Category: Visual Diagnosis
Keywords: spinal, international, tuberculosis, scoliosis, kyphosis, pulmonary, neurologic (PubMed Search)
Posted: 1/9/2013 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
These two Ethiopian boys present with “back problems”. What are the diagnoses and what do you need to worry about with each of them?
The boy on the left has spinal tuberculosis (Pott's Disease) while the one on the right has severe scoliosis.
Pott's Disease:
Severe Scoliosis:
Bottom Line:
Spinal tuberculosis most commonly causes anterioposterior (AP) deformity and can cause severe neurologic deficits. Anti-TB medication is needed for treatment.
Severe scoliosis involves lateral as well as AP deformity and can cause severe pulmonary dysfunction.
University of Maryland Section of Global Emergency Health
Author: Andi Tenner, MD, MPH
Center for Disease Control and Prevention. Guidelines for Preventing the Transmission of Mycobacerium tuberculosis in Health-Care Settings. MMWR 2005;54(No. RR-17):1-144.
Koumbourlis AC. Scoliosis and the respiratory System. Paediatric Respiratory Reviews 2006;7:152-160.
Turgut M. Spinal tuberculosis (Pott’s disease): its clinical presentation, surgical management, and outcome. A survey study on 694 patients. Neurosurg Rev 2001;24:8-13.
Category: Critical Care
Posted: 1/8/2013 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
The Crashing Cardiac Transplant Patient
Chacko P, Philip S. Emergency department presentation of heart transplant recipients with acute heart failure. Heart Failure Clinics 2009; 5:129-143.
Costanzo MR, et al. The International Society of Heart and Lung Transplantation Guidelines for the care of heart transplant recipients. J Heart Lung Transplant 2010; 29:914.956.
Category: Visual Diagnosis
Posted: 1/7/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
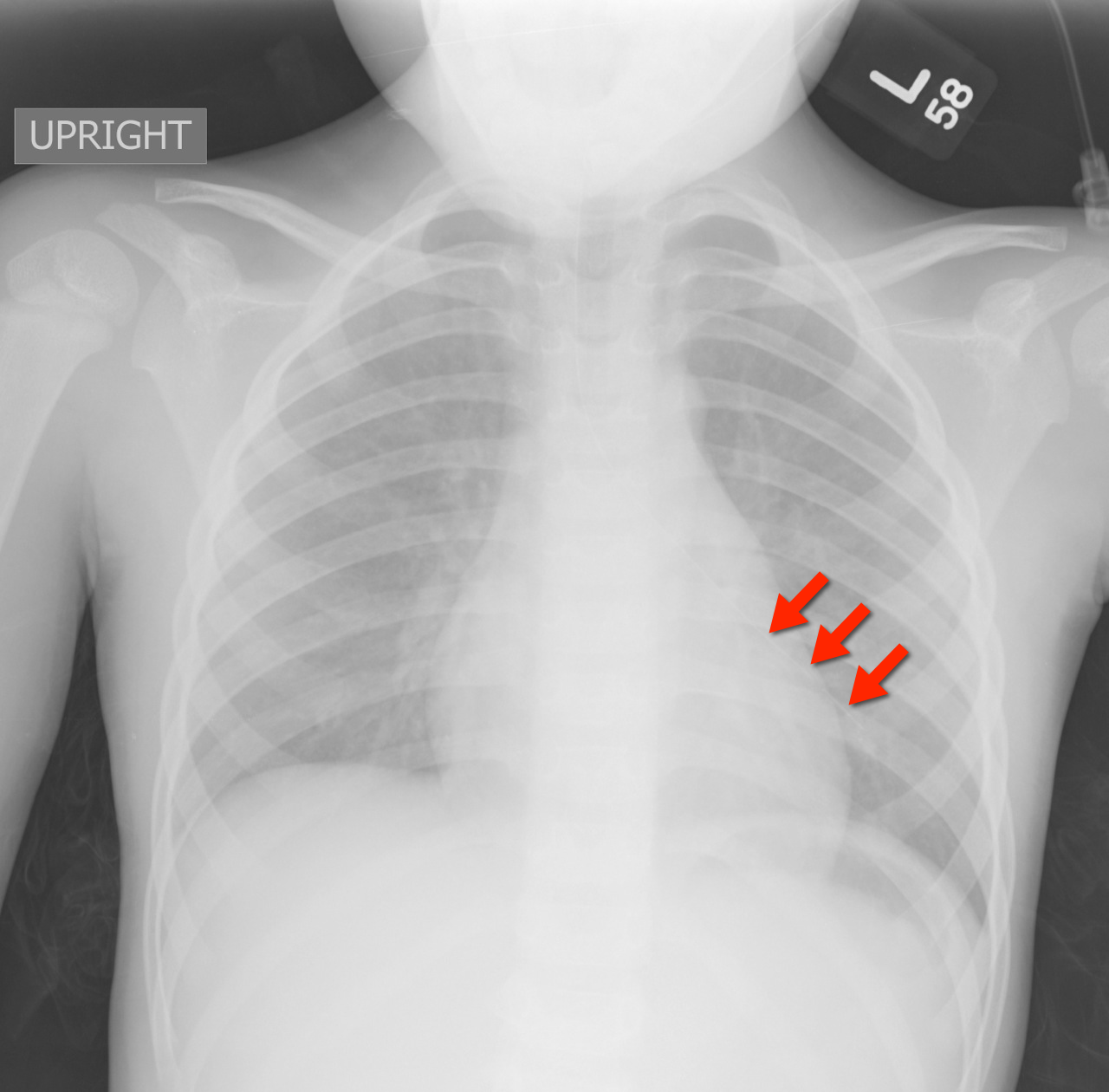
4 year-old female with the post-procedural CXR shown below. What's the diagnosis? (Hint: use the zoom...this one is tricky)
Answer: Nasogastric tube in the left mainstem bronchus. Patient was asymptomatic but ironically bubbling was heard when air was injected into the NG tube.
Nasogastric tube (NGT) pearls
The risk of NGT misplacement is 4% in adults, but is 21-43% in children.
Risk factors for misplacement are:
The ability to aspirate gastric contents, pH testing of the aspirated fluid, and the auscultation of “bubbling” over the epigastrium have all been suggested as reliable methods to confirm proper placement; unfortunately, they are often unreliable.
Visualization of the NGT by X-ray is the only way to be 100% certain of placement.
The risks of misplacement include pneumonia and pneumothorax.
Farrington et al. Nasogastric tube placement verification in pediatric and neonatal patients. Pediatric Nursing. Jan-Feb 2009. Vol 35. Issue 1.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 1/6/2013 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
Bock J, Benitez M. Blunt Cardiac Injury. Cardiology Clinics. 2012;30(4):545-55.
Category: Pharmacology & Therapeutics
Keywords: Tdap, tetanus, immunization, vaccine, pertussis (PubMed Search)
Posted: 1/3/2013 by Bryan Hayes, PharmD
(Updated: 1/5/2013)
Click here to contact Bryan Hayes, PharmD
The two available Tetanus/reduced diphtheria toxoid/acellular pertussis (Tdap) vaccine products in the U.S. are Boostrix and Adacel. Neither were originally approved in older adults age 65 and older. Boostrix received FDA-approval for use in this age group in July 2011, but Adacel never has.
However, in June 2012 ACIP issued new guidance recommending Tdap for all adults age 65 years and older.
"When feasible, Boostrix should be used for adults aged 65 years and older; however, ACIP concluded that either vaccine administered to a person 65 years or older is immunogenic and would provide protection. A dose of either vaccine may be considered valid."
Bottom line: Regardless of which Tdap product is stocked at your institution, both are considered safe to use in adults 65 years and older.
Centers for Disease Control and Prevention (CDC), “Updated Recommendations for Use of Tetanus Toxoid, Reduced Diphtheria Toxoid, and Acellular Pertussis (Tdap) Vaccine in Adults Aged 65 Years and Older - Advisory Committee on Immunization Practices (ACIP)," MMWR Morb Mortal Wkly Rep, 2012, 61(25):468-70. [PMID 22739778]
Follow me on Twitter (@PharmERToxGuy)
Category: Pediatrics
Posted: 1/4/2013 by Lauren Rice, MD
(Updated: 5/4/2026)
Click here to contact Lauren Rice, MD
Rotavirus is the leading cause of gastroenteritis worldwide and a leading cause of infant death in the developing world.
95% of U.S. children have had a rotavirus infection by the age of 5 years.
Most cases occur in late winter and early spring.
Route of transmission is mostly fecal-oral but may be airborne in cooler months.
