Category: Pharmacology & Therapeutics
Keywords: sepsis, antibiotics, vasopressors, shock (PubMed Search)
Posted: 2/4/2017 by Michelle Hines, PharmD
(Updated: 5/4/2026)
Click here to contact Michelle Hines, PharmD
Below is a list of pharmacy-related pearls from the 2016 Surviving Sepsis Guidelines:
Rhodes A, Evans LE, Alhazzani W, et al. Surviving sepsis campaign: International guidelines for management of sepsis and septic shock: 2016. Crit Care Med 2017; 3. [PMID 28098591]
Follow me on Twitter @mEDPharmD
Category: Critical Care
Keywords: Sepsis, Septic Shock, Fluid resuscitation (PubMed Search)
Posted: 1/31/2017 by Daniel Haase, MD
(Updated: 2/18/2017)
Click here to contact Daniel Haase, MD
At the Society of Critical Care Meeting (SCCM) this month, updates to the Surviving Sepsis Guidelines were released. Recommendations include:
--Initial 30mL/kg crystalloid resuscitation with frequent reassessment of fluid responsiveness using dynamic (not static) measures [goodbye CVP/ScvO2!]
--Initiation of broad-spectrum antibiotics within ONE hour of sepsis recognition [two agents from different classes]
--Further hemodynamic assessement (e.g. echo for cardiac function) if clinical assessment does not reveal the type of shock [get out the ultrasound!]
Rhodes A, Evans LE, et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Crit Care Med. 2017 Jan 18.
Category: Visual Diagnosis
Posted: 1/30/2017 by Tu Carol Nguyen, DO
Click here to contact Tu Carol Nguyen, DO
25 year-old female with hx of cerebral palsy with significant developmental delay, s/p G-tube who presented with acute hypoxic respiratory failure, hypotension and a distended, tense abdomen. A CT was done with the scout film below. What's the diagnosis?
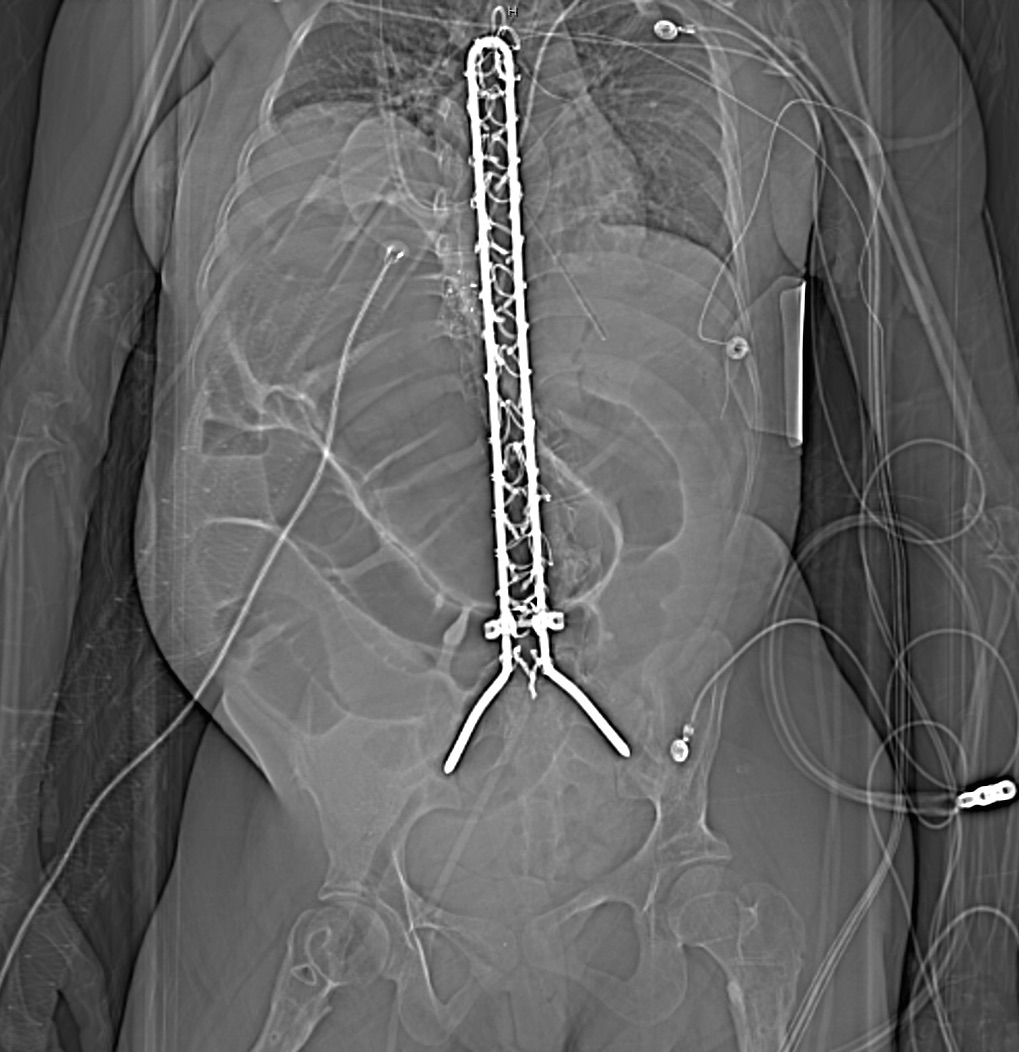
Answer: Cecal Volvulus
Patient was subsequently intubated, had an NG tube placed with over 500cc of fluid returned. Patient had multiorgan failure and received fluids, antibiotics, pressors, blood products and went to the OR, and had a partial bowel resection.
One way to differentiate cecal volvulus from sigmoid volvulus is that sigmoid volvulus generally do not have haustra.
Tonerini M, Pancrazi F, Lorenzi S, Pacciardi F, Ruschi F, et al. (2015) Cecal volvulus: what the radiologist needs to know. Glob Surg, 1: DOI: 10.15761/GOS.1000106.
Category: Orthopedics
Keywords: nerve, entrapment (PubMed Search)
Posted: 1/28/2017 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
During a busy ED shift, your 40yo charge nurse asked you to look at his hand. He is known avid mountain biker. He has pain in his right 4th and 5th digits. . He feels a lack of coordination and a feeling of “clumsiness” of the hand. Where is his possible nerve compression and what do you expect to find on exam?
Ulnar nerve entrapment is sometimes called “handlebar palsy.”
Compression location is Guyon’s canal.
The ulnar nerve supplies the intrinsic muscles of the hand AND the extrinsic muscles for flexion of the 4th and 5th digits. This is what aids in a “power grip” and why he may have diminished grip strength on exam.
Also innervates the ADDuctor pollicis and 1st dorsal interosseous muscles (pinch)
Note the ulnar nerve also passes through the radial tunnel at the elbow. Entrapment here is called Radial tunnel syndrome or Cubital tunnel syndrome and causes forearm pain and paresthesias in the 4th and 5th digits with grossly normal motor and sensory function.
Category: Pediatrics
Keywords: epinephrine, auto-injector (PubMed Search)
Posted: 1/27/2017 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
As a follow up to Dr. Winter’s Pearl on Anaphylaxis on 1/24/2017, here’s a handy pearl for pediatric anaphylaxis (part 1).
Anaphylaxis: rapid and potentially life-threatening involvement of at least 2 systems following exposure to an antigen.
Medications (max: adult doses)
Get it?!?! Easy right? Instead of fumbling through an app or reference card during your next case of pediatric anaphylaxis, be a rock star "EM DR" by remembering the “Rule of 2’s”.
(Can't help it...ya'll know I love my mnemonics!!)
Category: Toxicology
Keywords: methadone overdose, hypoglycemia (PubMed Search)
Posted: 1/26/2017 by Hong Kim, MD
Click here to contact Hong Kim, MD
Methadone overdose produces classic signs and symptoms of opioid intoxication - CNS and respiratory depression with pinpoint pupils. However, methadone overdose has also been associated with hypoglycemia – a relatively uncommon adverse effect.
Bottom line:
Several case reports have been published over the past years. Recently, a case of refractory hypoglycemia was reported in a woman, without a history of diabetes, after ingesting 250 mL of methadone (18.2 mg/kg).
She required, in additional to naloxone infusion for respiratory depression, dextrose infusion (initially D10 then D20) for 54 hours.
Incidence of hypoglycemia has also been observed in patient with rapid methadone dose escalation as well as in cancer patient who were started on methadone for pain control with dose-depedent association.
In a mice study, methadone induced a dose dependent hypoglycemia - 20 mg/kg methadone resulted in decrease in average glucose level of 172 +/- 7 mg/dL to 55 +/- 6 mg/dL. This effect was reversed by naloxone administration. morphine, fentanyl, oxycodone and levorphanol did not produce hypoglycemia.
However, in the case report published in Clinical Toxicology Nov 2016, naloxone infusion did not effect the hypoglycemia.
Category: Neurology
Keywords: weakness, ptosis (PubMed Search)
Posted: 1/25/2017 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
Patients may present to the ED with new onset weakness due to myasthenia gravis (MG). A group that is frequently missed is late-onset MG, which occurs after the age of 50. It is frequently misdiagnosed as a stroke or transient ischemic attach (TIA).
Two cardinal features:
Bonus pearl: Ocular symptoms are present in up to 85% of patients with MG, with unilateral ptosis or asymmetric bilateral ptosis being the most common presentations.
Nicolle MW. Myasthenia Gravis and Lambert-Eaton Myasthenic Syndrome. Continuum. 2016;22(6):1978–2005
Category: Critical Care
Posted: 1/24/2017 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Epinephrine in Anaphylaxis
Kawano T, et al. Epinephrine use in older patients with anaphylaxis: Clinical outcomes and cardiovascular complications. Resuscitation 2017; 112:53-58.
Category: Pediatrics
Keywords: Nail bed injuries, wound closure (PubMed Search)
Posted: 1/20/2017 by Jenny Guyther, MD
(Updated: 5/4/2026)
Click here to contact Jenny Guyther, MD
More studies are needed, but the existing data shows that medical adhesives may be quicker without impacting cosmetic and functional outcome.
Nail bed injuries occur in 15-24% of children with fingertip injuries.
In 1997, medical adhesive was first used to secure the avulsed nail plate back to the nail bed instead of suturing back into place. By 2008, there were small studies looking at the utility of using medical adhesive to close the laceration of the nail bed. The studies were small, but there was a tendency towards shorter repair times and no difference between pain, cosmetic outcome or function.
A total of 6 articles were included in this review – 2 using histoacryl and 4 using demabond.
Edwards, S, Parkinson L. Is Fixing Pediatric Nail Bed Injuries with Medical Adhesives as Effective as Suturing? A Review of the Literature. Pediatric Emergency Care. 2016.
Category: Toxicology
Keywords: Urine Drug Sreen (PubMed Search)
Posted: 1/19/2017 by Kathy Prybys, MD
(Updated: 1/20/2017)
Click here to contact Kathy Prybys, MD
Urine drug screens are most commonly performed by immunoassay technology utilizing monoclonal antibodies that recognizes a structural feature of a drug or its metabolites. They are simple to perform. provide rapid screening, and qualitative results on up to 10 distinct drug classes with good sensitivity but imperfect specificity. This can lead to false positive results and the need for confirmatory testing. UDS does not detect synthetic opiates or cannabinoids, bath salts (synthetic cathinones), and gamma-hydroybutyrate. Most common drug classes detected are the following:
Category: International EM
Keywords: Opioids, overdose, injury, death (PubMed Search)
Posted: 1/18/2017 by Jon Mark Hirshon, MPH, MD, PhD
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
· Opioid deaths, such as from heroin and prescription opioids, are a major problem globally
· In the U.S., since 1999 overdose deaths from prescription opioids have quadrupled.
o Almost half of opioid deaths involve a prescription opioid
· The most common drugs related to prescription opioid deaths are:
o Methadone
o Oxycodone
o Hydrocodone
https://www.cdc.gov/drugoverdose/data/overdose.html
Category: Critical Care
Keywords: Arterial Line, Ultrasound (PubMed Search)
Posted: 1/17/2017 by Rory Spiegel, MD
(Updated: 5/4/2026)
Click here to contact Rory Spiegel, MD
It is not uncommon for critically ill patients to require invasive monitoring of their blood pressure. In these patients, radial arterial lines are often inserted. Traditionally these lines are placed using palpation of the radial pulse. This technique can lead to unacceptably high failure rate in the hypotensive patient commonly encountered in the Emergency Department.
A recent meta-analysis by Gu et al demonstrated the use of dynamic US to assist in the placement of radial arterial lines decreased the rate of first attempt failure, time to line insertion and the number of adverse events associated with insertion.
Gu WJ, Wu XD, Wang F, Ma ZL, Gu XP. Ultrasound Guidance Facilitates Radial Artery Catheterization: A Meta-analysis with Trial Sequential Analysis of Randomized Controlled Trials. Chest. 2016;149(1):166-79.
Category: Orthopedics
Keywords: Airway, wheezing, exercise (PubMed Search)
Posted: 1/14/2017 by Brian Corwell, MD
(Updated: 6/26/2021)
Click here to contact Brian Corwell, MD
You are covering a sporting event or working an ED shift when a young adolescent athlete without significant PMH presents with SOB and wheezing associated with exercise.
You immediately think exercise-induced asthma, prescribe a short-acting bronchodilator and pat yourself on the back.
While you may be right, there is increasing recognition of an alternative diagnosis
Exercise-induced laryngeal obstruction (EILO)
During high intensity exercise, the larynx can partially close, thereby causing a reduction in normal airflow. This results in the reported symptoms of SOB and wheezing.
This diagnosis has previously been called exercise induced vocal cord dysfunction. As the narrowing most frequently occurs ABOVE the level of the vocal cord, EILO is a more correct term.
While exercise induced bronchoconstriction has a prevalence of 5-20%, EILO is less common with a prevalence of 5-6%.
Patients are typically adolescents, with exercise associated wheezing and SOB, frequently during competitive or very strenuous events. Wheezing is inspiratory and high-pitched. Symptoms are unlikely to be present at time of medical contact unless you are at the event as resolution occurs within 5 minutes though associated cough or throat discomfort can persist after exercise cessation. EIB symptoms typically last up to 30 minutes following exercise.
Inhaler therapy is unlikely to help though some athletes report subjective partial relief. This may be explained as approximately 10% of individuals have both EIB and EILO.
In athletes with respiratory symptoms referred to asthma clinic, EILO was found in 35%.
Consider EILO in athletes with unexplained respiratory symptoms especially in those with ongoing symptoms despite appropriate therapy for EIB.
Category: Toxicology
Keywords: salicylate poisoning (PubMed Search)
Posted: 1/13/2017 by Hong Kim, MD
(Updated: 5/4/2026)
Click here to contact Hong Kim, MD
A small retrospective study of an acute poisoning cohort attempted to identify risk factors for severe outcome in salicylate poisoning.
Severe outcomes were defined as
A multivariate analysis of 48 patients showed that older age and increased respiratory rate were independent predictors of severe outcomes when adjusted for salicylate level.
Initial salicylate acid level was not predictive of severe outcome.
Elevated lactic acid level was also a good predictor of severe outcome in univariate analysis but not in multivariate analysis.
Limitations
Bottom line
Shively RM et al. Acute salicylate poisoning: risk factors for sever outcome. Clin Toxicol 2017 Jan 9:1-6. doi: 10.1080/15563650.2016.1271127. [Epub ahead of print]
Category: Neurology
Keywords: concussion, driving performance, cognitive impairment (PubMed Search)
Posted: 1/11/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Schmidt JD, Hoffman NL, Ranchet M, et al. Driving after concussion: Is it safe to drive after symptoms resolve? J Neurotrauma. 2016 Dec 13. [Epub ahead of print]
Follow me on Twitter @EM_NCC
Category: Critical Care
Keywords: Sepsis, Antibiotics, Septic Shock (PubMed Search)
Posted: 1/10/2017 by Daniel Haase, MD
(Updated: 2/18/2017)
Click here to contact Daniel Haase, MD
--Recent meta-analysis comparing continuous infusion versus intermittent bolus dosing of beta-lactam antibiotics demonstrates mortality benefit (NNT = 15) in patients with severe sepsis or septic shock. (1)
--Consider beta-lactam continuous infusion on your septic patients if your hospital pharmacy allows
[Thanks to Anne Weichold, CRNP for providing the article for this pearl!]
--Beta-Lactams are time-dependent antibiotics (i.e. longer time above MIC = more time killing) annd continuous infusions should have concentrations consistently above MIC.
--Previous studies not powered to demonstrate mortality benefit, but showed pharmocokinetic improvement and higher rates of clinical cure (2)
Pratical aspects
This means the patient will require an additional IV most of the time
Most hospitals do not have a pharmacy protocol for infusion of most extended-spectrum B-lactams
1. Roberts JA, Abdul-Aziz MH, Davis JS, et al. Continuous versus Intermittent B-Lactam Infusion in Severe Sepsis. Am J Resp Crit Care Med. 2016; 194 (6): 681-91.
2. Abdul-Aziz MH, Sulaiman H, Mat-Nor MB, et al. Beta-Lactam Infusion in Severe Sepsis (BLISS): a prospective, two-centre, open-labelled randomised controlled trial of continuous versus intermittent beta-lactam infusion in critically ill patients with severe sepsis. Intensive Care Med. 2016; 42 (10) 1535-45.
Category: Visual Diagnosis
Posted: 1/9/2017 by Tu Carol Nguyen, DO
Click here to contact Tu Carol Nguyen, DO
A 60 year-old man with history of atrial fibrillation, CAD presents with left lower leg/foot pain for a few days. His foot is seen below. What's the diagnosis?
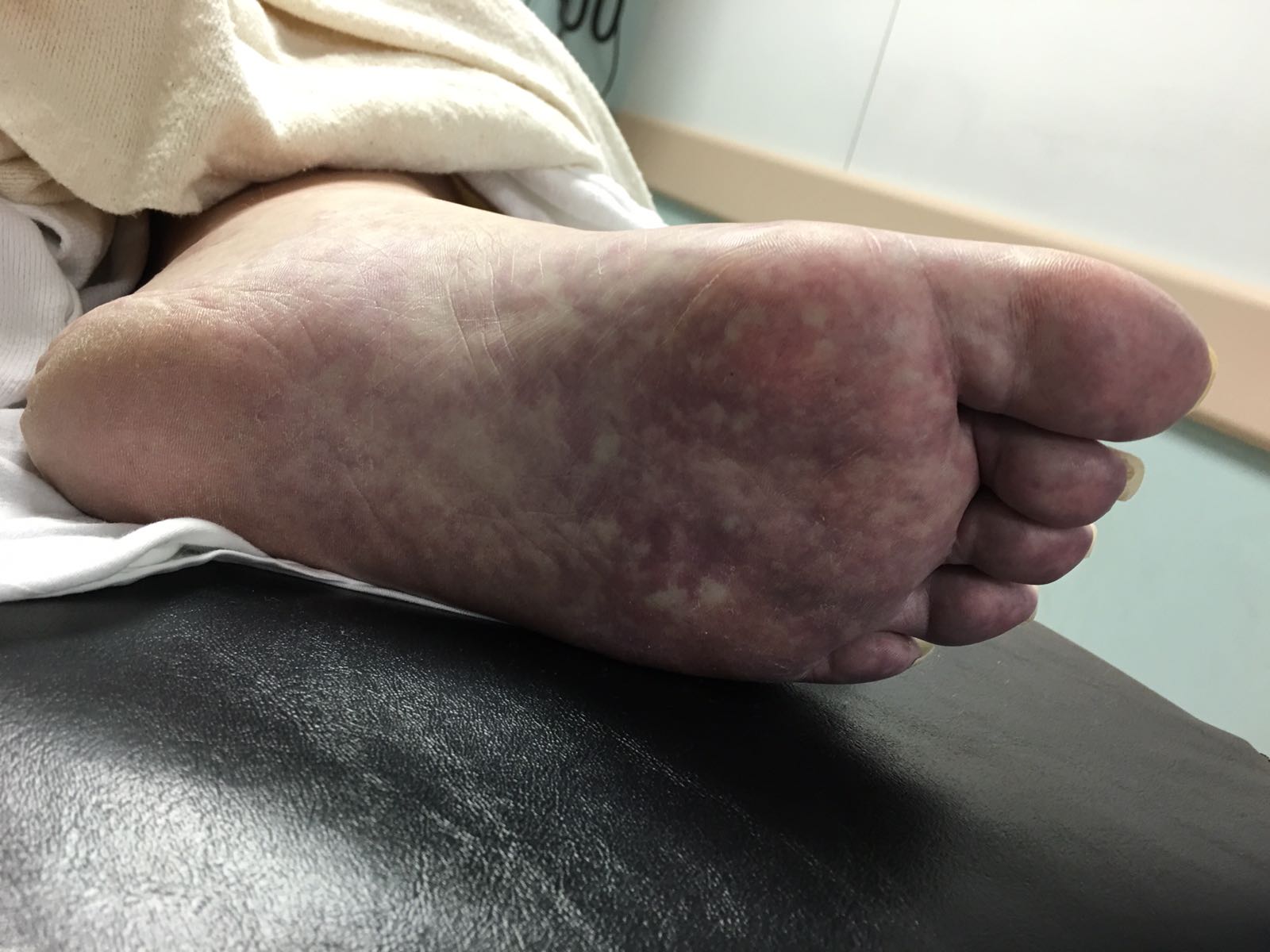
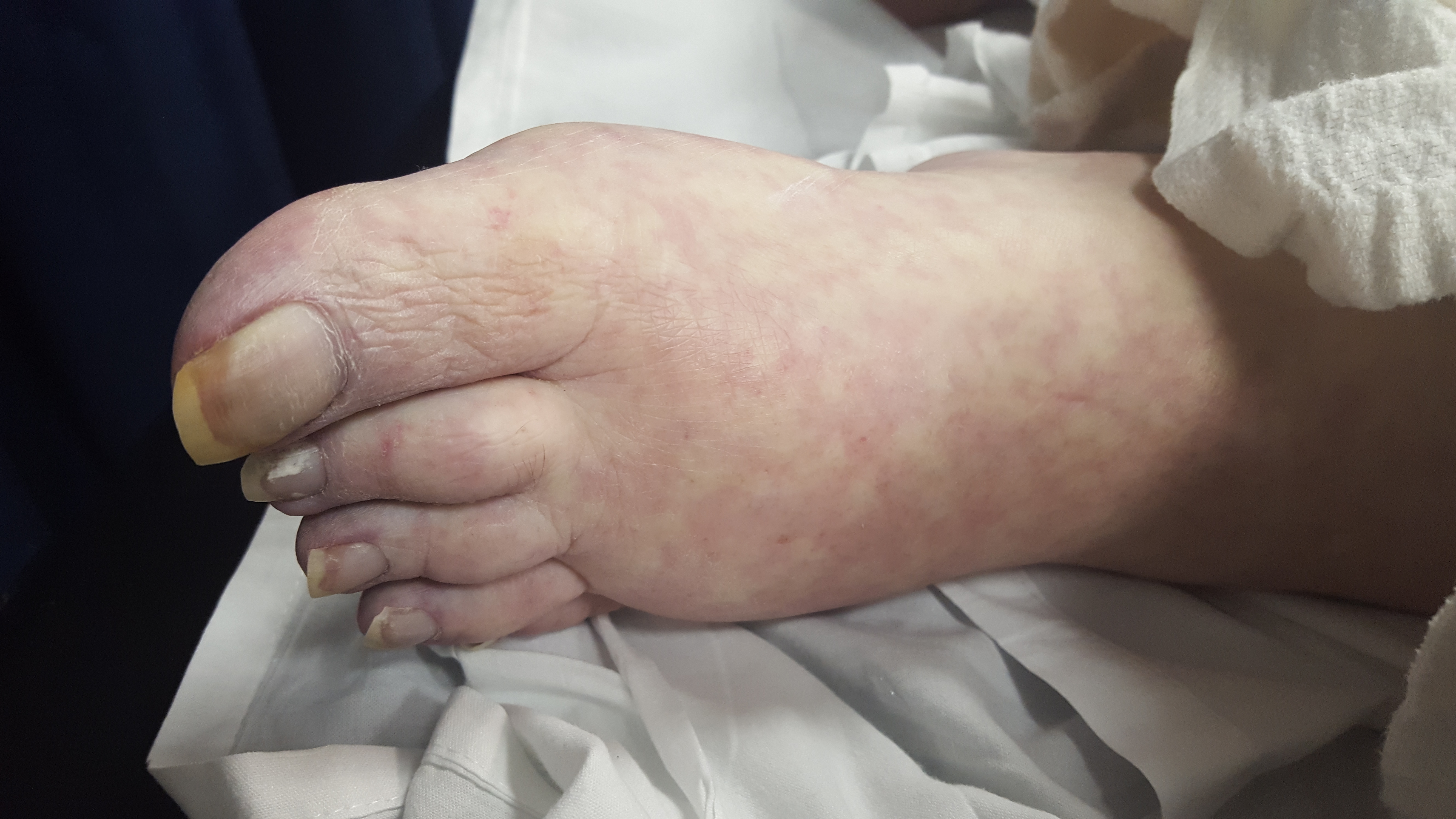
Mottling with concerns for Acute Limb Ischemia
Key Points:
Creager MA, Kaufman JA, Conte MS. Clinical practice. Acute limb ischemia. N Engl J Med. 2012;366(23):2198-206.
http://www.emdocs.net/acute-limb-ischemia-pearls-pitfalls/
Category: Pharmacology & Therapeutics
Keywords: ketorolac, NSAID, analgesia (PubMed Search)
Posted: 1/7/2017 by Michelle Hines, PharmD
(Updated: 5/4/2026)
Click here to contact Michelle Hines, PharmD
In a study comparing ketorolac IV doses of 10 mg, 15 mg, and 30 mg, no difference in pain score reduction or need for rescue analgesia was observed.
Based upon this study, lower ketorolac doses of 10 mg or 15 mg are equal in analgesic efficacy to a higher dose of 30 mg. A lower dose of 10 mg or 15 mg should be used to avoid adverse effects.
Motov S, Yasavolian M, Likourezos A, et al. Comparison of intravenous ketorolac at three single-dose regimens for treating acute pain in the emergency department: a randomized controlled trial. Ann Emerg Med 2016. PMID 27993418
Follow me on Twitter @mEDPharmD
Category: Toxicology
Keywords: Lactic acidosis (PubMed Search)
Posted: 1/5/2017 by Kathy Prybys, MD
(Updated: 1/6/2017)
Click here to contact Kathy Prybys, MD
Lactic acidosis is the most common cause of anion gap metabolic acidosis in all hospitalized patients. An elevated lactate level is an important marker of inadequate tissue perfusion causing subsequent shift to anaerobic metabolism and occuring in a variety of disease states such as sepsis. In patients with unexplained lactic acidosis without systemic hyoperfusion or seizure suspect the following toxins:
Understanding lactic acidosis in paracetamol (acetaminophen) poisoning. Shah, AD, Wood DM, et al. British Journal of Clinical Pharmacology 2011.71: 20–28.
Value of lactic acidosis in the assessment of the severity of acute cyanide poisoning. Baud FJ, et al. Crit Care Med. 2002;30(9):2044-50.
The Importance of the osmolality gap in ethylene glycol intoxication. Oostvogels R, et al. BMJ 2013 Dec 7;347:31-33.
Can Acute overdose metformin lead to lactic acidosis? Wilis BK, et al. Amer J Emerg Med. 2010;28:857.
Bench to bedside review: Severe lactic acidosis in HIV patients treated with nucleoside analogue reverse transcriptase inhibitors. Classens Y-E, et al. Critical Care. 2003;7(3):226-232.
A case of Kombucha Teas Toxicity. Kole A SH, Jones HD, et al. J Intensive care Med.2009:24(3) 205-7.
Category: International EM
Keywords: B12 deficiency, ataxia, dementia, pernicious anemia (PubMed Search)
Posted: 1/4/2017 by Jon Mark Hirshon, MPH, MD, PhD
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
Vitamin B12 deficiency can cause significant disease, including severe neurologic problems. However, patient presentations can vary greatly.
Signs and symptoms can include:
Prolonged B12 deficiency can lead to significant neurologic complications, frequently related to the spinal cord, and can include:
