Category: International EM
Keywords: water, international, cryptopsporidium, chlorine, iodine, boiling (PubMed Search)
Posted: 11/28/2012 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
• Millions of people around the world (including our patients who travel and victims of disasters like Hurricane Sandy) are exposed to non-potable water.
• How to treat contaminated water:
♦ Filter cloudy water through a clean cloth or allow to settle prior to treatment
♦ The safest method is boiling water vigorously for 1 minute (or, at least 3 minutes at altitudes >6,000ft)
♦ Chemical disinfection is not as effective but, if boiling is not possible, use either:
• 2 drops of unscented bleach (5.52% Cl) per quart/liter of water. (Unknown strength? Add 10 drops per quart/liter.)
-Or-
• 5 drops of tincture of 2% iodine per quart/liter.
- If the water is cloudy or cold, double the chlorine or iodine.
- Notes: Pregnant women or people with thyroid conditions should not use iodine
♦ UV decontamination can be accomplished by leaving clear bottles of water in direct sun for >6 hours or special equipment, but requires clear water
• Boiling, Chlorine/Iodine, and UV will kill viruses, bacteria, and Giardia
• Only Boiling kills Cryptosporidium
Bottom Line:
• If bottled water is available, use it.
• If not, boil your water.
• In order to treat for a wide variety of pathogens, it is best to combine available methods.
University of Maryland Section for Global Emergency Health
Author: Andi Tenner
United States Environmental Protection Agency. Water Health Series: Filtration Facts. 2005. http://water.epa.gov/drink/info/upload/2005_11_17_faq_fs_healthseries_filtration.pdf
United States Environmental Protection Agenecy. Emergency Disinfection of Drinking Water. 2006. http://water.epa.gov/drink/emerprep/emergencydisinfection.cfm .
United States Center for Disease Control. Water Treatment Methods. 2011. http://wwwnc.cdc.gov/travel/page/water-treatment.htm.
Category: Critical Care
Posted: 11/27/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Managing Critically Ill Patients with AKI
Brienza N, et al. Protocoled resuscitation and the prevention of acute kidney injury. Curr Opin Crit Care 2012; 18:613-622.
Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney Int 2012; 2(S):1-138.
Category: Visual Diagnosis
Posted: 11/25/2012 by Haney Mallemat, MD
(Updated: 11/26/2012)
Click here to contact Haney Mallemat, MD
2 year-old male with past medical history of asthma presents with fever and respiratory distress. CXR is shown below. What’s the diagnosis? (Hint: ...look beyond the obvious)
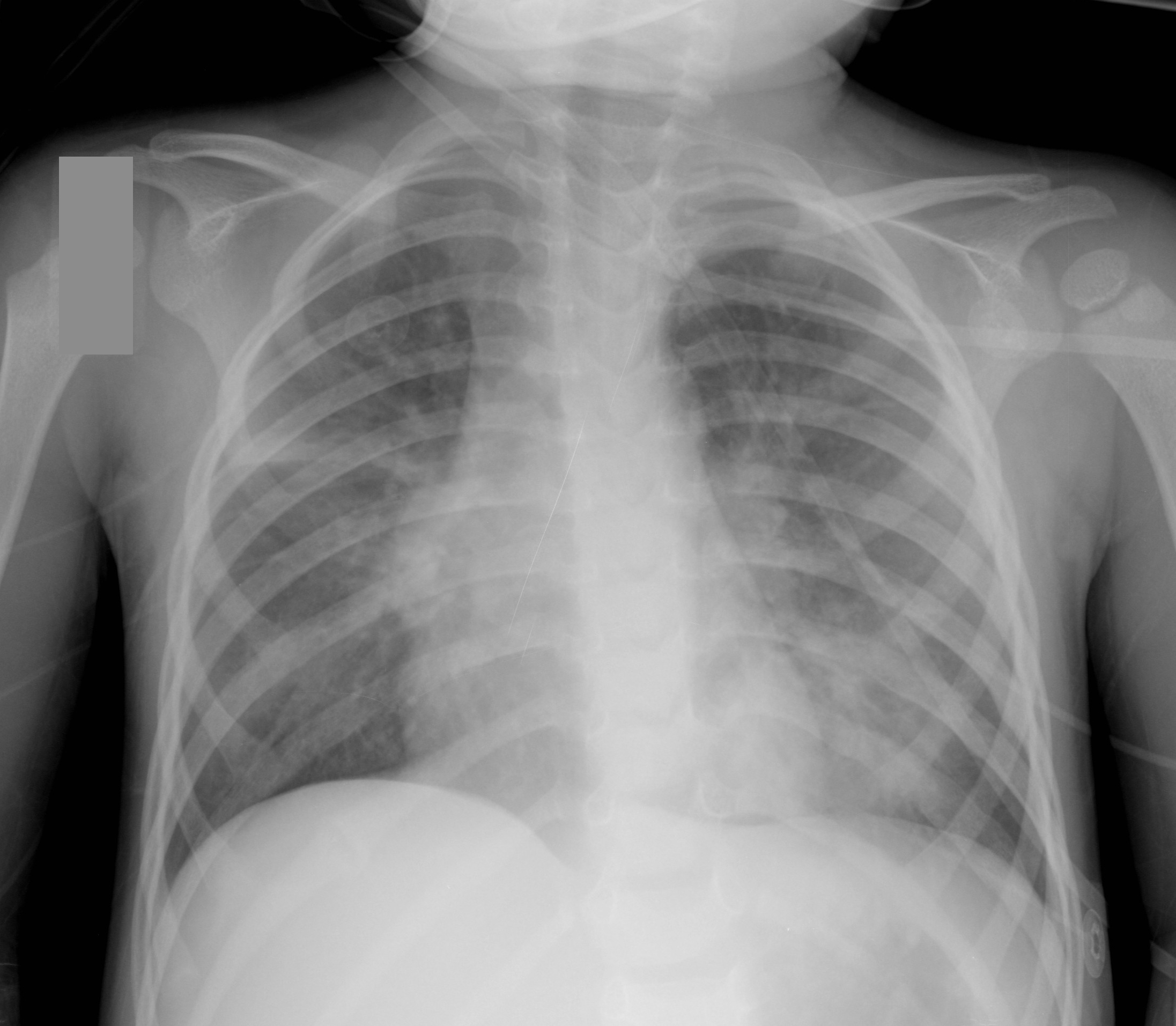
Answer #1: Multifocal opacities predominantly in left lower lobe representing pneumonia
Answer #2 Healing left-sided rib fractures involving the lateral aspects of ribs 8 through 10th suspicious for non-accidental trauma (see X-ray below)
Pediatric CXR pearls
Bottom line: Screen patients for the above risk factors when rib fractures have been identified, but always think of abuse and the child’s safety first….and don’t forget to thoroughly examine radiology despite finding one abnormal finding.

Reference: Cosway et al. Diagnostic indicators for NAI in children with rib fractures: A retrospective study. Arch Dis Child 2011; 96 (supplement)
Follow me on Twitter (@criticalcarenow) or Google+ (+Haney Mallemat)
Category: Cardiology
Keywords: Rheumatic fever, rheumatic heart disease (PubMed Search)
Posted: 11/25/2012 by Semhar Tewelde, MD
(Updated: 5/4/2026)
Click here to contact Semhar Tewelde, MD
Marijon E. Mirabel M. Celermajer DS. Jouven X. Rheumatic heart disease. Lancet. 379(9819):953-64, 2012 Mar 10.
Category: Orthopedics
Keywords: hematoma blocks, fracture analgesia (PubMed Search)
Posted: 11/24/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Hematoma blocks for distal radius fractures
Hematoma blocks provide safe, effective analgesia without an increased risk of post procedural infections when compared with other regional blocks
Provide equal reduction quality AND pain control as procedural sedation with Propofol.
However, mean time to reduction (0.9 vs. 2.6 hours) and time to discharge post procedure (0.74 vs. 1.17 hours) were reduced with hematoma blocks.