Most common presenting signs and symptoms include fever (1/3 of cases), vomiting (in the first 1-2 days), and diarrhea (copious, watery, lasting 5-21 days).
Diagnosis is largely based on clinical manifestations, but antigen assays are available and may be useful in patients with extraintestinal complications, such as hepatitis, pneumonitis, or encephalopathy.
Treatment is largely supportive with efforts to maintain hydration.
Prevention is key to disease control and accomplished with good hand hygiene and widespread vaccination.
Newly implemented vaccine programs worldwide have proven to be effective in decreasing hospitalizations and deaths in developing countries.
Cox, Elaine and Christenson, John. Rotavirus. Pediatrics in Review. 2012; 33 (10): 439 - 447.
Category: Toxicology
Keywords: creatine, supplement, weight lifting (PubMed Search)
Posted: 1/3/2013 by Ellen Lemkin, MD, PharmD
(Updated: 5/4/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Creatine
Adverse effects: weight gain, edema, GI cramping, fatigue and diarrhea
Dandoy C, Gereige RS. Performance-Enhancing Drugs. Pediatrics in Review June 2012;33(6):265-72.
Category: International EM
Keywords: Leptospirosis, Baltimore, jaundice, thrombocytopenia, international, tropical (PubMed Search)
Posted: 1/2/2013 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
-Leptospirosis is a tropical infectious disease that is also endemic in the US. (Estimated 16% seroprevalence in inner city Baltimore!)
-The spirochete is spread through animal urine and can survive in water or soil for weeks.
-Risk factors: rural exposure to animal urine (farming, adventure sports) or urban exposure to rat urine.
-Infection is acquired through breaks in the skin or mucus membranes
-Outbreaks are often seen following rain or floods.
Clinical Presentation:
-Non-specific febrile illness (usually not diagnosed in these cases)
-If untreated, 5-10% progress to jaundice, renal failure, thrombocytopenia, hemorrhage, and respiratory failure.
Diagnosis:
- Primarily based on clinical presentation and history
- Paired serum sent to CDC (the acute serum sample should be drawn in the ED)
Treatment:
- Doxycycline, Ceftriaxone and Penicillin are all effective
Bottom Line:
Consider and treat for Leptospirosis in patients with possible exposure animal urine (especially after a flood) who present in extremis with renal failure, jaundice, and thrombocytopenia.
University of Maryland Section of Global Emergency Health
Author: Andi Tenner, MD, MPH
Center for Disease Control. (2012) Leptospirosis. Retrieved January 1, 2013 from http://www.cdc.gov/leptospirosis/infection/index.html.
Childs JE, Schwartz BS, Ksiazek TG, et al. Risk Factors Associated with Antibodies to Leptospires in Inner-city Residents of Baltimore: A Protective Role for Cats. Am J Public Health. 1992;82:597-599.
Leung J, Schiffer J. Feverish, Jaundiced. Am J Med. 2009;122:129-131.
Category: Critical Care
Posted: 1/1/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
DRESS (Drug Reaction with Eosinophilia and Systemic Symptoms) or DIHS (Drug-Induced Hypersensitivity Syndrome) is a potentially life-threatening adverse drug-reaction.
Incidence is 1/1,000 to 1/10,00 drug exposures. It occurs 2-6 weeks after the drug is first introduced, distinguishing it from other adverse drug-reactions which typically occur sooner.
The syndrome classically includes:
The most commonly implicated drugs are anticonvulsants (e.g., carbamazepine, phenobarbital, and phenytoin), sulfonamides, and allopurinol.
Recovery is typically complete after discontinuing the offending drug; systemic steroids may promote resolution of the illness.
Cacoub P. et al. The DRESS syndrome: a literature review. Am J Med 2011 Jul;124(7):588-97. http://www.ncbi.nlm.nih.gov/pubmed/21592453
Follow me on Twitter (@criticalcarenow) or on Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 12/31/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
31 year-old male with recently diagnosed hypertension presents with rapid lip swelling. He started taking an unknown medication for his hypertension last week. Further history reveals that he has had prior, although milder, episodes previously. Name two medications that may help treat him.
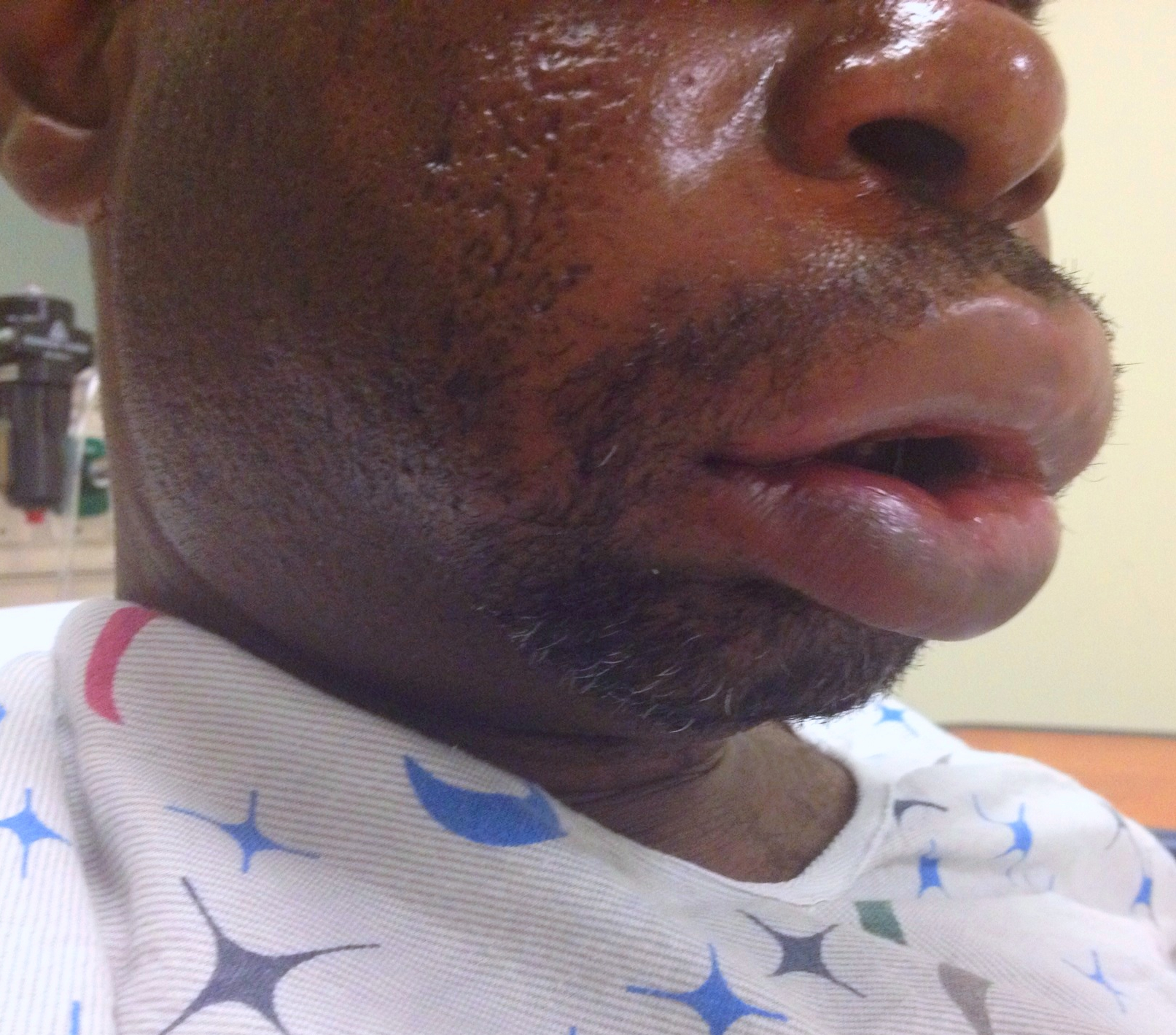
Answer: The patient has hereditary angioedema with an episode triggered by an ACE inhibitor. Treatment includes the usual cocktail of histamine blockers and steroids plus:
The precipitant cause is unknown in most cases, but common etiologies include drugs (e.g. ACE inhibitors), infections, dental work, or stress.
Serum C4 level may assist in the diagnosis, but are rarely helpful acutely.
Fifty percent of patients will have laryngeal swelling at one point in their lives and asphyxiation is the leading cause of death; mortality is ~14-33%
The airway must be emergently evaluated to determine the need for intubation. If required, the most skilled person should take the first look.
If access to the oropharynx is limited (secondary to lip and tongue swelling) fiberoptic nasolaryngoscopy may be considered however, always be prepared to perform an emergent surgical airway.
Bonus Pearl: Check out this months V-Cast hosted by Dr. Amal Mattu. Dr. Jim Roberts (of Roberts and Hedges fame) reviews angioedema. Check out this great review here: http://cmedownload.com/lecture/angioedema-v-cast
References
Joseph J. Moellman, and Jonathan A. Bernstein. Diagnosis and Management of Hereditary Angioedema: An Emergency Medicine Perspective. Journal of Emergency Medicine 2012 http://www.jem-journal.com/article/S0736-4679(11)01116-4/abstract
Follow me on Twitter (@criticalcarenow) or on Google+ (+criticalcarenow)
Category: Cardiology
Posted: 12/30/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Category: Orthopedics
Keywords: metacarpal, neck, fracture (PubMed Search)
Posted: 12/29/2012 by Michael Bond, MD
Click here to contact Michael Bond, MD
Metacarpal Neck Fractures (i.e.: Boxer’s Fracture if 5th Metacarpal)
Depending on the MCP joint involved a certain amount of angulation is permissible before it adversely affects normal function.
Wishing everybody a Happy and Healthy New Year.
Category: Pediatrics
Posted: 12/28/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Toxicology
Keywords: ketamine, pain (PubMed Search)
Posted: 12/27/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Despite a paucity of data, pain management clinics are administering topical gel mixtures that have included ketamine, tricyclics, calcium channel blockers and baclofen. Internet blogs have already identified this gel mixture as a way to "get high". This is one of those google searches you have to do on your own.
1: Lynch ME, Clark AJ, Sawynok J, Sullivan MJ. Topical 2% amitriptyline and 1% ketamine in neuropathic pain syndromes: a randomized, double-blind, placebo-controlled trial. Anesthesiology. 2005 Jul;103(1):140-6. 2: Lynch ME, Clark AJ, Sawynok J. A pilot study examining topical amitriptyline, ketamine, and a combination of both in the treatment of neuropathic pain. Clin J Pain. 2003 Sep-Oct;19(5):323-8. 3: Uzaraga I, Gerbis B, Holwerda E, Gillis D, Wai E. Topical amitriptyline, ketamine, and lidocaine in neuropathic pain caused by radiation skin reaction: a pilot study. Support Care Cancer. 2012 Jul;20(7):1515-24.
Category: International EM
Posted: 12/25/2012 by Walid Hammad, MD, MBChB
(Updated: 5/4/2026)
Click here to contact Walid Hammad, MD, MBChB
Bottom Line: A mild increase in blood parasite count after initiation of treatment is not uncommon. Marked increases should indicated treatment failure and the treatment drug should be changed to another class.
University of Maryland Section for Global Emergency Health
Author: Emilie J.B. Calvello, MD, MPH
Wurts, N. Et al. Early treatment failure during treatment of Plasmodium falciparum malaria with atovaquone-proquanil in the Repulic of Ivory Coast. Malar J 2012 May; 2(11): 146.
Silachomroon, U. Et al. Frequency of Early Rising Parasitemia in Falciparum Malaria Treated with Artemisinin Derivatives. Southeast Asian J Trop Med Pub Health 2001 Mar; 32(1): 50 – 56.
Category: Critical Care
Posted: 12/25/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
VV-ECMO for Refractory Hypoxemia
Combes A, et al. What is the niche for extracorporeal membrane oxygenation in severe acute respiratory distress syndrome? Curr Opin Crit Care 2012; 18:527-32.
Category: Visual Diagnosis
Posted: 12/24/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
52 year-old male with diabetes complains of severe left foot pain for one month and now inability to ambulate. Vital signs are normal and X-rays are shown below. What's the diagnosis and why should you get a biopsy early?
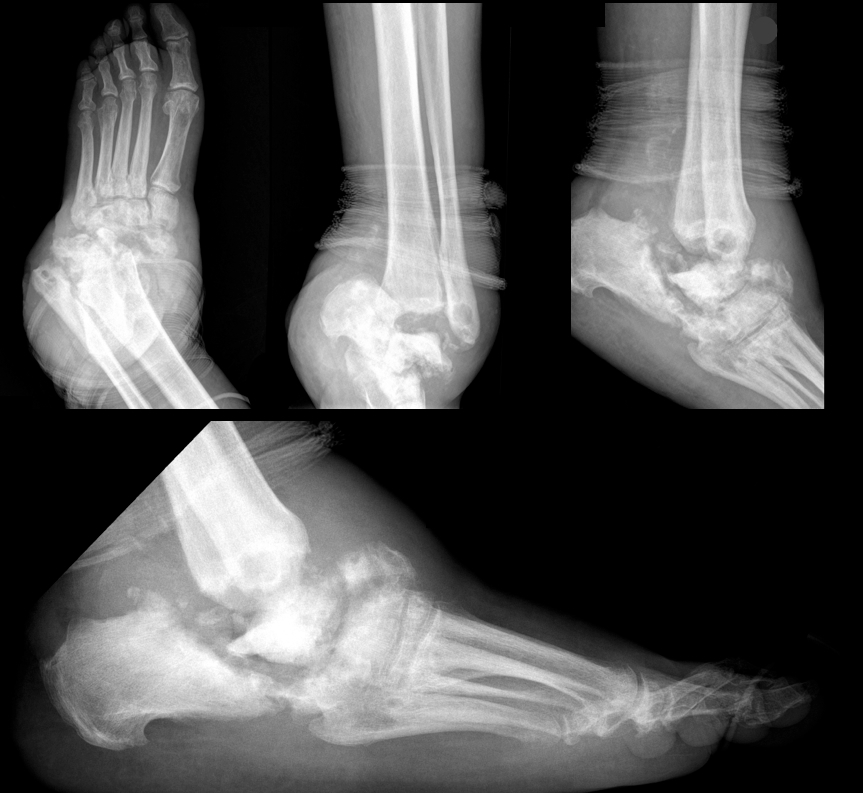
Answer: Osteomyelitis and a bone biopsy (with culture) should be obtained early and before starting antibiotics.
Osteomyelitis is inflammation of a bone secondary to an infecting organism.
Risk factors include:
Causative bacteria typically include S. Aureus, Pseudomonas, Salmonella (classically with Sickle cell)
Diagnosis
Early and long-term antibiotic treatment (4-6 weeks) is required, but should be done AFTER obtaining bone biopsy and culture; long-term antibiotics are the rule and the most narrow spectrum antibiotic should be determined.
Operative management is sometimes required; especially if secondary to infected prosthetics.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Posted: 12/23/2012 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
Armstrong E, MD, Kulkarni A, Hoffmayer K, et al. Am J Cardiol 2012;110: 345–349
Category: Orthopedics
Keywords: Exercise, NSAIDs, bowel injury (PubMed Search)
Posted: 12/22/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
NSAIDs are commonly used by professional and recreational athletes to both reduce existing and/or prevent anticipated exercise induced musculoskeletal pain
NSAIDs have potential hazardous effects on the gastrointestinal (GI) mucosa during strenuous physical exercise
Potential effects include mucosal ulceration, bleeding, perforation. and short-term loss of gut barrier function in otherwise healthy individuals
Intense exercise by itself has previously been shown to induce small intestine injury
Human intestinal fatty acid binding protein (1-FABP) is a protein found in mature small bowel enterocytes which diffuses into the circulation upon injury
Ibuprofen and endurance exercise (cycling) independently result in increased 1-FABP levels
When occurring together, ibuprofen ingestion with subsequent exercise causes significantly increased small bowel injury and intestinal permeability
Small bowel injury was found to be reversible in 2 hours
Taking empiric NSAIDs before endurance exercise may be an unhealthy practice and should be discouraged in the absence of a clear medical indication
Aggravation of exercise-induced intestinal injury by Ibuprofen in athletes. VAN Wijck K, Lenaerts K, VAN Bijnen AA, et al. Med Sci Sports Exerc. 2012 Dec;44(12):2257-62.
Category: Pediatrics
Posted: 12/15/2012 by Mimi Lu, MD
(Updated: 12/21/2012)
Click here to contact Mimi Lu, MD
Parents bring in their child who placed a bead, seed, or other object up her nose. What do you do? Who should you call?
Research suggests that a decades-old home remedy (of sorts) known as the “mother’s kiss” may do the trick for children 1-8 years of age. It’s also much less invasive or frightening than some of the tools and techniques used in emergency departments with a success rate approaching 60%
First described in 1965, here’s how the mother’s kiss technique works:
