Category: Pediatrics
Keywords: orthopedics, fracture, reduction, elbow (PubMed Search)
Posted: 6/15/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Definition: Fracture of the humerus just proximal to the epicondyles.
Category: Toxicology
Keywords: azithromycin, cardiovascular, death (PubMed Search)
Posted: 6/12/2012 by Bryan Hayes, PharmD
(Updated: 6/15/2012)
Click here to contact Bryan Hayes, PharmD
Ray WA, Murray KT, Hall K, et al. Azithromycin and the Risk of Cardiac Death. N Engl J Med 2012;366:1881-90.
Follow me on Twitter (@pharmERtoxguy).
Category: Critical Care
Posted: 6/13/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Use the Measured Sodium Concentration!
Beck, L. Cleveland Clin J Med 2001;68:673.
Category: Visual Diagnosis
Posted: 6/11/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
19 year-old male presents with L ankle pain and obvious deformity after jumping out of a window and landing on his inverted foot. What's the diagnosis?
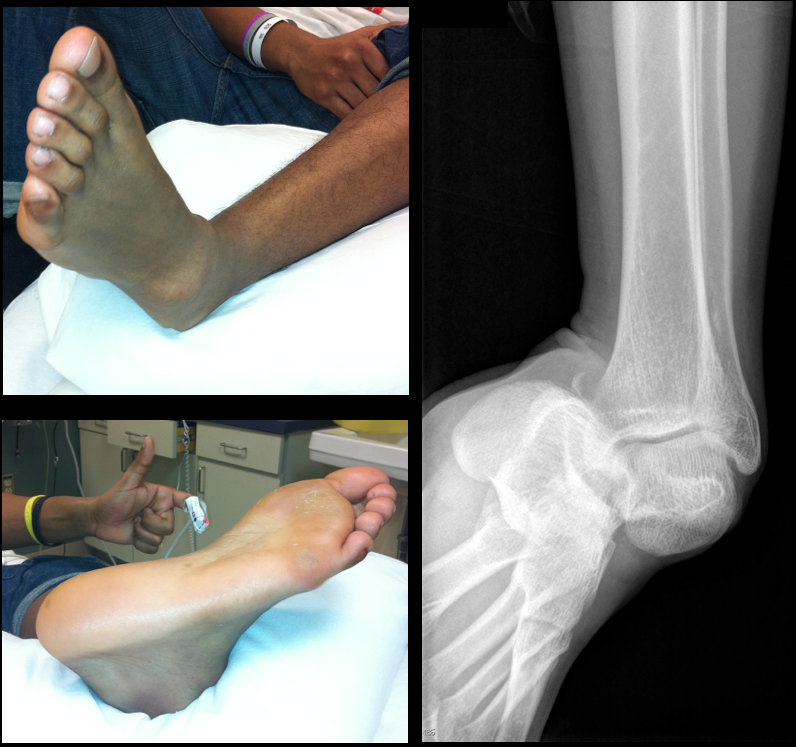
Sub-talar dislocation
Wheeless' Textbook of Orthopedics
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: hypothermia, cardiogenic shock (PubMed Search)
Posted: 6/10/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
New studies are utilizing mild therapeutic hypothermia as a treatment option in cardiogenic shock. These studies have reported improved circulatory support, an increase in systemic vascular resistance, and reduction in vasopressor use which ultimately may result in lower cardiac oxygen consumption. The preliminary results suggest that mild therapeutic hypothermia could be a therapeutic option in hemodynamically unstable patients independent of current recommendations which support its use in cardiac arrest survivors.
Mild therapeutic hypothermia in cardiogenic shock syndrome.
Category: Orthopedics
Keywords: back, vertebae, fracture (PubMed Search)
Posted: 6/9/2012 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
• Wedge compression fractures
http://jbjs.org/data/Journals/JBJS/855/JBJA0851224560G02.jpeg
Category: Toxicology
Keywords: Warfarin,vitamin K,coagulation,INR,supratherapeutic (PubMed Search)
Posted: 6/7/2012 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
It may not be necessary to give oral vitamin K to patients that are not bleeding that have INRs between 4.5 and 10.
Patients who were supratherapeutic on warfarin were randomized to vitamin K 1.25 mg (n=355) versus placebo (n=369).
In the 90 days after enrollment, 15.8% of patients allocated to vitamin K and 16.3% allocated to placebo had a bleeding event. Major bleeding events occurred in 9 patients in the vitamin K group and 4 in the placebo.
Thromboembolic events occurred in 1.1% of patients in the vitamin K group, compared to 0.8% of patients in the placebo group. An equal number of patients died in each group (n=7).
Crowther MA, Ageno W, Garcia D, et. al. Oral Vitamin K Versus Placebo to Correct Excessive Anticoagulation in Patients Receiving Warfarin. Ann Intern Med 2009, 150:293-300.
Category: Critical Care
Posted: 6/4/2012 by Haney Mallemat, MD
(Updated: 6/5/2012)
Click here to contact Haney Mallemat, MD
Consider rhabdomyolyisis secondary to heat exposure as summertime approaches; have a low threshold to screen patients if they are at risk (e.g., people exercising in high-ambient temperatures).
Symptoms include muscle tenderness, cramping, and swelling with associated weakness. Patients with altered mental status (e.g., heat stroke) should be examined for limb induration, skin discoloration (i.e., ischemia), or compartment syndrome.
Complications:
Treatment
Khan, F. Y. Rhabdomyolysis: a review of the literature. The Netherlands journal of medicine, 67(9), 272 – 283.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: myocarditis (PubMed Search)
Posted: 6/3/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
Kindermann I, Barth C, Mahfoud F, et al. Update on Myocarditis. JACC:59;9 Feb 28, 2012.
Category: Pharmacology & Therapeutics
Keywords: naltrexone, methylnaltrexone, constipation, opioid dependence (PubMed Search)
Posted: 6/1/2012 by Bryan Hayes, PharmD
(Updated: 6/15/2012)
Click here to contact Bryan Hayes, PharmD
Naltrexone and methylnaltrexone are both mu-receptor antagonists that look similar and have similar names. But, they have very different uses.
Follow me on Twitter (@pharmERtoxguy).
Category: Critical Care
Posted: 5/29/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Severe UGIB
Srygley FD, et al. Does this patient have a severe upper gastrointestinal bleed? JAMA 2012;307:1072-9.
Category: Visual Diagnosis
Posted: 5/28/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Ultrasound is useful during intubation; here is a video explaining how: http://ultrarounds.com/ultrarounds.com/Visual_Pearl_May_28,_2012.html
Today's Bonus Pearl:
EMRA has developed a great antibiotic guide for the iphone (http://itunes.apple.com/us/app/2011-emra-antibiotic-guide/id393020737?mt=8) or android (https://play.google.com/store/apps/developer?id=Emergency+Medicine+Residents'+Association). This app is a bit pricey ($15.99), but is easy to use and well organized. Enjoy!
Chou, H. et al. Tracheal rapid ultrasound exam (T.R.U.E.) for confirming endotracheal tube placement during emergency intubation. Resuscitation. Jun 2011
Werner SL,et al. Pilot study to evaluate the accuracy of ultrasonography in confirming endotracheal tube placement. Ann Emerg Med 2007;49:75–80.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: myocarditis (PubMed Search)
Posted: 5/27/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
[pearl provided by Dr. Semhar Tewelde]
Myocarditis is an under-diagnosed cardiac disease resulting from a broad range of infectious, immune, and toxic etiologies
Kindermann I, Barth C, Mahfoud F, et al. Update on Myocarditis. JACC:59;9 Feb 28, 2012.
Category: Orthopedics
Keywords: hamate, wrist, fracture (PubMed Search)
Posted: 5/26/2012 by Brian Corwell, MD
(Updated: 5/4/2026)
Click here to contact Brian Corwell, MD
Hamate Fractures
Occur in two locations: the body of the hamate and the hook (hamular process) of the hamate
Fractures are present in 2 to 4% of carpal bone fractures
Body fractures are less common and are associated with dislocation of the fourth and fifth metacarpals
Axial force transmitted down the metacarpal shaft (a fall or fist strike)
Hook fractures occur from a direct force from an object strikes the palm such as that from a bat, golf club or racket
Have increased suspicion in these athletes who present w/ ulnar sided wrist pain
Diagnosis is frequently missed; chronic fractures are associated w/ flexor tendon rupture and ulnar neuropathy
PE: Tenderness localized over the hamate (in the hypothenar eminence) and over the dorsal ulnar aspect of the wrist. Swelling may be present. Look for resisted flexion of the 5th digit when the wrist is held in ulnar deviation. May note sensory changes in ulnar nerve distribution
Imaging: PA and lateral views of the wrist will show a body fracture but will frequently MISS a fracture of the hook of the hamate. In those with a clinical suspicion for this entity, order a “carpal tunnel view.” In the proper clinical setting, CT imaging is excellent for those with high suspicion and normal plain films.
Category: Pediatrics
Keywords: breastfed, formula, obesity, weight gain (PubMed Search)
Posted: 5/25/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Proper Feeding of the Newborn
The emergency physician must be comfortable with providing anticipatory guidance to parents of newborn, especially with regards to proper feeds of the neonate.
Newborns will lose some weight in the first 5-7 days of life. A 5% weight loss is considered normal for a formula fed newborn. A 7%-10% loss is considered normal for the breastfed baby. Most babies regain their birth weight by days10-14 of life. During the first 3 months, infants gain about an ounce a day (30 g) or 2 pounds a month (900 g). By age 3-4 months, healthy term infants have doubled their birth weight.
Breast-fed Neonates:
- Should be fed every 2-3 hours while awake
- 5-20 minutes of sucking per breast
- May gain weight slower than formula-fed counterparts
Formula-fed Neonates:
- 0.5-1 ounces per feeding every 3-4 hours for the 1st week
- Then 1-3 ounces per feeding every 3-4 hours
- Typical formula contains 20 cal/ounce
In general, overfeeding during the neonatal period has been associated with adult obesity. The American Academy of Pediatrics recommends exclusive breastfeeding for at least the 1st 6 months of life. Earlier switches to formula has been associated with atopy, diabetes and obesity
References:
- Fleischer DM. “Introducing formula and solid foods to infants at risk for allergenic disease.” UptoDate;2012.
- Hammer LD, et al. “Development of feeding practices during the first 5 years of life.” Nutrition;1999;189-194.
- Philips SM and Jensen C. “Dietary history and recommended dietary intake in children.” UptoDate;2011.
- Prior LJ and Armitage JA. “Neonatal overfeeding leads to developmental programming of adult obesity.” J Physiol;2009:2419.
Category: Toxicology
Keywords: Nitrous Oxide (PubMed Search)
Posted: 5/24/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
Nitrous Oxide(N2O) is a common gas utilized to assist with procedural sedation especially in the pediatric population and dental offices. It has a long track history of safety but also has been abused.
N2O is 35x more solube in blood than N2. This means any air-filled space can have pressure increase thus complications like pneumothorax, TM rupture and bowel distention can occur.
When abused chronically can cause bone marrow suppression, B12 deficiency and resulting in polyneruopathy.
On the street, "whip its" are N2O from whipped cream containers. Balloons filled with N2O are inhaled which combine nitrous oxide and hypoxia effects.
Category: Critical Care
Posted: 5/21/2012 by Haney Mallemat, MD
(Updated: 5/22/2012)
Click here to contact Haney Mallemat, MD
Carcinoid tumors are neuroendocrine malignancies typically located in the GI tract; most commonly in the terminal ilium and appendix.
Carcinoid tumors produce serotonin, histamine, bradykinin, and/or prostaglandin that result in diarrhea, facial flushing, or bronchospasm. These vasoactive substances may also lead to hypotension and vasodilatory shock.
The tumor may also affect the tricuspid and pulmonary valves leading to right-heart failure secondary to valvular regurgitation, stenosis or both.
Treatment is directed at controlling the malignancy (e.g., octotrotide and tumor resection) as well as managing the right-sided heart failure when it occurs (e.g., inotropes, diuretics, vasopressors, etc.).
Fox, D. J. (2004). Carcinoid heart disease: presentation, diagnosis, and management. Heart, 90(10), 1224–1228
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Cardiology
Keywords: peripartum cardiomypathy, cardiomyopathy (PubMed Search)
Posted: 5/20/2012 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
Category: Pediatrics
Keywords: apparent life threatening event (PubMed Search)
Posted: 5/18/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
There has been no link found between Sudden Infant Death Syndrome (SIDS) and an Acute Life Threatening Event (ALTE)
There are several factors that dispute previous claims of each being manifestations of the same disease state:
1) Timing: approx 75-80% of SIDS deaths occur between midnight and 6 AM; 80-85% of ALTE occur between 8 AM and 8 PM
2) Prevention: Interventions to prevent SIDS (ex, “back to sleep”) have not resulted in a decreased incidence of ALTE
3) Risk factors:
a. SIDS: prone sleeping, bottle feeding, maternal smoking
b. ALTE: repeated apnea, pallor, history of cyanosis, feeding difficulties
BONUS PEARL: A thorough history and physical will lead to the diagnosis for the source of the ALTE in 21%
Pertinent historical items: detailed bystander history of event (parents, EMS), activity and behavior prior to event and any past medical issues or medications (focus on GERD and pulmonary)
Pertinent physical exam: detailed neurological and cardiopulmonary system eval with focus on signs of non-accidental trauma (retinal hemorrhaging, bulging fontanel, bruising) as up to 10% of ALTEs involve some form of abuse
Category: Toxicology
Keywords: vitamins (PubMed Search)
Posted: 5/17/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
More and more people are going to holistic medicine and "naturopaths". These have been an interesting source of toxicology case reports due to therapeutic misadventures. Vitamins have been an ever increasing adjunct to these health philosophies. The following are the vitamins and their related toxicity in overdose:
Vitamin A: Pseudotumor cerebri, increase ICH, hair thinning, hepatotoxicity
Vitamin D: Hypercalcemia
Vitamin E: can antagonize vitamin K particularly in vitamin K deficient people, could result in coagulopathy
Vitamin K: problem if supplement contains this and patient on coumadin, ask patient
Vitamin C: Association with increased kidney stones though controversial