Consider this option next time the department is busy or the patient is not an ideal procedural sedation candidate.
Emiley P, Schreier S and Pryor P. Hematoma Blocks for Reduction of Distal Radius Fractures. Emergency Physicians Monthly. September 2012. 16-17.
Category: International EM
Keywords: malaria, Plasmodium, falciparum, quinine, international, fever (PubMed Search)
Posted: 11/21/2012 by Andrea Tenner, MD
(Updated: 5/4/2026)
Click here to contact Andrea Tenner, MD
University of Maryland Section for Global Emergency Health
Author: Emilie J.B. Calvello, MD, MPH
Center for Disease Control. (2012). Malaria. Retrieved November 9, 2012, from http://www.cdc.gov/MALARIA/
Wattal, C. et al. Infectious disease emergencies in returning travelers: special referece to malaria, dengue and chikungunya. Med Clin North Am. 2012 Nov; 96(6): 1225 – 55.
Category: Critical Care
Posted: 11/20/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
A low-tidal volume (or protective) strategy of mechanical ventilation (i.e., tidal volume of 6-8cc/kg of ideal body weight) has previously been demonstrated to be beneficial in patients with acute respiratory distress syndrome (ARDS).
A meta-analysis was recently performed to determine whether this strategy of mechanical ventilation is also beneficial for patients without lung injury prior to initiation of mechanical ventilation.
Dr. Neto, et al. performed a meta-analysis of 20 studies (total of 2,822 mechanically ventilated patients) comparing a conventional ventilation strategy (average tidal volume was 10.6 cc/kg) to a protective ventilation strategy (average tidal volume was 6.4 cc/kg) of mechanical ventilation.
The authors concluded that patients ventilated with a protective lung-strategy had reductions in:
Bottom-line: This meta-analysis supports the notion that a strategy of low-tidal volume ventilation may have benefits for patients without ARDS, however prospective studies are needed.
Neto, S. et al. Association between use of lung-protective ventilation with lower tidal volumes and clinical outcomes among patients without acute respiratory distress syndrome. JAMA, Oct. 24/31; 308;16.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Visual Diagnosis
Posted: 11/19/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Do you like placing ultrasound-guided IV catheters? Check out this trick for covering the probe during the procedure.
http://ultrarounds.com/Ultrarounds/The_Vascular_Probe_Protector.html
or
https://www.youtube.com/watch?v=ZuOq6Ea_FbA&feature=plcp
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: Torsades de pointes, prolonged QT syndrome (PubMed Search)
Posted: 11/18/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Congenital and Acquired Long QT Syndrome.Cardiology in Review. 12(4):222-34, 2004 Jul-Aug.
Category: Orthopedics
Keywords: tarsal tunnel syndrome (PubMed Search)
Posted: 11/17/2012 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
Tarsal Tunnel Syndrome (TTS)
Prior pearls have addressed Carpal Tunnel Syndrome and Cubital Tunnel Syndrome, which affect the median and ulnar nerves, respectively. Tarsal tunnel syndrome, is a similar compression neuropathy of the tibial nerve as it transverses through the tarsal tunnel of the foot.
The tarsal tunnel is located behind the medial malleolus, and is where the posterior tibial artery, tibial nerve and several tendons transverse. Patients will present complaining of numbness of the foot radiating into Digits 1-4, pain, burning , and tingling of the base of the foot and heel. TTS has many causes and is more common in athletes.
Consider the diagnosis in patients with foot pain and numbness. If interested in more information about TTS please consider reading this eMedicine article, http://emedicine.medscape.com/article/1236852-overview
Category: Pediatrics
Keywords: meningitis, neck pain, retropharyngeal abscess (PubMed Search)
Posted: 11/16/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
A 1 year old gets sent from their pediatrician’s office for rule out meningitis. They presented with fever for 2 days and neck rigidity. Your LP results are normal. What additional test should you consider?
