knee pain and swelling after falling off of his bicycle. What's the diagnosis?
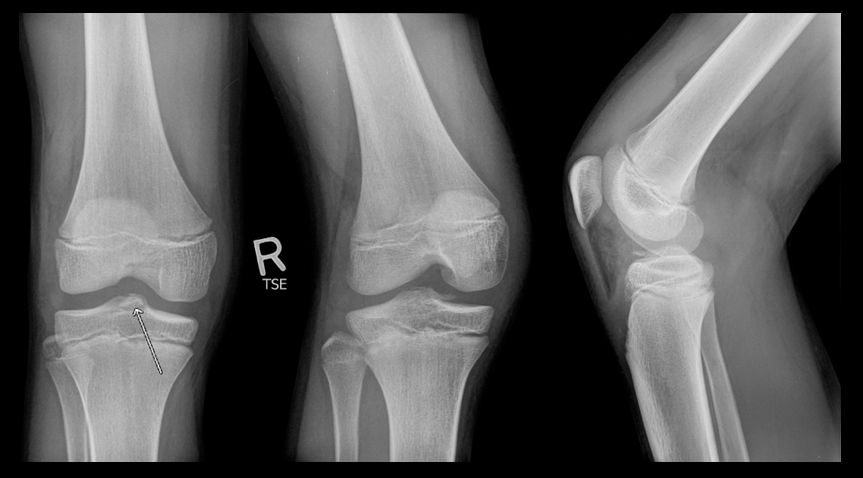
Answer: Fracture of the intercondylar eminence of the tibia; Meyers & McKeever Grade II (grading system described below)
Intercondylar Eminence Fracture
Reference: Tudisco, C., et al Intercondylar eminence avulsion fracture in children: long-term follow-up of 14 cases at the end of skeletal growth, J Pediatr Orthop B 19:403–408 c 2010
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: Kawasaki Disease, Mucocutaneous lymph node syndrome (PubMed Search)
Posted: 12/2/2012 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
Scuccimarri R. Kawasaki Disease. Pediatric Clin N Am 59(2012)425-445
Category: Pharmacology & Therapeutics
Keywords: doxycycline, PID, pelvic inflammatory disease, STD, azithromycin (PubMed Search)
Posted: 11/28/2012 by Bryan Hayes, PharmD
(Updated: 12/1/2012)
Click here to contact Bryan Hayes, PharmD
In the rare circumstance you need to treat a patient with suspected PID and an allergy to doxycycline, what is the alternative?
For oral regimens, azithromycin is an option in place of doxycycline.
Suggested regimen for PID with doxycycline allergy:
Bevan CD, Ridgway GL, Rothermel CD. Efficacy and safety of azithromycin as monotherapy or combined with metronidazole compared with two standard multidrug regimens for the treatment of acute pelvic inflammatory disease. J Int Med Res 2003;31:45–54.
Savaris RF, Teixeira LM, Torres TG, et al. Comparing ceftriaxone plus azithromycin or doxycycline for pelvic inflammatory disease: a randomized controlled trial. Obstet Gynecol 2007;110:53–60.
Follow me on Twitter (@PharmERToxGuy)
Category: Toxicology
Keywords: CT, carbon monoxide, cyanide (PubMed Search)
Posted: 11/29/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
It is not often that a CT will be able to give you a hint to a toxicologic diagnosis. The following are CT findings that are either suggestive and even sometimes almost diagnostic for a given to toxin:
1) Intraparenchymal or Subarachnoid Hemorrhage: sympathomimetics or mycotic anuerysm rupture secondary to IV drug abuse
2) Basal Ganglia bilateral focal necrosis: characteristic of carbon monoxide, cyanide, hydrogen sulfide and even methanol
3) Severe advanced atrophy out of proportion for age: alcoholism, toluene
Adapted from Goldfranks Textbook of Toxicologic Emergencies 8th edition, p.82 Table 6-5.
