Category: Critical Care
Keywords: DKA (PubMed Search)
Posted: 8/23/2016 by Rory Spiegel, MD
Click here to contact Rory Spiegel, MD
Is it possible to have a patient present in diabetic ketoacidosis (DKA) with both negative serum and urinary ketone levels?
A case report published in American Journal of Emergency Medicine by Jehle et al provides a helpful reminder of this phenomenon (1). The degree of acidosis is directly related to the ratio of the various ketones/ketone metabolites: acetone, acetoacetate and beta-hydroxybutyrate present in the serum. The proportion of each respective substance is determined by the existing redox state in the blood. At any given time, acetoacetate and beta-hydroxybutyrate exist in an equilibrium dependent upon the ratio of NAD+ and NADH(fig.1). These substances freely convert with the assistance of the enzyme beta-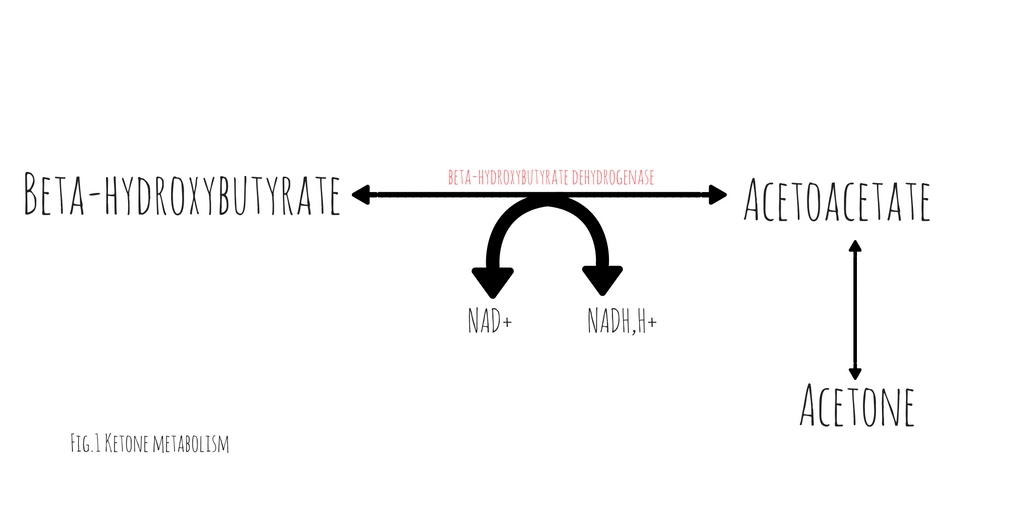 hydroxybutyrate dehydrogenase (2). This conversion requires the donation of a hydrogen atom from NADH. The balance between beta-hydroxybutyrate and acetoacetate, is determined by the ratio of NADH to NAD+. Acetoacetate will freely degrade into acetone through non-enzymatic decarboxylation. Early in DKA, acetoacetate is the most prevalent substance. As the disease progresses and the serum ratio of NADH to NAD+ increases, the proportion of beta-hydroxybutyrate rises, decreasing the quantity of acetoacetate and acetone.
hydroxybutyrate dehydrogenase (2). This conversion requires the donation of a hydrogen atom from NADH. The balance between beta-hydroxybutyrate and acetoacetate, is determined by the ratio of NADH to NAD+. Acetoacetate will freely degrade into acetone through non-enzymatic decarboxylation. Early in DKA, acetoacetate is the most prevalent substance. As the disease progresses and the serum ratio of NADH to NAD+ increases, the proportion of beta-hydroxybutyrate rises, decreasing the quantity of acetoacetate and acetone.
Traditional serum and urinary ketone assays react strongly to acetoacetate but neither reliably react with beta-hydroxybutyrate. Patients in whom the majority of their anion gap is filled by beta-hydroxybutyrate, urinary or serum ketone levels may be negative. In such cases, serum beta-hydroxybutyrate assays would be positive but are not universally available.
It is important to note, with resuscitation and insulin therapy, the ratio of NADH/NAD+ will start to normalize causing an increase in the quantity of acetoacetate. As the patient improves and the anion gap clears, the degree of ketones detected in the serum and urine will paradoxically increase.
1. Jehle D, et al, Severe diabetic ketoacidosis presenting with negative serum ketones: First case report and a review of the mechanism, Am J Emerg Med (2016)
2. Konijn, Abraham M., Naama Carmel, and Nathan A. Kaufmann. The redox state and the concentration of ketone bodies in tissues of rats fed carbohydrate free diets. The Journal of nutrition 10 (1976): 1507.
Category: Orthopedics
Keywords: Patellofermoral Syndrome (PubMed Search)
Posted: 8/20/2016 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
According to the 4th International Patellofemoral Pain Research Retreat recently published in British Journal of Sports Medicine, the core criterion required to define Patelofemoral Pain (PFP) syndrome is pain around or behind the patella, which is aggravated by at least one activity that loads the patellofemoral joint during weight bearing on a flexed knee (eg, squatting, stair ambulation, jogging/running, hopping/jumping).
Additional criteria (not essential):
PFP is common in young adolescents, with a prevalence of 7–28%, and incidence of 9.2%.
Stay tuned for recommendations on treatment and diagnosis.
Category: Pediatrics
Keywords: Trampoline, injury patterns (PubMed Search)
Posted: 8/19/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
From 2010-2014 ED visits in the US for injuries from trampoline parks (TPI) increased from 581 visits per year to 6932 visits per year. There was no change in the number of injuries related to home trampoline use. TPI were more likely to involve the lower extremity, be a dislocation and warrant admission and less likely to involve the head.
Bottom line: TPIs are increasing and have a different injury pattern compared to home trampolines.
Kasmire K, Rogers S and Sturm J. Trampoline Park and Home Trampoline Injuries. Pediatrics 2016: 138 (3).
Category: Toxicology
Keywords: One pill killers, pediatric (PubMed Search)
Posted: 8/17/2016 by Hong Kim, MD
(Updated: 8/18/2016)
Click here to contact Hong Kim, MD
In pediatric population, small dose or single pill ingestion can potential result in severe or lethal toxicity.
Clinicians should be mindful of potential toxicity following xenobiotic exposure (below) in pediatric population, especially under the age of 5 years old, even if the patient may initially appear asymptomatic.
Suspected ingestion of above medications/xenobiotics may warrent observation up to 24 hours in asymptomatic pediatric population.
Category: International EM
Keywords: Climate change, infectious diseases, environment (PubMed Search)
Posted: 8/17/2016 by Jon Mark Hirshon, MPH, MD, PhD
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
July 2016 was the hottest month ever recorded. As the temperature of the planet continues to rise, changes in infectious disease patterns of transmission are likely to occur. Many formerly exotic diseases, such as Zika, West Nile, malaria and cholera are spreading to new areas. Some of these are now found in the United States. Below is a table (from M. L. Wilson) that exemplifies how environmental changes can impact infectious diseases.
Bottom Line: Remain vigilant for unusual infectious diseases, especially among travelers. However recognize that many diseases have the potential to spread to the U.S., especially considering ongoing environmental changes.
www.who.int/globalchange/environment/en/chapter6.pdf
http://www.chgeharvard.org/topic/climate-change-and-infectious-disease
http://www.who.int/globalchange/climate/summary/en/index5.html
Wilson, M.L., Ecology and infectious disease, in Ecosystem Change and Public Health: A Global Perspective, J.L. Aron and J.A. Patz, Editors. 2001, Johns Hopkins University Press: Baltimore. p. 283-324.
Category: Orthopedics
Keywords: Hand infection (PubMed Search)
Posted: 8/13/2016 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
47yo M chef presents to your ED with 2 days of worsening left hand pain after sustaining a puncture wound to hand at work. The hand is red and swollen and he complains of pain. Interestingly, his index and middle digits are in an ABducted position at rest.
Collar Button Abscess
Web space infection of the palmer AND dorsal hand
The Palmer aponeurosis prevents volar extension (but promotes dorsal encroachment)
The pus spreads between the MC bones and erupts dorsally....creating a DORSAL abscess.
Loss of palmer concavity is seen.
ABduction of the adjacent digits, resulting in a "V" configuration with the apex pointing to the site of infection. This would not happen from simple pus in the dorsal space!
Can be missed if only focused on the dorsal hand. The palm will show the original injury (splinter, cut, foreign body)
Treatment is urgent surgical drainage.
http://www.eplasty.com/article_images/eplasty16ic06_fig1.gif
| Collar Button Abscess 2016 www.eplasty.com | |
| Elle Kalbfell, BSa, Nicholas S. Adams, MDa,b, and William T. Cullen, MD, MA, FACSa,b,c | |
|
|
Category: Neurology
Keywords: Uncal herniation, ipsilateral hemiplegia, Kernohan's notch, Kernohan's sign (PubMed Search)
Posted: 8/10/2016 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
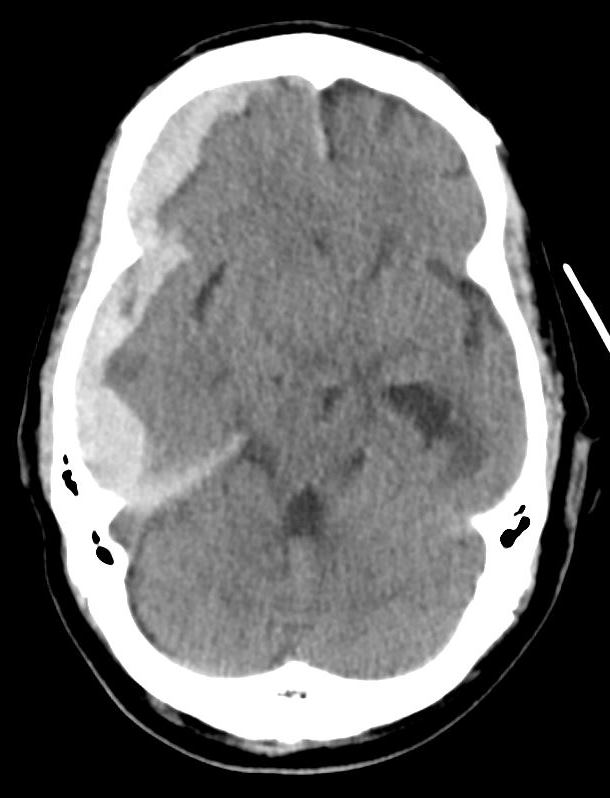
Diagram modified from "Localised Neurological Disease and Its Management A Intracranial". clinicalgate.com/localised-neurological-disease-and-its-management-a-intracranial/. Accessed 10 Aug 2016.
Follow me on Twitter @EM_NCC
Category: Critical Care
Keywords: Zika Virus, Guillain-Barre (PubMed Search)
Posted: 8/9/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Zika Virus-associated GBS
Thiery G, et al. Zika virus-associated Guillain-Barre syndrome: a warning for critical care physicians. Intensive Care Med 2016; epub ahead of print.
Category: Pharmacology & Therapeutics
Keywords: amiodarone, procainamide, ventricular tachycardia (PubMed Search)
Posted: 8/6/2016 by Michelle Hines, PharmD
Click here to contact Michelle Hines, PharmD
Amiodarone 150 mg IV over 10 minutes and procainamide IV 20-50 mg/min (up to 17 mg/kg) are two antiarrhythmic medications recommended in the American Heart Association (AHA) Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care for stable wide QRS complex tachycardia. [1]
What they did:
Multi-center, prospective, randomized, open-label trial comparing the incidence of major cardiac events in the acute treatment of hemodynamically stable patients with wide QRS monomorphic tachycardia (presumed to be VT) using amiodarone 5 mg/kg IV infused over 20 minutes versus procainamide 10 mg/kg IV infused over 20 minutes. [2] The study period was 40 minutes, starting from the beginning of the infusion.
What they found:
Application to clinical practice:
Follow me on Twitter (@mEDPharmD)
Category: Toxicology
Keywords: Hypoglycemia, Sulfonylureas (PubMed Search)
Posted: 8/4/2016 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
Drug-induced hypoglycemia is an often severe and symptomatic. It is a potentially preventable cause of significant morbidity. In one large study, it accounted for 23% for hospital admissions due to adverse drug events and 4.4% of overall admissions. The majority of hypoglycemic events occur with insulin and sulfonylureas. However, multiple drugs can affect glucose homeostasis and have been cited to cause hypoglycemia in therapeutic dose alone or in combination with other medications or illness. Factors that predispose to low blood sugar include reduced food intake, age, hepatic and renal disease, and severe infection. Beware of the possibility of inducing hypoglycemia in patients taking the following:
Agents with lesser quality evidence as predisposing medications or illnesses were present:
Drugs induced hypoglycemia should always be considered in the differential diagnosis of every patient presenting with low blood glucose. Octreotide antagonizes pancreatic insulin secretion and should be considered for first-line therapy in the treatment of sulfonylurea-induced hypoglycemia particularly when glucose levels cannot be maintained by dextrose infusions. Octreotide is administered 50 mcg subcutaneously (1-10 mcg in children) every 12 hours.
Category: Toxicology
Keywords: novel synthetic opioid, U-47700 (PubMed Search)
Posted: 8/1/2016 by Hong Kim, MD
(Updated: 5/4/2026)
Click here to contact Hong Kim, MD
Recently, there have been several news reports regarding the emergence of synthetic opioids in the U.S. and Canada. There are multiple synthetic opioids that have been identified as potential agents of abuse including W-18, U-47700, fentanyl derivatives, AH-7921 and MT-45. These compounds share a similar story with synthetic cannabinoid where they were synthesized for research purpose or by pharmaceutical companies but were not marketed. They are often sold as “research chemicals” over the internet.
In July 2016, three case reports have been published regarding several cases of U-47700 intoxication in San Diego, CA and Dallas, TX.
It is unknown if currently available heroin is cut with above mentioned synthetic opioids. Like other opioid receptor agonists, administration of naloxone will likely reverse the opioid toxidrome. But clinical experience in reversing synthetic opioids intoxication with naloxone is limited.
Bottom line:
Irrespective of whether an ED patient is exposed to synthetic opioids or "traditional" opioids of abuse (prescription opioid pain medication or heroin), the management of opioid intoxication management remains unchanged for respiratory depression.
Category: International EM
Keywords: Arbovirus, mosquitos (PubMed Search)
Posted: 8/3/2016 by Jon Mark Hirshon, MPH, MD, PhD
(Updated: 5/4/2026)
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
An Arbovirus is a virus transmitted primarily by an arthropod
There are a number of major arbovirus families:
The main viral family that causes substantial human disease is the Flaviviridae family.
Category: Critical Care
Keywords: ROSC, Cardiac Arrest, ETCO2 (PubMed Search)
Posted: 8/2/2016 by Rory Spiegel, MD
Click here to contact Rory Spiegel, MD
Despite a lack of prospective data, end-tidal CO2 (ETCO2) is often proposed as a viable replacement for the traditional pulse check to identify return of spontaneous circulation (ROSC) in patients presenting to the Emergency Department in Cardiac Arrest. A recent study by Tat et al examined this very question. The authors prospectively enrolled 178 patients suffering out-of-hospital cardiac arrest (OHCA) and examined the accuracy of a rise in ETCO2 at predicting ROSC. The authors examined both a rise of 10 and 20 mm Hg in ETCO2. Of the 178 patients included in this cohort, 60 (34%) experienced ROSC. The sensitivity and specificity of ETCO2 to predict ROSC at a threshold of 10 mm Hg was 33% and 97% respectively. At a threshold of 20 mm Hg ETCO2 performed no better with a sensitivity and specificity of 20% and 99% respectively.
What this data suggests is while a rise of ETCO2 of greater than 10 is highly suggestive of ROSC, the contrary cannot be said. The absence of a spike in ETCO2 does not rule out ROSC, as the large majority of patients experiencing ROSC in this cohort did so without demonstrating a significant rise in ETCO2. This evidence suggests that ETCO2 is a poor surrogate for a pulse check.
Tat LC, Ming PK, Leung TK, Abrupt rise of end tidal carbon dioxide level was a specific but non sensitive marker of return of spontaneous circulation in patient with out-of-hospital cardiac arrest, Resuscitation (2016), http://dx.doi.org/10.1016/j.resuscitation.2016.04.018
Category: Pediatrics
Keywords: airway. mac (PubMed Search)
Posted: 7/29/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
The pediatric epiglottis is more "U" shaped, often overlies the glottic opening, and is "less in line with the trachea."1 Because of this, it has traditionally been taught that a Miller blade is the ideal laryngoscope.
Varghese et al compared the efficacy of the Macintosh blade and the Miller blade when placed in the vallecula of children between the ages of 1 and 24 months. The blades provided similar views and suffered similar failure rates. When the opposite blade was used as a backup, it had a similar success rate as the opposing blade.2 Passi et al also compared these two blades, this time placing the Miller blade over the epiglottis. Again, similar views were achieved.3
1. Harless J, Ramaiah R, Bhananker S. Pediatric airway management. Int J. Crit Illn Inj Sci. 2014;4(1):65-70.
2. Varghese E, Kundu R. Does the Miller blade truly provide a better laryngoscopic view and intubating conditions than the Macintosh blade in small children? Paediatr Anaesth. 2014;24:825-829.
3. Passi Y, Sathyamoorthy M, Lerman J, et al. Comparison of the laryngoscopy views with the size 1 Miller and Macintosh laryngoscope blades lifting the epiglottis or the base of the tongue in infants and children <2 yr. of age. Br J Anaesth. 2014;113(5):869-874.
Category: Neurology
Keywords: SAH, headache, LP, CTA (PubMed Search)
Posted: 7/27/2016 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
Clinical Guidelines for the Emergency Department Evaluation of Subarachnoid Hemorrhage. Meurer WJ, Walsh B, Vilke GM and Coyne CJ. JEM 2016; 50(4) 696-701
Category: Critical Care
Posted: 7/26/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Predicting Fluid Responsiveness with ETCO2
Category: Orthopedics
Keywords: Chest, muscle injury (PubMed Search)
Posted: 7/24/2016 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
30yo male weight lifter who 10 days ago had a painful left shoulder injury after bench press. The next morning his left anterior chest wall and left upper arm were bruised and swollen. He went to see his PCP who diagnosed him with a muscle strain. 8 days later the bruising and swelling have resolved but he still cant move his shoulder and comes to the ED.
http://321gomd.com/wp-content/uploads/2015/01/pec-major-tears.jpg
The pec major attaches to the humerus and originates from the sternum and clavicle
Injury is usually due to tendon rupture off the humerus but can also occur at the muscle tendon junction or within the muscle belly itself.
Injury is becoming increasingly common due to the popularity in power lifting sports.
Mechanism: excessive tension on a maximally eccentrically contracted muscle.
Patients will complain of pain and weakness of the shoulder.
PE: Swelling and bruising to anterior medial arm. Palpable defect and deformity or anterior axially fold (may be hidden by swelling).
Weakness and pain with adduction and internal rotation and forward flexion
Chronic presentations can be challenging to diagnose. Consider ultrasound
Non operative treatment may be indicated for partial tears (sling, ice, NSAIDs)
Operative repair of tendon avulsions is very successful. Patients age, occupation/activity level and location of injury and condition of tear are considered.
Category: Critical Care
Posted: 7/20/2016 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Bucher J, Koyfman A. Intubation of the neurologically injured patient. J Emerg Med 2016; 49:920-7.
Category: International EM
Keywords: World Health Organization, blood donation (PubMed Search)
Posted: 7/9/2016 by Jon Mark Hirshon, MPH, MD, PhD
(Updated: 7/20/2016)
Click here to contact Jon Mark Hirshon, MPH, MD, PhD
Just the Facts:
112.5-million blood donations globally and half of these come from High-income countries
High-income countries more often use blood for supportive care during surgery, in traumas or therapy for malignancies
Low and middle-income countries more often use blood to manage pregnancy-related complications or in severe childhood anemia
General availability of blood is based on the donation rate
High-income countries have 33.1 donations/1000 people
Middle-income countries have 11.7 donations/1000 people
Low-income countries have 4.6 donations/1000 people
70 countries reported collecting fewer than 10 donations per 1000 people and half of these countries were in the African region
Disease prevalence in the region is reflected in the transmission rate of transfusion-transmissible infections (TTI)
Table 1. Prevalence of TTIs in blood donations (Median, Interquartile range (IQR)), by income groups
|
| HIV | HBV | HCV |
|
|---|---|---|---|---|
| High-income countries | 0.003% (0.001% – 0.040%) | 0.030% (0.008% – 0.180%) | 0.020% (0.003% – 0.160%) | |
| Middle-income countries | 0.120% (0.020% – 0.340%) | 0.910% (0.280% – 2.460%) | 0.320% (0.090% – 0.690%) | |
| Low-income countries | 1.080% (0.560% – 2.690%) | 3.700% (3.340% – 8.470%) | 1.030% (0.670% – 1.800%) |
Submitted by: Dr. Laura Diegelmann
Category: Misc
Keywords: Neck pain (PubMed Search)
Posted: 7/16/2016 by Michael Bond, MD
(Updated: 5/4/2026)
Click here to contact Michael Bond, MD
Non-Musculoskeletal Causes of Neck Pain
Neck pain is a common complaint of people presenting to the ED. Most of the cases will be musculoskeleteal in origin and will respond to conservative therapy with NSAIDs or acetominophen. However, other non-musculoskeletal causes of pain could be lurky behind this benign complaint.
Don't forget to consider:
