Category: Pediatrics
Keywords: premedication, RSI, ventilator, high flow nasal cannula (PubMed Search)
Posted: 9/21/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Toxicology
Keywords: arsenic, rice (PubMed Search)
Posted: 9/20/2012 by Fermin Barrueto
Click here to contact Fermin Barrueto
Just when you think buying organic protects you from chemicals and pesticide, along comes the studies detecting arsenic in rice products and specficially in organic foods with brown rice organic sweetener. An organic toddler milk formula reportedly had 6x EPA standards for safe drinking water limit.
The more toxic arsenic is the inorganic arsenic which can cause neuropathy but after chronic exposure can cause a classic arsenic keratosis - see attached pic. The inorganic is seen commonly in seafood and is more easily excreted by the body. Unfortunately, in the study referenced here, inorganic As was the predominant type.
Arsenic, organic foods, and brown rice syrup.
Jackson BP, Taylor VF, Karagas MR, Punshon T, Cottingham KL.
Environ Health Perspect. 2012 May;120(5):623-6. Epub 2012 Feb 13.
Category: Critical Care
Posted: 9/18/2012 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
The Lung Transplant Patient in Your ED
Fuehner T, et al. The lung transplant patient in the ICU. Curr Opin Crit Care 2012; 18:472-8.
Category: Visual Diagnosis
Posted: 9/17/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
27 year-old woman with AIDS presents complaining of a painful, puritic, and papular rash. What's the diagnosis?
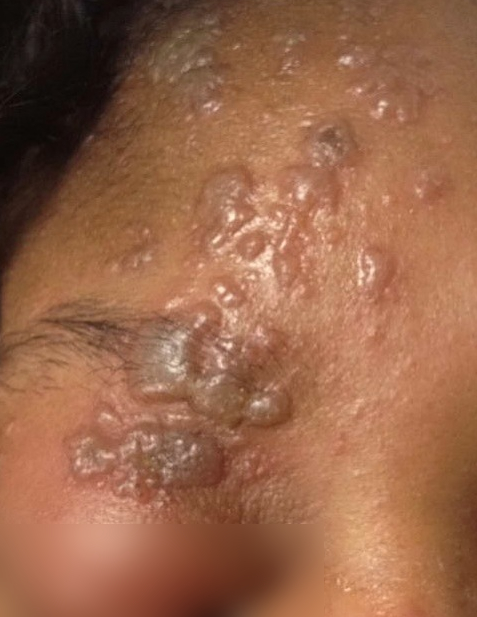
Answer: Herpes zoster ophthalmicus
Herpes Zoster Ophthalmicus
Follow me on Twitter (@criticalcarenow) or on Google+ (+haney mallemat)
Category: Airway Management
Keywords: Pericarditis (PubMed Search)
Posted: 9/16/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Pericarditis is based on clinical diagnosis; typically two of four criteria are found (pleuritic chest pain, pericardial rub, diffuse ST-segment elevation, and pericardial effusion).
Treatment of pericarditis should be targeted at the cause.
Most causes of pericarditis have a good prognosis and are self-limited.
Imazio M. Contemporary management of pericardial diseases. Current Opinion in Cardiology. 27(3):308-17, 2012 May.
Category: Misc
Keywords: CSF, lactate (PubMed Search)
Posted: 9/15/2012 by Michael Bond, MD
Click here to contact Michael Bond, MD
Lactate levels help to confirm septic arthritis but what about bacterial meningitis. As reported in the daily electronic ACEP newsletter a small study of 45 patients showed that all patients with a confirmed diagnosis of bacterial meningitis had a CSF lactate level > 3.5 mmol/L. Therefore, it might be true that viral meningitis will only have CSF lactate levels < 3.5 mmol/L.
With only 45 patients, this finding is clearly not ready for Prime Time but consider adding it to your next CSF study so more data can be collected on the utility of this test.
The story as seen in ACEP eNews on September 14th, 2012 is:
MedPage Today (9/14, Gever) reports, "Cerebrospinal fluid (CSF) levels of lactate were a perfect marker of viral versus bacterial meningitis in a small study, a researcher reported" at the Interscience Conference on Antimicrobial Agents and Chemotherapy. Researchers found that, "among 45 adults in whom the etiology of meningitis was microbiologically confirmed, all those with CSF lactate levels above 3.5 mmol/L had the bacterial form, whereas every patient with lower levels had viral meningitis."
Category: Pediatrics
Posted: 9/15/2012 by Rose Chasm, MD
(Updated: 5/4/2026)
Click here to contact Rose Chasm, MD
Category: Toxicology
Keywords: cyanide, smoke inhalation, enclosed-space fire, carbon monoxide (PubMed Search)
Posted: 9/7/2012 by Bryan Hayes, PharmD
(Updated: 9/13/2012)
Click here to contact Bryan Hayes, PharmD
Carbon monoxide (CO) and hydrogen cyanide (HCN) are two of the main gases causing injury and death from smoke inhalation in fire victims. During the first phase of a fire, and prior to depletion of oxygen reserves and subsequent production of CO, formation of HCN from the thermal breakdown of nitrogen-containing materials may be the primary cause of lethal poisoning in an enclosed-space fire.
A recent, retrospective, observational study from Poland assessed the prevalence of toxic HCN exposure in victims of enclosed-space fires.
Important findings:
Conclusion: The high prevalence of coincident HCN concentrations and COHb levels in victims of enclosed-space fires emphasises the need to suspect HCN as a co-toxin in all persons rescued from fire who show signs and symptoms of respiratory distress.
Grabowska T, et al. Prevalence of hydrogen cyanide and carboxyhaemoglobin in victims of smoke inhalation during enclosed-space fires: a combined toxicological risk. Clin Toxicol 2012;50:759-63.
Follow me on Twitter (@PharmERToxGuy)
Category: Critical Care
Posted: 9/11/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
40 year-old male with severe uncontrolled hypertension presents with altered mental status (head CT below). The CXR is from the same patient. What's the connection?
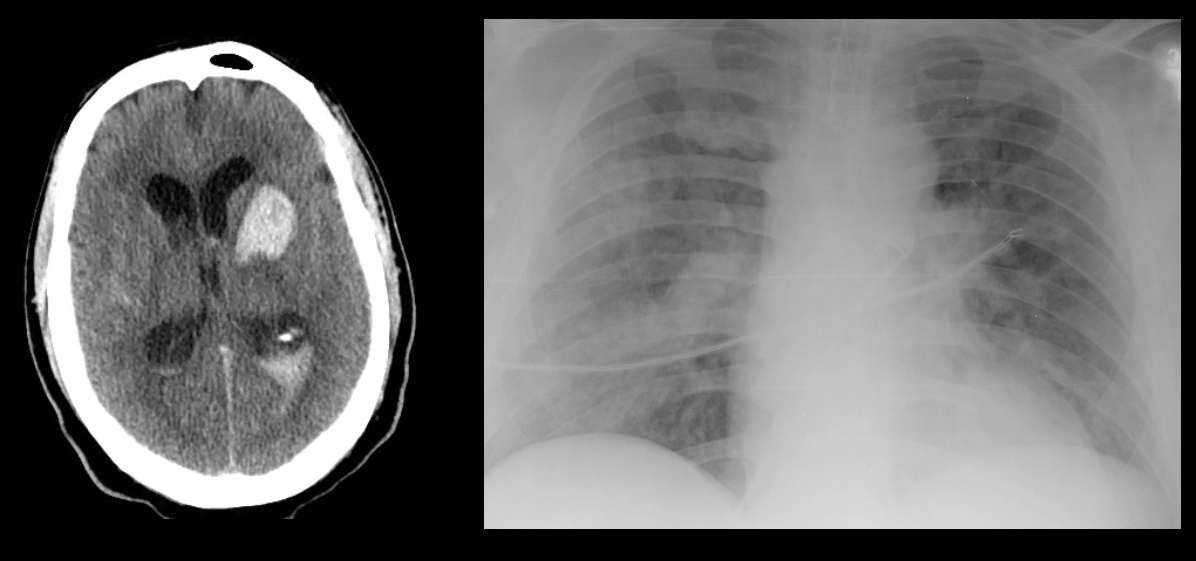
Answer: Neurogenic pulmonary edema (NPE)
NPE is defined as acute pulmonary edema following central nervous system (CNS) insult; NPE has been recognized for over 100 years, but its incidence is underreported due to a lack objective clinical criteria.
The pathophysiology of NPE is poorly understood but it is generally believed that both cardiogenic and non-cardiogenic pulmonary edema play a role. CXR (see above) demonstrates a pattern similar to acute respiratory distress syndrome (i.e., bilateral interstitial infiltrates).
CNS insults that are abrupt, rapidly progressive, and increase intracranial pressure (e.g., subarachnoid hemorrhage, intraparenchymal hemorrhage, traumatic brain injury, subdural, etc.) have the highest risk for NPE. Neural injury leads to sympathetic activation, the release of catecholamines, and one or all of the following:
Treatment of NPE includes:
Davidson, D. et al. Neurogenic pulmonary edema. Crit Care. 2012 Mar 20;16(2):212.
Follow me on Twitter (@criticalcarenow) and Google+ (+haneymallemat)
Category: Visual Diagnosis
Posted: 9/10/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
40 year-old male with severe uncontrolled hypertension presents with altered mental status. Head CT is shown here. Name three common anatomic locations generally seen for non-traumatic intracerebral hemorrhage.
Answer: The most common anatomic sites for intra-cerebral hemorrhage are:
...and, don't forget the most common causes of non-traumatic intra-cerebral hemorrhage:
Follow me on Twitter (@criticalcarenow) and Google+ (+haneymallemat)
Category: Cardiology
Keywords: mean arterial pressure, blood pressure (PubMed Search)
Posted: 9/9/2012 by Amal Mattu, MD
(Updated: 5/4/2026)
Click here to contact Amal Mattu, MD
Which patient has a better blood pressure, the patient with a blood pressure of 110/40 or the patient with a blood pressure of 90/60?
Mean arterial pressure (MAP) is generally considered to be the organ perfusion pressure in an individual. Because MAP requires an inconvenient calculation, we've all been taught...misled perhaps...into focusing on systolic blood pressure (SBP) as a marker of how well-perfused a patient is, and we tend to ignore the diastolic blood pressure (DBP).
It's important to remember, however, that we spend most of our lives in diastole, not systole. As a result, our organs spend more time being perfused during diastole than systole. The MAP takes this into account: MAP = (SBP + DBP + DBP)/3. DBP is more important than SBP!
So which patient is perfusing his vital organs better, the one with a BP of 110/40 or the one with a BP of 90/60? Do the MAP calculation...90/60 is better than 110/40!
Pay more attention to those diastolic BPs!
Category: Orthopedics
Keywords: Apprehension test, patellar dislocation, (PubMed Search)
Posted: 9/8/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Apprehension test for patellar dislocation
Test is used to access for the possibility of a patellar dislocation, prior to evaluation, now spontaneously reduced.
Similar to the shoulder apprehension test
Designed to place the patella in a position of imminent subluxation or dislocation
http://mulla.pri.ee/Kelley%27s%20Textbook%20of%20Rheumatology,%208th%20ed./HTML/f4-u1.0-B978-1-4160-3285-4..10042-7..gr16.jpg
http://www.youtube.com/watch?v=9AJxcbd9g8A
Place the knee in 20 - 30 degrees of flexion with the quadripces relaxed. Grasp the patella and attempt to place lateral directed stress.
If the patella is about to dislocate, the patient will experience apprehension due to the familiar pattern of dislocation, report the laxity and resist further motion by contracting the quadriceps
Category: Pediatrics
Keywords: cervical spine, trauma, pediatrics (PubMed Search)
Posted: 9/7/2012 by Lauren Rice, MD
Click here to contact Lauren Rice, MD
Ligamentous laxity is increased in children and ligamentous injury is more common than fractures.
If fractures occur, they are more likely to be in the upper cervical spine in infants and the lower cervical spine in older children.
Pseudosubluxation: physiologic subluxation between C2-3 and C3-4 may exist until age 16 years
Screening Assessment/Clearance for Verbal Children
-Midline C-spine tenderness?
-Pain with active motion?
-Altered level of alertness?
-Evidence of intoxication?
-Focal neurological deficit?
-Distracting painful injury?
-High impact injury?
Screening Assessment/Clearance for Pre-Verbal Children
-Neurological assessment of basic reflexes
-Response to painful stimuli
-Equal movements of all extremities
-Response to sound (eye tracking)
-Extremity strength and resistance
-Palpate posterior C-spine (observe for facial grimace)
-Feel for step-offs, deformities
-Verify full range of motion of neck (may need to be creative)
-Repeat neurological assessment
If concern arises on screening assessment, keep child in hard cervical collar and image (may start with x-ray and progress to CT if still concerned and x-rays negative).
If imaging negative, but persistent suspicion based on neurological deficits consider SCIWORA (Spinal Cord Injury WithOut Radiographic Abnormality) which exists in up to 50% of children with cervical cord injury, and may require MRI to further identify injury.
Category: Toxicology
Keywords: organophosphates, intermediate syndrome (PubMed Search)
Posted: 9/6/2012 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
Category: Critical Care
Posted: 9/4/2012 by Mike Winters, MBA, MD
(Updated: 5/4/2026)
Click here to contact Mike Winters, MBA, MD
Right Heart Failure in the Critically Ill
Greyson CR. Right heart failure in the intensive care unit. Curr Opin Crit Care 2012; 18:424-31.
Category: Visual Diagnosis
Posted: 9/3/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
32 year-old female presents with 5 days of fever, chills, and flank pain. She is hypotensive on presentation and urinalysis shows pyuria. Click here for the non-contrast CT scan. What's the diagnosis and what type of antibiotics should be started empirically?
Answer: Staghorn caliculi secondary to struvite stone. Broad-spectrum antibiotics to cover anaerobic bacteria should be initiated.
Follow me on Twitter (@criticalcarenow) and Google+ (+haneymallemat)
Category: Cardiology
Keywords: Lyme disease, Lyme carditis, AV block (PubMed Search)
Posted: 9/2/2012 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
Lyme disease is the most prevalent arthropod zoonosis in the Northern hemisphere
Rostoff P, Gajos G, Konduracka E, Gackowski A, Nessler J, Piwowarsk W. Lyme carditis: Epidemiology, pathophysiology, and clinical features in endemic areas. International Journal Cardiology
Category: Pharmacology & Therapeutics
Keywords: carbapenem, penicillin, allergy, skin test, cross-reactivity (PubMed Search)
Posted: 8/26/2012 by Bryan Hayes, PharmD
(Updated: 9/4/2013)
Click here to contact Bryan Hayes, PharmD
Carbapenems (meropenem, ertapenem, doripenem, imipenem/cilastatin) are broad-spectrum antibiotics that have good gram-negative and anaerobic coverage and are used to treat resistant bacterial infections.
Early retrospective studies showed ~10% cross-reactivity in penicillin-allergic patients.
More recent prospective studies verified penicillin allergy by the accepted standard (ie, skin test to the major and minor penicillin determinants) and tested for carbapenem allergy by administering a full therapeutic dose to carbapenem skin test-negative patients.
The cross-reactivity between skin tests appears to be around 1%, with all carbapenem skin test-negative patients tolerating the challenge.
Frumin J, Gallagher JC. Allergic cross-sensitivity between penicillin, carbapenem, and monobactam antibiotics: what are the chances? Ann Pharmacother 2009;43(2):304-15.
Herbert ME, Brewster GS, Lanctot-Herbert M. Medical myth: ten percent of patients who are allergic to penicillin will have serious reactions if exposed to cephalosporins. West J Med 2000;172:341.
Follow me on Twitter (@PharmERToxGuy)
Category: Pediatrics
Keywords: septic shock, fluid resuscitation, PALS (PubMed Search)
Posted: 8/31/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Toxicology
Keywords: LSD, hashish, marijuana, jobs (PubMed Search)
Posted: 8/30/2012 by Fermin Barrueto
(Updated: 5/4/2026)
Click here to contact Fermin Barrueto
I was reading the biography of Steve Jobs looking for incredible insights into leadership and innovation. I have realized that you basically have to be a genuis and it doesn't matter what you do. His favorite drug was LSD which he believed was necessary to improve creativity and innovation. His description of the hallucinations confirm that he was taking this drug.
We describe LSD hallucinations as a crossing of the senses or "synesthesias" - you hear the color blue, you see the smell of roses.
Steve Jobs describes a moment in a wheat field while on LSD and (paraphrasing from the biography) ..." the wheat was playing Bach beautifully"
If you have a patient describing this type of hallucination you can almost be guaranteed that they have taken LSD or some other tryptamine.
