Category: Visual Diagnosis
Posted: 7/8/2012 by Haney Mallemat, MD
(Updated: 7/9/2012)
Click here to contact Haney Mallemat, MD
A previously healthy 3 year-old male presents with a one-day history of fever, drooling, and refusal to move his neck. The lateral neck x-ray is shown. What's the diagnosis?
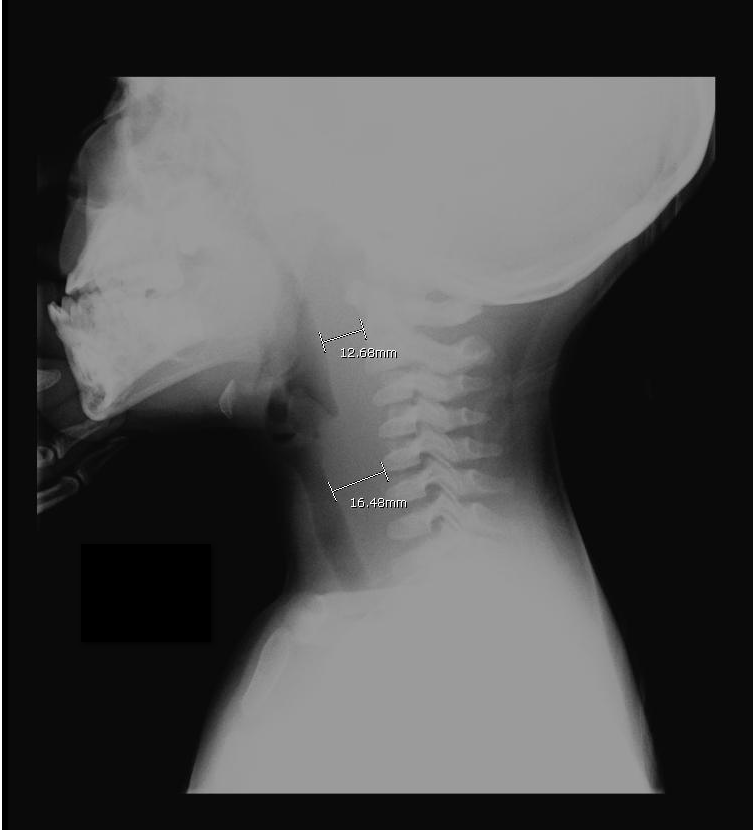
Answer: Retropharyngeal abscess
Retropharyngeal Abscess (RPA)
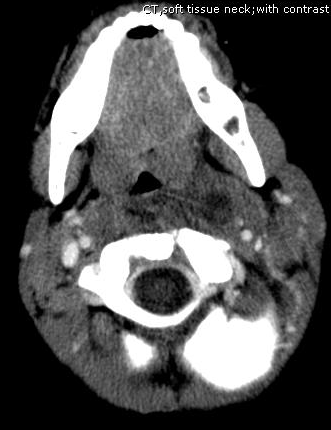
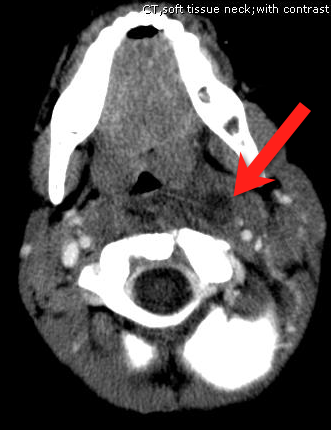
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Pharmacology & Therapeutics
Keywords: alteplase, tPA, warfarin, INR, ischemic stroke (PubMed Search)
Posted: 7/2/2012 by Bryan Hayes, PharmD
(Updated: 7/7/2012)
Click here to contact Bryan Hayes, PharmD
Issue 1: Mean INR in study patients was only 1.22 (median 1.2). An INR of 1.2 represents very little actual anticoagulation.
Issue 2: In the small subgroup of patients with INR 1.5 to 1.7 (n = 269) there was a higher risk of ICH (7.8%), but did not reach statistical significance (it was significant in the unadjusted risk population).
Bottom line: Patients with INRs < 1.5 may be ok to receive tPA. Patients with INRs 1.5 or greater need further study.
Xian Y, Liang L, Smith EE, et al. Risk of Intracranial Hemorrhage Among Patients With Acute Ischemic Stroke Receiving Warfarin and Treated with Intravenous Tissue Plasminogen Activator. JAMA. 2012;307(24):2600-8.
Follow me on Twitter (@PharmERToxGuy)
Category: Toxicology
Keywords: envenomation,stings,jellyfish (PubMed Search)
Posted: 7/5/2012 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
No one treatment has demonstrated consistency of pain relief from jellyfish stings over all species; conversely, a treatment for one species may worsen an envenomation from another.
Deionized water, seawater, meat tenderizer, and urea treatment do not appear to produce any improvement in pain sensation.
Ammonia, acetic acid, and ethanol may cause an increased stinging sensation, and in most species vinegar may cause nematocyst discharge.
Application of topical lidocaine reduced the local sensation of pain (10% and 15% produced immediate pain relief), and hot water results in pain relief in the majority of patients tested.
Ward NT, Darracq MA, Tomasewski C, Clark RF. Evidence-Based Treatment of Jellyfish Stings in North America and Hawaii. Article published online, Annals of Emergency Medicine June 8, 2012.
Category: Critical Care
Keywords: hydroxyethyl starch crystalloid, colloid, lactated ringers, normal saline, resuscitation, sepsis, hypotension (PubMed Search)
Posted: 7/3/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Septic patients with hemodynamic instability often require intravenous fluids as part of their resuscitation. Major debate has occurred whether the optimal resuscitation fluids are crystalloids (e.g., normal saline) or colloids (e.g., albumin).
In theory, colloids are more potent intravascular expanders than crystalloids because their oncotic pressure is higher and should increase intravascular volume similarly to larger amounts crystalloid (i.e., colloids require less volume during resuscitation).
Despite these theoretical benefits, the colloid hydroxyethyl starch (HES), has come under scrutiny after prior studies have linked its use with adverse outcomes.
A recent prospective randomized-control trial compared the use of HES to lactated acetate for resuscitating septic patients and found that HES significantly increased both the incidence of renal-replacement therapy and mortality at 90 days (both primary end-points in the study).
Bottom line: There is no convincing data that HES performs superiorly to crystalloid for resuscitation in sepsis and there is increased harm with its use. Furthermore, the increased cost of HES compared to crystalloids does not justify its routine use.
Perner A., et al. Hydroxyethyl Starch 130/0.4 versus Ringer's Acetate in Severe Sepsis. NEJM. 2012 Jun 27.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Visual Diagnosis
Posted: 7/2/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Have you ever had to give a national presentation, but can't find that one ultrasound clip or image that you really need? You could "borrow" it from someone on the internet, but you are secretly afraid that the "owner" of the clip is lurking somewhere in the audience. Well, the guys at the Ultrasound Podcast (www.ultrasoundpodcast.com) have come to your rescue by creating SonoCloud, a free access ultrasound library. At Sonocloud, you will find several categories of ultrasound clips and images for you to view and share,...and again it's FREE. In fact, the only thing you are expected to do is upload some of your own ultrasounds to share.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: cocaine (PubMed Search)
Posted: 7/1/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
[Pearls provided by Dr. Semhar Tewelde]
Cocaine...
1. causes systolic and diastolic dysfunction, arrhythmias, and atherosclerosis even in young users with relatively few cardiac risk factors, typically TIMI risk score <1
2. decreases myocardial contractility and ejection fraction by blocking sodium and potassium channels within the myocardium
3. prolongs the PR, QRS, and QT intervals on the ECG
4. users have a higher overall incidence of MI (odds ratio 3.8 to 6.9)
5. -induced chest pain is associated with acute MI in approx. 6% of cases
6. increases the risk of MI by 24-fold in the first hour after use
7. contributes to approx. 1 of every 4 MIs between 18 and 45 years of age
Cardiovascular Effects of Cocaine. Schwartz B, et al. Circulation. 2010;122:2558-2569.
Category: Orthopedics
Keywords: Bennett, Rolando, fracture (PubMed Search)
Posted: 6/30/2012 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
First Metacarpal Fractures:
There are two types of fractures that commonly occur at the base of the 1st metacarpal. They are:
Bennett Fracture: This is an intraarticular fracture at the base of the 1st metacarpal that always involves some degree of subluxation or dislocation of the 1st carpometacarpal joint.
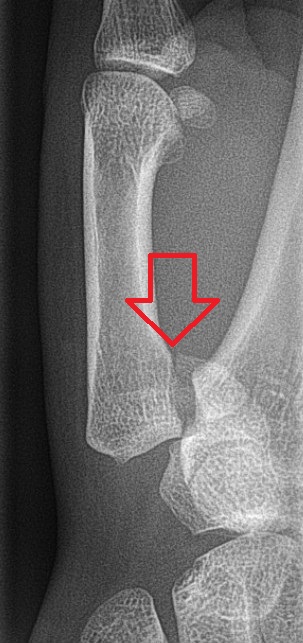
Image from Wikipedia Commons
Rolando Fracture: This is a communited intraarticular fracture at the base of the first metacarpal that typically has a T or Y shaped configuration with 3 fragments.

Image courtesy of WikiPedia Commons
Category: Pediatrics
Posted: 6/29/2012 by Rose Chasm, MD
(Updated: 5/4/2026)
Click here to contact Rose Chasm, MD
Submitted by Dr. Lauren Rice
The summertime can be full of lots of fun activities (beach, fireworks, cookouts, and campfires) that can put children at risk of burns.
Burn depth classification:
1. Superficial (first-degree): red and blanching with minor pain, resolves in 5-7 days
2. Partial thickness (second-degree): red and wet with blisters, very painful, resolves in 2-5 weeks
Treatment: clean with soap and water twice daily, and apply silvadene wrap with gauze, kerlex
3. Full thickness (third-degree): dry and leathery without pain, no resolution after 5-6 weeks, may require graft
Treatment: wound debridement and dressings as above
Parkland formula: 4ml/kg/%TBSA in 1st 24 hours with 50% of total volume in 1st 8 hours
Calculate burn surface area:
-SAGE: free computerized burn diagram available at www.sagediagram.com
-Rule of Nines > 14 years old
-Rule of Palm <10 years old
Burn Center Referral
-Extent: partial thickness of >30% TBSA or full thickness of >10-20%
-Site: hands, feet, face, perineum, major joints
-Type: electrical, chemical, inhalation
1. Cross, J.T. and Hannaman, R.A. MedStudy Pediatrics Board Review Core Curriculum, 5th edition, p. 3-11, 3-12.
2. Children’s National Medical Center, Department of Trauma and Burn Surgery. Trauma Cheat Sheet.
Category: Pediatrics
Posted: 6/23/2012 by Mimi Lu, MD
(Updated: 6/29/2012)
Click here to contact Mimi Lu, MD
Pathology at the umbilicus can manifest as inflammation, drainage, a palpable mass, or herniation.
Omphalitis - A cellulitis of the umbilicus. Mild cases often respond to local application of alcohol to clean the area, but due to the possibility of rapid progression and abdominal wall necrotizing fasciitis, admission for observation and IV antibiotics is usually warranted. Cover staph, strep, and GNRs.
Umbilical granuloma - As the umbilical ring closes and the cord sloughs off, granulation tissue formation is a normal part of umbilical epithelialization. There is sometimes an overgrowth of granulation tissue which can be treated once or twice with silver nitrate. Should the tissue not regress after a 1-2 treatments, the patient should be referred to pediatric surgery for excision and evaluation of other pathology (urachal or vitelline remnants).
Umbilical fistula - This is a patent vitelline duct and is characterized by persistent drainage that is bilious or purulent. A fistulogram using a small catheter and radio opaque dye can sometimes be helpful in determining the source of drainage (dye should be seen in the small bowel).
Umbilical polyp - Often confused with an umbilical granuloma with its glistening cherry red appearance, this is actually a vitelline duct remnant and contains small bowel mucosa. It does not regress with silver nitrate.
Vesicoumbilical fistula/sinus - The urachal versions of the umbilical fistula. This are a failure of complete closure of the urachus, resulting in persistent drainage of urine from the umbilicus, and infection (including recurrent UTIs). A fistulogram can be helpful for diagnosis.
Category: Toxicology
Keywords: thrombocytopenia, sulfa, bactrim (PubMed Search)
Posted: 6/28/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Though an uncommon event, Drug-Induced Autoimmune thrombocytopenia occurs in a variety of drugs. Having recently diagnosed a patient that was receiving the "double-dose" bactrim for an MRSA abscess, it is worth mentioning the other drugs that have been reported to do it. Platelet count can go down to lethal levels and result in death due to the coagulopathy. Treatment is effective with platelets and no contraindication like in TTP.
Drugs that have been reported to do it:
abciximab, acetaminophen, amiodarone, amphotericin B
Carbamazepine, danazol, diclofenac, digoxin
Methyldopa, procainamide
Rifampin, trimethoprim-sulfamethoxazole, vancomycin
Category: Critical Care
Posted: 6/26/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Acute Kidney Injury and Tumor Lysis Syndrome
McCurdy MT, Shanholtz CB. Oncologic emergencies. Crit Care Med 2012; 40:2212-2222.
Category: Visual Diagnosis
Posted: 6/24/2012 by Haney Mallemat, MD
(Updated: 6/25/2012)
Click here to contact Haney Mallemat, MD
77 year old male presents to the Emergency Department one week after a motor vehicle crash in which he suffered minor facial injuries. He is now concerned because his eye looks like this. Diagnosis?
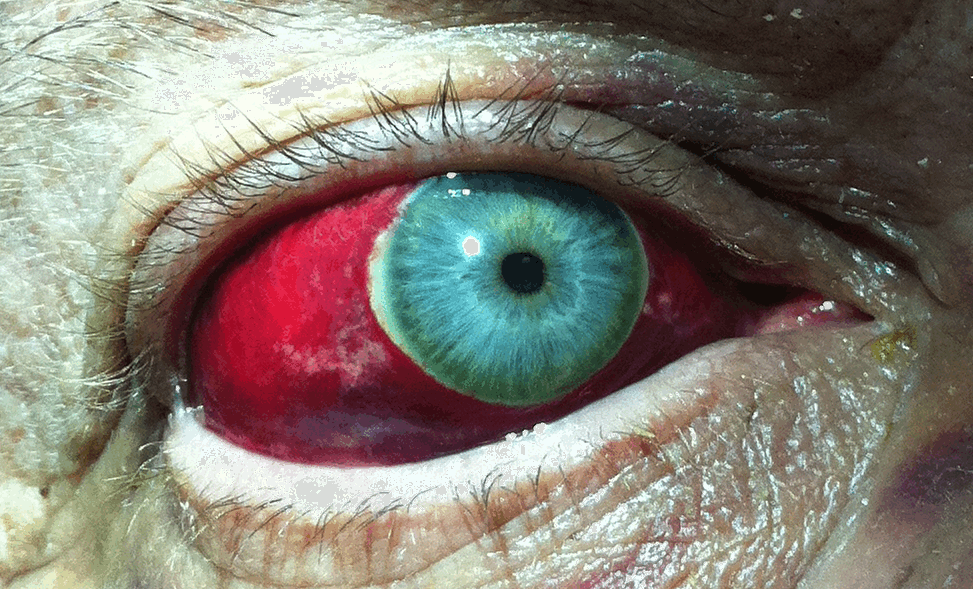
Answer: Subconjunctival Hemorrhage
Subconjunctival hemorrhage is the accumulation of blood between the conjunctiva and sclera (i.e., subconjunctival space) secondary to bleeding from conjunctival or episcleral blood vessels.
Subconjunctival hemorrhage may be caused by:
Treatment should be directed towards reversing the underlying cause and providing symptomatic relief (e.g., artificial tears)
Prognosis is typically good. Occasionally the hemorrhage becomes yellowish-green (similar to a bruise) during the healing phase; this eventually resolves.
Bonus Pearl: As July 1rst approaches a new class of doctors will begin their journey to become Emergency Medicine specialists. The EM Basic website, created by Dr. Steve Carroll, was developed as a boot camp guide for Emergency Medicine. At the EM Basic website, you can find podcasts and discussions of must know topics within Emergency Medicine. Check it out today at http://embasic.org or on iTunes
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: Sgarbossa Criteria, MI, LBBB (PubMed Search)
Posted: 6/24/2012 by Semhar Tewelde, MD
(Updated: 7/15/2012)
Click here to contact Semhar Tewelde, MD
LBBB is defined by 3 criteria QRS >125msec, V1- QS or rS, and R wave peak time 60ms with no q wave in leads I, V5, V6
Sgarbossa E, et al. ELECTROCARDIOGRAPHIC DIAGNOSIS OF EVOLVING ACUTE MYOCARDIAL INFARCTION IN THE PRESENCE OF LEFT BUNDLE-BRANCH BLOCK. NEJM Feb 22, 1996: Vol 334; No. 8
Category: Orthopedics
Keywords: knee, cartilage, physical activity (PubMed Search)
Posted: 6/23/2012 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
I am often asked whether physical activity has a positive or negative effect on the overall health of knee cartilage. The answer is unclear. Published data are conflicting.
What is known and generally agreed on:
1) Physical activity has been shown to facilitate cartilage development in children
2) Forced immobility (spinal cord injury) results in rapid cartilage loss
3) The medial knee compartment experiences significant mechanical loads during weight-bearing activity and is often the primary site of knee OA
A recent study attempted to answer whether 1) long-term (10yrs) participation in vigorous physical activity would benefit knee cartilage in healthy adults and 2) whether there were certain subgroups with asymptomatic preexisting structural knee changes which predict a harmful cartilage response to long-term physical activity.
Vigorous = activity generating sweating or SOB at least 20min 1/wk
Healthy older adults (mean age 57.8 yr) performing persistent vigorous physical activity had an increased risk (odds ratio 1.5) of worsening medial knee cartilage defects but not of a change in cartilage volume
In those w/ asymptomatic preexisting structural knee changes, there was worsening of cartilage defects (odds ratio 3.4) and a trend toward increased rate of loss of cartilage volume (again in the medial knee compartment)
Long-term effects of vigorous physical activity may depend on the preexisting health of the joint
Teichtahl, A.J., et al. Effect of long-term vigorous physical activity on healthy adult knee cartilage. Medicine and Science in Sports and Exercise. June 2012
Category: Pediatrics
Keywords: abdominal pain, vomiting, bloody stool, altered mental status, lethargy (PubMed Search)
Posted: 6/22/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Intussusception is the telescoping or prolapse of one portion of the bowel into an immediately adjacent segment.
Category: Toxicology
Keywords: transplant, cyclosporine, tacrolimus (PubMed Search)
Posted: 6/21/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Transplant patients are the norm now in the ED. Their drug lists are immense and are usually on some form of immunosuppression to prevent rejection of the transplanted organ. Two common medications are cyclosporine and tacrolimus. They share many adverse effects like hepatotoxicity, nephrotoxicity and hypertension. Here is the mechanism of action and some unique adverse effects to these powerful immunosuppressants (there are many more so be wary):
1) Cyclosporine - suppresses T-cell activation and growth. Unique toxicity - painful neuropathy of the fingertips and toes, cortical blindness
2) Tacrolimus - simiar to cyclosporine but actually hampers T-cell communication/signal transduction. Unique toxicity - can also cause cortical blindness but is also known to cause diabetes/hyperglycemiad
Category: Critical Care
Posted: 6/19/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Two recently presented abstracts at the 2012 Society of Critical Care Medicine conference suggest that the combination of vancomycin and piperacillin-tazobactam may lead to acute kidney injury (AKI) in the critically ill. There may also be evidence to suggest that piperacillin-tazobactam alone increases the risk of AKI.
Both abstracts retrospectively compared patients who received either vancomycin alone or the combination of vancomycin and piperacillin-tazobactam. In both studies, the rates of AKI were significantly lower in patients treated with vancomycin alone as compared to patients receiving both vancomycin and piperacillin-tazobactam.
Bottom line: Although the current evidence does not support a change in our clinical practice, more prospective studies exploring this topic are necessary.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Min, et al. Acute Kidney Injury in Patients Recieving Concomitant Vancomycin and Piperacillin/Tazobactam. Critical Care Medicine. December 2011. 39(12); p 200
Hellwig, et. al. Retrospective Evaluation of the Incidence of Vancomycin and/or Piperacillin-Tazobactam Induced Acute Renal Failure. Critical Care Medicine. December 2011. 39(12); p 79
Category: Visual Diagnosis
Posted: 6/18/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
79 year old male with headaches, ataxia, falls, and difficulty urinating. What's the diagnosis?
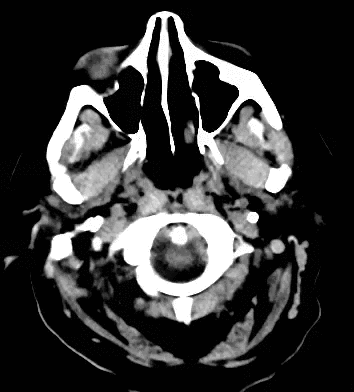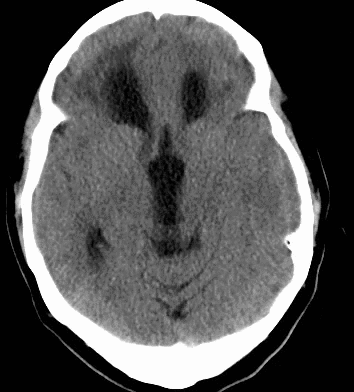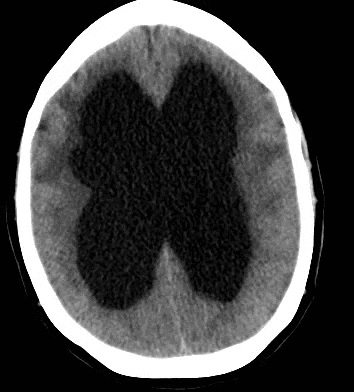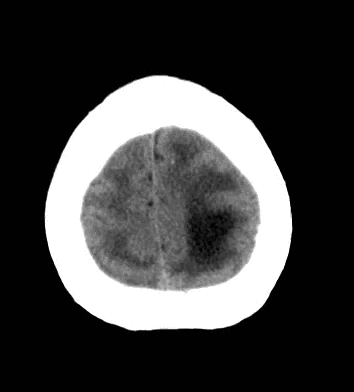
Diagnosis: Ventriculomegaly secondary to Normal Pressure Hydrocephalus
An approach to ventriculomegaly
Ventriculomegaly is due to cerebral atrophy (e.g., Parkinson disease) or increased cerebrospinal fluid (CSF) within the ventricles. Increased CSF is due to:
Congenital causes of ventriculomegaly:
Acquired causes of ventriculomegaly:
Category: Cardiology
Keywords: chest pain, acute coronary syndrome, history of present illness, predictor (PubMed Search)
Posted: 6/17/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
For patients presenting to the ED with chest pain, we've been taught that “classic” or “typical” presentations for ACS (chest pressure with radiation to the left neck/jaw/shoulder/arm, dyspnea, diaphoresis, nausea, vomiting, lightheadedness) are most worrisome. Yet, many of the patients that present with typical symptoms end up having negative workups for ACS. What are the symptoms that truly predict ACS? Three major studies have demonstrated that the best predictors of ACS in patients presenting to the ED with chest pain are (not necessarily ranked in order):
1. chest pain that radiates to the arms, especially if the pain radiates bilaterally or to the right arm
2. chest pain associated with diaphoresis
3. chest pain associated with vomiting
4. chest pain associated with exertion
The description of the chest pain (e.g. "pressure" or "squeezing," etc.), the dyspnea, nausea, lightheadedness, and pain at rest were, surprisingly, not helpful at predicting ACS.
The simple takehome point is the following: always ask your patient with chest pain if the pain radiates, if there was associated diaphoresis, if there was associated vomiting, and if the pain is associated with exertion. If the answers to any of these 4 questions is "yes," think twice before labeling the patient with a non-ACS diagnosis.
1. Swap CJ, Nagurney JT. Value and limitations of chest pain history in the evaluation of patients with suspected acute coronary syndromes. JAMA 2005;294:2623-2629.
2. Body R, Carley S, Wibberley C, et al. The value of symptoms and signs in the emergent diagnosis of acute coronary syndromes. Resuscitation 2010;81:281-286.
3. Panju AA, Hemmelgarn BR, Guyatt GH, et al. Is this patient having a myocardial infarction? JAMA 1998;280:1256-1263.
Category: Misc
Keywords: contrast media, iodine, shellfish (PubMed Search)
Posted: 6/16/2012 by Michael Bond, MD
Click here to contact Michael Bond, MD
Contrast Allergy:
Many patients will report that they have a allergy to iodinated contrast by saying that they are allergic to iodine
Iodine, itself, is not an allergen and is a required element for thyroid homrone production. Plus could you imagine the hordes of people that would be having allergic reactions everyday when they add salt to their french fries. Our EDs would be completely swamped.
A recent meta-analysis by Drs. Schabelman and Witting also showed the following:
As we enter Crab eating season in Maryland, lets stop giving shellfish a bad name. A patent with any allergy is at increased risk, but shellfish is no higher a risk than those allergic to Strawberries.
Schabelman E, Witting M. The relationship of radiocontrast, iodine, and seafood allergies: a medical myth exposed.J Emerg Med. 2010 Nov;39(5):701-7. Epub 2010 Jan 4.
