Category: Critical Care
Posted: 1/3/2017 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
PaCO2 and the Post-Arrest Patient
McKenzie N, et al. A systematic review and meta-analysis of the association between arterial carbon dioxide tension and outcomes after cardiac arrest. Resuscitation 2017; 111:116-126.
Category: Visual Diagnosis
Posted: 1/2/2017 by Hussain Alhashem, MBBS
Click here to contact Hussain Alhashem, MBBS
A 36-year-old male, who recently immigrated from Africa, presented to the ED with fever, rash, cough and shortness of breath. He was noted to be febrile to 39.0 C. The rash is disseminated but present mainly in his trunk as shown in the picture.
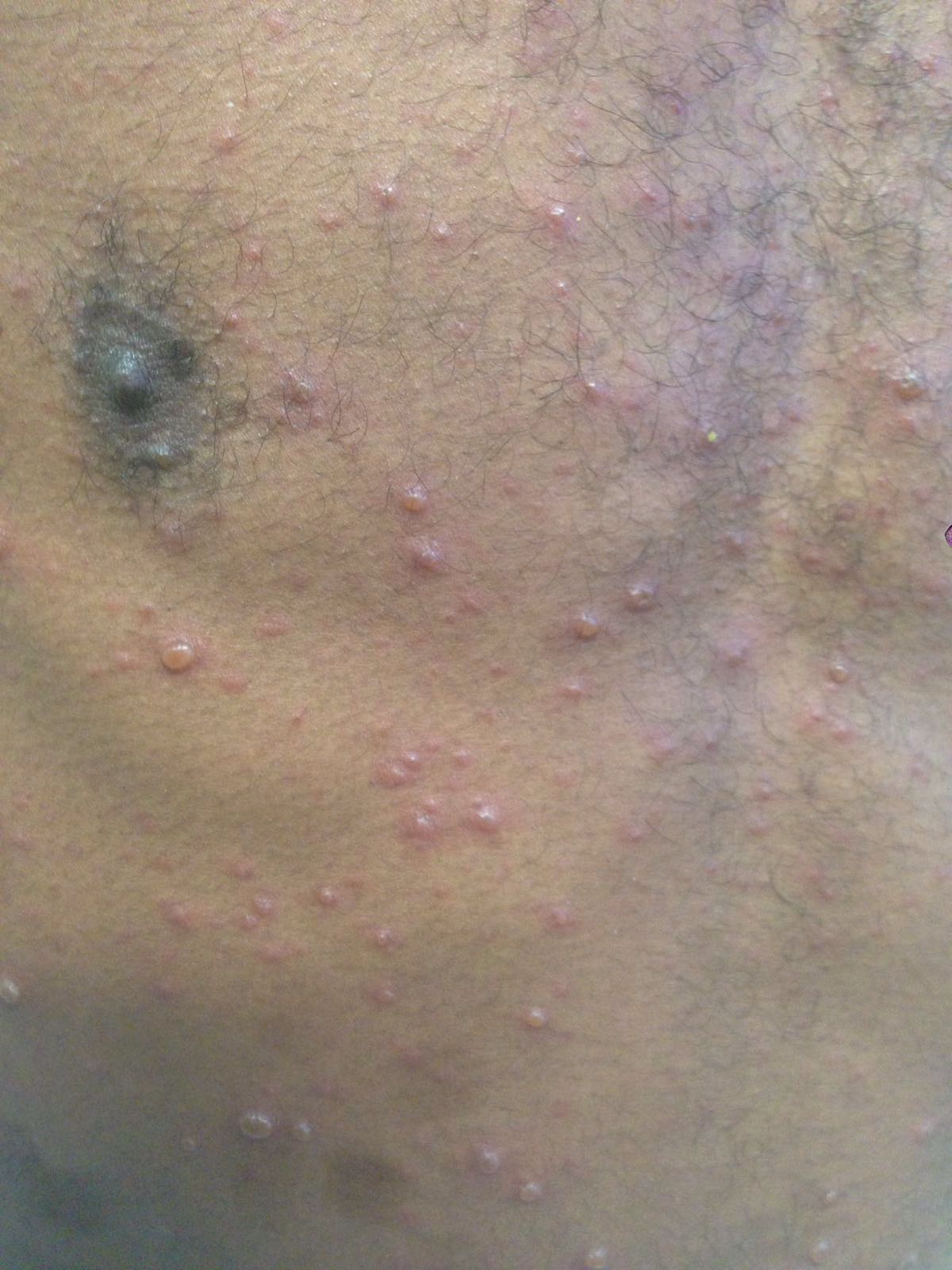
Disseminated Varicella Zoster Virus (VZV) Infection
- The patient is presenting with a rash in different stages, associated with fever and signs of systematic involvement, indicating a disseminated varicella infection.