Answer:
Lateral neck x-ray
http://www.hawaii.edu/medicine/pediatrics/pemxray/v2c20.html
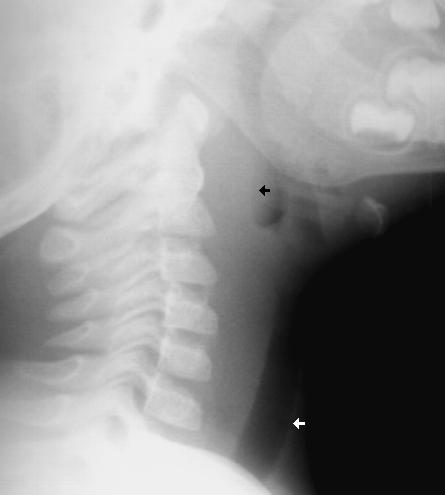
Retropharyngeal abscess (RPA) can commonly present like meningitis. Have a high suspicion in
children who are too young to complain of sore throat or difficulty swallowing.
A recent article in Pediatric Infectious Disease Journal detailed the rising incidence of retropharyngeal abscess, especially in younger patients, which is attributed to community acquired MRSA.
From 2004-2010 there was a 2.8 fold increase in RPA from the previous study period (1993-2003).
Children whose abscess grew MRSA were younger (mean 11 months) than the others (mean 62 months) (P < 0.001) and required longer duration of hospitalization (mean 8.8 days) than the rest (mean 4.5 days) (P = 0.002).
Bottom line: Consider a plain film in the child you are preparing to LP for meningitis.
Reference:
Abdel-Haq, N, Quezada M, Asmar BI. Retropharyngeal abscess in children: the rising incidence
of methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2012; 31: 696–699
Category: International EM
Posted: 11/14/2012 by Walid Hammad, MD, MBChB
Click here to contact Walid Hammad, MD, MBChB
· Explosions can cause a complex series of injuries, which may include subtle or delayed findings. Repeated evaluations, such as serial abdominal exams, may be required.
· Blast injuries are divided into 4 categories:
o Primary blast injuries: Injury from blast wave over-pressure. Found in gas filled structures (ear, lung, hollow organs)
o Secondary blast injuries: Injury from thrown objects (primarily penetrating trauma, but may blunt)
o Tertiary blast injuries: Injuries from patient being thrown by blast wave (blunt trauma)
o Miscellaneous (quaternary) blast injuries: Injuries from other causes, such as burns, crush injuries, rhabdomyolysis, and toxic chemicals.
· The most common primary blast injury is tympanic membrane rupture.
University of Maryland Section for Global Emergency Health
Author: Jon Mark Hirshon
Category: Critical Care
Posted: 11/13/2012 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Burn Patients and Antibiotic Dosing
Jamal JA, et al. Improving antibiotic dosing in special situations in the ICU: burns, renal replacement therapy and extracorporeal membrane oxygenation. Curr Opin Crit Care 2012; 18:460-71.
Category: Visual Diagnosis
Posted: 11/12/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
33 year-old male found unconscious by EMS and complains of right shoulder pain upon waking up in the ED. Diagnosis?
Answer: Posterior shoulder dislocation
Follow me on Twitter (@criticalcarenow) or Google+ (+Haney Mallemat)
Category: Cardiology
Posted: 11/11/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Bazett's Formula QTc = QT/RR1/2
Category: Cardiology
Keywords: Long QT Syndrome (PubMed Search)
Posted: 11/11/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Congenital and Acquired Long QT Syndrome.Cardiology in Review. 12(4):222-34, 2004 Jul-Aug
Category: Orthopedics
Keywords: calf tear, muscle tear (PubMed Search)
Posted: 11/10/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Injury is often caused by sudden dorsiflexion on a plantar flexed foot w/ the knee in extension or similarly sudden knee extension with the ankle in a dorsiflexed position.
Injury has a predilection for the poorly conditioned middle-aged athlete, with "thick calves" who are engaged in strenuous activity
Strains are treated with ice, analgesics, and compression (decreases hematoma size and facilitates healing)
Also, consider casting/splinting as dictated by injury severity, such as with a night splint or a CAM boot.
Severe strains and ruptures can be splinted in plantar flexion for 3 weeks.
Gallo et al. Common Leg injuries of long-distance runners:Anatomic and Biomechanical approach. Sports Health. 2012
Category: Toxicology
Keywords: PCP, phencyclidine, haloperidol (PubMed Search)
Posted: 11/7/2012 by Bryan Hayes, PharmD
(Updated: 11/8/2012)
Click here to contact Bryan Hayes, PharmD
Background
Patients who are intoxicated with, or emerging from, phencyclidine (PCP) highs present with acute agitation that can be challenging to treat
Risks of physical restraints for combative patients include injury, hyperthermia, rhabdomyolysis, and increased agitation or excited delirium
Haloperidol is an option for chemical restraint that is typically safe and rapid acting
Some concerns related to haloperidol use in PCP-intoxicated patients include worsened PCP-induced hyperthermia, dystonic or anticholinergic reactions, lower seizure threshold, and hypotension
Data
A recent retrospective case series assessed the frequency of adverse effects from the combination of PCP and haloperidol
Of 59 cases, only two patients experienced an adverse reaction, and neither could be conclusively linked to haloperidol administration
This analysis had several major limitations including retrospective design for identifying adverse reactions, potential for false positive PCP screens, and possible haloperidol administration more than 24 hours after PCP intoxication
Bottom Line
While haloperidol may be safe for agitated PCP-intoxicated patients, this paper adds nothing to refute or support its use. Benzodiazepines and calm environment are still first-line therapy.
It should be noted that no data exist showing poor outcomes in PCP-intoxicated patients administered haloperidol, which begs the question "Is there even an issue?" Dr. Leon Gussow, author of The Poison Review, provides a nice answer and summary of the article here.
MacNeal JJ, et al. Use of haloperidol in PCP-intoxicated individuals. Clin Toxicol 2012;50:851-3.
Gussow L. The Poison Review. http://www.thepoisonreview.com/2012/11/07/is-haloperidol-dangerous-in-pcp-associated-agitation-a-non-answer-to-a-non-problem/ Accessed Nov 8, 2012.
Category: International EM
Keywords: Hantavirus, Sin Nombre, Pulmonary, Infectious Disease (PubMed Search)
Posted: 11/7/2012 by Andrea Tenner, MD
(Updated: 11/16/2012)
Click here to contact Andrea Tenner, MD
University of Maryland Section for Global Emergency Health
Author: Andi Tenner
Center for Disease Control. (2012). Hantavirus. Retrieved September 3, 2012, from http://www.cdc.gov/hantavirus/index.html
Berger, S. A., Calisher, C. H., and Keystone, J. H., (2003). Exotic Viral Disease: A Global Guide. Hamilton, Ontario: BC Decker.
Category: Critical Care
Posted: 11/6/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Previous pearls have described the increasing evidence against colloid (e.g., hydroxyethyl starch) use during resuscitation. Now it appears that the crystalloid 0.9% normal saline (NS) may be under fire.
The use of large volumes of NS has been associated with hyperchloremic metabolic acidosis and harm in animal studies. The risk of harm in humans, however, has been less clear.
Bellomo et al. conducted a prospective observational study in which patients being resuscitated in the control group received NS at the clinicians' discretion; i.e., chloride-liberal strategy. The use of NS was restricted in the intervention group, where other less chloride containing fluids were used for resuscitation (e.g., Ringer's Lactate); i.e., a chloride-restrictive strategy.
The authors found that when compared to patients in the chloride-liberal group, the chloride-restrictive group had significantly less rise in baseline creatinine, less overall AKI, and a reduced need for renal replacement therapy.
Bottom line: Although this was only an observational study, the liberal use of normal saline during resuscitation may increase the risk of AKI and renal replacement therapy.
Bellomo, R. et al. Association between a chloride-liberal vs. chloride-restrictive intravenous fluid administration strategy and kidney injury in critically ill adults. JAMA. 2012 Oct 17;308(15):1566-72. doi: 10.1001/jama.2012.13356.
Follow me on Twitter (@criticalcarenow) and Google+ (+haney mallemat)
