Category: Pediatrics
Keywords: Influenza (PubMed Search)
Posted: 3/2/2011 by Mimi Lu, MD
(Updated: 3/5/2011)
Click here to contact Mimi Lu, MD
Now that influenza season is in full swing, remember that early antiviral treatment can reduce the risk of complications in high-risk individuals. One of those high-risk groups is children <2 years, with the highest hospitalizations and mortality in infants <6 months.
According to the CDC website:
Recommended antiviral medications (neuraminidase inhibitors) are not FDA-approved for treatment of children aged <1 year (oseltamivir) or those aged <7 years (zanamivir). Oseltamivir was used for treatment of 2009 pandemic influenza A (H1N1) virus infection in children aged <1 year under an Emergency Use Authorization, which expired on June 23, 2010. Nevertheless,
Current CDC guidance on treatment of influenza should be consulted; updated recommendations from CDC are available at http://www.cdc.gov/flu
.
Category: Toxicology
Keywords: Brown Recluse,envenomation,spider,loxoscelism (PubMed Search)
Posted: 3/3/2011 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
Recently a case report was published in which a child was incorrectly diagnosed with MRSA. He actually had systemic loxoscelism from a Brown Recluse spider bite.
A patient who has been bitten by brown recluse spider bite may present with pruritis, pain and swelling. The classic lesion has a bluish-purple central region, surrounded by concentric rings of pale ischemia and erythema. (“red, white and blue”) Bites may progress over days to a bleb with necrosis and eschar formation, followed by ulceration.
Systemic loxoscelism presents with a scarlatiniform rash that spreads dependently. It may have the classic purple lesion surrounded by concentric rings of pale ischemia and erythema. The patient may be uncomfortable but is usually stable. Treatment is supportive care.
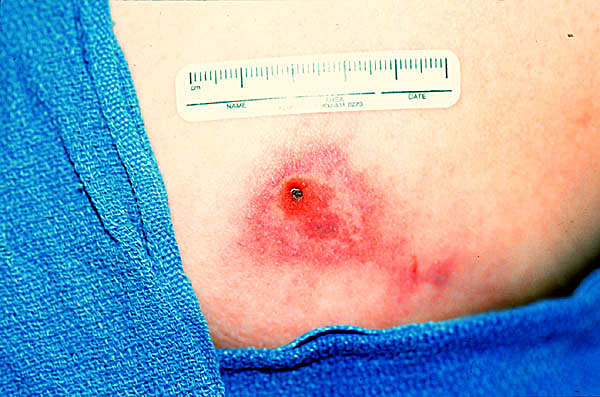
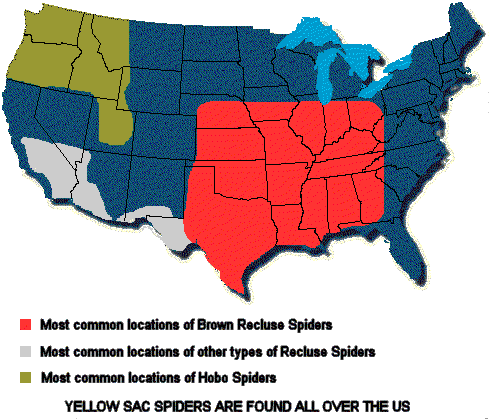
Rogers, KM, Klotz CR, Jack M, Seger D. Systemic Loxoscelism in the Age of Community-Acquired Methicillin-Resistant Staphylococcus aureus. Ann of EM Feb 2011 57(2); 138-40.
Category: Neurology
Keywords: phenytoin, dilantin, seizure, dilantin level, phenytoin level (PubMed Search)
Posted: 3/2/2011 by Aisha Liferidge, MD
(Updated: 5/5/2026)
Click here to contact Aisha Liferidge, MD
Category: Visual Diagnosis
Keywords: ultrasound, ectopic, free fluid, hypotension, pregnancy (PubMed Search)
Posted: 2/27/2011 by Haney Mallemat, MD
(Updated: 8/28/2014)
Click here to contact Haney Mallemat, MD
24 yo woman presents with syncope, abdominal pain, and normal menses 4 days prior. Urine HCG(+) and quantitative beta-HCG is 1300 with the transvaginal ultrasound seen below. Diagnosis?
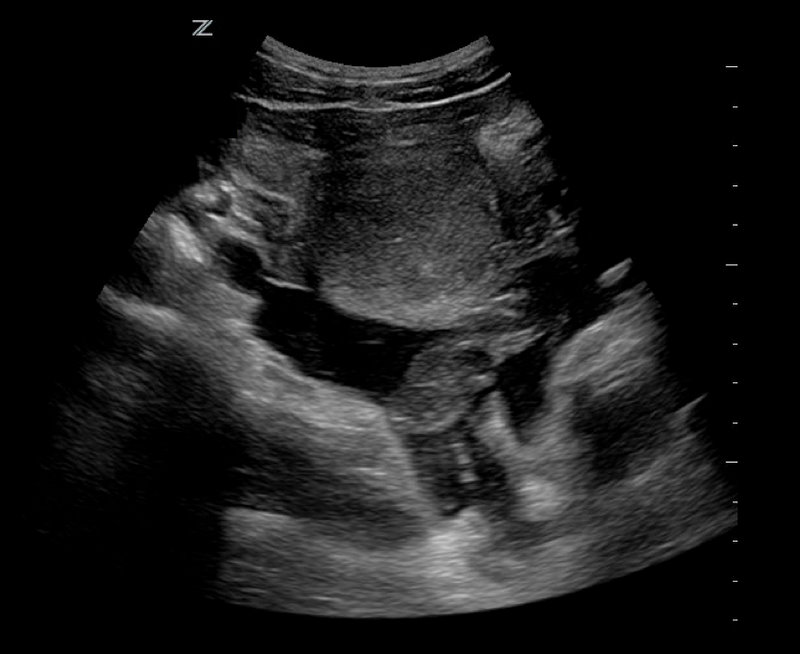
Ectopic Pregnancy Pearls
Tintinalli, Judith, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7th Edition. 2011, McGraw-Hill Companies, Inc, China
Category: Cardiology
Keywords: short QT, QT, QT interval, QTc (PubMed Search)
Posted: 2/27/2011 by Amal Mattu, MD
(Updated: 5/5/2026)
Click here to contact Amal Mattu, MD
The long QT syndrome and causes of acquired long QT interval are well-known to most emergency physicians, but a short QT can be problematic as well. Short QT-syndrome is an inherited ion-channel disease that predisposes to ventricular dysrhythmias and sudden death. The QTc in these patients is generally < 340 msec. This condition is more common in children, and it should be considered in the differential diagnosis and evaluated on ECG in children presenting with syncope.
Category: Orthopedics
Keywords: apophysitis, overuse injuries, heel pain, achilles (PubMed Search)
Posted: 2/26/2011 by Brian Corwell, MD
(Updated: 5/5/2026)
Click here to contact Brian Corwell, MD
Sever's disease ,aka calcaneal apophysitis, is a common overuse injury in the pediatric and adolescent population.
Occurs secondary to traction of the calcaneus that most often occurs in young athletes (8-12 yo)
-Avg. age of presentation is 11 years 10 months in boys & 8 years 8 months in girls
-Repetitive traction to the weaker apophysis, induced by the pull of the Achilles on its insertion
Hx: Heel pain that increases with activity (running, jumping).
-May involve one (40%) or both (60%) feet
PE: Tenderness of the posterior heel at the Achilles tendon insertion and ankle dorsiflexor weakness
Imaging: Radiography is often normal. When positive, show fragmentation and sclerosis of the calcaneal apophsis. NOTE: These findings are nonspecific and also are observed in asymptomatic feet.
http://t0.gstatic.com/images?q=tbn:ANd9GcQ9R-fx1iyhbhNJpNL2W72bWdK72_mRBLNX5DUDtcMfnDli-x7Ong
DDx: Includes osteomyelitis and tarsal coalition.
Tx: Rest from aggravating activities, NSAIDs, ice (both pre and post sport). When pain free a program of stretching (gastrocnemius-soleus), strengthening (dorsiflexors) and shoe inserts (heel cups, lifts, pads, or orthotics) can provide significant pain relief.
Category: Pediatrics
Posted: 2/25/2011 by Rose Chasm, MD
(Updated: 5/5/2026)
Click here to contact Rose Chasm, MD
Pediatrics Board Review Core Curriculum
MedStudy 1st edition, Book 3
Category: Toxicology
Keywords: mephedrone, bath salts (PubMed Search)
Posted: 2/24/2011 by Fermin Barrueto
(Updated: 5/5/2026)
Click here to contact Fermin Barrueto
Continuing with the synthetic/designer drug theme. Last time we were discussing synthetic marijuana. Another old drug making a resurgence under the designer drug category is mephedrone.This amphetamine-like drug has been purportedly the active substance in "bath salts". It has also been sold as "plant food" - still trying to figure that one out.
Sold in head shops under the name Bliss or Cloud 9 - they have been reported to be available in Baltimore, MD recently. They can also be bought over the internet. Crushed, snorted or ingested, the effect is similiar to cocaine with a largely sympathomimetic toxidrome. Mephedrone has been labeled an entactogen with users behaving similiar to an MDMA ingestion. A Baltimore news station incorrectly called it "synthetic cocaine" - though the effect may be similiar, completely different molecular structure.
Treatment is cooling, check lytes (especially sodium), check for rhabdomyolysis and sedation with benzodiazepines. Below is one link from a Denver News Station. Attached is a picture of a bath salt product.
The latest and greatest on the street - synthetic marijuana and bath salts!
http://www.thedenverchannel.com/news/26567376/detail.html
Category: Neurology
Keywords: lumbar puncture, seizure, febrile seizure (PubMed Search)
Posted: 2/23/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
-- 6 to 12 months > "strongly consider" LP
-- 12 to 18 months > "consider" LP
-- 18 months and up > LP not routinely necessary; may consider after clinical assessment
-- Any infant/child with recent antibiotic treatment plus SFS > "strongly consider" LP
Category: Critical Care
Posted: 2/22/2011 by Mike Winters, MBA, MD
(Updated: 5/5/2026)
Click here to contact Mike Winters, MBA, MD
Hemodynamic Monitoring in the Ventilated Patient
Magder S. Hemodynamic monitoring in the mechanically ventilated patient. Curr Opin Crit Care 2011;17:36-42.
Category: Visual Diagnosis
Posted: 2/21/2011 by Rob Rogers, MD
Click here to contact Rob Rogers, MD
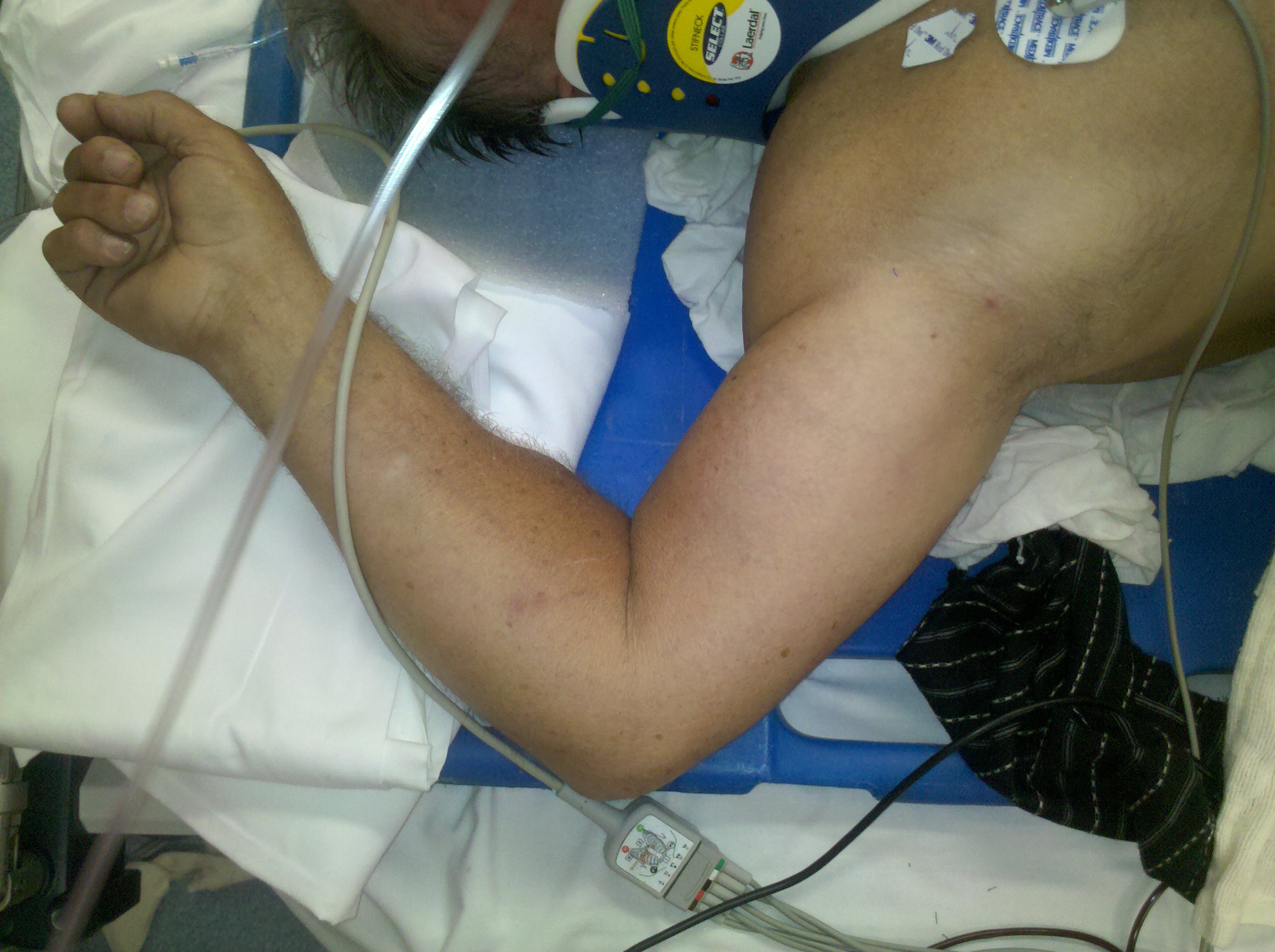
Luxatio Erecta-inferior glenohumeral dislocation
A rare shoulder dislocation caused by a hyperabduction injury to the arm.
Category: Cardiology
Keywords: bradycardia, bradydysrhythmia, digoxin, hyperkalemia (PubMed Search)
Posted: 2/20/2011 by Amal Mattu, MD
(Updated: 5/5/2026)
Click here to contact Amal Mattu, MD
[Here's a nice simple pearl from Jeff Tabas, MD (Prof of EM at UCSF).]
3 causes of bradycardia to consider when the rhythm is not clearly sinus bradycardia:
1. Junctional bradycardia
2. Hyperkalemia
3. Digoxin toxicity
Category: Orthopedics
Keywords: radius, fracture, treatment (PubMed Search)
Posted: 2/19/2011 by Michael Bond, MD
Click here to contact Michael Bond, MD
Distal Radius Fractures
Typically distal radius fractures are treated with closed reduction and splinting in the ED, followed by operative repair. This is done because it is felt that patients will have the best functional outcomes if the bones are restored to their normal anatomic alignment. However, two studies published in 2010 suggest differently.
The study by Neidenbach showed that after one year there was no difference in functional outcomes between patients that were just splinted in the ED in the position the fracture was found versus those that had closed reduction with splinting.
The second study by Ego showed that there was no difference in outcomes between those that underwent conservative treatment with closed reduction and splinting versus those that underwent operative repair.
The take home point from these studies for the EM physician is that most distal radius fractures can be splinted in the position found with them following up with an orthopaedist. There is probably little advantage to performing a closed reduction in the ED knowing that this procedure can use a lot of valuable time and resources.
Neidenbach P, Audige L, Wilhelmi-Mock M, Hanson B, De Boer P. The efficacy of closed reduction in displaced distal radius fractures. Injury. 2010;41(6):592-598.
Egol KA, Walsh M, Romo-Cardoso S, Dorsky S, Paksima N. Distal radial fractures in the elderly: operative compared with nonoperative treatment. J Bone Joint Surg Am. 2010;92(9):1851-1857.
Category: Toxicology
Keywords: THC, marijuana (PubMed Search)
Posted: 2/18/2011 by Fermin Barrueto
(Updated: 5/5/2026)
Click here to contact Fermin Barrueto
Sold under the name of K2, Spice. Patients exposed to this will present with dry mouth, paranoia, tachycardia, hallucinations but will resolved rather quickly over several hours. Observation in the ED and supportive care is usually all that is needed. A little history about synthetic marijuana:
Category: Neurology
Keywords: ketamine, conscious sedation, procedural sedation (PubMed Search)
Posted: 2/16/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Keywords: Pulmonary embolism, PE, echocardiography, ultrasound, hemodynamics, McConnell sign, right ventricle (PubMed Search)
Posted: 2/15/2011 by Haney Mallemat, MD
(Updated: 5/5/2026)
Click here to contact Haney Mallemat, MD
Casazza F., et al. Regional right ventricular dysfunction in acute pulmonary embolism and right ventricular infarction.Eur J Echocardiography 2005 Jan; 6(1): 11-4.
Category: Trauma
Keywords: blunt trauma, pneumothorax, CXR supine, ultrasound, seashore, stratasphere (PubMed Search)
Posted: 2/14/2011 by Haney Mallemat, MD
(Updated: 8/28/2014)
Click here to contact Haney Mallemat, MD
(Please note the prior version of this pearl was incorrect with respect to the images referenced. This version is corrected.)
Patient s/p blunt chest trauma. CXR (image 1) vs. lung ultrasound (image 2), do you see any inconsistencies?
Lung ultrasound in traumatic pneumothorax: The "Stratosphere Sign"
Written by Dr. Michael Allison.
For advanced sonographers:
1. Blaivas, M. et al. A prospective comparison of supine chest radiography and bedside ultrasound for the diagnosis of traumatic pneumothorax. Academic Emergency Med. 2005 Sep;12(9):844-9.
2. Lichtenstein D et al. Ultrasound diagnosis of occult pneumothorax. Crit Care Med. 2005 June;33(6): 1231-8.
Category: Cardiology
Keywords: syncope, near-syncope, pre-syncope (PubMed Search)
Posted: 2/13/2011 by Amal Mattu, MD
(Updated: 5/5/2026)
Click here to contact Amal Mattu, MD
Is there a difference in the workup, etiologies, or prognosis between patients with syncope vs. near-syncope? Traditional teaching indicates that there is no difference, but that doesn't necessarily reflect common practice. Physicians sometimes are a bit less concerned about patients with near-syncope vs. patients with true, full-blown syncope; and many syncope studies exclude patients with near-syncope.
Grossman and colleagues recently published a useful reminder that patients with syncope and near-syncope have a similar 30-day rate of adverse outcome. However, they have a lower admission rate, reflecting the lower level of concern physicians have in their evaluation. Be wary of those patients with near-syncope. Don't be reassured just because they didn't hit the floor...yet!
Grossman SA, Babineau M, Burke L, et al. Do outcomes of near syncope parallel syncope? Amer J Emerg Med 2010 (article currently in press)
Category: Pediatrics
Keywords: head CT, trauma, pediatrics, head injury (PubMed Search)
Posted: 2/11/2011 by Adam Friedlander, MD
(Updated: 5/5/2026)
Click here to contact Adam Friedlander, MD
Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study.Lancet2009;374:1160-
Category: Toxicology
Keywords: dose-response, paracelsus (PubMed Search)
Posted: 1/26/2011 by Bryan Hayes, PharmD
(Updated: 2/10/2011)
Click here to contact Bryan Hayes, PharmD
Many consider Paracelsus (1493–1541) as the father of modern toxicology.
The introduction of the dose–response concept might have been his most important contribution to toxicology, meaning that everything is toxic at the right dose (even oxygen and water).