- Definitive diagnosis of disseminated VZV infection is made by detecting its DNA in multiple anatomic sites.
- The most common complication of VZV infection in immunocompetent adults is VZV pneumonia. Early detection of VZV pneumonia can be done with bronchoalveolar lavage and PCR testing.
- Treatment is with IV acyclovir and is more effective if started within 24 hours of the beginning of symptoms. In cases that require prolonged treatment, gene sequencing should be done to detect resistant strains.
Beby?Defaux, Agnès, et al. "Disseminated varicella with multiorgan failure in an immunocompetent adult." Journal of medical virology 81.4 (2009): 747-749.
Category: Orthopedics
Keywords: DVT, Leg, Cast (PubMed Search)
Posted: 12/31/2016 by Michael Bond, MD
Click here to contact Michael Bond, MD
Take Home Point:
Low-molecular-weight heparin doesn't seem to prevent symptomatic venous thromboembolism (VTE) in patients undergoing knee arthroscopy or lower leg casting, suggest two trials in the New England Journal of Medicine.
The study was conducted by Dutch researcheers and randomized 1500 patients who underwent lower leg casting or knee arthoscopy to receive no anticoagulation or low molecular weight heparin. Patients were either treated for the entire duration of immobilzation or 8 days after their surgery (arthroscopy patients)
The rates of VTE in patients at 3 months of follow up where arthroscopy: 0.7% vs. 0.4%; casting: 1.4% vs. 1.8%. So overall very low rates of VTE, and no real difference between the groups.
A large cohort might have shown some benefit, but since the incidence is so low there is probably no reason to prophlactically treat these patients and increase their risk of major bleeding events, which was also low in the study.
The article can be found at http://www.nejm.org/doi/full/10.1056/NEJMoa1613303?query=pfw&jwd=000100949960&jspc=EM
van Adrichem RA, Nemeth B, Algra A, le Cessie S, Rosendaal FR, Schipper IB, et al. Thromboprophylaxis after Knee Arthroscopy and Lower-Leg Casting. N Engl J Med 2016.
Category: Pediatrics
Posted: 12/31/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
In pediatrics, providers typically prescribe 10 mg/kg (max 500 mg) and 5 mg/kg daily x 4 (max 250 mg) for treatment of pneumonia, but this dosing regimen is NOT recommended for all azithromycin usage. There are other dosing regimens that are important to keep in mind during the respiratory season:
1) Pharyngitis/ tonsillitis (ages 2-15 yr): 12 mg/kg daily x 5 days (max 500 mg/ 24 hr)
2) Pertussis
3) Acute sinusitis >/= 6 months: 10 mg/kg daily x 3 days
Tschudy MM, Arcara KM. The Harriet Lane Handbook 19th edition. Elsevier Mosby; 2012
Category: Toxicology
Keywords: cyanide toxicity, lactic acid (PubMed Search)
Posted: 12/29/2016 by Hong Kim, MD
(Updated: 12/30/2016)
Click here to contact Hong Kim, MD
Smoke inhalation victims (house fires) are at risk of carbon monoxide (CO) and cyanide poisoning (CN). CO exposure/poisoning can be readily evaluated by CO - Oximetry but CN level can be obtained in majority of the hospital.
Lactic acid level is often sent to evaluate for CN poisoning.
Bottom line:
In a manuscript published in 1991, N Engl J Med by Dr. FJ Baud is the source of this data.
CN blood levels were measured in 109 residetial fire victims in France prior to any treatment was initiated.
Baud FJ et al. Elevated blood cyanide concentrations in victims of smoke inhalation. N Engl J Med 1991;325:1761-6.
Category: Critical Care
Keywords: Acute pulmonary edema, Bolus nitrates (PubMed Search)
Posted: 12/27/2016 by Rory Spiegel, MD
(Updated: 5/4/2026)
Click here to contact Rory Spiegel, MD
It is well known that the early aggressive utilization of IV nitrates and non-invasive positive pressure ventilation (NIV) in patients presenting with acute pulmonary edema will decrease the number of patients requiring endotracheal intubation and mechanical ventilation.
Often our tepid dosing of nitroglycerine is to blame for treatment failure. Multiple studies have demonstrated the advantages of bolus dose nitroglycerine in the early management of patients with acute pulmonary edema. In these cohorts, patients bolused with impressively high doses of IV nitrates every 5 minutes, are intuabted less frequently than patients who received a standard infusion (1,2). No concerning drops in blood pressure in the patients who received bolus doses of nitrates were observed. Using the standard 200 micrograms/ml nitroglycerine concentration, blood pressure can be rapidly titrated to effect.
1. Cotter G, Metzkor E, Kaluski E, et al. Randomised trial of high-dose isosorbide dinitrate plus low-dose furosemide versus high-dose furosemide plus low-dose isosorbide dinitrate in severe pulmonary oedema. Lancet. 1998;351(9100):389-93.
2. Levy P, Compton S, Welch R, et al. Treatment of severe decompensated heart failure with high-dose intravenous nitroglycerin: a feasibility and outcome analysis. Ann Emerg Med. 2007;50(2):144-52
Category: Visual Diagnosis
Posted: 12/27/2016 by Tu Carol Nguyen, DO
Click here to contact Tu Carol Nguyen, DO
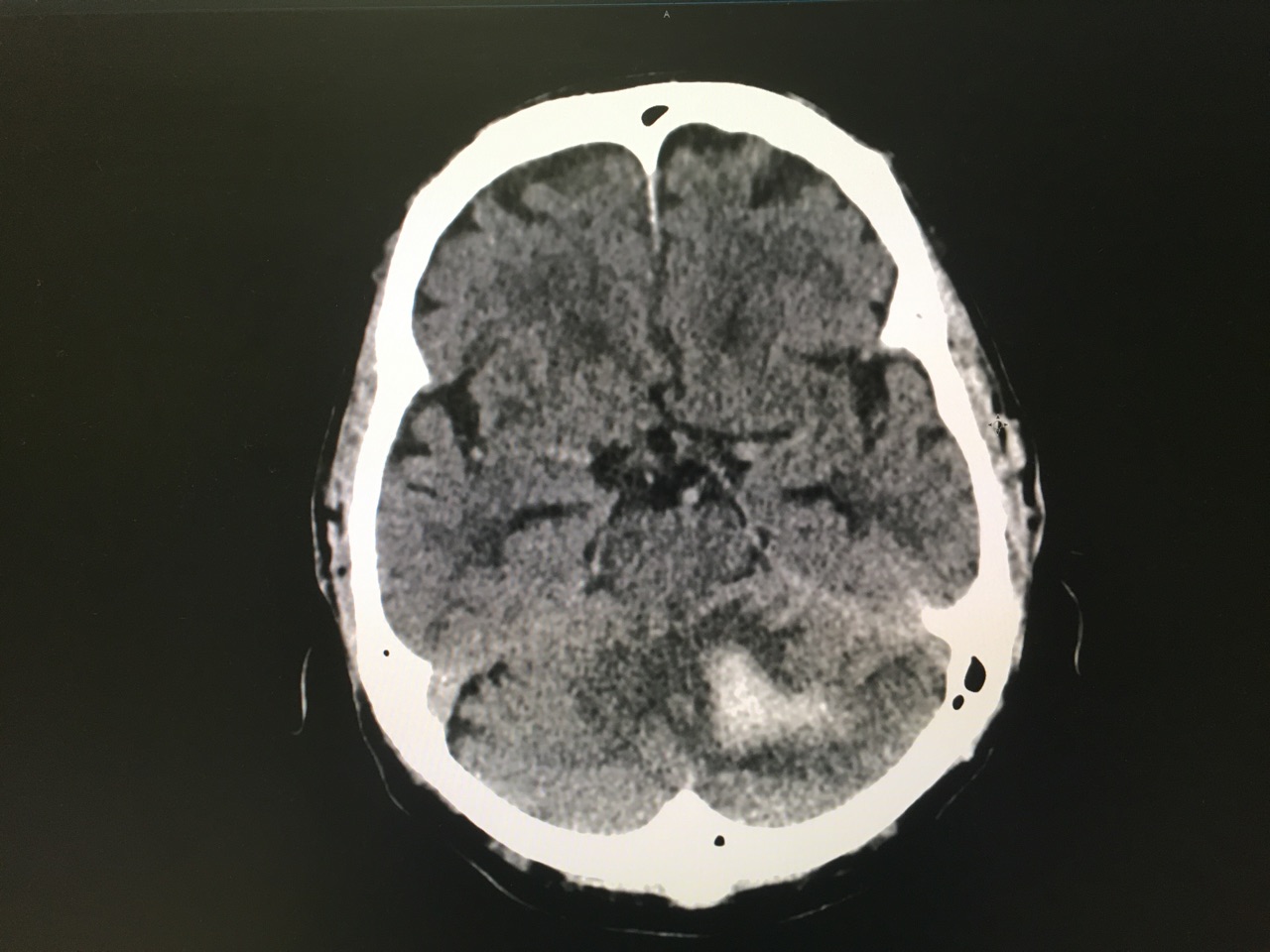
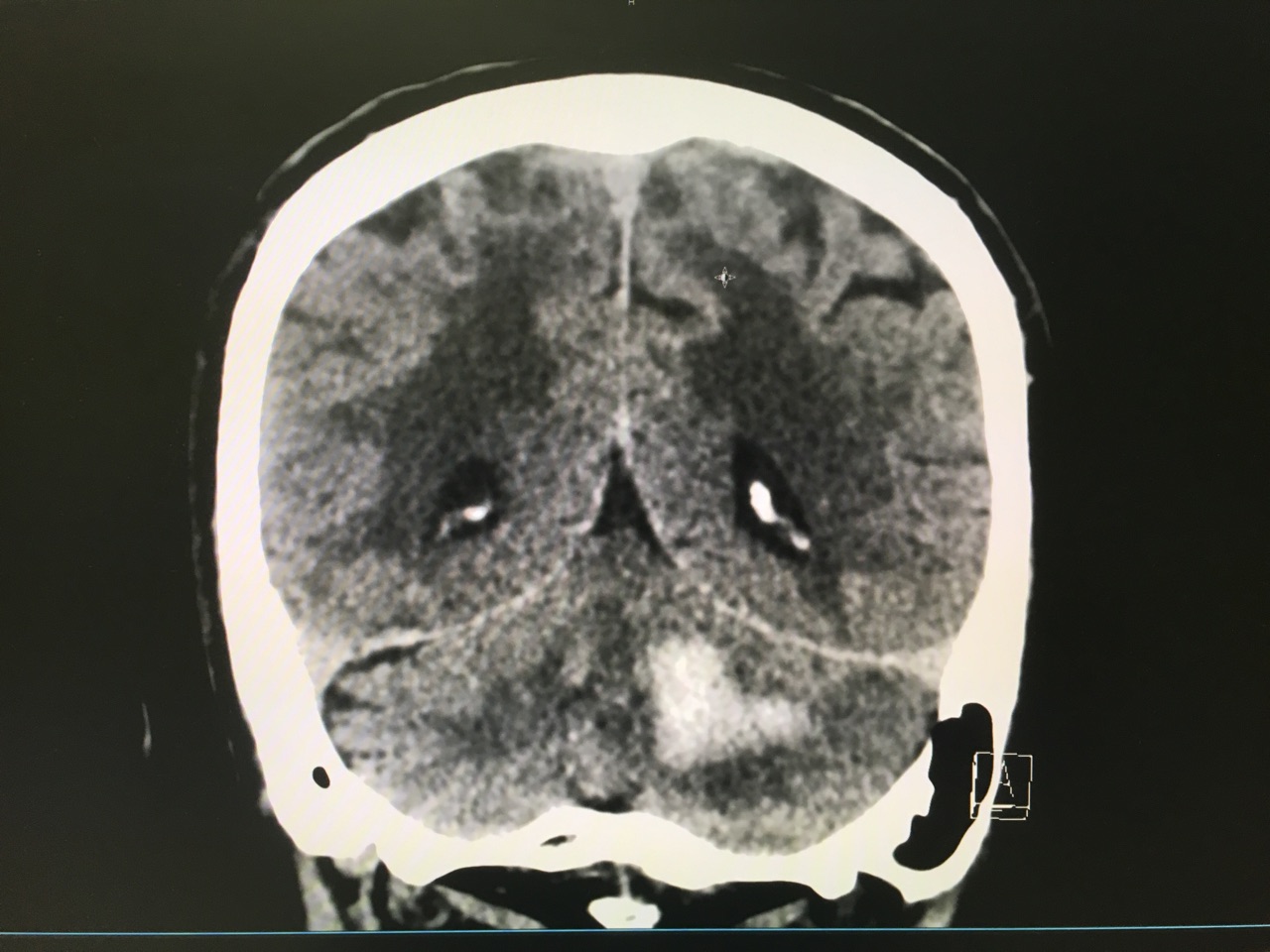
Answer: Large left cerebellar intraparenchymal hemorrhage with surrounding vasogenic edema with mild infratentorial midline shift of ~4mm
Take Home Points:
Hemphill JC, Greenberg SM, Anderson CS, et al. Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. 2015;46(7):2032-60.
Category: Orthopedics
Keywords: Concussions, musculoskeletal injury (PubMed Search)
Posted: 12/24/2016 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Significant associations were found between concussion and
Lateral ankle sprain (P = 0.012)
Knee injury (P = 0.002)
Lower extremity muscle injury (P = 0.031)
Keep in mind that 50 – 80% of concussions may go undiagnosed or unreported.
A discussion about risks of early return after concussion should include mention of risks beyond repeat head injury/2nd impact syndrome
Study limits: Retrospective design limits ability to establish causation/reporting bias
Gilbert, Burdette, et al., 2016 Association between concussion and lower extremity injuries in collegiate athletes. Sports Health 8 (6), 561-567.
Category: International EM
Keywords: Vitamin B12, pernicious anemia (PubMed Search)
Posted: 12/21/2016 by Jon Mark Hirshon, MPH, MD, PhD
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
Vitamin B12 deficiency, including pernicious anemia, is typically seen in malnourished individuals. Globally, it is widespread in those who live in poverty.
In the U.S., we often consider it in individuals who are chronic alcoholics. However, it can be seen in others, including:
Category: Critical Care
Keywords: Intracranial hemorrhage, ICH, PCC, FFP, vitamin K antagonist, VKA, coumadin, warfarin (PubMed Search)
Posted: 12/20/2016 by Daniel Haase, MD
(Updated: 2/18/2017)
Click here to contact Daniel Haase, MD
The Neurocritical Care Society and Society of Critical Care Medicine just came out with new Guidelines for Reversal of Antithrombotics in Intracranial Hemorrhage (ICH) [1]
--PCC is now recommended over FFP in reversal of vitamin K antagonists (VKA) with elevated INR. Either should be co-administered with 10mg IV vitamin K. (Strong recommendation, moderate quality evidence)
TAKE AWAY: PCC should be probably be given over FFP in VKA-ICH when available
--Seems to be primarily based on a recent Lancet trial, which was stopped early due to safety concerns [2], but demonstrated more rapid reversal of INR and less hematoma expansion.
--In that study, all hematoma expansion related deaths occurred in the FFP group.
--Study was not designed to look at 90 day outcome, but trended towards improved survival.
1. Guideline for Reversal of Antithrombotics in Intracranial Hemorrhage: Executive Summary. A Statement for Healthcare Professionals From the Neurocritical Care Society and the Society of Critical Care Medicine. Frontera JA, Lewin JJ 3rd, et al. Crit Care Med. 2016 Dec;44(12):2251-2257.
2. Fresh frozen plasma versus prothrombin complex concentrate in patients with intracranial haemorrhage related to vitamin K antagonists (INCH): a randomised trial. Steiner T, Poli S, et al. Lancet Neurol. 2016 May;15(6):566-73.
Category: Infectious Disease
Keywords: cellulitis (PubMed Search)
Posted: 12/15/2016 by Michael Bond, MD
(Updated: 12/17/2016)
Click here to contact Michael Bond, MD
Take home points:
Category: Pediatrics
Keywords: fever, diarrhea, urinary tract infection (PubMed Search)
Posted: 12/16/2016 by Jenny Guyther, MD
(Updated: 5/4/2026)
Click here to contact Jenny Guyther, MD
After 4 months old, the answer MAY be no.
80 children between 4 months and 6 years of age with fever > 101 degress F and watery stools (> 3 episodes) were evaluated for hydration status using urine samples. The urine was collected either by catheterization or clean catch, depending on age. All urine cultures were negative.
Nibhanipudi KV. A Study to determine the Incidence of Urinary Tract Infections in Infants and Children Ages 4 months to 6 Years with Febrile Diarrhea. Glob Pediatr Health. 2016. Published online Sept 12, 2016.
Category: Toxicology
Keywords: Acetaminophen, Liver Failure (PubMed Search)
Posted: 12/16/2016 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
Acetaminophen is one of the most common pharmaceutical ingestions in overdose and a leading cause of acute of liver failure in the U.S. Early recognition and treatment is critical for prevention of morbidity.
Category: Neurology
Keywords: pharmacist, thrombolysis, door-to-needle time, acute ischemic stroke (PubMed Search)
Posted: 12/14/2016 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Impact of an ED pharmacist on time to thrombolysis in acute ischemic stroke
Montgomery K, Hall AB, Keriazes G. Impact of an emergency medicine pharmacist on time to thrombolysis in acute ischemic stroke. Am J Emerg Med 2016;34:1997-9.
Follow me on Twitter @EM_NCC
Category: Critical Care
Posted: 12/13/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Mechanical Ventilation in the Obese Patient
Goyal M, et al. Body mass index is associated with inappropriate tidal volumes in adults intubated in the ED. Am J Emerg Med 2016; 34:1682-3.
Category: Visual Diagnosis
Posted: 12/12/2016 by Hussain Alhashem, MBBS
Click here to contact Hussain Alhashem, MBBS
30 Year-old female presents to the ED for a rash. The rash started suddenly, mainly in her extremities and it is painful. The patient denied having fever or chills. Her past medical history is unremarkable. She admits to using cocaine frequently. The rash is shown in the picture.
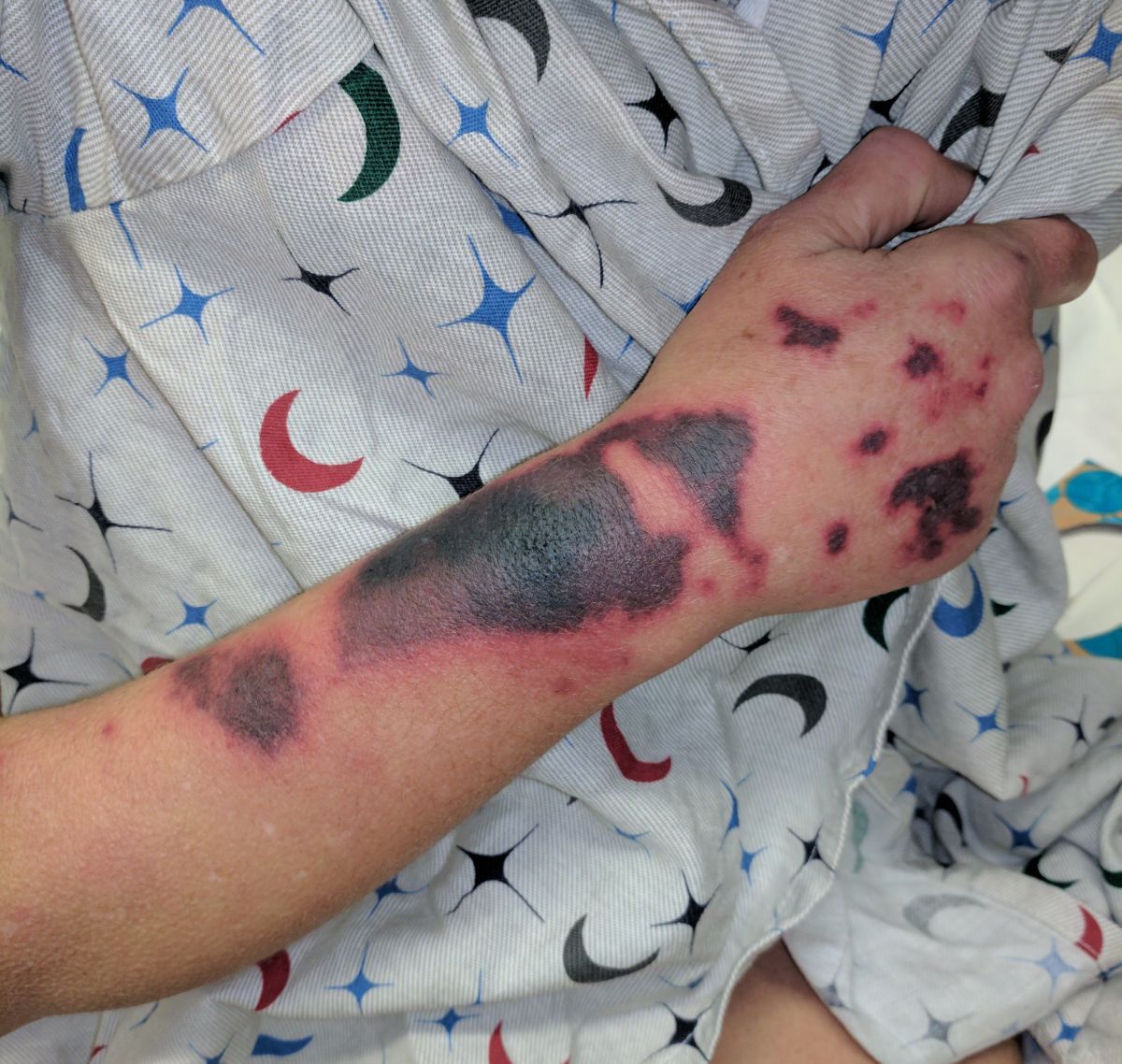
Levamisole-Induced Vasculitis
- Levamisole is an antihelmintic drug that was banned by the US Food and Drug Administration in 2000 because of its adverse effects.
- It is added to cocaine to increase its weight and potentiate its effect.
- Patients usually present with painful purpuric rash without central necrosis.
- Laboratory values might include agranulocytosis and elevated ESR.
- Treatment is by cessation of cocaine use.
- Because Levamisole is strongly associated with agranulocytosis, corticosteroids should be avoided to prevent immunosuppression.
Roberts, Jordan A., and Patricia Chévez-Barrios. "Levamisole-induced vasculitis: a characteristic cutaneous vasculitis associated with levamisole-adulterated cocaine." Archives of pathology & laboratory medicine 139.8 (2015): 1058-1061.
Category: Toxicology
Keywords: acetaminophen overdose, APAP levels (PubMed Search)
Posted: 12/8/2016 by Hong Kim, MD
(Updated: 12/9/2016)
Click here to contact Hong Kim, MD
Recent study evaluated whether an acetaminophen (APAP) level obtained less than 4-hour post acute ingestion can predict which patient would not require n-acetylcysteine (NAC). APAP cutoff level of 100 ug/mL was used for analysis. This was a secondary analysis of the Canadian Acetaminophen Overdose Study database (retrospective study).
Bottom line:
Table 2. Diagnostic accuracy of acetaminophen concentration obtained 2 to 4 hours post-ingestion to identify subsequent potentially toxic concentration measured 4 to 20 hours pos-ingestion.
|
| Subsequent 4-hour equivalent [APAP] | |
| [APAP] obtained 2 to 4 hours post-ingestion | >150 ug/mL | < 150 ug/mL |
| <10 | 0 | 89 |
| 10-20 | 2 | 79 |
| 20-50 | 6 | 209 |
| 50-100 | 19 | 249 |
| 100-150 | 46 | 253 |
| 150-200 | 161 | 195 |
| 200-300 | 276 | 46 |
| 300-450 | 148 | 5 |
| >450 | 38 | 0 |
Yarema MC, et al. Can a serum acetaminophen concentration obtained less than 4 hours post-ingestion determine which patients do not rquire treatment with acetylcysteine? Clin Toxicol 2016; online early: doi: 10.1080/15563650.2016.1247959
Category: Critical Care
Keywords: OHCA, ROSC (PubMed Search)
Posted: 12/6/2016 by Rory Spiegel, MD
(Updated: 5/4/2026)
Click here to contact Rory Spiegel, MD
The prognosis of patients who experienced OHCA, who have not achieved ROSC by the time they present to the Emergency Department, is dismal. As such, it behooves us as Emergency Physicians to identify the few patients with a potentially survivable event. Drennan et al examined the ROC data base and identified the cohort of patients who had not achieved ROSC and were transported to the hospital. The overall survival in this cohort was 2.0%. Factors that predicted survival were initial shockable rhythm and arrest witnessed by the EMS providers. Patients arriving to the ED without ROSC, that had neither of those prognostic factors had a survival rate of 0.7%.
Drennan IR, et al. A comparison of the universal TOR Guideline to the absence of prehospital ROSC and duration of resuscitation in predicting futility from out-of-hospital cardiac arrest. Resuscitation (2016)
Category: Visual Diagnosis
Posted: 12/5/2016 by Tu Carol Nguyen, DO
Click here to contact Tu Carol Nguyen, DO
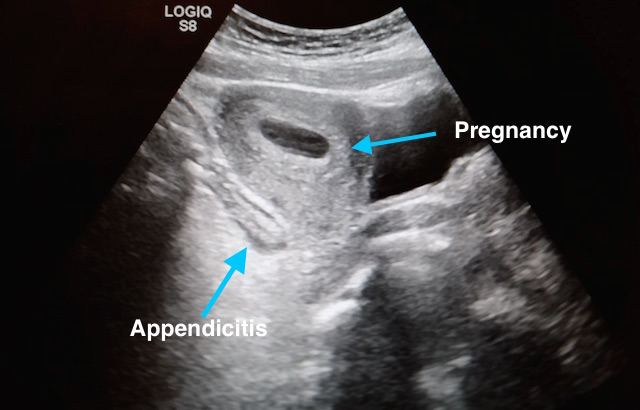
27 year-old G2P1 presents with 3 days of abdominal pain that is mostly suprapubic. Denies any urinary symptoms and vaginal bleeding. Physical examination reveals slight rebound in the right lower quadrant.
An ultrasound revealed the following. What's the diagnosis?
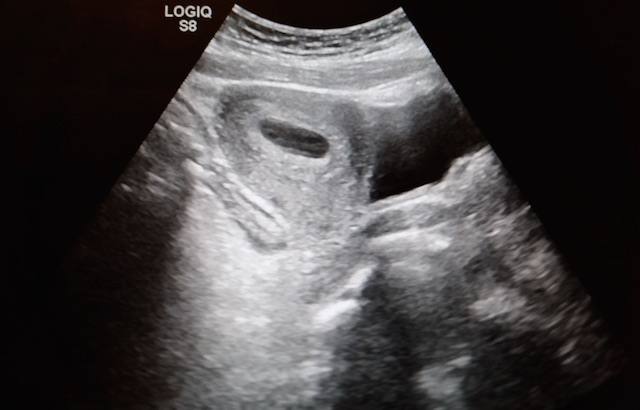
Pregnancy with Appendicitis
Take Home Points:
See previous pearl for how to conduct an ultrasound to evaluate for appendicitis.
Dewhurst C, Beddy P, Pedrosa I. MRI evaluation of acute appendicitis in pregnancy. J Magn Reson Imaging. 2013;37(3):566-75.
Israel GM, Malguria N, Mccarthy S, Copel J, Weinreb J. MRI vs. ultrasound for suspected appendicitis during pregnancy. J Magn Reson Imaging. 2008;28(2):428-33.
Segev L, Segev Y, Rayman S, Nissan A, Sadot E. The diagnostic performance of ultrasound for acute appendicitis in pregnant and young nonpregnant women: A case-control study. Int J Surg. 2016;34:81-85.
Segev L, Segev Y, Rayman S, Nissan A, Sadot E. Acute Appendicitis During Pregnancy: Different from the Nonpregnant State?. World J Surg. 2016.
Theilen LH, Mellnick VM, Longman RE, et al. Utility of magnetic resonance imaging for suspected appendicitis in pregnant women. Am J Obstet Gynecol. 2015;212(3):345.e1-6.
Category: Pharmacology & Therapeutics
Keywords: esmolol, ventricular fibrillation, cardiac arrest (PubMed Search)
Posted: 11/21/2016 by Michelle Hines, PharmD
(Updated: 12/3/2016)
Click here to contact Michelle Hines, PharmD
Consider esmolol IV 500 mcg/kg loading dose followed by a continuous infusion of 0-100 mcg/kg/min for patients in refractory ventricular fibrillation
Follow me on Twitter @mEDPharmD
